A systematic review and retrospective individual participant-level meta-analysis of 18 trials comprised of more than 1,700 participants found that initiating treatment with an angiotensin-converting enzyme inhibitor (ACEi) or angiotensin-receptor blocker (ARB) protects against kidney failure in patients with advanced chronic kidney disease (CKD).
Tag: Kidney Failure
INCREASING ORGAN TRANSPLANT ACCESS (IOTA) MODEL ANNOUNCED TO INCREASE PATIENT ACCESS TO KIDNEY TRANSPLANTATION
The long-awaited Increasing Organ Transplant Access (IOTA) Model was released yesterday by the Center for Medicare and Medicaid Innovation (CMMI) focusing on increasing patients’ access to kidney transplantation across the United States.
New device can treat injury from sepsis
Therapeutic tool used for children with kidney issues stemming from sepsis
Resistant Starch Could Help Combat Leading Cause of End-stage Kidney Failure
Combining a low dose of blood pressure medication with a higher intake of dietary-resistant starch might help stave off diabetic kidney disease, according to results from a new animal study. Researchers will present their work this week at the American Physiology Summit.
Even lower levels of albuminuria associated with increased risk for CKD progression and kidney failure
A study of patients with chronic kidney disease (CKD) found substantial excess risk for CKD progression and kidney failure as albuminuria (protein in the urine) increased even at levels below 30 mg/g.
Patients With Obesity and Kidney Failure May Be Newly Eligible for Kidney Transplants
A collaborative study between a bariatric and transplant surgery team has introduced new hope for patients suffering from end-stage renal disease (ESRD) who are also struggling with obesity. The study authors explored the outcomes of metabolic and bariatric surgery in ESRD patients and whether the surgery can improve their eligibility for kidney transplants. The findings are published in the Journal of the American College of Surgeons (JACS).
AMERICAN SOCIETY OF NEPHROLOGY COMMENDS CONGRESS FOR HIGHLIGHTING THE HONOR OUR LIVING DONORS ACT (H.R. 6020)
At a hearing today focused on supporting patients with rare diseases, the House Energy and Commerce Health Subcommittee will consider Honor Our Living Donors Act (H.R. 6020), legislation to improve support for living organ donors.

New Cedars-Sinai Study Pinpoints Why Some Injured Kidneys Do Not Heal
Cedars-Sinai investigators have discovered why some injured kidneys heal while others develop scarring that can lead to kidney failure. Their findings, detailed in a paper published in the peer-reviewed journal Science, could lead to the development of noninvasive tests to detect kidney scarring and, eventually, new therapies to reverse the condition.

Despite social media claims, Borax is not safe to consume
A nephrologist explains the damage that this trend can cause
Major step forward reduces mortality in kidney failure patients
Mortality in patients with kidney failure has been found to be 23% lower among those treated with high dose haemodiafiltration compared to those treated with high flux haemodialysis, according to new research from the CONVINCE consortium led by University Medical Center Utrecht.
Growing number of states provide coverage for outpatient hemodialysis for undocumented immigrants
A brief research report has found that, due to increased advocacy and awareness of outcomes, a growing number of states have implemented policies that provide statewide coverage for undocumented persons with kidney failure to receive outpatient hemodialysis. The report is published in Annals of Internal Medicine.
Researchers find new pathway to prevent kidney failure for thousands
Researchers at the University of Bristol have made a breakthrough that could prevent certain kidney patients progressing towards renal failure.

Three Kidney Transplants, Weight Gain and a Journey Back to Wellness
Rowena Roque, 46, was having a problem that many people can relate to: doing everything in her power to lose weight and get healthy but never succeeding.
Podocyte Protectors: NIH Awards CHLA’s GOFARR Laboratory Additional Grants to Combat Chronic Childhood Kidney Disease
CHLA has received a new five-year award of $3.2 million from the National Institutes of Health (NIH) to research the underlying mechanisms that lead to kidney failure and to develop new treatments to protect kidney function.
