The scorching heat can be inescapable this time of year, and as temperatures hover around triple digits, experts at UT Southwestern Medical Center caution that uncomfortable weather can escalate to dangerous health conditions.
Tag: Emergency Medicine
Study Challenges ED Protocols for Geriatric Head Injuries and Blood Thinners
Out of 3,425 patients enrolled in the study, 0.4% (13 patients) experienced a delayed intracranial hemorrhage, a significantly lower rate than previously reported (7.2%).
Benjamin S. Abella, MD, MPhil, Named as Chair of the Department of Emergency Medicine for the Mount Sinai Health System
Benjamin S. Abella, MD, MPhil, a national leader in the study of sudden cardiac arrest and cardiopulmonary resuscitation (CPR), has been appointed Chair of the Department of Emergency Medicine for the Icahn School of Medicine at Mount Sinai and the Mount Sinai Health System.
High Blood Pressure in the Hospital: What Doctors Should Know
A new statement from the American Heart Association recommends a much more conservative approach to treating high blood pressure in acute care.
Injury Prediction Rule Could Decrease Radiographic Imaging Exposure in Children, Study Shows
In a study published today in The Lancet Child & Adolescent Health, researchers in the Pediatric Emergency Care Applied Research Network (PECARN) created a highly accurate cervical spine injury prediction rule. When applied, the rule decreases the use of CT by more than 50% without missing clinically significant injuries or increasing normal X-ray use.
Loyola Medicine Hosts First Annual Regional Keeley Cup To Benefit Emergency Medicine Education
Loyola Medicine’s Emergency Medicine Residency Program is proud to host the inaugural Regional Keeley Cup on Thursday, May 30th at 12 pm. This pioneering team-based competition is brought to life each year through the support of the Barbara G. & John L. Keeley, Jr. Center for Emergency Medicine Education.
AI Can Help Improve ER Admission Decisions, Mount Sinai Study Finds
Generative artificial intelligence (AI), such as GPT-4, can help predict whether an emergency room patient needs to be admitted to the hospital even with only minimal training on a limited number of records, according to investigators at the Icahn School of Medicine at Mount Sinai.
Mount Sinai’s Yvette Calderon, MD, MS, Receives Prestigious Award From Society for Academic Emergency Medicine
Top honor recognizes her commitment to justice, equity, diversity, and inclusion through scholarship, mentorship, and leadership
ER patient portal usage increasing, study shows
More people are using online patient portals to view their information while in the emergency room, but access is challenging for members of medically underserved communities and the elderly, UT Southwestern Medical Center researchers and national colleagues found in a new study.
Undocumented Latinx patients got COVID-19 vaccine at same rate as U.S. citizens
For undocumented Latinx patients who sought care in the emergency room during the pandemic, the reported rate of having received the COVID-19 vaccine was found to be the same as U.S. citizens, a new UCLA Health study found.
New study validates prediction rules for pediatric intra-abdominal and traumatic brain injuries
A new study from UC Davis Health’s Emergency Medicine may lead to a reduction in inappropriate computed tomography use in injured children.
Mental Health Emergencies in Kids Were More Severe During the Pandemic
A new study found that during the pandemic pediatric emergency departments (EDs) saw more children and adolescents who needed a psychiatric admission, as well as an increase in severe conditions, such as bipolar disorder, schizophrenia and substance use disorders.
Chicagoans are dying from cardiac arrest outside the hospital at increasingly younger ages
The biggest decrease in age happened among Black men
Mount Sinai Ophthalmologists Develop Novel Protocol to Rapidly Diagnose and Treat Eye Stroke
Study shows using advanced technology and time can prevent permanent vision loss
Quality of Care for Patients Who Call 911 Varies Greatly Across the United States, Study Finds
Mount Sinai research could lead to more consistency and safety measure.

