Combining a low dose of blood pressure medication with a higher intake of dietary-resistant starch might help stave off diabetic kidney disease, according to results from a new animal study. Researchers will present their work this week at the American Physiology Summit.
Tag: Type 1 Diabetes

Pancreas Cells in People Who Have Died Show Significant Signs of Stress
Rockville, Md. (April 1, 2024)—People with Type 1 diabetes require daily insulin shots to regulate their blood sugar levels. This is because their immune system kills beta cells found in islets in the pancreas. Beta cells release and disburse insulin…
Endocrine Society celebrates extension of Special Diabetes Program
The Endocrine Society applauds Congress for approving the first funding increase for the Special Diabetes Program in two decades.
Shifting focus: Investigators describe changes to pancreatic β cell at onset of Type 1 Diabetes
About eight million people live with Type 1 diabetes (T1D) worldwide, a chronic autoimmune condition in which the body attacks and destroys its own insulin-producing β-cells (pronounced “beta”) in the pancreas, leading to a lack of insulin and inability to regulate blood sugar. It’s not known why the body suddenly perceives its own β-cells as the enemy; some lines of evidence suggest environmental factors such as viral infections may trigger the onset of T1D, others suggest genetics may also play some role.
Groundbreaking research by investigators at Joslin Diabetes Center sheds new light on the specific changes β-cells go through at the onset of T1D. Their findings—published in Nature Cell Biology—offer new avenues for targeted interventions for the chronic autoimmune condition.

High out-of-pocket costs hindering treatment of diabetes
Diabetes care providers should account for impacts caused by financial insecurity, researchers suggest

Study links small pancreas size to faster progression to stage 3 Type 1 diabetes
A multicenter, longitudinal study, co-led by investigators at the Vanderbilt Diabetes Research and Training Center (DRTC), has discovered that a small pancreas size predicts a faster progression to stage 3 Type 1 diabetes (T1D), the point at which clinical diagnosis occurs.
Almost 4 in 10 adults with type 1 diabetes are not diagnosed until after age 30
A brief research report including more than 900 adults with type 1 diabetes found that 37 percent, or nearly 4 in 10 participants, were diagnosed with type 1 diabetes after age 30. Age of diagnosis was higher for men and racial minority adults. The findings are published in Annals of Internal Medicine.
VUMC receives $28 million to lead national study of COVID-diabetes link
Researchers at Vanderbilt University Medical Center have received a four-year, $28 million grant from the National Institute of Diabetes and Digestive and Kidney Diseases, part of the National Institutes of Health, to study the relationship between COVID-19 and diabetes.
NIH awards $3M to Wayne State to impact Black youth with type 1 diabetes
A Wayne State University School of Medicine professor has received a $3 million award from the National Institute on Minority Health and Health Disparities of the National Institutes of Health to develop an intervention aimed at improving health outcomes in Black youth with type 1 diabetes.
Closed-loop insulin delivery systems may improve blood sugar control in children with type 1 diabetes
Closed-loop insulin delivery systems improve glucose control in children with type 1 diabetes without causing adverse effects, according to a study presented Saturday at ENDO 2023, the Endocrine Society’s annual meeting in Chicago, Ill.
CGM alarms often not set to alert children with diabetes to harmful blood glucose fluctuations
Children and teenagers who use continuous glucose monitors (CGM) to manage diabetes often fail to use the appropriate alarm settings to alert to dangerously low or harmful high blood sugar levels, according to a study being presented Thursday at ENDO 2023, the Endocrine Society’s annual meeting in Chicago, Ill. This variability makes the monitors less useful in tracking glucose levels.
Many people with type 1 diabetes continue to struggle to control blood sugar surrounding exercise
Many people with type 1 diabetes struggle to exercise safely while keeping their blood sugar levels within a healthy range, according to a study presented Thursday at ENDO 2023, the Endocrine Society’s annual meeting in Chicago, Ill.
Teens with type 1 diabetes who see a pediatrician longer may have a smoother transition to adult care
Keeping adolescents with type 1 diabetes in pediatric diabetes care until at least age 17 may increase the chance that they will have a successful transition to adult care, according to a study presented Thursday at ENDO 2023, the Endocrine Society’s annual meeting in Chicago, Ill.
