A new study by researchers at UCLA Health finds that early detection of specific microRNAs (miRNAs) packaged in vesicles may offer the opportunity to predict preeclampsia in pregnant people before clinical symptoms manifest.
Tag: Mortality
Researchers develop an AI model that predicts Continuous Renal Replacement Therapy survival
A UCLA-led team has developed a machine-learning model that can predict with a high degree of accuracy the short-term survival of dialysis patients on Continuous Renal Replacement Therapy (CRRT).
Intake of Ultra-Processed Foods Linked with Increased Risk of Death
In a new study, older adults who reported consuming higher amounts of ultra-processed foods, as defined by the NOVA classification system, were about 10% more likely to die over a median follow-up of 23 years compared with those who consumed less processed food.
NUTRITION 2024 Press Materials Available Now
Press materials are now available for NUTRITION 2024, the annual flagship meeting of the American Society for Nutrition (ASN). Top nutrition scientists and practitioners from around the world will gather to share the latest research findings on food and nutrition during the meeting in Chicago from June 29–July 2.
Non-Hodgkin lymphoma mortality disparities across different sexes, races, and geographic locations
Background: Non-Hodgkin lymphoma (NHL) is one of the common hematological cancers in the United States (U.S.), accounting for 4% of new cancer cases in 2023. The mortality rate of NHL is the sixth highest among all cancers in the U.S. Our…
Trend and burden of cancer related hospitalizations in the US: Insights from a National Inpatient Sample Database analysis
Background: Cancer-related hospitalizations constitute one of the primary drivers of cancer-related healthcare expenses. Understanding the burden and characteristics of these hospitalizations is essential to appropriately direct resources, improve outcomes, and avoid unnecessary hospitalizations. Our study sought to evaluate the national…
PARC MODEL OF CARE ASSOCIATED WITH FEWER DEATHS AMONG VETERANS POST-ICU
Research presented at the ATS 2024 International Conference demonstrates that veterans who received care via the Post-acute Recovery Center (PARC) model after a serious illness experienced fewer deaths and more days outside of the hospital compared to those not enrolled in PARC.
Being treated by a female physician associated with lower risk for death
An observational study of more than 700,000 male and female patients found that patients treated by female physicians experienced lower mortality and readmission rates compared to patients treated by male physicians.
CDC Sharply Overestimates Maternal Death Rate, New Study Finds
Researchers from Rutgers Health and other institutions dispute claims that the maternal death rate in the United States has climbed steeply in the past two decades.
Extreme Weather Events Tied to Increased Mortality and Emergency Department Activity
Mass General Brigham study reveals that ED visits and death are heightened weeks after major climate-driven extreme weather events – highlighting the long-lasting impacts these events may have on health and infrastructure
Could Ultra-processed Foods Be the New ‘Silent’ Killer?
Hundreds of novel ingredients never encountered by human physiology are now found in nearly 60 percent of the average adult’s diet and nearly 70 percent of children’s diets in the U.S. An emerging health hazard is the unprecedented consumption of these ultra-processed foods in the standard American diet. This may be the new “silent” killer, as was unrecognized high blood pressure in previous decades.
Study links childhood trauma to COVID-19 deaths, hospitalizations
People who endured childhood adversity, like abuse or neglect, were 12-25% more likely to be hospitalized or die from COVID-19 in adulthood, a new University of Pittsburgh study found.
High Pregnancy Weight Gain Tied to Higher Risk of Later Death
Findings from 50 years of data highlighted the health risks when more weight is gained in pregnancy than recommended, especially when it comes to heart disease- and diabetes-related mortality
For older men, treating urinary symptoms may lead to lower mortality risk
Effective treatment for lower urinary tract symptoms (LUTS) in men aged 50 or older is associated with a lower risk of death over the next few years, reports a study in the October issue of The Journal of Urology®, an Official Journal of the American Urological Association (AUA).