Researchers examine what happens when patients can choose concurrent dialysis and hospice care
Today, patients utilizing their Medicare Hospice Benefits with end-stage kidney disease (ESKD) are forced to make the traumatic choice between continuing dialysis or enrolling in hospice.
AMERICAN SOCIETY OF NEPHROLOGY STRONGLY SUPPORTS CONGRESSIONAL OVERSIGHT OF TRANSPLANT SYSTEM
The American Society of Nephrology (ASN) supports efforts by Congress to improve the US transplant system. Today, the Senate Finance Committee will conduct an oversight hearing, A System in Need of Repair: Addressing Organizational Failures of the U.S.’s Organ Procurement and Transplantation Network (OPTN).
Combining Melatonin with Vancomycin Reduces Kidney Failure
A study by researchers at the Rutgers Ernest Mario School of Pharmacy finds that melatonin significantly reduces kidney failure in people being treated with the antibiotic vancomycin.
Do family members understand the end-of-life wishes of patients on chronic dialysis?
Most surveyed family members of patients with kidney failure on long-term dialysis reported they had spoken with the patient about their end-of-life wishes but not about stopping dialysis or initiating hospice.
Is “Patient Activation Measure” Relevant for Adults on Dialysis?
• The Patient Activation Measure describes an individual’s knowledge, ability, skills, and confidence in self-managing chronic conditions.
• A recent study examined the measure’s relevance for patients with kidney failure who are undergoing long-term dialysis.
Artificial Pancreas Trialled for Outpatients with Type 2 Diabetes for First Time
An artificial pancreas could soon help people living with type 2 diabetes and who also require kidney dialysis.
New Score Measures Health-Related Quality of Life in Patients with Kidney Failure
Highlights
• The results of a new study support the validity of a score that considers various patient-reported outcome measures and preferences for assessing health-related quality of life in individuals with kidney failure.
• The score is calculated from assessments of cognitive function, depression, fatigue, pain interference, physical functioning, sleep disturbance, and ability to participate in social roles
For Individuals Undergoing Dialysis, More Frequent Visits with Kidney Specialists Does Not Improve Patient-Reported Experiences
• Patients with kidney failure did not report better experience with care from more frequent face-to-face visits with kidney specialists at dialysis facilities.
• In fact, more frequent visits were linked with slightly lower patient-reported experiences with kidney-related care.
Newly discovered proteins provide protection against progression of kidney disease in diabetes
Elevated levels of three specific circulating proteins are associated with protection against kidney failure in diabetes, according to research from the Joslin Diabetes Center in Boston.
Disparities in COVID-19 Rates among Adults with Kidney Failure in New York City
• Among adults with kidney failure undergoing hemodialysis in New York City, Black and Hispanic patients were more likely to develop symptomatic COVID-19 than White patients.
• Neighborhood-level social vulnerability factors were associated with COVID-19 incidence among White patients, but these factors did not explain racial/ethnic disparities.
Aerobic Exercise May Help Address Dialysis-Related Symptoms in Patients with Kidney Failure
• An analysis of published clinical trials suggests that aerobic exercise lessens several hemodialysis-related symptoms, including restless leg syndrome, symptoms of depression, muscle cramping, and fatigue.
• More research, with more diverse patients, is needed to determine the extent of benefits from aerobic exercise for individuals with kidney failure who are undergoing dialysis.
Patients with Sickle Cell–Related Kidney Failure Benefit from Transplants But Are Less Likely to Receive Them
• Patients with kidney failure associated with sickle cell disease benefit from kidney transplants, but they’re less likely than other patients to receive them.