Machine-learning method used for self-driving cars could improve lives of type-1 diabetes patients
The same type of machine learning methods used to pilot self-driving cars and beat top chess players could help type-1 diabetes sufferers keep their blood glucose levels in a safe range.
nPOD honors Estefania Quesada Masachs for type 1 diabetes discoveries
La Jolla Institute for Immunology (LJI) Instructor Estefania Quesada Masachs, M.D., Ph.D., has won the 2023 Young Investigator of the Year Award from the Network for Pancreatic Organ donors with Diabetes (nPOD). This prestigious award recognizes Quesada Masachs’ groundbreaking research in type 1 diabetes.
Family’s participation key to advancing diabetes research
A study of one family from Alabama has led Vanderbilt University Medical Center researchers to discover that insulin deficiency, independent of the autoimmunity associated with Type 1 diabetes, is the principal factor leading to a markedly smaller pancreas.
Incidence Rates of Diabetes Continue to Increase in Children, Young Adults
New findings from researchers at Wake Forest University School of Medicine confirm that the rates of Type 1 and Type 2 diabetes continue to increase in children and young adults. Non-Hispanic Black and Hispanic children and young adults also had higher incidence rates of diabetes.
Overweight and obesity prevalent and poorly managed among adults with type 1 diabetes
A brief research report found adults with type 1 diabetes had overweight or obesity at the same rates as adults without diabetes, but only half of these patients received lifestyle recommendations from providers or engaged in lifestyle modification for weight management. The report is published in Annals of Internal Medicine.
Language of Care: University of Utah Health Researchers Co-Design Health Care With the Deaf Community
Navigating health care is hard enough when English is your first language—imagine the difficulty when American Sign is your first language. How can we bridge the linguistic and cultural gaps needed to better care for patients? University of Utah Health is proud to present Language of Care, an incredible short film of how a community of Deaf patients are breaking barriers by co-designing their own care with U of U Health researchers.
Racial, ethnic, socioeconomic disparities in insulin pump use have persisted over 20 years
While use of insulin pumps to manage type 1 diabetes has grown over 20 years, there has been no improvement in racial, ethnic, and socioeconomic disparities in their use.
Parkinson’s medication improved blood pressure in teens with Type 1 diabetes
Teens with Type 1 diabetes (T1D) who took bromocriptine, a medication used to treat Parkinson’s disease and Type 2 diabetes, had lower blood pressure and less stiff arteries after one month of treatment compared to those who did not take the medicine, according to a small study published today in Hypertension, an American Heart Association journal.
Children with type 1 diabetes miss more school, study suggests
Children living with type 1 diabetes miss an average of nine more sessions of school a year compared to children without the condition, a new study led by Cardiff University has found.
New Startup Develops Potential Cure for Type 1 Diabetes
Insulin injections to treat Type 1 diabetes could become a thing of the past, but finding the cure faces many challenges. Although transplanting insulin-producing cells represents a promising approach, this cell therapy requires immunosuppression to prevent rejection. Georgia Tech researchers have developed a new biomaterial called iTOL-100 that could cure Type 1 diabetes by inducing immune acceptance of curative transplanted cells without immunosuppression.
Researchers ID Pathway Involved in Inflammatory Bladder Damage in Mouse Model of Type 1 Diabetes
Article title: Diabetes causes NLRP3-dependent barrier dysfunction in mice with detrusor overactivity but not underactivity Authors: Michael R. Odom, Francis M. Hughes Jr., Huixia Jin, J. Todd Purves From the authors: “This is the first study to demonstrate that NLRP3-mediated…
COVID-19 associated with increase in new diagnoses of type 1 diabetes in youth, by as much as 72%
Children who were infected with COVID-19 show a substantially higher risk of developing type 1 diabetes (T1D), according to a new study that analyzed electronic health records of more than 1 million patients ages 18 and younger.
Rutgers Will Conduct the Most Comprehensive Study Ever Done of High-Risk Children Newly Diagnosed with Type 1 Diabetes
Rutgers researchers will conduct the largest and most comprehensive study of children at high risk of developing a life-threatening complication of Type 1 diabetes with funding from JDRF.
