In a study in mice published in Nature, a research team showed that a newly developed compound was able to block necroptosis, a type of cell death that leads to lung inflammation and damage following infection with the flu virus.
Tag: Immune Response
Fatty food before surgery may impair memory in old, young adults
Eating fatty food in the days leading up to surgery may prompt a heightened inflammatory response in the brain that interferes for weeks with memory-related cognitive function in older adults – and, new research in animals suggests, even in young adults.
Long COVID patients show distinct immune, hormone responses to virus
People suffering from long COVID symptoms show different immune and hormonal responses to the virus that causes COVID-19, according to a new study led by researchers at Yale School of Medicine. An estimated 7.5% of people infected with the SARS-CoV-2…
Immune system changes behavior to promote allergen avoidance
The immune system plays a key role in changing our behaviors in response to environmental dangers, a new Yale School of Medicine study finds. Researchers found ova-allergic mice lost their avoidance behavior to the egg protein when Immunoglobulin E antibodies,…
Tracing maternal behavior to brain immune function
Immune system changes in the pregnant body that protect the fetus appear to extend to the brain, where a decrease in immune cells late in gestation may factor into the onset of maternal behavior, new research in rats suggests.
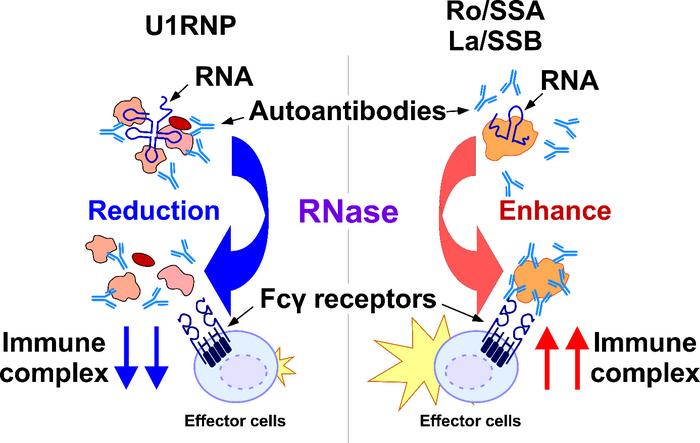
The double face of RNase as a treatment for systemic autoimmune diseases
Systemic autoimmune diseases are characterized by inflammation of multiple organs and can have devastating consequences for patients. There is a dire need for treatments against these diseases.
NUS researchers invent powerful tool to gather data on immune response at single-cell level
Scientists from the National University of Singapore have invented a powerful tool that captures data on immune cell response at a single-cell level. This groundbreaking technique will accelerate the discovery of new immunotherapies to treat diseases such as cancer, autoimmune disorders, and infectious diseases.
Researchers Reveal Why Viruses Like SARS-CoV-2 Can Reinfect Hosts, Evade the Immune Response
The human body is capable of creating a vast, diverse repertoire of antibodies—the Y-shaped sniffer dogs of the immune system that can find and flag foreign invaders.
Not getting enough sleep could blunt antibody response to vaccination, leaving you more vulnerable to infection
In reviewing data from previous studies, a team lead by researchers at the University of Chicago and the French National Institute of Health and Medical Research (Inserm) found that individuals who had fewer than six hours of sleep per night in the days surrounding vaccination had a blunted antibody response. That indicates efforts to promote heathy sleep duration ahead of an immunization could be an easy way to improve vaccine effectiveness.
New testing approach diagnoses COVID-19 with near-perfect accuracy
By inspecting the body’s immune response at a molecular level, a research team has developed a new way to test patients for COVID-19.
Protein ‘anchors’ found to play key role in neurotransmitter GABA action
New clues about the way brain chemical transmitter GABA functions suggest that a protein ‘anchor’ plays a key role in helping position its receptors in nervous cells.
