Flu vaccination mandates for hospital staff have increased in recent years, especially at hospitals serving veterans, the latest in a series of surveys shows.
Tag: Influenza

Bird Flu Basics: Safety, Symptoms and Risks
The highly infectious bird flu, also known as avian influenza H5N1, primarily spreads among birds. However, there have been rare cases of infection to humans. According to the Centers for Disease Control and Prevention, two human cases of H5N1 have…
Digital reminders for flu vaccination improves turnout, but not clinical outcomes in older adults
An analysis of the the NUDGE-FLU (Nationwide Utilization of Danish Government Electronic letter system for increasing inFLUenza vaccine uptake) trial found that using digital reminders, or “electronic nudges,” improved influenza vaccine rates among older adults, but did not improve clinical outcomes.
Measles: How to Spot it, When to Seek Care and Importance of Vaccination
As the Measles outbreak continues to grow in Florida, Francesca Torriani, MD, infectious disease specialist with UC San Diego Health is available to discuss symptoms to look out for, when to seek medical care, and the importance of vaccination. Biography…
Study Could Help Clear Up Confusion and Hesitancy Surrounding RSV Vaccines
Efforts to vaccinate vulnerable populations against respiratory syncytial virus (RSV) faced an uphill battle this season. However, now a new study by researchers at New York Institute of Technology College of Osteopathic Medicine (NYITCOM) could help to combat RSV vaccine misinformation and quell vaccine…
Scientists discover hidden army of lung flu fighters
Scientists have long thought of the fluid-filled sac around our lungs merely as a cushion from external damage.
Interactions between flu subtypes predict epidemic severity more than virus evolution
Researchers have shed new light on how viral evolution, population immunity, and the co-circulation of other flu viruses shape seasonal flu epidemics.
Infectious Disease Expert Available: Flu Season, COVID-19 Variant and other Respiratory Viruses
In the United States, flu season usually occurs in the fall and winter, and while influenza viruses spread year-round, most of the time flu activity peaks between December and February. The overall impact of the flu varies from season to…
Navigating Childhood Asthma: Insights From a Pediatric Pulmonologist
As the seasons transition from warm fall nights to cool and wintry evenings, children with asthma often experience a rise in wheezing or chest tightness, because weather changes and cold temperatures are often asthma triggers.
Initiative to Strengthen Response to Infectious Disease Outbreaks in the Mountain West
The COVID-19 pandemic spotlighted how a rapid and effective response to infectious disease outbreaks is critical for saving lives and protecting communities. With a $17.5 million, five-year grant from the U.S. Centers for Disease Control and Prevention (CDC), University of Utah researchers, in collaboration with Washington State University, are leading efforts to provide data and tools that guide decisions to improve responses to emerging public health threats in the Mountain West.
Avoiding a “Tripledemic” This Winter
A Rutgers infectious disease expert explains what you need to know about this year’s flu, COVID and new RSV shots
Scientists unpick how lung cells induce immune response to influenza
Researchers from Trinity College Dublin have discovered some new and surprising ways that viral RNA and influenza virus are detected by human lung cells, which has potential implications for treating people affected by such viruses.
Study Reveals Patients Hospitalized with COVID-19 Faced Nearly Twice the Rates of Death After Discharge As Patients with Flu
Researchers demonstrate that among individuals who were admitted to the hospital with COVID-19 and were discharged alive, the risk of post-discharge death was nearly twice that observed in those who were discharged alive from an influenza-related hospital admission.

Sick of sports? Study shows flu deaths rise when pro sports teams move into cities
Given their research indicating public health suffers when a professional sports team makes its home in a new city, West Virginia University economists are asking whether publicly funded subsidies for sports arenas make sense.
Mutation accessibility fuels influenza evolution
Scientists at St. Jude Children’s Research Hospital showed that fixed mutations within a viral population most likely stem from how easy it is to acquire that mutation (i.e., mutation accessibility) rather than just its benefit.