Endocrine Society celebrates passage of historic insulin affordability measure
The Endocrine Society cheered the Senate’s passage of the Inflation Reduction Act, including meaningful measures to make insulin more affordable.
Helping the body make more insulin
Aresearch team is testing a protein block to suppress specific cells of the body’s immune system contribute to developing type 1 diabetes. If successful, the drug would diminish autoimmunity, preserving the body’s ability to naturally produce more insulin, the researchers said.
Researchers develop pancreatic beta-cell restoring therapy for treating type 1 diabetes
Researchers have successfully treated type 1 diabetes in mice using pancreatic beta-cell, target-specific, chimeric antigen-receptor (CAR) regulatory T cells (Tregs), and demonstrated the feasibility of their approach to treat the human condition according to data being presented Monday, June 13 at ENDO 2022, the Endocrine Society’s annual meeting in Atlanta, Ga.
Stem-cell based therapy shows promise in treating high-risk type 1 diabetes
An investigative stem cell-based therapy called PEC-Direct, designed to act as a replacement pancreas, has the potential to provide blood sugar control in patients with high-risk type 1 diabetes, suggests a clinical study presented Saturday, June 11 at ENDO 2022, the Endocrine Society’s annual meeting in Atlanta, Ga.
Stem cell therapy protects against the side effects of cancer drugs
Immune checkpoint inhibitors are widely used to treat a variety of cancers; however, one serious side effect is the onset of type 1 diabetes.
Childhood obesity increases risk of type 1 diabetes
Being overweight in childhood increases the risk of developing type 1 diabetes in later life, according to the findings of a new study that analysed genetic data on over 400,000 individuals. The study, co-led by researchers from the Universities of Bristol and Oxford and published today in Nature Communications, also provides evidence that being overweight over many years from childhood influences the risk of other diseases including asthma, eczema and hypothyroidism.
Personalized medicine research focuses on Hispanics with diabetes in South Texas
A team of researchers studying genetic data to identify hormone responses in a population of Mexican Americans with prediabetes, Type 2 diabetes, and obesity recently received a $3.5 million grant to fund a five-year study set to begin in late 2021.
Structural Racism and Inequitable Pediatric Diabetes Care
Data show racial disparities in type 1 diabetes treatment and outcomes in non-Hispanic Black (NHB) children in the US. NHB children are less likely to be treated with diabetes technology, have poorer glycemic control and higher rates of diabetes complications and diabetes-related mortality than non-Hispanic white children. There is much to be done to ensure equitable care, but as yet, structural racism has not been a focus.
Researchers develop novel method for glucagon delivery
In a new study, published in the Journal of the American Chemical Society, Matthew Webber, associate professor of chemical and biomolecular engineering, is rethinking the traditional use of glucagon as an emergency response by administering it as a preventive measure.
Babies at Risk for Diabetes May Have Microbiota Restored
Newborns at risk for Type 1 diabetes because they were given antibiotics may have their gut microorganisms restored with a maternal fecal transplant, according to a Rutgers study.
Precision medicine helps identify “at-risk rapid decliners” in early-stage kidney disease
A novel therapeutic may halt rapid kidney function in some type 1 diabetic kidney disease patients.
Genetic Tools Help Identify a Cellular Culprit for Type 1 Diabetes
By mapping its genetic underpinnings, researchers at University of California San Diego School of Medicine have identified a predictive causal role for specific cell types in type 1 diabetes, a condition that affects more than 1.6 million Americans.
Experts mark the centennial anniversary of the discovery of insulin by highlighting the critical role adipose tissue has played in understanding insulin’s control of metabolism.
2021 marks 100 years since researchers identified insulin, a hormone produced by the pancreas that regulates the amount of glucose, or sugar, in the blood. Soon after, insulin was shown to be effective in lowering blood glucose in humans with…
High readmission rate found for adults with type 1 diabetes hospitalized for diabetic ketoacidosis
One in five adults with type 1 diabetes who require in-hospital treatment of the life-threatening condition diabetic ketoacidosis has an unplanned repeat hospital visit within a month and is twice as likely to die during the second hospitalization, a new study finds. The results, which will be presented at ENDO 2021, the Endocrine Society’s annual meeting, also identified several factors that increased the readmission risk for these patients.