A Consistent Lack of Sleep Negatively Impacts Immune Stem Cells, Increasing Risk of Inflammatory Disorders and Heart Disease
Mount Sinai study also shows catching up on sleep doesn’t reverse possible negative effects on cellular level
Cleveland Clinic Researchers Discover New Signal for Triggering Human Immune Response
Researchers from Cleveland Clinic’s Florida Research and Innovation Center (FRIC) found that disruption of a cellular structure, known as the actin cytoskeleton, is a “priming signal” for the body to respond to a virus. These findings, published in Cell this week, potentially lay the groundwork for development of new anti-viral vaccines and treatments.
Enhancing the effect of protein-based COVID-19 vaccines
Adding an ingredient called an adjuvant can help vaccines elicit a more robust immune response. In a study in ACS Infectious Diseases, researchers report a substance that boosted the immune response to an experimental COVID-19 shot in mice by 25 times, compared to injection with the vaccine alone.
Scientists develop effective intranasal mumps-based COVID-19 vaccine candidate
New research has advanced COVID-19 vaccine work in several ways: using a modified live attenuated mumps virus for delivery, showing that a more stable coronavirus spike protein stimulates a stronger immune response, and suggesting a dose up the nose has an advantage over a shot.
Mount Sinai Researchers Develop a Rapid Test to Measure Immunity to COVID-19
Mount Sinai researchers have developed a rapid blood assay that measures the magnitude and duration of someone’s immunity to SARS-CoV-2, the virus that causes COVID-19. This test will allow large-scale monitoring of the population’s immunity and the effectiveness of current vaccines to help design revaccination strategies for vulnerable immunosuppressed individuals, according to a study published in Nature Biotechnology in June.
Blocking enzyme could hold the key to preventing, treating severe COVID-19
Blocking an immune response-related enzyme holds promise in preventing or treating severe COVID-19 symptoms by reducing inflammation, tissue injury and blood clots in the lungs, new research in mice suggests.
Researchers find new mechanism to turn on cancer-killing T cells
In a new study, researchers at the University of Chicago Medicine Comprehensive Cancer Center and the University of Amsterdam have brought insight into one crucial step in the anti-cancer immune response process: T cell priming.
Study shines light on longevity of COVID-19 immune response
By uniting research from 8 cohorts across the U.S., a group of researchers has accelerated collection of data integral in answering questions about immune responses needed for long lasting protection from SARS-CoV-2.
COVID booster needed for broad protection against omicron variants
A COVID-19 booster shot will provide strong and broad antibody protection against the range of omicron sublineage variants of the SARS-CoV-2 virus in circulation, two new studies using serum from human blood samples suggest.
Researchers assess the power of T-cell immune response to Omicron BA.1 and BA.2
Scholars from HSE University and the RAS Institute of Bioorganic Chemistry have demonstrated the efficiency of T-cell immune response against the Omicron variant of SARS-CoV-2.
Study: Obesity raises the risk of gum disease by inflating growth of bone-destroying cells
Chronic inflammation caused by obesity may trigger the development of cells that break down bone tissue, including the bone that holds teeth in place, according to new University at Buffalo research that sought to improve understanding of the connection between obesity and gum disease.
A potential role for ibuprofen in older adults’ immunity to RSV
New research suggests there may someday be a role for ibuprofen in providing older adults with lasting immunity against RSV, a virus commonly associated with infants and young kids that also rivals the flu as a dangerous wintertime infection for the elderly.
Researchers Explore How Lack of Cadherin-11 Protein Drives Immune Response in Atherosclerosis
Article title: Impaired macrophage trafficking and increased helper T-cell recruitment with loss of cadherin-11 in atherosclerotic immune response Authors: Camryn L. Johnson, Lance Riley, Matthew Bersi, MacRae F. Linton, W. David Merryman From the authors: “The results from this study…
Long-term immune response to Sputnik-V COVID vaccine
The contributors are Kazan Federal University, Kazan State Medical Academy, Thapar Institute of Engineering and Technology, and the University of Liverpool.
