A target trial emulation study found that concomitant use of CYP2D6-metabolized opioids (hydrocodone, codeine, tramadol, and oxycodone) with antidepressants was associated with adverse outcomes among older nursing home residents.
Tag: Opioid
It’s easier now to treat opioid addiction with medication — but use has changed little
In the first year after the sudden removal of a requirement that prescribers get special permission to prescribe medication for opioid addiction, a study finds more prescribers started providing it, but the number of patients receiving it didn’t rise very much.
A New Study Shows How Neurochemicals Affect fMRI Readings
A landmark study, led by Yen-Yu Ian Shih, PhD, at the UNC School of Medicine, shows how neurochemicals can influence blood vessels. The new findings may alter how researchers interpret results from functional magnetic resonance imaging.
Geographic disparities in access to addiction treatment medication may be linked to race, ethnicity
Buprenorphine, a life-saving medication for opioid use disorder, is far less accessible in geographic areas of the United States with racially and ethnically diverse populations than in predominantly white areas, according to a new study of pre-pandemic data led by health policy scientists at the University of Pittsburgh School of Public Health published today in Journal of Addiction Medicine.
Homelessness leads to more drug, alcohol poisoning deaths
Reducing homelessness by 25% could save almost 2,000 lives lost to opioid overdoses, according to new research from the University of Georgia.
Stigma felt by opioid-dependent moms impacts the health care received by their babies
The rate of opioid use among pregnant women in the United States quadrupled between 1999 and 2014 and continues to rise — an alarming trend that researchers from the University of Missouri and University of Iowa say has exposed the stigma felt by opioid-dependent mothers and how their shame has negatively impacted the health care received by their infants.
Sylvester study shows how thoracic surgeons who treat lung cancer are helping to reduce patients’ risk of opioid dependence
Researchers at Sylvester Comprehensive Cancer Center found that robot-assisted surgeries and new patient-care protocols are enabling lung cancer surgery patients to go home earlier, with less pain and almost always without a need for potentially addictive opioids.
These Eight Habits Could Lengthen Your Life by Decades
A new study involving over 700,000 U.S. veterans reports that people who adopt eight healthy lifestyle habits by middle age can expect to live substantially longer than those with few or none of these habits.
NJ Medicaid Reforms Tied to Increased Use of Opioid Addiction Treatment
Rutgers study shows higher number of caregivers prescribing buprenorphine
Cerebral palsy patients at higher risk of receiving opioid prescriptions
Opioids are commonly prescribed as an all-purpose pain killer for patients with the condition
“Put profit margins aside,” says Saint Joseph’s University expert on Narcan over-the-counter approval by FDA
Narcan, a prescription nasal spray that reverses opioid overdoses, can now be sold over the counter after the FDA authorized the move on March 29. Peter A. Clark, S.J., PhD, is the director of the Institute of Bioethics and professor…
Pain management pathway reduces use of opioids after urethral repair surgery
For men undergoing surgery to repair scarring in the urethra (urethroplasty), a new approach to pain management can reduce the need for strong opioid drugs without compromising pain control, reports a study in Urology Practice®, an Official Journal of the American Urological Association (AUA). The journal is published in the Lippincott portfolio by Wolters Kluwer.
Expert alert: Anesthesiologists can discuss implications of new CDC opioid guidelines
The Centers for Disease Control and Prevention (CDC) yesterday released its long-awaited updated Guideline for Prescribing Opioids for Chronic Pain. The American Society of Anesthesiologists (ASA) and its members – who are experts in pain medicine and have led the…
‘Years of Life Lost’ to unintentional drug overdose in adolescents spikes during pandemic
COLUMBUS, Ohio – The first year of the COVID-19 pandemic saw a 113% increase in the “Years of Life Lost” among adolescents and young people in the United States due to unintentional drug overdose, according to researchers at The Ohio State University Wexner Medical Center and College of Medicine.
Duration of Preoperative Pain Linked to Chronic Opioid Use After Adult Spinal Deformity Surgery
In a Johns Hopkins Medicine study of patients who underwent adult spinal deformity (ASD) surgery, preoperative opioid use and pain duration of four or more years were independently associated with higher odds of chronic post-surgery opioid use.
