JMIR Publications invites submissions to a new theme issue titled “First Look: Early Research, Viewpoints, and Experiences with Apple Vision Pro in Health Care Settings” in its new open access journal JMIR XR and Spatial Computing.
Tag: Telemedicine
MSU study reveals rapid growth, persistent challenges in telemedicine adoption among US hospitals
A new study led by Michigan State University researchers shows a significant increase in telemedicine services offered by U.S. hospitals from 2017 to 2022, while also highlighting persistent barriers to its full implementation.
Telemedicine may increase endocrinology care access for under-resourced patients with diabetes and heart disease
Widespread availability of telemedicine during the pandemic led to more equitable access to endocrinology care for patients with type 2 diabetes and heart disease, according to a study being presented Monday at ENDO 2024, the Endocrine Society’s annual meeting in Boston, Mass.
Telemedicine Can Help Change Care for the Better — If We Get the Rules Right
Experts say pandemic-era rules that promoted telemedicine should be made permanent to protect gains in quality of care and greater access for millions of patients. New analysis shows enhanced telemedicine services led to higher quality of care and better access and only a modest increase in spending.

Medicare pays for message-based e-visits. Are older adults using them?
E-visits have become a regular part of everyday health care for some of the 30 million older Americans who have traditional Medicare. About 1% of them have used asynchronous patient portal messaging in a way that prompted their doctor or other health care provider to bill Medicare for their time.
Rapid Telehealth Consults Improve Care for Rural Patients With Stroke
A telestroke program at Essentia Health addressed barriers to rapid diagnosis and intervention for rural patients with stroke symptoms, decreasing door-to-needle time and improving outcomes.
Deep-dive on telehealth use in Michigan shows importance for mental, rural & out-of-state care
A new single-state report looks at patterns of telehealth use by people with different forms of insurance before and during the pandemic, and could inform post-pandemic health policy.
Wake Forest University School of Medicine Approved for $4.4 Million PCORI Funding Award to Study Telehealth
A team of researchers at Wake Forest University School of Medicine has been approved for a $4.4 million funding award from the Patient-Centered Outcomes Research Institute (PCORI) to assess the benefits of expanding telehealth by primary care physicians to children with complex chronic conditions and their caregivers. The project is a collaboration with Atrium Health Wake Forest Baptist Brenner Children’s in Winston-Salem and Atrium Health Levine Children’s in Charlotte.
Mount Sinai Launches Center for Ophthalmic Artificial Intelligence and Human Health
The Icahn School of Medicine at Mount Sinai has launched the Center for Ophthalmic Artificial Intelligence and Human Health, the first of its kind in New York and one of the first in the United States.
Telemedicine Visits Cut Health System Employee Care Costs by Nearly 25 Percent
Comparing Penn Medicine OnDemand services with in-person care showed that telemedicine visits are significantly less expensive to deliver
ACP calls for appropriate and meaningful measures to evaluate telemedicine
As the amount of health care services provided to patients using telemedicine increases, physicians must ensure the quality of the performance measures being used to evaluate that care, says the American College of Physicians (ACP) in a new policy paper. The paper details new recommendations to ensure that as measures are developed to gauge telemedicine services they are evidence-based, methodologically sound and clinically meaningful. The paper is published in Annals of Internal Medicine.
Local Leaders Announce Plan to Strengthen Health Services in Imperial County
Representatives from the City of El Centro, El Centro Regional Medical Center (ECRMC), and UC San Diego Health today announced a strategic and operational plan to stabilize and financially bolster ECRMC.