COVID vaccine booster increases antibody responses, is protective in rhesus macaques
A booster dose of the mRNA-1273 COVID-19 vaccine given to rhesus macaques about six months after their primary vaccine series significantly increased levels of neutralizing antibodies against all known SARS-CoV-2 variants of concern, according to a new study from National Institutes of Health scientists and colleagues.
Einstein-Developed Treatment Strategy May Lead to HIV Cure
Armed with a novel strategy they developed for bolstering the body’s immune response, scientists at Albert Einstein College of Medicine have successfully suppressed HIV infections in mice—offering a path to a functional cure for HIV and other chronic viral infections. Their findings were published today in the Journal of Clinical Investigation.
LLNL joins Human Vaccines Project to accelerate vaccine development and understanding of immune response
Lawrence Livermore National Laboratory has joined the international Human Vaccines Project, bringing Lab expertise and computing resources to the consortium to aid development of a universal coronavirus vaccine and improve understanding of immune response.
Proteins that outwit emerging and re-emerging viruses
A family of proteins best known for their role in diminishing HIV infectivity may have the goods to outwit other emerging and re-emerging viruses, scientists have found.
Radiation Therapy Effectiveness for Cancer Patients Influenced by Gut Fungi
Cedars-Sinai Cancer researchers have discovered that intestinal microorganisms help regulate anti-tumor immune responses to radiation treatments, and that fungi and bacteria have opposing effects on those responses.
World-first COVID vaccine booster randomized clinical trial in transplant patients proves third shot is very effective
The study enrolled 120 transplant patients between May 25th and June 3rd. None of them had COVID previously and all of them had received two doses of the Moderna vaccine. Half of the participants received a third shot of the vaccine (at the 2-month mark after their second dose) and the other half received placebo.
The primary outcome was based on antibody level greater than 100 U/ml against the spike protein of the virus. In the placebo group – after three doses (where the third dose was placebo), the response rate was only 18% whereas in the Moderna three-dose group, the response rate was 55%.
Blocking how the malaria parasite suppresses the immune response
The parasites that cause severe malaria are well-known for the sinister ways they infect humans, but new research may lead to drugs that could block one of their most reliable weapons: interference with the immune response.
Studying how microbiome affects immunity could improve vaccine effectiveness
A new grant will help Iowa State University researchers figure out how the microbiome, or all the microorganisms that live inside and on human systems, affects immunity and the effectiveness of vaccines. Not everyone responds to vaccines in identical ways, and the researchers will search for ways humans can adjust their microbiomes to optimize vaccine response.
COVID-19 vaccine generates immune structures critical for lasting immunity
A new study from researchers at Washington University School of Medicine in St. Louis, published June 28 in the journal Nature, has found evidence that the immune response to Pfizer’s mRNA vaccine against COVID-19 is both strong and potentially long-lasting.
For Transplant Recipients, Third Time May Be the Charm for Better COVID Vaccine Protection
In a study published today in the Annals of Internal Medicine, Johns Hopkins Medicine researchers say they believe that, for the first time, there is evidence to show that three doses of vaccine increase antibody levels against SARS-CoV-2 — the virus that causes COVID 19 — more than the standard two-dose regimen for people who have received solid organ transplants.
Research Uncovers How ‘Non-professional’ Cells Can Trigger Immune Response
Researchers are finding new details on the complex dynamics involved in how organisms sense an infection from pathogens. The researchers found that worms can sense changes in their metabolism in order to unleash protective defenses, even if they don’t directly sense an incursion from pathogens.
Organ Transplant Recipients Remain Vulnerable to Covid-19 Even After Second Vaccine Dose
In a study published today in the Journal of the American Medical Association (JAMA), Johns Hopkins Medicine researchers show that although two doses of a vaccine against SARS-CoV-2 — the virus that causes COVID 19 — confers some protection for people who have received solid organ transplants, it’s still not enough to enable them to dispense with masks, physical distancing and other safety measures.
Story Tips from Johns Hopkins Experts on COVID-19
NEWS STORIES IN THIS ISSUE:
PREGNANT AFTER THE FIRST DOSE OF COVID-19 VACCINE — NOW WHAT?
