The U.S. Supreme Court has blocked the Sackler family’s bid for immunity from opioid-related lawsuits in a landmark decision. This ruling marks a pivotal moment in the ongoing opioid crisis, potentially reshaping how litigation against pharmaceutical companies is handled nationwide.
Tag: Opioid Addiction
It’s easier now to treat opioid addiction with medication — but use has changed little
In the first year after the sudden removal of a requirement that prescribers get special permission to prescribe medication for opioid addiction, a study finds more prescribers started providing it, but the number of patients receiving it didn’t rise very much.
New Addiction Treatment Research Receives Major Funding
Researchers at Huntsman Mental Health Institute at the University of Utah have been selected by Wellcome Leap to research an innovative ultrasound-based treatment for addiction as part of a $50 million commitment.
Do Prisons Hold the Key to Solving the Opioid Crisis?
Rutgers study finds improved prison reentry programs could help flatten the rate of opioid overdose deaths in the U.S.
Study Shows Differences in How Patients With Heroin Use Disorder Process Drug and Reward Cues
Findings may help inform the development of intervention and prevention strategies
Study: Treatment for opioid addiction lags despite policies designed to increase it
Treating opioid addiction should be much easier now than it was a few years ago, thanks to pandemic-era rule changes that aim to improve access to buprenorphine, a medicine proven to help in recovery. But a new study shows prescriptions and adherence rates have remained flat.
Millions with opioid addiction don’t receive residential treatment
First study to do apples-to-apples comparison of residential treatment use among Medicaid enrollees across several states
“Put profit margins aside,” says Saint Joseph’s University expert on Narcan over-the-counter approval by FDA
Narcan, a prescription nasal spray that reverses opioid overdoses, can now be sold over the counter after the FDA authorized the move on March 29. Peter A. Clark, S.J., PhD, is the director of the Institute of Bioethics and professor…
How AI Can Help Design Drugs to Treat Opioid Addiction
ROCKVILLE, MD – Approximately three million Americans suffer from opioid use disorder, and every year more than 80,000 Americans die from overdoses. Opioid drugs, such as heroin, fentanyl, oxycodone and morphine, activate opioid receptors. Activating mu-opioid receptors leads to pain relief and euphoria, but also physical dependence and decreased breathing, the latter leading to death in the case of drug overdose.
Outpatient Visits Are Critical to Success of Treating Opioid-Use Disorder, Researchers Find
Rutgers researchers find that patients in treatment for opioid use disorder are more likely to stay in treatment if they participate in multiple outpatient visits early in their care.
Telehealth by phone & video proves a lifeline for veterans with opioid addiction
Phone-based and video-based telehealth visits both helped veterans with opioid addiction stay on buprenorphine medication to treat their opioid use disorder during the pandemic. The findings could inform telemedicine policy.
Hepatitis C Infections Among Pregnant People Increased Substantially Between 2009 and 2019
The leading cause of HCV in the U.S. is injection drug use as a result of opioid use disorder (OUD), which has seen a rise in most populations, including pregnant people, in recent years. HCV rates have also risen. Between 2009 and 2019, the overall rate per 1,000 live births of HCV in pregnant people increased from 1.8 to 5.1.
Tulane scientists develop ‘living nerve circuit’ to fight opioid epidemic
Michael J. Moore, a professor of biomedical engineering at Tulane University School of Science and Engineering, is part of a national study that aims to turn around the statistics on opioid addiction.
UM School of Medicine Study Finds Mobile Telemedicine Unit as Effective as Traditional Clinics to Treat Opioid Addiction in Rural Areas
Rural regions in the U.S. have been disproportionately affected by the opioid epidemic, while also having the fewest number of programs to treat opioid use disorder.
Foundation for Opioid Response Efforts (FORE) to Release Results from National Survey of Peer Recovery Coaches at Webinar on Understanding and Bolstering the Recovery Workforce
The Foundation for Opioid Response Efforts (FORE) will host a webinar on Understanding and Bolstering the Recovery Workforce and release results from the qualitative portion of its first-ever national surgery of peer recovery coaches. The webinar will take place on Wednesday, July 14, 2021, from 3pm to 4:30pm EST.
New Diagnostic Method May Predict Relapse Risk for Those Recovering from Prescription Opioid Addiction
Rutgers scientists have used a diagnostic technique for the first time in the opioid addiction field that they believe has the potential to determine which opioid-addicted patients are more likely to relapse.
Rutgers Expert Available to Discuss New Loosened Restrictions for Prescribing Buprenorphine
Lewis Nelson, professor and chair of emergency medicine at the Rutgers New Jersey Medical School, is available to discuss the loosened restrictions in prescribing buprenorphine to treat opioid use disorder, an issue many physicians have advocated for to help reduce…
Two Novel Biobanks Offer Investigatory Targets for Cocaine and Oxycodone Addiction
Researchers have created to novel biobanks of diverse tissues from animals to further explore the biological bases and consequences of addiction to cocaine and oxycodone.
Researchers find large trade of opioids on the dark web
A string of opioid trade sites on the dark web have been uncovered by researchers with The University of Texas Health Science Center at Houston (UTHealth) School of Biomedical Informatics.