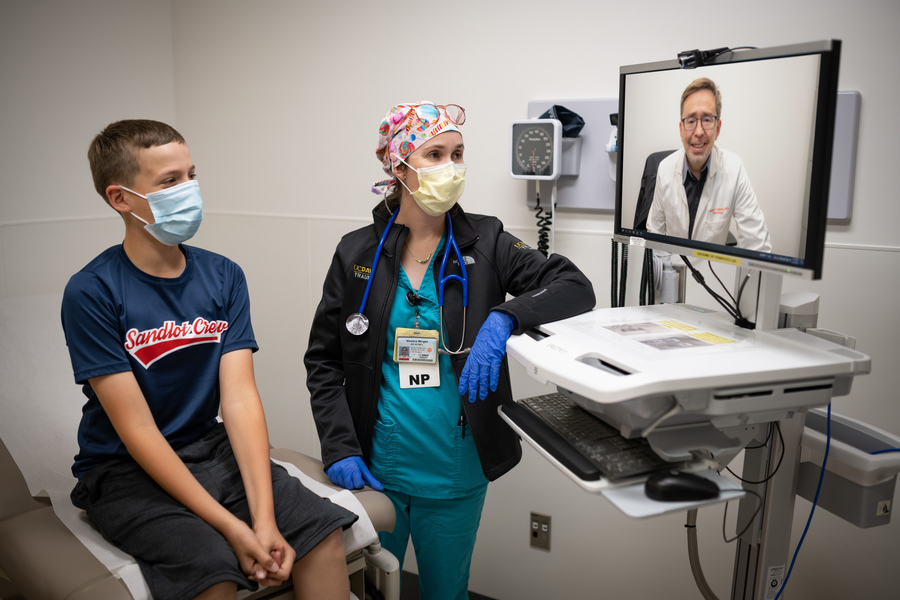
Telemedicine reduces hospital transfers for very ill kids at rural, community emergency departments
New UC Davis Health research confirms that pediatric critical care telemedicine consults with clinicians in rural and community emergency departments result in fewer hospital transfers.
Telemedicine Has Been ‘Hugely Beneficial’ for Health Care, Study Shows
Telemedicine and virtual appointments have become more popular in routine health and wellness since the COVID-19 pandemic began. Cal State Fullerton assistant professor of management David Cho co-authored a study examining the costs and benefits of these services. He notes that the…
For shared decision-making, telemedicine may be as effective as in-person appointments
Telemedicine may be just as effective as in-person visits when it comes to shared decision-making and communication for patients undergoing a first-time surgery consultation.
Telehealth cuts health care’s carbon footprint and patient’s costs during pandemic
UC Davis Health researchers assessed the carbon footprint and potential savings in lives, costs and time of telehealth visits during the pandemic’s first two years. They found that video visits in five UC health systems resulted in substantial savings in patient costs and carbon emissions.
Perspective: Audio Phone Visits with Medical Providers Remain Crucial Links to Delivering Equitable Health Care, Say Johns Hopkins Medicine Experts
Writing in the Nov. 17 issue of the New England Journal of Medicine, two telemedicine experts and a historian at Johns Hopkins Medicine say audio-only telephone visits are an essential link to health care providers for patients without access to video visit options.
Study Finds Automated Texts Decrease Odds of Rehospitalization
Text messages sent automatically from patients’ primary care office after hospitalization were tied to decreased odds of needing further emergency care
Study: During Pandemic, High Blood Pressure Control Declined
Hypertension control and management worsened during the early months of the COVID-19 pandemic, according to a new analysis conducted at three large health systems, led by Cedars-Sinai investigators.
Telemedicine reduces odds of no-show clinic visits by more than two-thirds for surgical patients
Surgical patients who use telehealth services are much more likely to show up for their initial clinic visit or follow-up appointment during the post-surgery period than those who rely on in-person visits only.
Fast Track to Fertility Program Sharply Cuts Time to Treatment
Telemedicine-driven program cut the time from an initial new patient visit to fertility treatment from more than two months to 41 days
Endocrine Society experts recommend individualized approach to use of telehealth
Following rapid growth during the COVID-19 pandemic, telehealth visits are expected to remain an important part of endocrine care, according to a new Endocrine Society policy perspective published in The Journal of Clinical Endocrinology & Metabolism.