Mouse study links changes in microbiome to prenatal opioid exposure
Prenatal exposure to opioids had been linked to a range of adverse outcomes in infants, including poor fetal growth, low birthweight, possible congenital defects and a higher risk of admission to neonatal intensive care. Less information is known, however, on how developmental opioid exposure shapes an infant’s microbiome and how that influence, in turn, may trigger neurological or behavioral effects later in life.
How the Pandemic Limited Access to Opioid Addiction Treatment for Racial and Ethnic Minority Groups
Members of racial and ethnic minority groups were less likely to obtain prescriptions to treat opioid addiction during the COVID-19 pandemic, according to a study by researchers at Rutgers and Indiana University.
New Drugs with High Abuse Potential More Likely to Be Approved, Go to Market to Treat Pain
CHICAGO – “Despite the prevalence and societal costs of pain in the United States, investment in pain medication development is low, due in part to poor understanding of the probability of successful development of such medications,” said the authors of a study published Online First in Anesthesiology, the official peer-reviewed journal of the American Society of Anesthesiologists (ASA).
Disparities in opioid treatment access remain for women, Black and Hispanic people
Buprenorphine is a prescription approved by the Food and Drug Administration (FDA) that effectively treats opioid dependence or addiction. But women, as well as Black and Hispanic populations, do not have equal access to this potentially lifesaving medication, new Mayo Clinic research finds.
UCLA neuroscientists use electrical stimulation to restore breathing in surgery patients undergoing opioid-based anesthesia
New UCLA research published in The Journal of Physiology points to a novel treatment for respiratory depression associated with opioid use that administers electrical pulses to the back of the neck, helping patients regain respiratory control following high dosage opioid use. This could offer an alternative to pharmacological treatments, which can cause withdrawal symptoms, heart problems and can negatively affect the central nervous system.
Diverted Buprenorphine May Help Prepare People With Opioid-Use Disorder for Treatment
New research finds people who were using buprenorphine obtained without a prescription were more likely to remain in treatment for opioid-use disorder, underscoring need to expand access to this medication.
Study: Treatment Minimizes Infants’ Opioid-Related Brain Abnormalities
Treating pregnant women with opioid use disorder can help minimize opioid-related brain abnormalities in their newborns. Led by scientists at Cedars-Sinai, this is the first study to report evidence validating the benefits of using medication for opioid use disorder during pregnancy.
Medication that lowers risk of overdose underused
Researchers at Washington University School of Medicine in St. Louis and Saint Louis University found that less than half of Americans who received treatment for opioid use disorder over a five-year period were offered a potentially lifesaving medication. The numbers were even lower for those with what’s known as polysubstance use disorder — when opioid users also misuse other substances.
Study Finds Duloxetine Added to Multimodal Pain Management Reduced Opioid Use After Knee Replacement
A study by researchers at Hospital for Special Surgery (HSS) found that the antidepressant duloxetine reduced the use of opioid medication when added to a multimodal pain management regimen after knee replacement surgery. The study appeared in The Journal of Arthroplasty.
Just over half of Michigan pharmacies offer overdose-fighting naloxone without prescription
Despite the ability of any Michigan pharmacy to dispense medication to combat opioid overdose without writing prescriptions, slightly more than half of pharmacies in the state offer the drug in such a way.
Tulane scientists develop ‘living nerve circuit’ to fight opioid epidemic
Michael J. Moore, a professor of biomedical engineering at Tulane University School of Science and Engineering, is part of a national study that aims to turn around the statistics on opioid addiction.
Patient-Centered Protocols Help Eliminate Excess Opioid Use after Lung Surgery
Lung surgery patients who utilize a comprehensive, evidence-based enhanced recovery after surgery (ERAS) program require fewer opioid prescriptions when discharged and this effect was sustained over the 4-year study period.
University of Kentucky Law Expert Available to Address Recent Proposed National Opioid Settlements with Drug Companies
Richard Ausness is a product liability expert and the Stites and Harbison Professor of Law at the University of Kentucky J. David Rosenberg College of Law. He currently teaches Property, Trusts & Estates and Products Liability. His other teaching interests…
Hackensack Meridian School of Medicine and Seton Hall University Opioid Conference to Feature Addiction Experts Working to Combat National Crisis
The July 30 virtual conference is part of a three-year grant to train clinicians to prescribe medications to treat addiction.
People With Back Pain Miss Far Fewer Workdays When They Receive Recommended Treatments
Medical guidelines help doctors understand the best way to treat health conditions. Surprisingly, many doctors do not adhere to them, and this is a problem, according to a new study. People with lower back pain injury miss 11 more days of work in a year when they only receive treatments for lower back pain that are not recommended by medical guidelines compared to people treated according to guidelines.