Initiative to Get COVID-19 Vaccines to People with Substance Use Disorder Launched by Addiction Policy Forum (APF) and Foundation for Opioid Response Efforts (FORE)
The Foundation for Opioid Response Efforts (FORE) and the Addiction Policy Forum (APF) are launching a program to assist people with substance use disorder obtain COVID-19 vaccinations.
Foundation for Opioid Response Efforts (FORE) Announces Grants Totaling $1.3 Million to Assess Impact of COVID-19 on Opioid Use Disorder Treatment and Equity
The coronavirus pandemic has led to several temporary regulatory relaxations and policy innovations in treatment for opioid use disorder aimed at making it easier for those seeking care to access treatment without risking in-person interactions. The Foundation for Opioid Response Efforts (FORE) today announced it is providing grants totaling $1.3 million to six organizations to assess the impact of these temporary measures and inform future policies to improve access and promote equity for the treatment of opioid use disorder.

Opioid overdose reduced in patients taking buprenorphine
The drug buprenorphine is an effective treatment for opioid use disorder, but many who misuse opioids also take benzodiazepines — drugs that treat anxiety and similar conditions. Many treatment centers hesitate to treat patients addicted to opioids who also take benzodiazepines. Researchers at Washington University School of Medicine in St. Louis studied overdose risk in people taking buprenorphine and found that the drug lowered risk, even in people taking benzodiazepines.
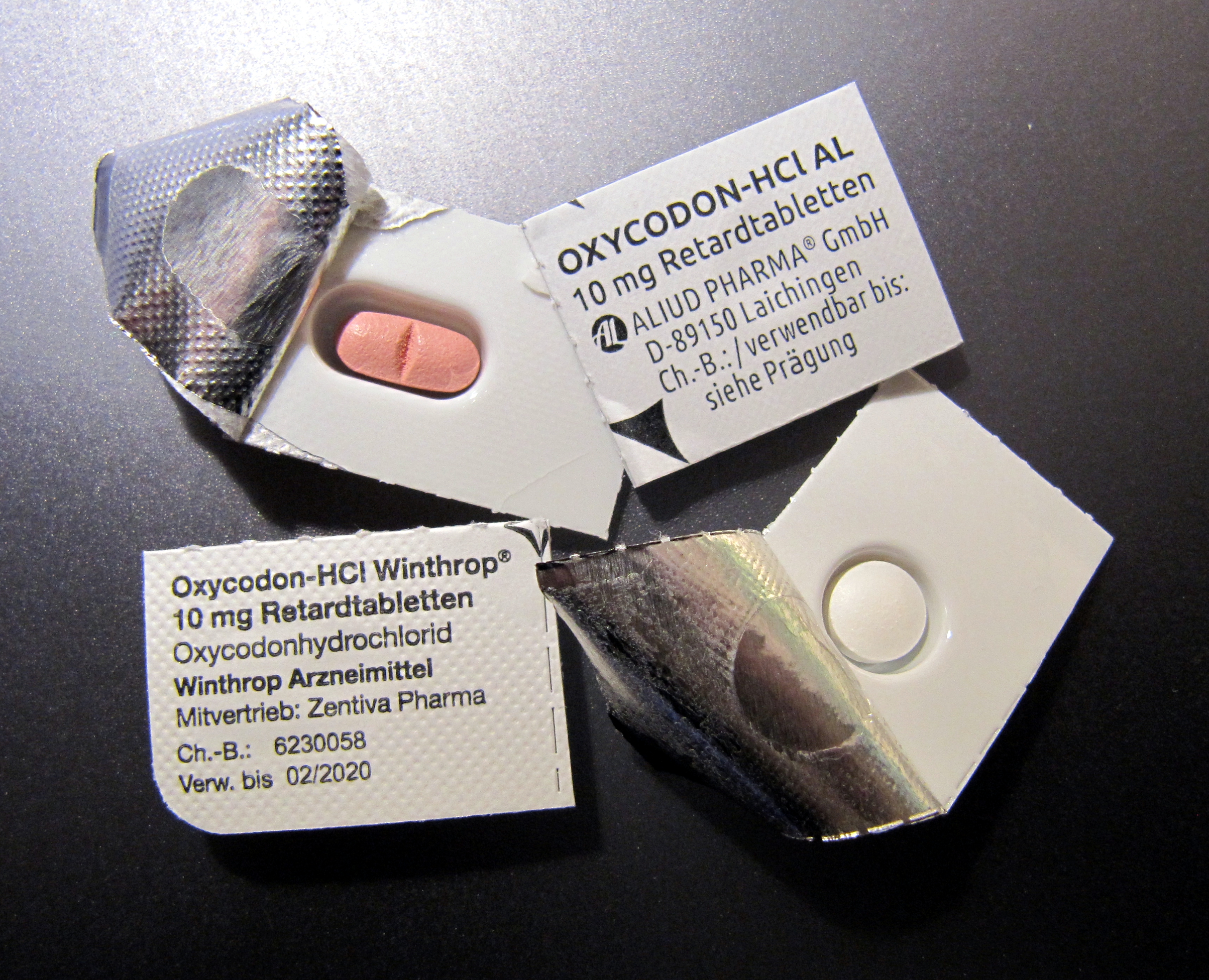
Mexico’s poor have little luck obtaining opioids intended for palliative care
Despite a Mexican government initiative launched in 2015 to improve access to prescription opioids among palliative care patients, the country has seen only a marginal increase in dispensing levels, and inequities in dispensing have left many of the nation’s poorest residents without comfort in their final days
Taking a scalpel to opioid painkiller risks: New surgery research shows progress and opportunities
A wave of new studies shows what happens when surgical teams work together to reduce the emphasis on, and supply of, opioid painkillers while still seeking to ease surgery patients’ pain.
Rutgers Experts Available to Discuss Purdue Pharma Guilty Plea
Rutgers emergency physician and opioid addiction experts are available to discuss Purdue Pharma’s guilty plea for its role in the nation’s opioid crisis. “This stark admission from Purdue Pharma demonstrates that it was a driving force for the nation’s opioid…