Heart transplant patients from socioeconomically distressed communities face higher mortality, organ failure risk
FINDINGS People from socioeconomically distressed communities who underwent heart transplantation between 2004 and 2018 faced a 10% greater relative risk of experiencing graft failure and dying within five years compared to people from non-distressed communities. In addition, following implementation of the 2018 UNOS Heart Allocation policy, transplant recipients between 2018 and 2022 faced an approximately 20% increase in relative risk of dying or experiencing graft failure within three years compared with the pre-policy period.
“Well-being index” predicts population cardiovascular risk
Well-being index (WBI) is a comprehensive measure of an individual’s satisfaction with their career, social and community relationships, finances and health. Researchers compared results from a Gallup national WBI survey to CDC cardiac death data, and found a nearly 14%…
Mortality, Survival, and Readmissions During a 12-Month Follow-Up After Hip Fracture: Inpatient Rehabilitation Versus Home Rehabilitation
Abstract Purpose This study compared readmissions, survival, and mortality during a 12-month follow-up period of inpatient rehabilitation and home rehabilitation for older persons who had experienced a hip fracture. Methods This work was retrospective cohort research. Between January 1 and December 30, 2019, the medical records of 280…
Patients With Alzheimer Disease, Dementia Face 2x Risk of Dying After ICU Discharge
Older adults with Alzheimer disease and related dementia who were admitted to an ICU were much less likely to be discharged home and faced almost twice the risk of dying soon after discharge and within the 12 months afterward.
Coronary Bioresorbable Scaffolds Nearly as Safe and Effective as Conventional Metal Stents for Heart Disease Patients
First-generation bioresorbable vascular scaffolds (BVS) may be just as effective as drug-eluting metallic stents, which are currently the standard treatment for heart disease patients undergoing percutaneous coronary intervention (PCI).
Long-term mortality in individuals diagnosed with cancer during pregnancy or postpartum
About The Study: This population-based study found that pregnancy-associated cancers had increased overall 5-year mortality, though not all cancer sites presented the same risk. Authors: Amy Metcalfe, Ph.D., of the University of Calgary in Calgary, Canada, is the corresponding author. To access…
In Epilepsy, Higher Risk of Early Death Varies Based on Severity, Other Factors
A new study has found that people with epilepsy have an increased risk of early death and the increased risk varies depending on where they live, the number of medications they take and what other diseases they may have. The study is published in the March 22, 2023, online issue of Neurology®, the medical journal of the American Academy of Neurology.
‘Other’ race/ethnicity linked to higher suicide and overdose risk in military members with mild TBI
Previous studies have reported high rates of death by suicide and drug overdose – including opioid overdose – in military service members with a history of mild traumatic brain injury (mTBI). A new study finds that those risks are highest among military members with mTBI who identify their racial/ethnic status as “Other,” as opposed to standard racial/ethnic categories, reports the March/April issue of the Journal of Head Trauma Rehabilitation (JHTR). The official journal of the Brain Injury Association of America, JHTR is published in the Lippincott portfolio by Wolters Kluwer.
Men Over 65 Are at Greater Risk than Women of Skull Fractures from Falls
Because females 65 and older have an increased rate of falls and facial fractures, researchers compared the risk of skull fracture secondary to head trauma in geriatric female and male patients. Results showed that males had a significantly increased incidence of skull fracture secondary to head trauma, due mostly to falls. This outcome was unexpected, as previous research has indicated females are more susceptible to facial fractures. This trend also was seen across race/ethnicity, though results were only statistically significant for whites.

Upward trend in ‘deaths of despair’ linked to drop in religious participation, economist finds
Over the past 20 years, the death rate from drug poisonings in the U.S. has tripled and suicide and alcoholic liver disease death rates have increased by 30 percent — particularly among middle-aged white Americans. Daniel Hungerman, professor of economics at the University of Notre Dame, and his co-authors studied the connection between a sharp downturn of religious participation in the late 1980s and the swift rise in these “deaths of despair” among white Americans ages 45 to 54 in the early 1990s.