Overlooked Cilium Could Be Genetic Key to Common Diseases
Long thought a vestigial part of human cells, new genetic analysis of the primary cilium shows that it may be tied to common conditions like diabetes and kidney failure
Cincinnati Children’s Uses New Device to Help Critically Ill Infants with Kidney Failure
The Cardio-Renal Pediatric Dialysis Emergency Machine (CARPEDIEM) is a new system for patients with acute kidney injury or kidney failure requiring dialysis. This ground-breaking technology is intended to provide continuous renal replacement therapy (CRRT) to patients weighing between 5 and 20 pounds.
AMERICAN SOCIETY OF NEPHROLOGY CALLS ON BIDEN- HARRIS ADMINISTRATION TO INCREASE TRANSPLANT AVAILABILITY AND EQUITY
— The American Society of Nephrology (ASN) re- affirms its supporti for the Organ Procurement Organizations (OPOs) Conditions for Coverage final rule issued on November 20, 2020. The society calls for the Biden-Harris administration to implement this final policy as expediently as possible. By bringing objective and verifiable standards to assess the performance of OPOs, this final rule will increase the number of organs available for transplant and reduce racial inequity in the U.S. transplant system.
Study Finds Patients with Kidney Failure Are Ready and Willing to Use Mobile Health
• In a survey of adults with kidney failure who were receiving dialysis, most owned mobile devices and had intermediate or advanced mobile health proficiency.
• The main reasons for using mobile health were for making appointments, communicating with healthcare personnel, and obtaining laboratory results.
Baylor Scott & White Medical Center – Temple Performs 1000th HoLEP Procedure That Improves Men’s Quality of Life
In mid-October, Baylor Scott & White Medical Center – Temple conducted its 1000th holmium laser enucleation of the prostate (HoLEP), a minimally invasive procedure that can address benign prostatic hyperplasia (BPH). BPH can prevent the bladder from emptying properly and could lead to kidney damage or failure. It also impacts quality of life in about one third of men older than 50 years old.
Do Accountable Care Organizations Reduce Kidney Failure–Related Healthcare Costs?
• A recent analysis indicates that Accountable Care Organizations may reduce the cost of medical care for patients undergoing dialysis.
• The cost savings were seen only for patients who regularly received care from primary care physicians.
Depression Screening Tools in Patients with Kidney Failure
• A recent analysis found limited research evaluating depression screening tools in patients with kidney failure.
• Many studies were small in size and had other shortcomings.
Patients With COVID-19 May Have Higher Risk of Kidney Injury
According to Jochen Reiser, MD, PhD, the Ralph C Brown MD professor and chairperson of Rush’s Department of Internal Medicine, patients with COVID-19 experience elevated levels of soluble urokinase receptor (suPAR), an immune-derived pathogenic protein that is strongly predictive of kidney injury.
Kidney Problems as a Young Adult May Affect Thinking Skills in Midlife
If you have moderate-to-high risk of kidney failure as a young adult, you may be at risk for worse cognitive function in middle age, according to a study published in the September 2, 2020, online issue of Neurology®, the medical journal of the American Academy of Neurology.
Blocking brain signals detected in the kidney could help unlock future treatments for kidney failure, heart disease, and stroke
Scientists have discovered an important cell signalling pathway in the kidney which if stopped, could hold the key to treating chronic kidney disease as well as other deadly conditions, including heart attack and stroke.
Many Patients with Kidney Failure Regret Initiating Dialysis
• In a study of adults with kidney failure treated with dialysis, 21% of patients reported regret that they decided to initiate dialysis.
Certain factors were linked with a higher likelihood of experiencing regret
KIDNEY HEALTH INITIATIVE URGES THE ACCELERATION OF HOME THERAPY TECHNOLOGY IN RESPONSE TO CORONAVIRUS 2019 (COVID-19)
The COVID-19 pandemic highlights the vulnerability of people with kidney failure who rely on in-center hemodialysis. People with kidney failure are at high risk of severe COVID-19 complications and are exposed to infection due to a kidney replacement therapy process that requires traveling to a dialysis facility multiple times a week.