Genetic change increased bird flu severity during U.S. spread
Scientists at St. Jude Children’s Research Hospital have discovered H5N1 avian influenza viruses gained the ability to cause severe disease and target the brain in mammals as they spread across North America.

Global health and zoonotic diseases expert available to speak on avian flu virus
Oladele “Dele” Ogunseitan, PhD serves as the University of California Presidential Chair and Professor of Population Health and Disease Prevention at the UC Irvine Program in Public Health. He is a renowned expert in the field of global health and…
Method for improving seasonal flu vaccines also aids pandemic prediction
The seasonal flu vaccine is less effective in some years than others. New St. Jude research showed one reason behind this lack of efficacy is the inclusion of flu strains with an unstable viral protein.
Journal of Medical Internet Research | Can Artificial Intelligence Be Used to Diagnose Influenza?
JMIR Publications published “Examining the Use of an Artificial Intelligence Model to Diagnose Influenza: Development and Validation Study” in the Journal of Medical Internet Research, which reported that it may be possible to diagnose influenza infection by applying deep learning to pharyngeal images given that influenza primarily infects the upper respiratory system.
Is it COVID-19 or the flu? New sensor could tell you in 10 seconds
Scientists report using a single-atom-thick nanomaterial to build a device that can simultaneously detect the presence of the viruses that cause COVID-19 and the flu — at much lower levels and much more quickly than conventional tests for either. They will present their results at ACS Spring 2023.
Stickiness may determine how influenza spreads
Influenza viruses have an enormous impact in the U.S., with an estimated 25 million illnesses and 18,000 deaths in the 2022-23 flu season alone. However, the majority of virus particles are not infectious or are only partially infectious. How, then, do they become such a contagious and deadly virus?
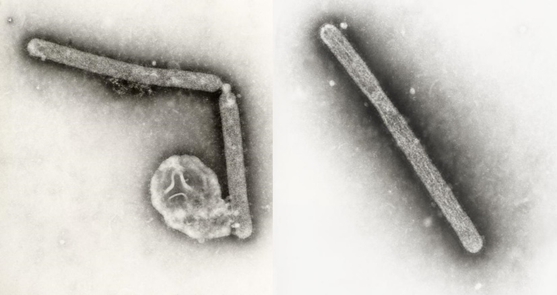
Avian influenza viruses could spawn the next human pandemic
The next pandemic that cascades through the human population could be caused by a new influenza virus strain concocted in animals, against which humans will have little to no immunity.
Not getting enough sleep could blunt antibody response to vaccination, leaving you more vulnerable to infection
In reviewing data from previous studies, a team lead by researchers at the University of Chicago and the French National Institute of Health and Medical Research (Inserm) found that individuals who had fewer than six hours of sleep per night in the days surrounding vaccination had a blunted antibody response. That indicates efforts to promote heathy sleep duration ahead of an immunization could be an easy way to improve vaccine effectiveness.
The Achilles heel of the influenza virus: ubiquitin protein may be an approach for future medicines
Every year, the influenza season presents a challenge to hospitals. Despite having been vaccinated, older people and patients with health problems in particular run a heightened risk of falling prey to a severe bout of influenza.
Octavio Ramilo, M.D., named chair of the Department of Infectious Diseases at St. Jude Children’s Research Hospital
Internationally renowned expert will focus on growing
St. Jude into a global leader in infectious diseases research.
Flu season came early, hit hard in Tennessee
Flu season came a month early this year in Tennessee and hit hard, disproportionately affecting children, according to Epidemic Intelligence Service (EIS) data gathered by the Centers for Disease Control and Prevention (CDC), Tennessee Department of Health and Vanderbilt University Medical Center.
Study Finds Risk of Seizures Is Higher After COVID-19 Than After Influenza
People who have a COVID-19 infection are more likely to develop seizures or epilepsy within the next six months than people who have an influenza infection, according to a study published in the November 16, 2022, online issue of Neurology®, the medical journal of the American Academy of Neurology.