A new path to recovery: Specialized unit looks to take mental health patients out of the emergency room for better care
The EmPATH unit at Overlook Medical Center will put adult behavioral emergency patients into a setting in which they will get the appropriate care more quickly, thereby lessening volumes and wait times in the emergency department, and, ultimately, reducing the need for inpatient hospitalization.
Women stroke survivors believe they will receive worse care in the emergency room
Women who have survived a stroke believe they are less likely to receive adequate emergency care – based on gender and race or ethnicity, a study shows. Researchers say future studies must focus on whether the beliefs these women hold about emergency care are leading to delays in stroke care.
Dr. Federico Vaca to lead Association for the Advancement of Automotive Medicine
Irvine, Calif., Sept. 25, 2023 —University of California, Irvine emergency medicine physician Federico Vaca, one of the nation’s leading researchers on motor vehicle crash injuries and prevention, has been named president of the Association for the Advancement of Automotive Medicine.
Anesthesiologist, Emergency Physician and Radiologist Groups Laud Court Decision, Urge HHS Action to Unfreeze Arbitration Process
In its fourth ruling regarding the flawed implementation of the No Surprises Act, the U.S. District Court for the Eastern District of Texas agreed with the plaintiffs, the Texas Medical Association, that the government was incorrectly permitting insurers to use a faulty methodology when calculating their median in-network rate, also known as the qualifying payment amount (QPA). This TMA III ruling does not impact the patient protections included in the No Surprises Act that the American College of Radiology® (ACR®), (ACR), American College of Emergency Physicians (ACEP) and the American Society of Anesthesiologists (ASA) advocated for and continue to fully support, nor does it raise patient out-of-pocket costs.
Be cautious to avoid burns in extreme heat or when grilling
With triple-digit temperatures continuing across many parts of the country and the outdoor grilling season still in full swing, a UT Southwestern Medical Center physician who specializes in burn care wants to remind people to be careful around hot surfaces such as a grill or a playground slide.
UTSW Q&A: Experts talk about opioid abuse, risks, treatment
Overdose deaths from opioids, including prescription painkillers and synthetics like fentanyl, continue to rise.
Emergency General Surgery Verification Program Verifies First Five Hospitals
Five hospitals are among the first in the nation to be verified under the new American College of Surgeons Emergency General Surgery Verification Program (ACS EGS-VP) launched in September 2022.
UT Southwestern toxicologist offers tips to keep food safe during summer grilling season
The arrival of summer marks the return of a cherished activity: backyard grilling. A UT Southwestern Medical Center toxicologist offers some cautionary guidelines to help you and your guests avoid food poisoning.
Heat-related Emergencies on the Rise – Ochsner Health Expert Available to Interview
With temperatures and the heat index reaching 100 degrees, taking the proper precautions to prevent heat stroke is important. Heat Stroke is a major cause of illness and even death during the hot summer months. It is a danger for…
Brain stimulation may prove helpful to acute stroke patients, pilot study suggests
There are few effective treatments for acute stroke, and many patients aren’t eligible for them. An innovative pilot study from UCLA Health found promising results for a new potential treatment: highly targeted electrical stimulation to the affected brain area.
Transgender people seen in the ER much more likely than cisgender people to be admitted to hospital
Transgender people who come to the emergency room for care tend to be sicker than cisgender people who are otherwise similar to them and are much more likely to be admitted to the hospital once they visit the ER, according to a study being presented Saturday at ENDO 2023, the Endocrine Society’s annual meeting in Chicago, Ill.
‘Concerning’ CT scans may cause unnecessary hospitalization for some pulmonary embolism patients
Some pulmonary embolism patients may be hospitalized unnecessarily due to CT imaging results rather than clinical risk factors, a study finds. Roughly half of the low risk patients had CT imaging features that physicians consider “concerning”, and these patients fared just as well in the hospital as those whose CT scans showed no concerning findings.
Bilingual, digital health tool helps reduce alcohol use, UC Irvine-led study finds
An automated, bilingual, computerized alcohol screening and intervention health tool is effective in reducing alcohol use among Latino emergency department patients in the U.S., according to a study led by the University of California, Irvine. “This is the first bilingual, large-scale, emergency department-based, randomized clinical trial of its kind in the country focused on English- and Spanish-speaking Latino participants,” said lead author Dr.
UC San Diego Health Sheds Light on Stroke Awareness
Every minute counts when it comes to responding to a stroke. It is the second leading cause of death worldwide according to the World Health Organization. High blood pressure, high cholesterol, smoking, obesity and diabetes are the leading causes of…
Bypassing contrast in patients with kidney disease and contrast allergies may lead to less accurate scans
Upon an arrival to the emergency department for abdominal pain of unknown cause, most non-pregnant adult patients receive a CT scan with IV contrast to diagnose the source of the pain. However, IV contrast can be a risk in patients with severe kidney disease or at risk for an allergic reaction from the dye. When scans are performed without IV contrast, though, they are usually less accurate, which can lead to misdiagnosis.

