Top honor recognizes her commitment to justice, equity, diversity, and inclusion through scholarship, mentorship, and leadership
Tag: Emergency Room
Quality of Care for Patients Who Call 911 Varies Greatly Across the United States, Study Finds
Mount Sinai research could lead to more consistency and safety measure.
Women stroke survivors believe they will receive worse care in the emergency room
Women who have survived a stroke believe they are less likely to receive adequate emergency care – based on gender and race or ethnicity, a study shows. Researchers say future studies must focus on whether the beliefs these women hold about emergency care are leading to delays in stroke care.
Hazardous Drinking in Young Adults: Personal Characteristics Can Help Identify Effective Interventions
Young adults whose drinking lands them in the emergency room respond differently to different interventions to reduce their hazardous drinking, and those differences may be driven by certain personal characteristics.
‘Concerning’ CT scans may cause unnecessary hospitalization for some pulmonary embolism patients
Some pulmonary embolism patients may be hospitalized unnecessarily due to CT imaging results rather than clinical risk factors, a study finds. Roughly half of the low risk patients had CT imaging features that physicians consider “concerning”, and these patients fared just as well in the hospital as those whose CT scans showed no concerning findings.
Cost concerns keep older adults from seeking emergency care
Worries about what emergency care might cost them have kept some older adults from seeking medical attention even when they felt they might need it, a new study shows. In all, 22% of older adults who may have needed care from the emergency department didn’t go because of concerns about what they might have to pay.
Objective Blood Alcohol Measures Confirm the Limitations of Questionnaires and Offer Increased Clinical Opportunities for Treating Dangerous Drinking
Patients in the Emergency Room (ER) should be blood-tested for hazardous drinking rather than evaluated by questionnaires alone, according to a new study comparing alcohol use screening methods. A sizeable minority of patients attend the ER for alcohol-related reasons (12–15% in the UK). That proportion is growing, a US study has found. The ER offers valuable opportunities to identify hazardous drinking and intervene with treatments that can help patients reduce their alcohol use. This requires efficiently and reliably screening ER patients for risky consumption. Validated methods include the Alcohol Use Disorders Identification Test (AUDIT) — and its shorter version, AUDIT-C —which are among the most frequently used screening questionnaires. Another, the Timeline Followback Questionnaire (TLFB), is a retrospective self-administered survey estimating daily alcohol consumption over a specific prior period. In contrast, phosphatidylethanol (PEth), a metabolite of ethanol, is a direct and
Happy, Healthy Holiday Tips — Johns Hopkins Children’s Center Experts Available to Discuss Staying Safe and Healthy this Holiday Season
Navigating RSV, COVID-19 and the Flu As more people travel and gather with family and friends this holiday season, cases of COVID-19, RSV and the flu are high and, in some areas, rising across the country. How can we keep…
Mount Sinai First in Region Offering Telehealth Visits for Low-Acuity 911 Ambulance Calls
Unique program keeps patients with less severe conditions out of the Emergency Department, saving them time and money

Mental health, substance use issues prevalent among nonpsychiatric emergency room patients
A new study found that about 45% of patients who visit the emergency department for physical injuries and ailments also have mental health and substance use problems that are often overlooked.
Study Finds Automated Texts Decrease Odds of Rehospitalization
Text messages sent automatically from patients’ primary care office after hospitalization were tied to decreased odds of needing further emergency care
An emergency in U.S. emergency care: Two studies show rising strain
Despite decades of effort to change emergency care at American hospitals and cope with ever-growing numbers of patient visits, the system is showing increasing signs of severe strain, according to two new studies of patients leaving without being seen or waiting in emergency department for hours for a hospital bed.
Mount Sinai’s Brendan Carr, MD, MS, Receives Prestigious “Chair of the Year Award” from Emergency Medicine Residents’ Association
The Emergency Medicine Residents’ Association (EMRA) of the American College of Emergency Physicians has honored Brendan G. Carr, MD, MS, Chair of Emergency Medicine at the Icahn School of Medicine of Mount Sinai and Mount Sinai Health System, with the prestigious “2022 Chair of the Year Award.” He is the only department chair in the country to receive this distinction for 2022, recognizing his exceptional leadership.