STUDY SHOWS VACCINES MAY PROTECT AGAINST NEW COVID-19 STRAINS … AND MAYBE THE COMMON COLD
EXPANDED DASHBOARD TOOL RANKS ACCESSIBILITY OF STATE VACCINE WEBSITES
Scientists Discover How the Body Fights Viruses That Try to Evade the Immune System Response
Scientists have discovered a molecular pathway that counteracts the ability of some viruses to evade the immune response. The findings raise hope in generating better immune responses to viral infections, such as COVID-19, as well as to cancer.
Apes show dramatically different early immune responses compared to monkeys
A new study out of the University of Chicago and the University of Illinois Urbana-Champaign in humans, chimpanzees, rhesus macaques and baboons has found key differences in early gene expression in response to pathogen exposure, highlighting the importance of choosing the right animal model for the right questions.

MAJORITY OF CANCER PATIENTS WITH COVID-19 HAVE SIMILAR IMMUNE RESPONSE TO PEOPLE WITHOUT CANCER
Most people with cancer who are infected by the novel coronavirus produce antibodies at a rate comparable to the rest of the population—but their ability to do so depends on their type of cancer and the treatments they’ve received, according to a new study by researchers at Montefiore Health System and Albert Einstein College of Medicine. The findings, published online today in Nature Cancer, may lead to better care for cancer patients, who face a heightened risk of dying from COVID-19, and suggests that cancer patients should respond well to COVID-19 vaccines.
Genetics May Play Role in Determining Immunity to COVID-19
UC San Diego researchers report that individual immune response to SARS-CoV-2 may be limited by a set of variable genes that code for cell surface proteins essential for the adaptive immune system. The finding may help explain why COVID-19 immunity varies by individual.
COVID-19 vaccine creates incentive to improve our health
While we wait for our turn to get vaccinated against SARS-CoV-2, we could – and probably should – use the time to make sure we bring our healthiest emotional and physical selves to the treatment, a new review of previous research suggests.
Scientists identify “immune cop” that detects SARS-CoV-2
Scientists at Sanford Burnham Prebys Medical Discovery Institute have identified the sensor in human lungs that detects SARS-CoV-2 and signals that it’s time to mount an antiviral response.
Protecting lungs from ventilator-induced injury
An unfortunate truth about using mechanical ventilation to save lives is that the pressure can cause further lung damage. Scientists are working to boost a natural cellular process in pursuit of a therapy that could lower the chances for lung damage in patients on ventilators.
E-cigarette Users at Greater Risk of Poor Immune Response to Viruses
In a controlled study, scientists found that smokers and e-cigarette users exhibited significantly altered immune responses to a model of influenza virus infection, suggesting increased susceptibility to disease, including COVID-19
Researchers Find Impaired Mitochondrial and Metabolic Function in COVID-19 Patients
New research published ahead of print in the American Journal of Physiology-Cell Physiology explores the role of mitochondrial function and related metabolic changes in the inflammatory response seen in people with COVID-19, the disease caused by the SARS-CoV-2 virus. Dysfunction…
Story Tips From Johns Hopkins Experts On COVID-19
For many of us, this year’s holiday season may look different, and many are asking how we can enjoy the fellowship of the season while keeping ourselves, our loved ones and our communities safe from COVID-19.

Fighting Zika? Call in the T cells
In a new Science Advances study, Shresta and her colleagues at LJI report that the immune system’s T cells have the power to prevent Zika infection in mice. This finding suggests that effective Zika vaccines need to activate T cells to work alongside antibodies.
New Johns Hopkins Center for Research on COVID-19 Immunity
Researchers at the Johns Hopkins Bloomberg School of Public Health and Johns Hopkins University School of Medicine have been jointly awarded a major grant from the National Cancer Institute, part of the National Institutes of Health, to set up a center for research on the human serological immune response to SARS-CoV-2, the coronavirus that causes COVID-19.