Seven Hackensack Meridian Medical Centers Recognized for Excellence with ACC Heart Failure Accreditation
Facilities that achieve accreditation meet or exceed an array of stringent criteria and have organized a team of doctors, nurses, clinicians and other administrative staff that earnestly support the efforts leading to better patient education, improved patient outcomes, and more effective and efficient disease control.

Patients prefer immediate access to medical test results online, even if it’s bad news
Patients overwhelmingly prefer to receive test results as soon as they are available on online medical portals, even if it means viewing the results prior to discussing them with their doctor, a new study co-led by researchers at UT Southwestern and Vanderbilt University medical centers reports.
Men Over 65 Are at Greater Risk than Women of Skull Fractures from Falls
Because females 65 and older have an increased rate of falls and facial fractures, researchers compared the risk of skull fracture secondary to head trauma in geriatric female and male patients. Results showed that males had a significantly increased incidence of skull fracture secondary to head trauma, due mostly to falls. This outcome was unexpected, as previous research has indicated females are more susceptible to facial fractures. This trend also was seen across race/ethnicity, though results were only statistically significant for whites.
CHOP Researchers Find Rate of Fatal Opioid Poisonings Among Children More Than Doubled Over 13-Year Span
Researchers found opioids were responsible for more than half of all fatal poisonings in children ages 5 and younger, more than double the proportion of fatal poisonings caused by opioids in 2005. Additionally, over-the-counter drugs still contribute to fatal poisonings in this age group despite increased regulation. The findings, published today in the journal Pediatrics, underscore the need for improved intervention to prevent further fatal poisonings.

Researchers Uncover Mechanisms of Brexanolone and the Role of Inflammation in Post-partum Depression
Brexanolone, an IV infusion comprised of a derivative of progesterone, was approved by the U.S. Food and Drug Administration for the treatment of PPD in 2019. The fast-acting medication significantly reduces depression symptoms and provides effects for up to 90 days. However, exactly how the drug provides these therapeutic effects has remained a mystery – until now.
How Better Feedback at Work Can Also Reduce Gender Disparities
A study published recently in JAMA Network Open, led by Mira Mamtani, MD, MSEd, an associate professor of Emergency Medicine, found vast differences in the feedback given and received by emergency medicine residents. Mamtani draws upon the findings of the study to offer guidance for providing better feedback.
CHOP Study Finds Multidisciplinary Approach Best When Assisting Families with Limited English Proficiency
Pediatric patients with limited English proficiency (LEP) may face additional challenges when they present to an emergency room. However, researchers found that a multidisciplinary approach helped implement the services of interpreters earlier and significantly improved the identification of these patients to help them receive the care they need.
Fentanyl overdoses are on the rise. Here’s what to know and how you can help.
Community awareness is critical to preventing overdoses
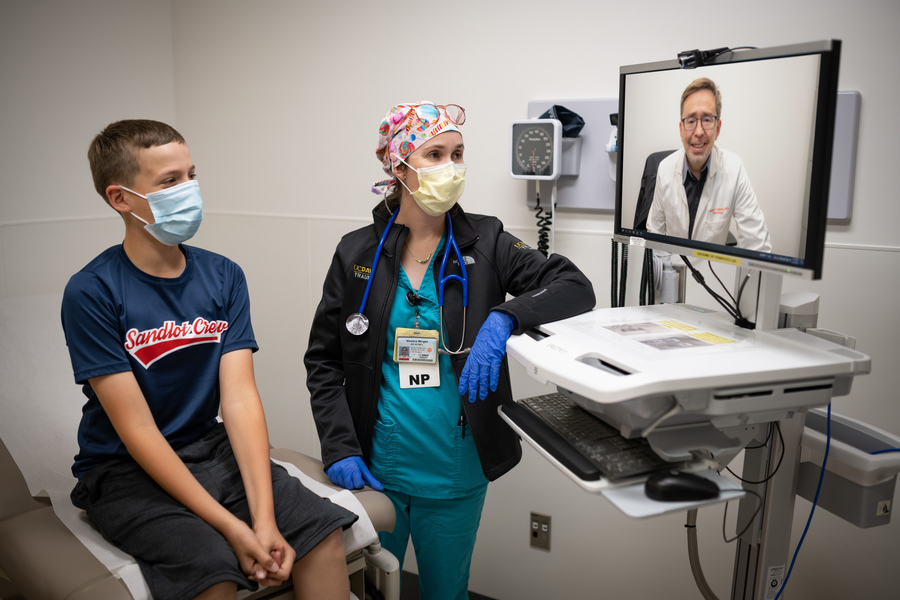
Telemedicine reduces hospital transfers for very ill kids at rural, community emergency departments
New UC Davis Health research confirms that pediatric critical care telemedicine consults with clinicians in rural and community emergency departments result in fewer hospital transfers.