Shrinking Waveforms on Electrocardiograms Predict Worsening Health and Death of Hospitalized COVID-19 and Influenza Patients
Spotting changes in the heart’s electrical activity may prompt more-aggressive treatment and monitoring.
UCLA Investigators Approved for Study on Youth Suicide Prevention
A research team from the UCLA Youth Stress and Mood Program at UCLA’s Jane and Terry Semel Institute for Neuroscience and Human Behavior has been approved to lead a $13 million funding award by the Patient-Centered Outcomes Research Institute (PCORI) to compare two evidence-based interventions for reducing suicide attempts and improving patient outcomes for youth presenting to emergency departments.
The Medical Minute: When to head for urgent care instead of the hospital emergency room
Urgent care or emergency room? A certified nurse practitioner discusses how to choose what’s right for your crisis in this week’s Medical Minute.
Latest COVID Wave Fills Beds, Hammers Michigan ER Workers
Michigan Medicine’s adult and pediatric emergency rooms are experiencing a surge in positive COVID cases and hospitalizations. Younger patients are being admitted and Michigan is seeing a spread of the B.1.1.7 variant. Physicians are again asking the public for help to save lives and keep the ICUs from hitting capacity.
Artificial Intelligence Algorithm Can Predict Outcomes of COVID-19 Patients With Mild Symptoms in Emergency Rooms
Technology may lead to quicker triage and treatment based on patient data and scans
Canadian discovery: a potential game-changer to reverse alcohol intoxication
In a study published today in Scientific Reports, a Nature Research Journal, a team of researchers led by Dr. Joseph Fisher presents a proof of concept of a simple method that could become a game-changer in rescue therapy for severe alcohol intoxication, as well as just “sobering up.”
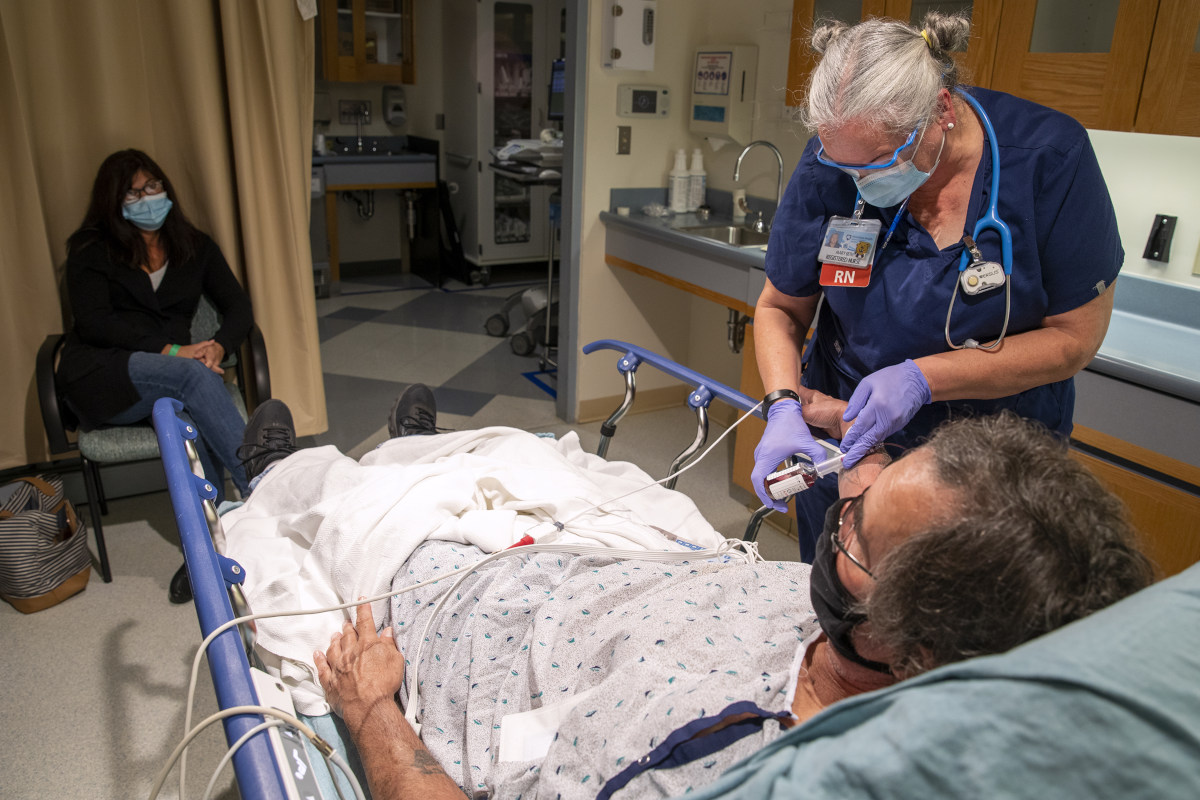
The Medical Minute: Planning ahead for a potential emergency department visit
Medical emergencies, by their nature, come with very little or no warning. While any injury or illness that requires a trip to the emergency department will likely cause distress, putting an action plan in place now can help minimize the anxiety and fear of a future visit.
MEDIA ADVISORY- Back to School, Cold & Flu Season and COVID-19 – What do you do if you get sick?
Mount Sinai experts say get your flu shot early and have a plan for point-of-care
AI Shows Promise in Accurately Identifying Infants with Low Risk of Serious Bacterial Infection