COVID poses hardships for people with substance abuse problems
FACULTY Q&ABoth fatal and nonfatal overdoses have increased this year compared to last, according to a recent report by the Overdose Data Mapping Application Program. And, anecdotal information suggests that compared to last year, people in recovery are relapsing at alarming rates.Faculty from the University of Michigan School of Nursing’s Center for the Study of Drugs, Alcohol, Smoking and Health discuss why the pandemic has hit people with substance abuse problems especially hard and the expanded role of virtual recovery programs.
Barriers to addiction care fell because of COVID-19, experts say; now the challenge is keeping them down
The opioid epidemic didn’t go away when the coronavirus pandemic began. But rapid changes in regulations and guidance could also help many more people get care for addiction, experts say. They caution that it will take more changes to truly lower barriers that stand in the way of delivering evidence-based addiction care to more people via telemedicine.

The Ethics of Ventilators During COVID-19
Diane Hoffmann is the Jacob A. France Professor of Health Law at University of Maryland School of Law where she directs the Law & Health Care Program and the Maryland Health Care Ethics Committee Network. She is able to speak…
Rutgers Expert Discusses How to Manage Chronic Pain, Opioid Addiction During COVID-19
Many people trying to manage their pain and addiction have lost their support programs due to COVID-19. A Rutgers expert in Emergency Medicine discusses how patients can manage the disease during the coronavirus crisis.
How our brains create breathing rhythm is unique to every breath
Breathing propels everything we do—so its rhythm must be carefully organized by our brain cells, right?