Poor diabetes control in children tied to high risk for COVID-19 complications, death
Children with poorly controlled type 1 diabetes have a 10 times higher risk of COVID-19-related complications and death compared to those with well-controlled diabetes, according to a study presented virtually at ENDO 2021, the Endocrine Society’s annual meeting.
Tubeless automated insulin delivery system improves blood glucose outcomes
People with type 1 diabetes can improve their blood sugar control while reducing time with low blood sugar, or hypoglycemia, using Insulet Corporation’s Omnipod 5 Automated Insulin Delivery System compared to their standard insulin therapy. Results from an industry-sponsored study of the latest Omnipod, the first tubeless, wearable insulin pump, will be presented at ENDO 2021, the Endocrine Society’s annual meeting.
Children, teens with type 1 diabetes had better glucose control during COVID-19 lockdown
Blood glucose levels improved among children and teens with type 1 diabetes during the first 12 weeks of COVID-19 lockdown in the United Kingdom, according to a study presented virtually at ENDO 2021, the Endocrine Society’s annual meeting.

Addressing the Impact of Structural Racism on Disparities in Children with Type 1 Diabetes
Advancements in diabetes technology have improved quality of life and glycemic control in children with type 1 diabetes. However, data show that a subset of children is being left behind. Those from low-income families and non-Hispanic Black (NHB) children are not experiencing benefits associated with technological advances, and are at higher risk for diabetes complications and adverse outcomes through ongoing poor glycemic control.
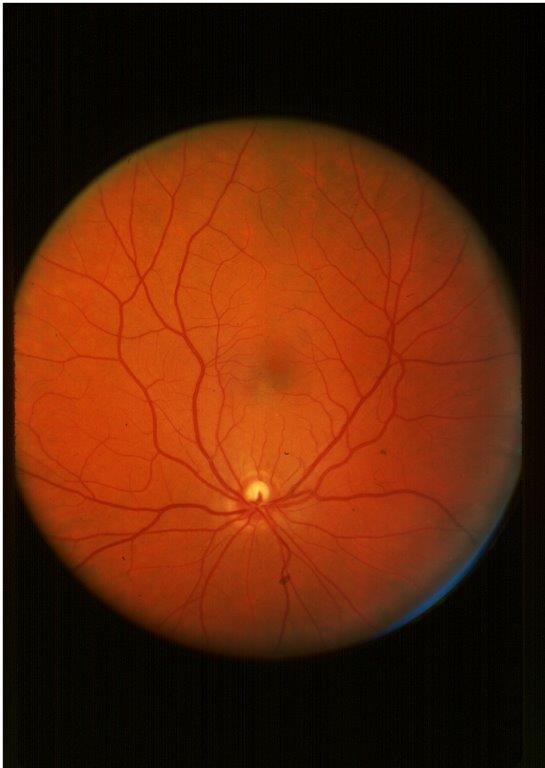
Routine eye scans may give clues to cognitive decline in diabetes
In older people with type 1 diabetes, damage to the retina may be linked to memory problems and other cognitive conditions.BOSTON – (December 31, 2020) – As they age, people with diabetes are more likely to develop Alzheimer’s disease and other cognitive disorders than are people without diabetes. Scientists at Joslin Diabetes Center now have shown that routine eye imaging can identify changes in the retina that may be associated with cognitive disorders in older people with type 1 diabetes.