Artificial intelligence, or “supervised machine learning,” could help identify which well-appearing infants with fever, who are 60 days old or younger, are at low risk for a serious bacterial infection, according to a study published in Pediatrics. Accurate risk determination could reduce unnecessary lumbar puncture, antibiotics and hospitalizations for these infants, as well as decreasing parental anxiety.
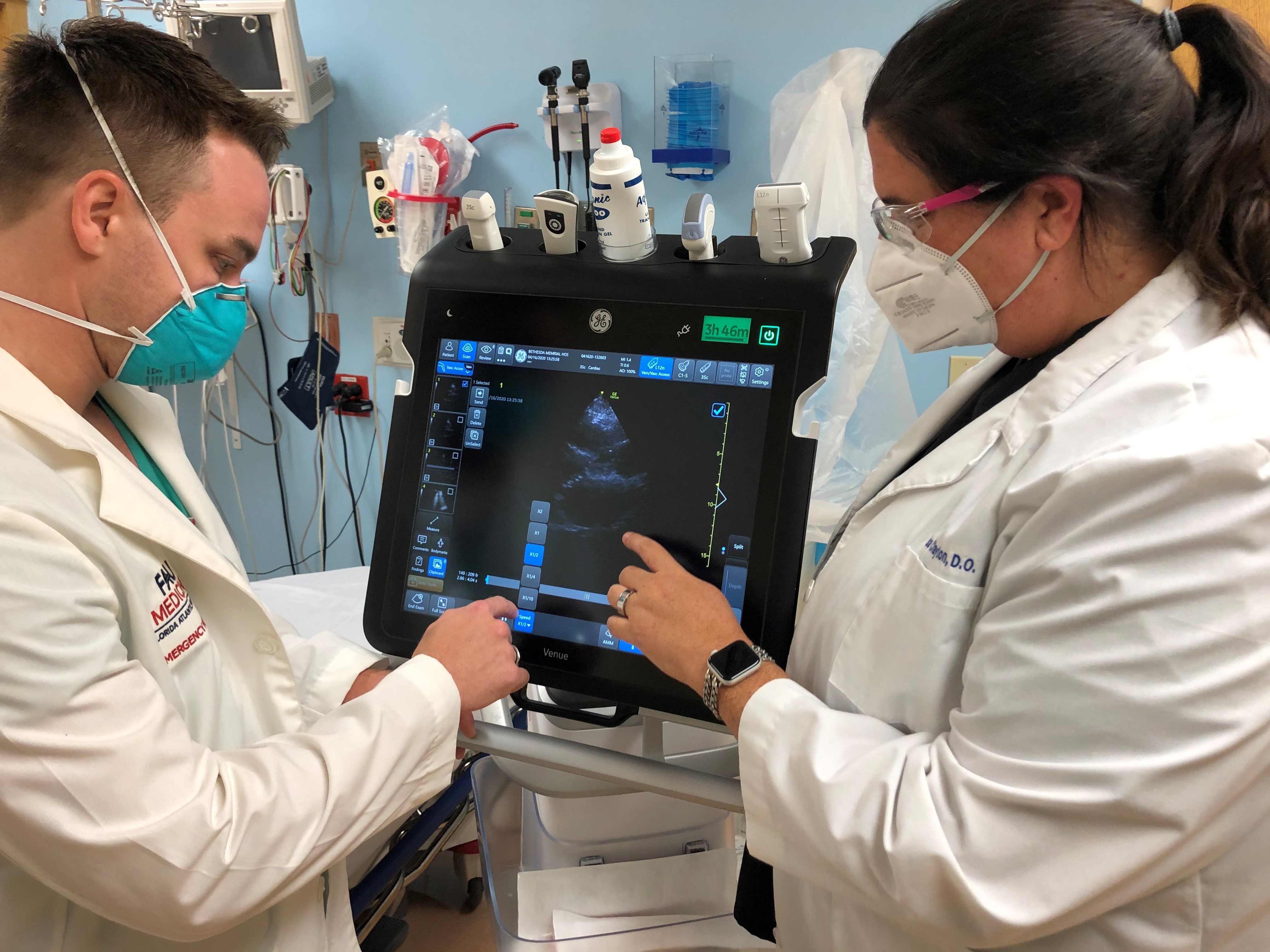
‘With This Ring,’ Scientists Hope to Predict COVID-19 in Healthcare Workers
A three-pronged approach will help to predict COVID-19 infection in healthcare workers. At the center of it all – a ring, which tracks vitals such as heart rate and temperature and alerts the user that they might be getting sick without even realizing it. The study also will determine if participants go on to develop an acute COVID-19 infection and the prevalence rate in that population. Researchers hope to better identify patterns that could predict the emergence and recovery from novel infections to prevent and contain future pandemics.
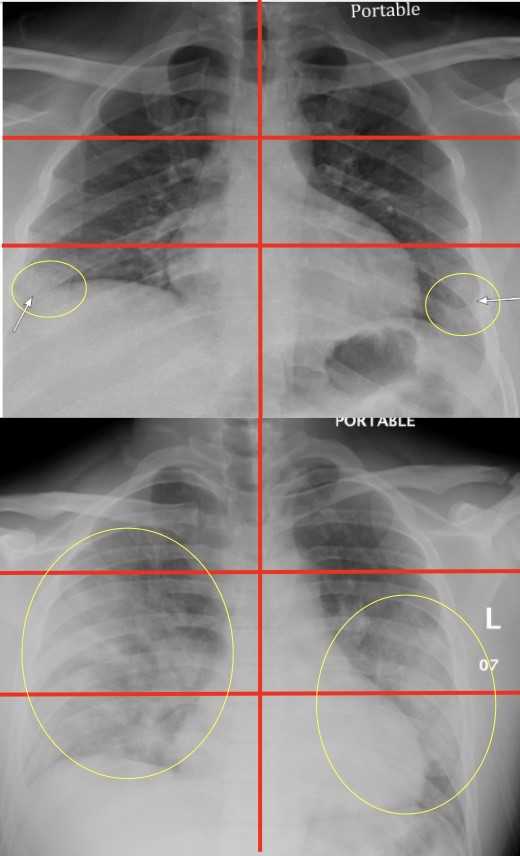
Chest X-Rays in Emergency Rooms Can Help Predict Severity of COVID-19 Illness in Young and Middle-aged Adults
Chest X-rays performed on young and middle-aged adults with COVID-19 when they arrive at the emergency room can help doctors predict who is at higher risk of severe illness and intubation, Mount Sinai researchers report.