Wrong. Every breath we take arises from a disorderly group of neurons – each like a soloist belting out its song before uniting as a chorus to harmonize on a brand-new melody. Or, in this case, a fresh breath.
Medication Treatments Led to 80 Percent Lower Risk of Fatal Overdose for Patients with Opioid Use Disorder than Medication-free Treatments
Patients with opioid use disorder (OUD) receiving treatment with opioid agonists (medications such as methadone or buprenorphine) had an 80 percent lower risk of dying from an opioid overdose compared to patients in treatment without the use of medications.
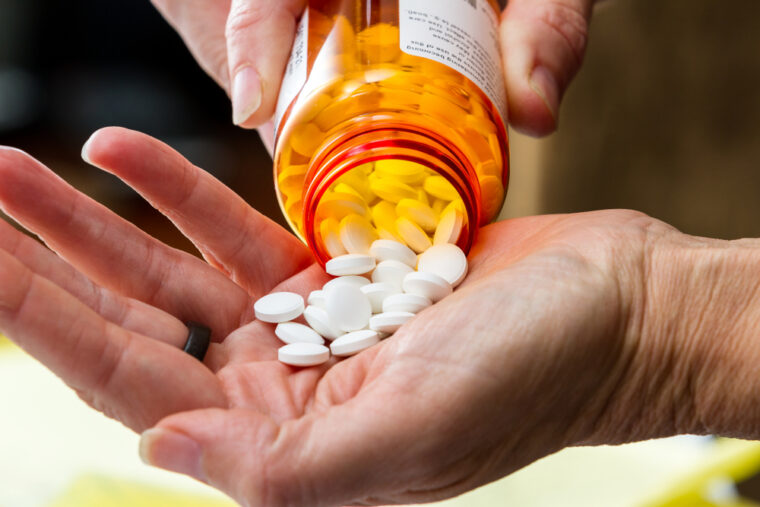
Battling treatment resistant opioid use disorder
Similar to treatment resistant depression, there is a subpopulation of those addicted to opioids who do not respond to standard opioid use disorder (OUD) treatments. In a new paper, an addiction expert at the Brown School at Washington University in St. Louis suggests a new category for these types of patients: treatment resistant opioid use disorder (TROUD).
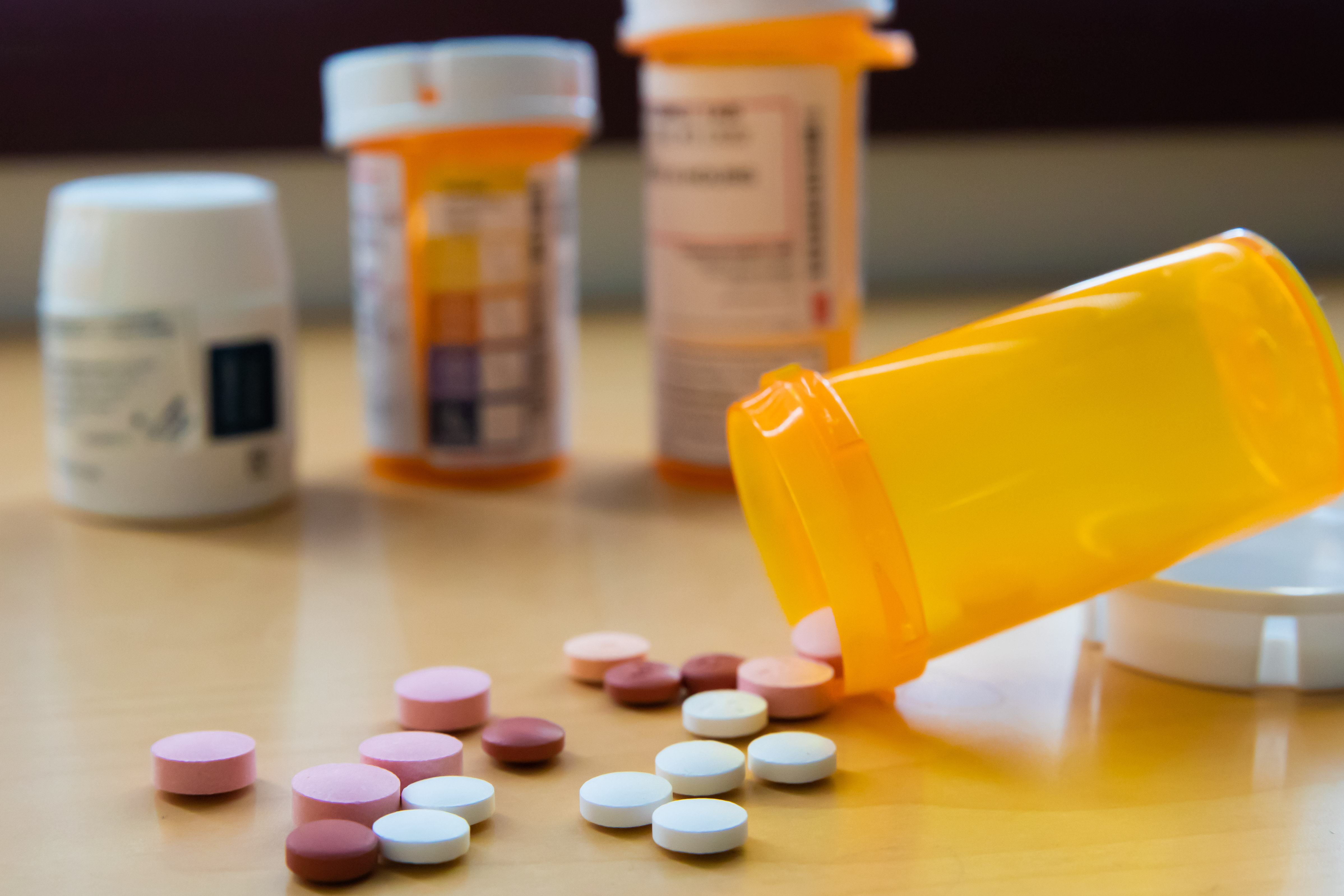
UCI researchers identify a connection between early life adversity and opioid addiction
Individuals with a history of early life adversity (ELA) are disproportionately prone to opioid addiction. A new UCI-led study reveals why.
Published in Molecular Psychiatry, the study titled, “On the early life origins of vulnerability to opioid addiction,” examines how early adversities interact with factors such as increased access to opioids to directly influence brain development and function, causing a higher potential for opioid addiction.
Opioid Dependence Found to Permanently Change Brains of Rats
Approximately one-quarter of patients who are prescribed opioids for chronic pain misuse them, with five to 10 percent developing an opioid use disorder or addiction. In a new study, UC San Diego researchers found that opioid dependence produced permanent changes in the brains of rats.