Traitement de première intention inapproprié de l’état de mal épileptique : problématique et solutions
Malgré les recommandations, le traitement de première intention de l’état de mal épileptique est souvent inapproprié. Des études suggèrent que jusqu’à deux tiers des patients reçoivent des doses subcliniques de benzodiazépines, soit avant d’arriver à l’hôpital, soit pendant un traitement hospitalier d’urgence. Existe-t-il des solutions ?
University Hospitals Lake West Medical Center Designated Provisional Level 3 Trauma Center by the State of Ohio
University Hospitals (UH) Lake West Medical Center has been designated as a provisional Level 3 Trauma Center by the state of Ohio, based on consultation from reviewers of the American College of Surgery Verification, Review, and Consultation Program for excellence in trauma centers. The Program is designed to help hospitals evaluate and improve trauma care as well as provide objective, external review of institutional capability and performance. This is accomplished by an on-site review and assessment of the hospital’s commitment, readiness, resources, policies, patient care, performance improvement and other features.

Virtual reality tool helps UT Southwestern physicians learn to de-escalate tense situations
An innovative virtual reality (VR) training tool – developed by UT Southwestern Medical Center’s Department of Emergency Medicine in partnership with UT Dallas – could soon play a major role in helping physicians recognize and respond to potentially violent patient encounters.
Cost concerns keep older adults from seeking emergency care
Worries about what emergency care might cost them have kept some older adults from seeking medical attention even when they felt they might need it, a new study shows. In all, 22% of older adults who may have needed care from the emergency department didn’t go because of concerns about what they might have to pay.
Rural hospital closures affect operations of surrounding hospitals
A study by Penn State College of Medicine researchers found that nearby hospitals see increased emergency department visits and admissions as a result of rural hospital closures.
UC San Diego Health Recognized for Health Equity in Care of Sickle Cell Crisis
UC San Diego Health has been awarded the prestigious 2022 California Association of Public Hospitals and Health Systems Quality Leaders Award in the category of health equity.

Mental health, substance use issues prevalent among nonpsychiatric emergency room patients
A new study found that about 45% of patients who visit the emergency department for physical injuries and ailments also have mental health and substance use problems that are often overlooked.
NIH awards emergency medicine physicians two grants
The Department of Emergency Medicine has been awarded two National Institutes of Health grants totaling over $5 million to improve patient care. They include an effort to better evaluate pediatric trauma patients and another to identify effective treatments early in emergency care.
Study Finds Automated Texts Decrease Odds of Rehospitalization
Text messages sent automatically from patients’ primary care office after hospitalization were tied to decreased odds of needing further emergency care
Mount Sinai’s Yvette Calderon, MD, MS, Elected to National Academy of Medicine for Contributions to Emergency Medicine
Yvette Calderon, MD, MS, Chair of Emergency Medicine at Mount Sinai Beth Israel and Professor of Emergency Medicine at the Icahn School of Medicine at Mount Sinai, has been elected to the National Academy of Medicine (NAM). Election to the NAM is considered one of the highest honors in health and medicine, recognizing individuals who have demonstrated outstanding professional achievement and commitment to service. With her election, Mount Sinai has 26 faculty members in the NAM.
American Neurological Association Publishes Research Abstracts for ANA2022, Oct. 22–25 in Chicago
Abstracts of breaking research in neurology and neuroscience, to be presented at the 2022 American Neurological Association Annual Meeting Oct. 22-25, are now available in Annals of Neurology and on the ANA2022 website.