CHOP Study Explores the Use of Telemedicine in Child Neurology in Largest Study to Date
Researchers found that across nearly 50,000 visits, patients continued to use telemedicine effectively even with the reopening of outpatient clinics a year after the onset of the COVID-19 pandemic. However, prominent barriers for socially vulnerable families and racial and ethnic minorities persist, suggesting more work is required to reach a wider population with telemedicine.
Global Health Panel Publishes New Research Highlighting Ambiguity in Digital Health-Related Definitions
Value in Health, the official journal of ISPOR, announced the publication of a new report examining digital health terms and their definitions from the perspective of their applicability for outcomes research.
Telehealth by phone & video proves a lifeline for veterans with opioid addiction
Phone-based and video-based telehealth visits both helped veterans with opioid addiction stay on buprenorphine medication to treat their opioid use disorder during the pandemic. The findings could inform telemedicine policy.
Study: Text Messaging Shows Promise in Reaching Unvaccinated Patients
While automated texting did not get more patients to get their vaccinations against COVID-19, it reached roughly the same amount as manned phone calls
Doctors across state borders: Telehealth study could inform policy
Under special interstate licensure rules, telehealth across state lines rose sharply from before the pandemic, a new study finds. But now that those rules have expired or will soon, the study could help guide those who will decide what happens next.

Study Evaluates How to Eliminate Telemedicine’s Virtual Waiting Room
UC San Diego Health conducted a 10-week study to evaluate how text messaging a link to patients when their doctor is ready provides a way to connect patients and doctors without relying on the virtual waiting room.
June 2022 Issue of Neurosurgical Focus: “Best Practice With Telemedicine for Optimizing Patient Care”
Announcement of contents of the June 2022 issue of Neurosurgical Focus
Telemedicine, continuous glucose monitoring mitigated effects of pandemic on children with diabetes
The rapid adoption of telemedicine and increased use of continuous glucose monitoring helped to attenuate the impacts of the COVID-19 pandemic on children with Type 1 diabetes, according to a new study from UT Southwestern researchers.
Racial Gap in Completed Doctor Visits Disappeared in 2020 as Telemedicine Adopted
As COVID-19 necessitated the wider adoption of telemedicine, the rate of completed primary care visits for Black patients rose to the same level of non-Black patients, Penn Medicine study finds
Penn Medicine, Philadelphia Department of Public Health Partner to Increase Virtual Care for Patients with Opioid Use Disorder
Through a collaboration, a virtual “bridge clinic” will expand access to more extensive and personalized care for patients struggling with opioid use
Home is where the hospital is
Hospital at home programs, and remote patient monitoring from home, hold promise for discharging patients earlier or keeping them out of the emergency room or hospital. But policy decisions will affect their future.
“Perfect for some but disastrous for others”: Patients and clinicians express concerns over phone and video consultations
A study of rheumatology patients and clinicians has found that while the majority found phone or video consultations more convenient than face-to-face consultations, they viewed so-called telemedicine as less diagnostically accurate than in-person consultations and as having the potential to increase health inequalities and barriers to accessing appropriate care.
Race, Age, Sex and Language Affected Telemedicine Use by Rheumatology Clinic Patients During COVID-19 Pandemic
New research presented this week at ACR Convergence, the American College of Rheumatology’s annual meeting, shows a significant lack of fairness among telemedicine and electronic patient portals used by rheumatology clinic patients based on their race, age, sex and English language proficiency.
Virtual lung cancer screening is just as effective as in-person screening
A novel telemedicine lung cancer screening effort during the COVID-19 pandemic shows that virtual single-visit screenings are just as effective as single-visit screenings done in person at the hospital.
Jefferson Launches Center for Connected Care
Plans national Consensus Conference on Research in Telehealth
UM School of Medicine Study Finds Mobile Telemedicine Unit as Effective as Traditional Clinics to Treat Opioid Addiction in Rural Areas
Rural regions in the U.S. have been disproportionately affected by the opioid epidemic, while also having the fewest number of programs to treat opioid use disorder.