A treatment barrier falls, but more remain, for people with opioid issues
Now that a key policy regarding prescription of a medication for opioid use disorder has been changed, experts reflect on the remaining challenges standing in the way of more people getting effective medication-assisted treatment, and discuss efforts to overcome those barriers.

Guideline for reducing opioid use post-surgery leads to high pain management satisfaction and disposal rates
A prescribing guideline tailored to patients’ specific needs reduced the number of opioid pills prescribed after major surgery.
Three Longtime Antibiotics Could Offer Alternative to Addictive Opioid Pain Relievers
DALLAS – Feb. 22, 2021 – Three decades-old antibiotics administered together can block a type of pain triggered by nerve damage in an animal model, UT Southwestern researchers report. The finding, published online today in PNAS, could offer an alternative to opioid-based painkillers, addictive prescription medications that are responsible for an epidemic of abuse in the U.S.

Modified pain management strategy reduces opioid exposure to trauma patients, study shows
A pain management regimen comprised mostly of over-the-counter medication reduced opioid exposure in trauma patients while achieving equal levels of pain control, according to a new study by physician-researchers at UTHealth.
Opioid Use Can Trigger Deafness
Opioid receptors in the inner ear can cause partial or full hearing loss, says Rutgers study
Negative side effects of opioids could be coming from users’ own immune systems (video)
Opioid users can develop chronic inflammation and heightened pain sensitivity. These side effects might stem from the body’s own immune system, which can make antibodies against the drugs. The researchers will present their results at the American Chemical Society Fall 2020 Virtual Meeting & Expo.

Traditional PTSD Therapy Doesn’t Trigger Drug Relapse
Johns Hopkins researchers have demonstrated that behavior therapy that exposes people to memories of their trauma doesn’t cause relapses of opioid or other drug use, and that PTSD severity and emotional problems have decreased after the first therapy session.
Follow-up Treatments After Opioid Overdose Rare Among Insured Patients
Of nearly 6,500 commercially insured patients treated in EDs nationwide for an overdose or other opioid-related medical complications, only 16 percent accessed opioid use disorder (OUD) medications or another form of treatment within three months of the ED visit.
Sedative Drug in Combination with Opioids May Be Especially Dangerous
• In an analysis of information on US adults initiating hemodialysis, 16% of patients were dispensed a short-acting benzodiazepine, and approximately one-quarter of these patients were also dispensed opioids.
• Among patients with an opioid prescription, being dispensed a short-acting benzodiazepine had a 1.9-fold higher risk of dying over a median follow-up of 16 months compared with patients without a short-acting benzodiazepine.
Rutgers Expert Discusses How to Manage Chronic Pain, Opioid Addiction During COVID-19
Many people trying to manage their pain and addiction have lost their support programs due to COVID-19. A Rutgers expert in Emergency Medicine discusses how patients can manage the disease during the coronavirus crisis.
Anterior insula activation restores prosocial behavior in animal model of opioid addiction
Researchers in the Arizona State University Department of Psychology have shown that chemogenetic activation of the anterior insula restores prosocial behavior in an animal model of opioid addiction and empathy. The findings suggest an important role for the anterior insula in the brain response to addiction.

Saint Louis University Forms Missouri’s First Addiction Medicine Fellowship
Saint Louis University School of Medicine is tackling the country’s opioid abuse crisis by training community physicians to recognize and treat addictions.
Second phase of massive opioid lawsuit announced; case is ‘bellwether’ for thousands of similar cases nationwide, says CWRU law professor Andrew Pollis
The massive multidistrict litigation over the nation’s opioid crisis recently reached its conclusion with a $260 million settlement with drug manufacturers. Now, the second phase— focusing on the pharmacy industry’s role in the opioid epidemic—is slated to begin. “This is…
Gaps Remain in Rural Opioid Crisis Research
Rural areas have been hit hard by the opioid crisis, but few studies have been done to understand how to improve access to treatment and reduce the overdose death rate in these communities, according to a new study by Rutgers University, the University of Michigan, and Wayne State University.
Press registration now open for 2020 Experimental Biology meeting
Complimentary press passes and virtual newsroom access are now available for the Experimental Biology (EB) 2020 meeting, to be held April 4–7 in San Diego.