Ignoring Native American data perpetuates misleading white ‘deaths of despair’ narrative
An increase in “deaths of despair” in recent decades has been frequently portrayed as a phenomenon affecting white communities, but a new analysis in The Lancet shows the toll has been greater on Native Americans.
Increasing Robo4 expression may help with infections
The researchers screened a library of drugs using a mouse endothelial cell line to identify pathways that are involved in the regulation of Robo4 and found that two competitive SMAD signaling pathways appear to regulate Robo4 expression. When the researchers treated LPS-injected mice with a drug that inhibits ALK1-SMAD signaling, they observed increased Robo4 expression, decreased vascular permeability, and reduced mortality.

Vitamin D deficiency linked to premature death
Now, new research from the University of South Australia gives strong evidence that vitamin D deficiency is associated with premature death, prompting calls for people to follow healthy vitamin D level guidelines.
Needs and Challenges for COVID-19 Boosters and Other Vaccines in the U.S.
FAU researchers and collaborators provide the most updated guidance to health care providers and urge how widespread vaccination with these boosters can now avoid the specter of future and more lethal variants becoming a reality.
New Risk Score Predicts Mortality for Atrial Fibrillation Patients Undergoing Transcatheter Aortic Valve Replacement
Mount Sinai researchers develop new risk stratification tool to optimize patient care and outcomes after TAVR
Feeling Anxious or Blue? Ultra-processed Foods May be to Blame
A study measuring mild depression, number of mental unhealthy days and number of anxious days in 10,359 adults 18 and older found those who consumed the most ultra-processed foods as compared with those who consumed the least amount had statistically significant increases in the adverse mental health symptoms of mild depression, “mentally unhealthy days” and “anxious days.” They also had significantly lower rates of reporting zero “mentally unhealthy days” and zero “anxious days.” Findings are generalizable to the entire U.S. as well as other Western countries with similar ultra-processed food intakes.
Cardiac death rates declined for both Black and white Americans since 1999, but racial disparities persist
Researchers at Beth Israel Deaconess Medical Center conducted a comprehensive investigation of national trends in cardiovascular mortality among Black and white women and men across multiple socio-demographic domains and found a decline in cardiovascular mortality rates across all groups over the last 20 years.
Research Shows Alarming Increases in Deaths from Alcoholic Cirrhosis in the U.S.
Researchers conducted an original research study utilizing the U.S. Centers for Disease Control and Prevention’s Wide-ranging Online Data for Epidemiologic Research (WONDER) to compare trends in mortality from alcoholic cirrhosis in the U.S. in 1999 with those 20 years later in 2019.
Heart Failure Patients Unvaccinated Against COVID-19 Are Three Times More Likely to Die From It Than Boosted Heart Failure Patients
EMBARGOED UNTIL JUNE 9, 2022, 10AM EST (New York, NY – June 9, 2022) – Heart failure patients who are unvaccinated against SARS-CoV-2, the virus that causes COVID-19, are three times more likely to die if infected with the virus…
Many Historically “Redlined” California Communities Have Higher COVID-19 Incidence and Mortality
One of the legacies of “redlining” may be higher incidence and mortality rates of COVID-19 affecting the largely minority and poor residents of these neighborhoods, according to research published at the ATS 2022 international conference. ” Redlining is a Great Depression-era federal policy in which neighborhoods with large ethnic/racial minority groups were denied federal resources.
For older men, urinary symptoms may affect mortality risk – even if not ‘bothersome’
For men in their fifties and older, moderate to severe lower urinary tract symptoms (LUTS) such as incontinence and frequent nighttime urination (nocturia) are associated with an increased risk of death during long-term follow-up, suggests a Finnish study in The Journal of Urology®, an Official Journal of the American Urological Association (AUA). The journal is published in the Lippincott portfolio by Wolters Kluwer.