Saving Lives in Black Barbershops
A new look at data from a landmark Cedars-Sinai study of health interventions in Black barbershops, and a new study that looks at barbershop patrons’ virtual visits with pharmacists, have added to the evidence that convenient, community-based health programs can cost-effectively control high blood pressure and prevent heart attack and stroke.
Masking, breakthrough infections and telehealth: Keck Medicine of USC experts on life after June 15
June 15 is a banner day in California. Most COVID-19 statewide restrictions will be eliminated, including physical distancing and in many situations, mask mandates. How will life change and how will it stay the same? Keck Medicine of USC experts weigh in on what to expect next in the golden state.
The Mount Sinai Hospital Recognized as No. 4 on Newsweek’s World’s Best Smart Hospital 2021 List
The Mount Sinai Hospital is ranked No. 1 in the New York City metropolitan area and No. 4 globally among the most technologically advanced health care institutions on Newsweek’s list of “The World’s Best Smart Hospitals 2021.”
Remote patient monitoring may reduce need to hospitalize cancer patients
ROCHESTER, Minn. — A study by researchers at Mayo Clinic Cancer Center has found that cancer patients diagnosed with COVID-19 who received care at home via remote patient monitoring were significantly less likely to require hospitalization for their illness, compared to cancer patients with COVID-19 who did not participate in the program. Results of the study were presented Friday, June 4, at the American Society of Clinical Oncology Annual Meeting and published in the Journal of Clinical Oncology.
When the Parking Lot Becomes a Health Clinic
The Free Clinic in Lubbock, Texas, came up with an innovative solution to continue to see patients who didn’t have access to the internet.
Disparities persisted as orthopaedic visits shifted to telemedicine
Like other medical specialties at the start of the COVID-19 pandemic, orthopaedic surgery rapidly pivoted from in-person visits to remote appointments via telemedicine. Analysis of that initial experience finds that some groups of patients faced persistent or worsening disparities as the shift to telemedicine occurred, reports Clinical Orthopaedics and Related Research® (CORR®), a publication of The Association of Bone and Joint Surgeons®. The journal is published in the Lippincott portfolio by Wolters Kluwer.
LEVERAGING TELEMEDICINE TO IMPROVE SKIN HEALTH AND WELLBEING FOR THOSE WHO ARE INCARCERATED
The American Academy of Dermatology (AAD) named board-certified dermatologist Jun Lu, MD, FAAD, and Tara Hood, FNP-BC, as Patient Care Heroes for using telemedicine to improve the health and well-being of women who have been incarcerated.

Story Tips from Johns Hopkins Experts on COVID-19
Coping with childhood anxiety amid returning to the classroom; new global tracker measures pandemic’s impact on education worldwide; Covid-19 drives innovation and evolution in patient care…
University Hospitals Chooses Visuwell as New Telehealth Provider
In order to better serve patients through access and convenience, University Hospitals (UH) has chosen Visuwell as its new principal telehealth vendor.
Rush Adds Telemedicine Management of DBS for Parkinson’s, Essential Tremor
First-of-its kind technology allows Rush doctors to remotely deliver a digital prescription for patients with brain stimulation therapy for Parkinson’s Disease and Essential Tremor.
Precision medicine, digital technology hold potential as powerful tools against tuberculosis
The global fight against tuberculosis is gaining some powerful tools. Precision medicine — already used to personalize diagnosis and treatment of noncommunicable diseases such as cancer — and health care technologies such as telemedicine have the potential to advance the prevention and treatment of tuberculosis, says Zelalem Temesgen, M.D., an infectious diseases expert and medical director of the Mayo Clinic Center for Tuberculosis.
Many endocrine patients, providers want to continue telehealth after pandemic
Two-thirds of patients with chronic endocrine health problems who need close monitoring say they would like to continue with telemedicine follow-up visits after the COVID-19 pandemic ends, according to a survey that will be presented virtually at ENDO 2021, the Endocrine Society’s annual meeting. Three-quarters of providers also said they want to continue with telehealth after the pandemic.