This drug could save their lives, but less than 2% of them get it
Only a tiny minority of people at risk for an opioid overdose actually are prescribed a drug that could save their lives, a new study suggests. And the odds of having a dose of the rescue drug were very low among some of the most at-risk groups, including those who had already survived a previous opioid overdose.

Research shows nasal spray antidote is easiest to give for opioid overdose
Of three possible ways for people to deliver the life-saving antidote naloxone to a person experiencing an opioid overdose, the use of a nasal spray was the quickest and easiest according to research conducted by William Eggleston, clinical assistant professor at Binghamton University, State University of New York, and colleagues at SUNY Upstate Medical University.
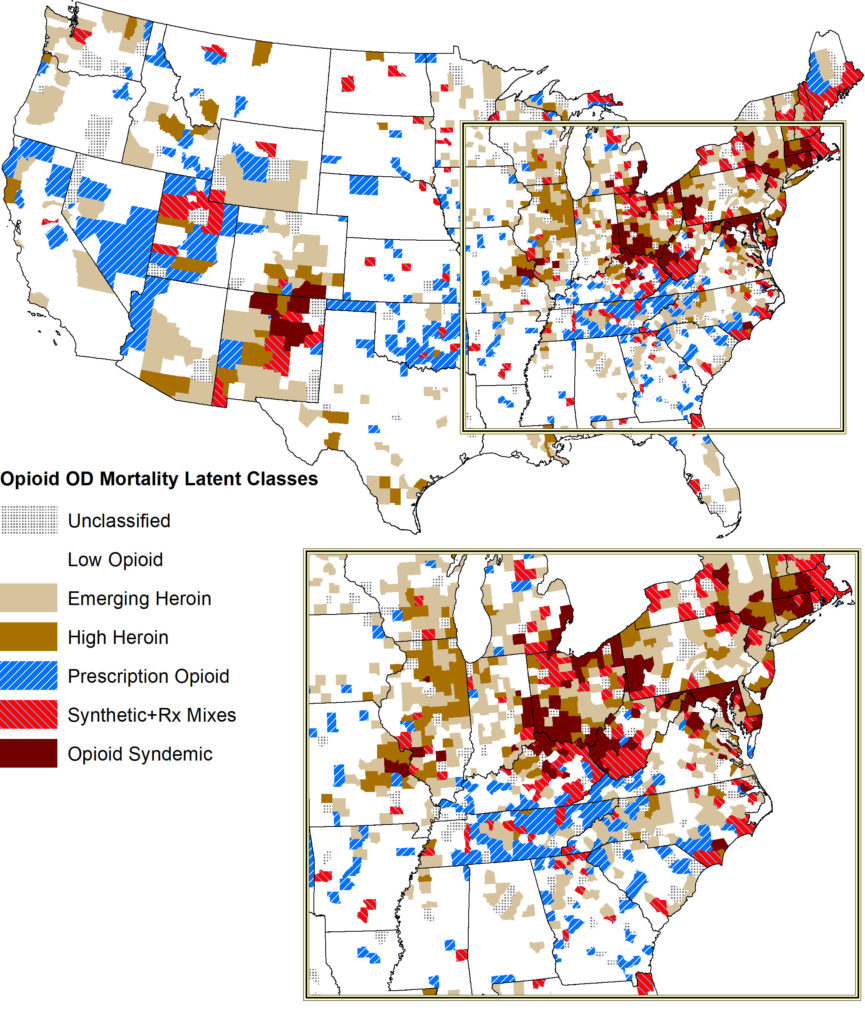
Regional trends in overdose deaths reveal multiple opioid epidemics, according to new study
A recently published study shows the United States in the grip of several simultaneously occurring opioid epidemics, rather than just a single crisis. The epidemics came to light after the researchers analyzed county-level data on drug overdose deaths. The study highlights the importance of different policy responses to the epidemics rather than a single set of policies.
A Person’s Perception of Risk Can Tell Us About Their Chances of Opioid Relapse
People in treatment for opioid addiction are more likely to relapse when they become more tolerant of risks, according to a study by Rutgers and other institutions. The findings can help clinicians better predict which patients are most vulnerable.
Computer Game May Help to Predict Reuse of Opioids
A computer betting game can help predict the likelihood that someone recovering from opioid addiction will reuse the pain-relieving drugs, a new study shows.