Patients with rare scleroderma have deadlier organ damage, despite getting standard treatment
Patients with a rare form of scleroderma that causes more skin thickening have a greater chance of dying from related heart, lung and kidney problems, a new study found. This occurs despite the patient population taking drugs used to treat most people with scleroderma. Researchers say it is an opportunity for more targeted drug development.
COVID-19 slows birth rate in U.S., Europe
Throughout history, pandemics have been a key driver of human population change, thanks to mortality and declining fertility rates. And, according to a new study co-authored by a Cornell professor, COVID-19 is no exception.
Language barriers do not explain why immigrants have higher mortality from COVID-19
Language barriers or lack of institutional awareness do not explain why immigrants in Sweden have a higher mortality from COVID-19.
Molecular Mechanism for COVID-19 Mortality Identified
An enzyme with an elusive role in severe inflammation may be a key mechanism driving COVID-19 severity and could provide a new therapeutic target to reduce COVID-19 mortality. This finding by a team of researchers is detailed in a study to be published in the Journal of Clinical Investigation.
Who Lives, Who Dies, and How and Why?
In a world dealing with the worst public health crisis in a century, the current U.S. system for tracking deaths suffers from organizational, political and procedural flaws that actually put public health and safety at risk, and requires significant updates and reform to solve the problems laid bare by the COVID-19 pandemic.
Inequity in the air of India
Air pollution in India is generated more by the wealthy, while the poor suffer most of the health impact, according to a study by five IIASA researchers published in Nature Sustainability.
Americans with Higher Net Worth at Midlife Tend to Live Longer
One of the keys to a long life may lie in your net worth.
UCLA-led Research Finds Connections Between Air Quality and COVID Vulnerability
Even as governments across the United States consider lifting mask mandates and relaxing preventative measures as vaccination numbers creep up, new research from a UCLA-led team has found that such basic techniques significantly reduce the risk of getting COVID-19. In addition, the research found that U.S. counties with higher exposures to poor air quality, historically, saw higher county-level COVID-19 mortality rates in 2020.
Researchers Test Model to Predict Drug Overdose Deaths in U.S.
Researchers at UC San Diego, San Diego State University, and international collaborators have designed and validated a prediction model to signal counties at risk of future overdose death outbreaks.
Efforts to reduce opioid prescriptions may be hindering end-of-life pain management
Policies designed to prevent the misuse of opioids may have the unintended side effect of limiting access to the pain-relieving drugs by terminally ill patients nearing the end of their life, new research led by the Oregon State University College of Pharmacy suggests.
Black, Hispanic, Native Americans Have Borne the Burden of Years of Life Lost From the Pandemic
A UCLA Fielding School of Public Health-led team has found that Hispanic, Black, and Native Americans have carried the burden of the pandemic, both in overall mortality and specifically in years of potential life lost, in an analysis of 45 U.S. states and the District of Columbia (D.C.).