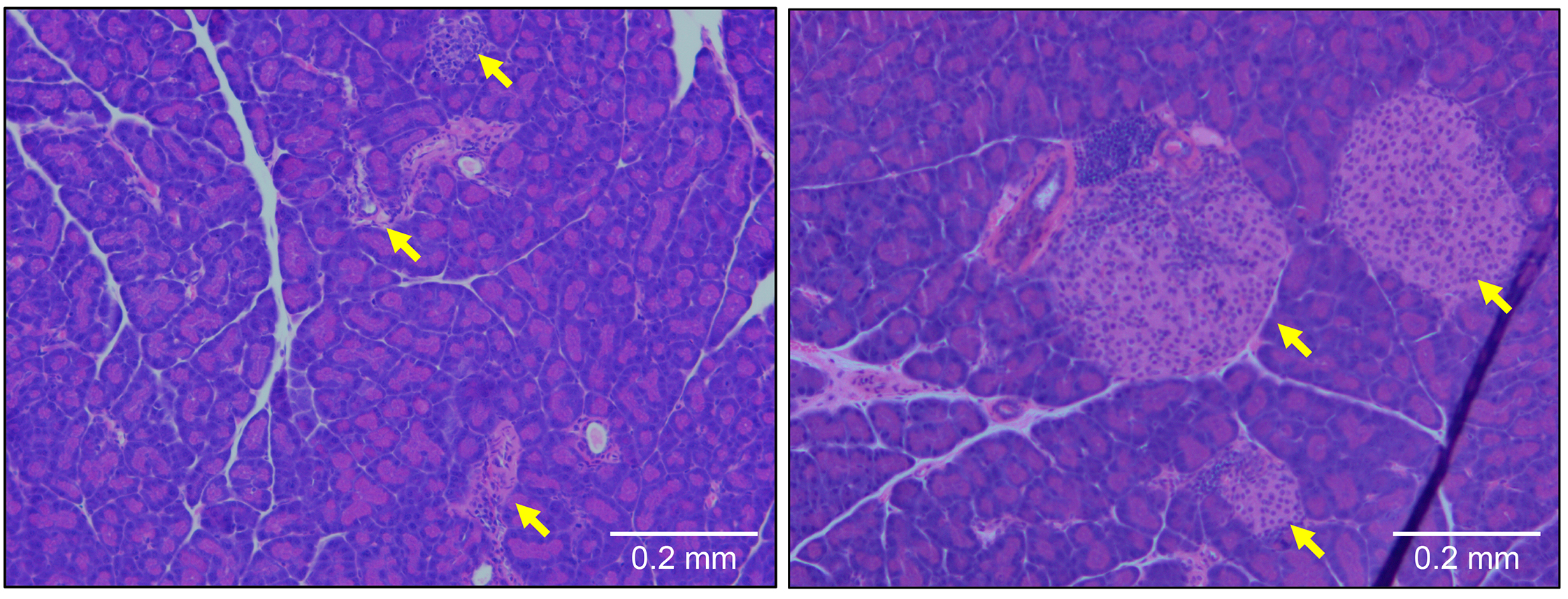
Targeting T cell protein could prevent type 1 diabetes, study suggests
Researchers at the University of Utah School of Medicine have identified a new therapeutic target to treat patients with type 1 diabetes. The study, which will be published December 9 in the Journal of Experimental Medicine (JEM), reveals that inhibiting a protein called OCA-B protects mice from type 1 diabetes by limiting the activity of immune cells that would otherwise destroy the pancreas’ insulin-producing β cells.

Racial Disparities in Pediatric Diabetes Treatment
Type 1 diabetes (T1D) is the third most common pediatric chronic disease in the United States, and the risk of the disease has risen sharply in non-Hispanic Black (NHB) children in the last 20 years, data show. Ironically, the significant advances in T1D therapeutics over recent years, especially new technologies, may have exacerbated racial disparities in diabetes treatment and outcomes
$14 Million Push for Type 1 Diabetes Breakthroughs: New JDRF Center of Excellence at the University of Michigan
A collaboration to accelerate research to cure type 1 diabetes and improve lives.

Raising Awareness During Diabetes Awareness Month – Adult and Pediatric Diabetes Experts Available
More than 34 million people in the U.S, or 10.5% of the population, have diabetes, according to the Centers for Disease Control and Prevention. And as many as 7 million more Americans have the disease and don’t know it. Diabetes is the seventh-leading cause of death in the country..

Type 1 diabetes: Tannic acid encapsulation protects transplanted islets from rejection
Transplanting cadaver pancreatic islets is a promising therapy for Type 1 diabetes, but a reactivated autoimmunity means low graft viability after five years. Research now shows that a protective coating of two biopolymers can delay allograft and autoimmune-mediated rejection in mouse models of T1D.