As respiratory illnesses increase, WVU experts share information to prevent possible ‘tridemic’
Respiratory illnesses are affected the United States as winter approaches, and a “tridemic” is possible with the flu, COVID-19 and RSV.
Potential therapy derived from a banana protein works against SARS-CoV-2
A paper in Cell Reports Medicine details the efficacy of H84T-BanLec against all known human-infecting coronaviruses, including MERS, the original SARS, and SARS-CoV2, including the omicron variant.
Needs and Challenges for COVID-19 Boosters and Other Vaccines in the U.S.
FAU researchers and collaborators provide the most updated guidance to health care providers and urge how widespread vaccination with these boosters can now avoid the specter of future and more lethal variants becoming a reality.
UCLA Fielding School of Public Health-led research demonstrates the importance of influenza vaccination globally
An international team of researchers has demonstrated that among patients hospitalized for influenza, those who were vaccinated had less severe infections, including reducing the odds for children requiring admittance to an intensive care unit by almost half.
Houston Methodist seeing December flu season peak numbers now
Texas already has a moderately high rate of flu cases in September. This doesn’t look good for flu season, which was uncharacteristically low last year because of masks and people isolating. Houston Methodist experts are encouraging the community to get the flu shot early. Experts say cases aren’t usually seen this high until December, which is when the season usually peaks.
Can I Get the Flu From Touching Surfaces? Rutgers Researcher Says No.
In the early stages of the COVID-19 pandemic, the coronavirus was everywhere – stuck to our cellphone screens, smeared on our mail, dangling from doorknobs, even clinging to our cereal boxes. Except that it wasn’t.
Despite public health guidance suggesting surfaces be disinfected to stop the spread of COVID-19, the virus wasn’t significantly transmitted through inanimate surfaces and objects, what microbiologists call “fomites.” As with all respiratory viruses – from the flu to the common cold – transmission was and remains almost exclusively airborne.
Emanuel Goldman, a professor of microbiology at the Rutgers New Jersey Medical School, was among the first scientists to challenge conventional wisdom by warning that hygiene theater – overzealous disinfection of surfaces – had “become counterproductive” for public health.
Why the Flu Vaccine is More Important Than Ever This Year
A Rutgers infectious disease expert explains why getting the annual flu shot is important to individual and public health
University Hospitals Chosen as Site for United States Flu Vaccine Effectiveness Network
The Center for Disease Control’s National Center for Immunization and Respiratory Diseases has awarded University Hospitals of Cleveland a sizable grant to support its assignment as a study site in the United States Flu Vaccine Effectiveness Network.
Universal flu vaccine protects against variants of both influenza A and B viruses
A new universal flu vaccine protects against diverse variants of both influenza A and B viruses in mice, according to a new study by researchers in the Institute for Biomedical Sciences at Georgia State University.
JMIR Public Health and Surveillance | Diagnostic Accuracy of Self-test for Influenza
JMIR Publications recently published “Diagnostic Accuracy of an At-Home, Rapid Self-test for Influenza: Prospective Comparative Accuracy Study” in JMIR Public Health and Surveillance which reported that rapid diagnostic tests (RDTs) for influenza used by individuals at home could potentially expand access to testing and reduce the impact of influenza on health systems. Improving access to testing could lead to earlier diagnosis following symptom onset, allowing more rapid interventions for those who test positive, including behavioral changes to minimize spread.
UTSW scientists identify protein key to inhibiting flu virus
A collaborative study from UT Southwestern scientists has identified a new function for a protein called TAO2 that appears to be key to inhibiting replication of the influenza virus, which sickens millions of individuals worldwide each year and kills hundreds of thousands. The findings were published in PNAS.