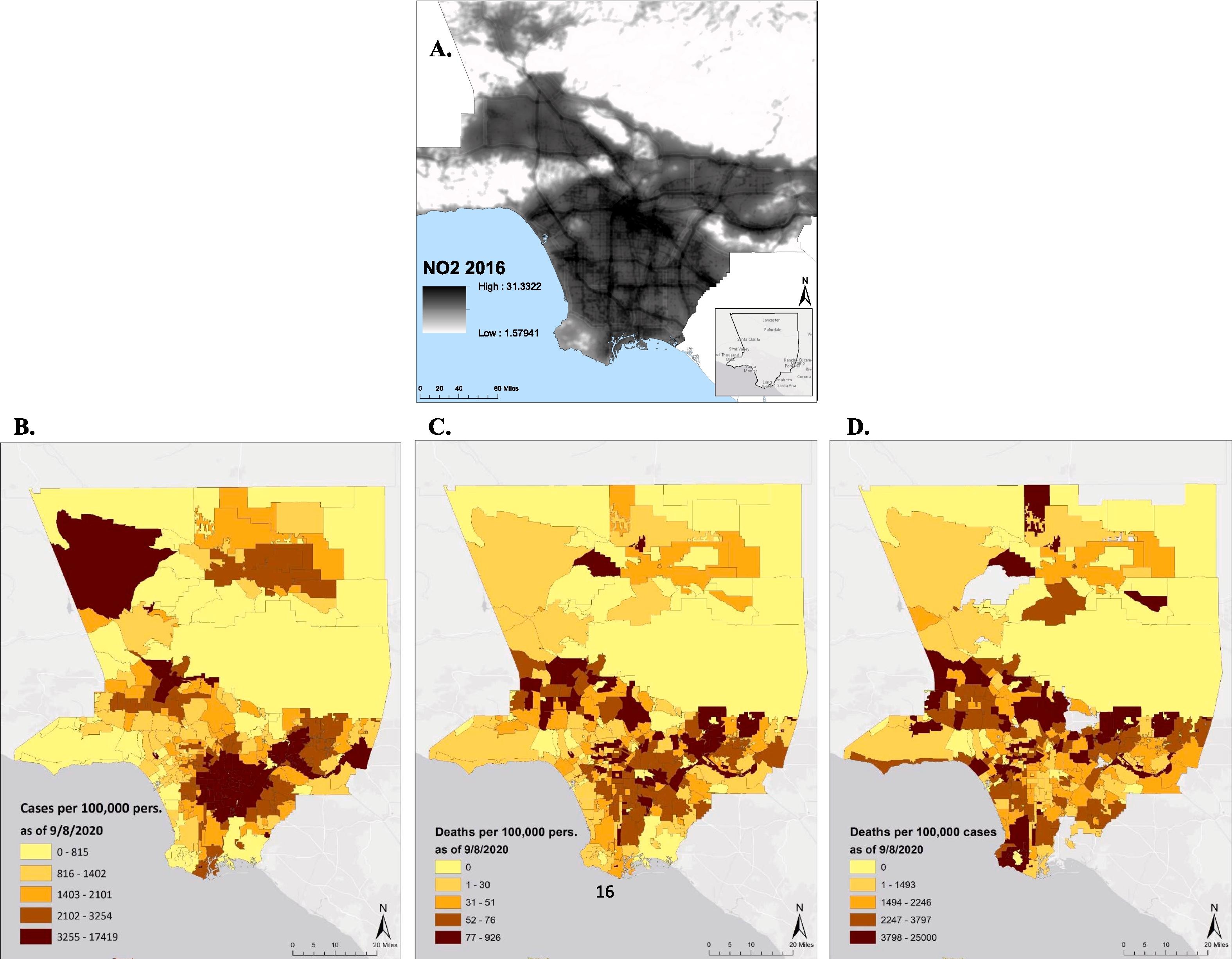
COVID-19 Mortality Rates in Los Angeles County Higher in Communities with Poor Air Quality
A research project led by the UCLA Fielding School of Public Health has found that Los Angeles County neighborhoods with poor air quality had the highest death rates from the pandemic.
High readmission rate found for adults with type 1 diabetes hospitalized for diabetic ketoacidosis
One in five adults with type 1 diabetes who require in-hospital treatment of the life-threatening condition diabetic ketoacidosis has an unplanned repeat hospital visit within a month and is twice as likely to die during the second hospitalization, a new study finds. The results, which will be presented at ENDO 2021, the Endocrine Society’s annual meeting, also identified several factors that increased the readmission risk for these patients.
Health declining in Gen X and Gen Y, national study shows
Recent generations show a worrying decline in health compared to their parents and grandparents when they were the same age, a new national study reveals.
Study finds racial disparities in COVID-19 deaths in nursing homes
Nursing homes with the largest proportions of non-White residents experience 3.3 times more COVID-19 deaths than do nursing homes with the largest proportions of White residents, according to a new study from the University of Chicago.