Sedative Drug in Combination with Opioids May Be Especially Dangerous
• In an analysis of information on US adults initiating hemodialysis, 16% of patients were dispensed a short-acting benzodiazepine, and approximately one-quarter of these patients were also dispensed opioids.
• Among patients with an opioid prescription, being dispensed a short-acting benzodiazepine had a 1.9-fold higher risk of dying over a median follow-up of 16 months compared with patients without a short-acting benzodiazepine.
Reducing Kidney Failure Rate Among Patients with Diabetic Kidney Disease
Now, as part of an effort to reduce the rate of patients with diabetic kidney disease who develop kidney failure, researchers at Penn Medicine are spearheading a collaboration to better understand the progression of DKD and advance research aimed at preserving kidney function in these patients.
HOUSE ENERGY AND COMMERCE COMMITTEE HOLDS HEARING ON IMMUNOSUPPRESSIVE DRUG COVERAGE, A KEY LEGISLATIVE PRIORITY OF AMERICAN SOCIETY OF NEPHROLOGY
Washington, DC (January 8, 2020) — The House Energy and Commerce Committee is scheduled to hold a hearing on Wednesday, January 8, on the Comprehensive Immunosuppressive Drug Coverage for Kidney Transplant Patients Act of 2019, advancing a long-standing legislative priority of the American Society of Nephrology.
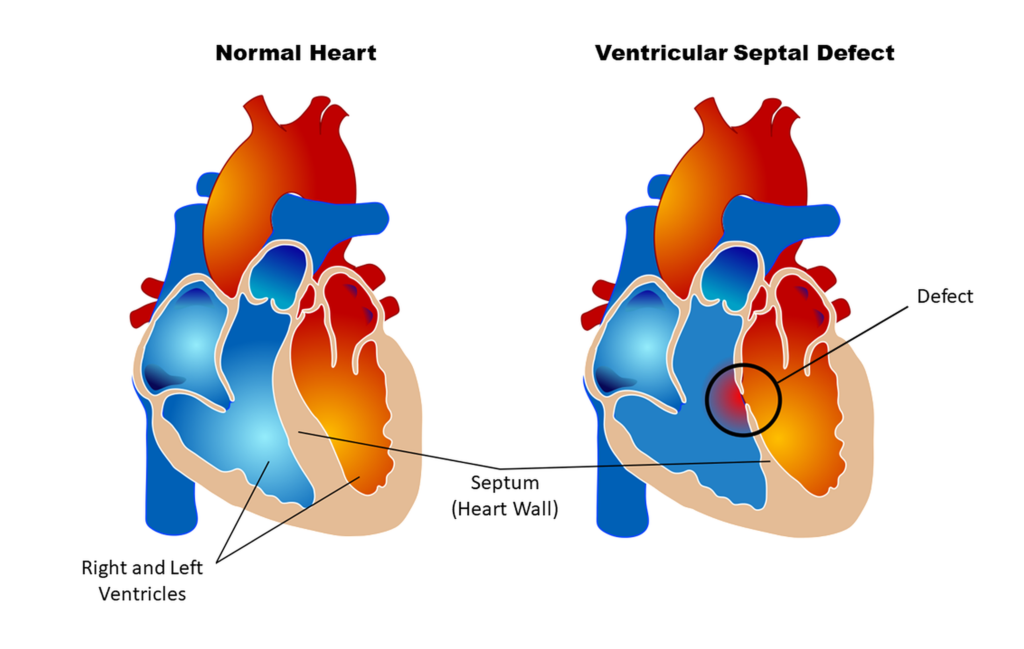
Careful Monitoring of Children Following Cardiac Surgery May Improve Long-Term Outcomes
In a medical records study covering thousands of children, a U.S.-Canadian team led by researchers at Johns Hopkins Medicine concludes that while surgery to correct congenital heart disease (CHD) within 10 years after birth may restore young hearts to healthy function, it also may be associated with an increased risk of death and kidney failure within a few months or years after surgery.