FAU and Georgia State Partner to Assist Children and Families Affected by Addiction
FAU and GSU have partnered on a program to assist children and families affected by addiction. They have received a $2.64 million grant from the U.S. Department of Health and Human Services for a program aimed at improving outcomes of Georgia’s children and families and strengthening the partnership between the Division of Family and Children Services and family treatment courts.

Tulane team researching ways to end opioid addiction
A Tulane University researcher is part of a nationwide initiative to improve treatment of chronic pain and ultimately achieve long-term recovery from opioid addiction.
Michael J. Moore, professor of biomedical engineering in the Tulane School of Science and Engineering, is part of a $945 million National Institutes of Health project called the HEAL Initiative, or Helping to End Addiction Long-term Initiative.
Mindfulness May Reduce Opioid Cravings, Study Finds
People suffering from opioid addiction and chronic pain may have fewer cravings and less pain if they use both mindfulness techniques and medication for opioid dependence, according to Rutgers and other researchers.
Designing a new class of drugs to treat chronic pain
A UC Davis research team, led by Vladimir Yarov-Yarovoy and Heike Wulff, will receive a $1.5 million grant from the National Institutes of Health (NIH) to develop a novel class of peptides that are better at treating pain and don’t have the side effects of opioids. The grant is part of the NIH initiative Helping to End Addiction Long-Term (HEAL Initiative).
Other treatments can reduce need for addictive pain medication
Hardly a day goes by without the public being warned about the dangers of opioids. But still, according to the National Institute on Drug Abuse, more than 130 people die every day of opioid overdose and the problem is getting worse. A Houston Methodist pain specialist says new advancements in pain management are giving patients options.

WashU Expert: Opioid cases represent tipping point in addiction fight
An Oklahoma judge ordered Johnson & Johnson to pay $572 million for its role in the opioid crisis in a historic ruling Aug. 26. A federal case in Ohio involves at least 1,600 lawsuits from cities and counties throughout the country. Oxycontin maker Purdue Pharma has offered to settle more than 2,000 lawsuits from states and cities for between $10 billion and $12 billion.

Aftermath of J&J ruling: Opioid expert available for comment
On Monday, an Oklahoma judge ruled Johnson & Johnson must more than half a billion dollars for its role in the state’s opioid crisis. Stefan Kertesz, M.D., an addiction scholar and professor at the University of Alabama at Birmingham School…

Professor says building socially responsible businesses will help women’s workforce participation, substance use recovery
A West Virginia University assistant professor wants to see the Mountain State increase women’s workforce participation, particularly women in substance use recovery. While Jenifer Gamble, field education director for West Virginia University’s School of Social Work and a United State of Women ambassador representing…