New research at UH Rainbow Babies & Children’s Hospital evaluates critical illness from COVID-19 vs influenza in children
Researchers at UH Rainbow published new findings that COVID-19 is not equivalent to flu infection for children. Among 66 pediatric ICUs in the US, the number admitted each quarter with COVID-19 or MIS-C during the first 15 months of the pandemic was twice as high as that for flu pre-pandemic.
Cleveland Clinic Appoints Ted Ross, Ph.D., as Global Director of Vaccine Development
Ted Ross, Ph.D., has been appointed Global Director of Vaccine Development at Cleveland Clinic.
In this newly created role, he will lead the development of novel vaccine platforms for a variety of infectious diseases, including influenza, HIV and COVID-19. A highly renowned scientist with expertise in virology, vaccines, immunology and microbiology, Dr. Ross’ research focuses on the design of new vaccines and the implementation of new vaccine trials.
Flu Season Underway Amid Ongoing COVID-19 Pandemic
For the second straight year, flu season is emerging against the backdrop of the COVID-19 pandemic. While the number of flu cases was relatively low last year, experts at Johns Hopkins Medicine say that this year, it could be much higher.
Which older adults are getting flu shots and COVID boosters? Poll shows variation
With two viruses threatening to make older adults sick this winter, a new poll shows most people over 50 have gotten protected by vaccines against both influenza and coronavirus, or plan to. And a majority of those who have gotten the COVID-19 vaccine plan to get an additional dose. But the poll also reveals major differences in vaccine attitudes between older adults, including those of different political leanings.
Clip Health (formerly Luminostics) Announces Company Rebranding, Immediate Product Pipeline
Clip Health has rebranded from Luminostics ahead of exciting product launches this fall.
Shrinking Waveforms on Electrocardiograms Predict Worsening Health and Death of Hospitalized COVID-19 and Influenza Patients
Spotting changes in the heart’s electrical activity may prompt more-aggressive treatment and monitoring.
Flu Season Is Around the Corner–Get Your Shot Now
Masking, physical distancing and other measures employed to fight the COVID-19 pandemic virtually eliminated influenza during the 2020-2021 flu season. But Cedars-Sinai physicians say the flu is headed for a comeback and they urge everyone 6 months and older to get their flu shots.
Flu Season Returns: How to Stay Safe
While social distancing and wearing masks kept last year’s flu season at an all-time low, experts expect flu cases will soar this year as students return to school and employees go back to the office and are urging people to get their flu vaccine to prevent the nation’s health care system from being overwhelmed by influenza and COVID-19.
David Cennimo, an infectious disease expert at Rutgers New Jersey Medical School, discusses what you should do to protect yourself during the upcoming flu season.
Vaccines grown in eggs induce antibody response against an egg-associated glycan
Researchers have found that viral vaccines grown in eggs, such as the H1N1 flu vaccine, produce an antibody response against a sugar molecule found in eggs, which could have implications for the effectiveness of these vaccines.
Study Links COVID-19 Public Health Efforts to Dramatic Drop in COPD Hospitalizations
Public health measures designed to reduce the spread of the COVID-19 virus may have fostered a substantial side benefit: A 53 percent drop in hospital admissions for chronic obstructive pulmonary disease (COPD), likely due to a drop in circulating seasonal respiratory viruses such as influenza.
Rutgers Engineers Developing Rapid Breathalyzer Test for COVID-19
New Brunswick, N.J. (April 30, 2021) – Rutgers University–New Brunswick engineering professors Edward P. DeMauro, German Drazer, Hao Lin and Mehdi Javanmard are available for interviews on their work to develop a new type of fast-acting COVID-19 sensor that detects the presence…
UGA to establish national NIH-funded center to fight flu
The National Institutes of Health has awarded the University of Georgia a contract to establish the Center for Influenza Disease and Emergence Research (CIDER). The contract will provide $1 million in first-year funding and is expected to be supported by the National Institute of Allergy and Infectious Diseases (NIAID), part of NIH, for seven years and up to approximately $92 million.