A study from The Ohio State University finds important differences among patients who survive a cardiac arrest to receive hospital care before their death.
Tag: Cardiac Arrest
New, simple test detects rare fatal genetic heart condition
A team of international researchers has revealed a new, simple clinical test to detect Calcium Release Deficiency Syndrome (CRDS), a life-threatening genetic arrhythmia that causes dangerously fast heartbeats and can lead to severe complications such as sudden cardiac arrest and death.
Expert: Bolstering cardiac arrest survival rates
Since Illinois Heart Rescue launched in 2012, the state’s cardiac arrest survival rate has more than doubled, and survival is almost 6% more than the national average due in part to partnerships with over 200 hospitals and emergency medical service…
Simulation Sessions Help ICU Clinicians Prepare for High-Risk, Infrequent Emergency Procedures
The cardiovascular ICU at the University of Mississippi Medical Center developed a simulation training program to improve clinicians’ ability to recognize clinical signs that would prompt an emergency ICU sternotomy for a postoperative cardiac surgery patient and rehearse the high-risk but infrequent procedure.
Chicagoans are dying from cardiac arrest outside the hospital at increasingly younger ages
The biggest decrease in age happened among Black men

AEDs often not used in cardiac arrest, even where they’re mandated
Automated external defibrillators (AEDs) are underutilized during cardiac arrest episodes despite laws in some states requiring their availability in high-risk areas such as athletic facilities, researchers at UT Southwestern Medical Center found.
Heart Checkups Advised for Kids Who Play Sports
Key Takeaways:Sudden cardiac arrest is a leading cause of death among young athletes.Pre-participation heart screenings are advised for athletes ages 12 and above.Cardiac tests can detect 99% of abnormalities.Heart defects don’t prohibit kids from playing sports.The fact that sudden cardiac arrest is a leading cause of death in young athletes seems illogical, provoking an obvious question: “That’s the point,” says Children’s Hospital Los Angeles cardiologist Paul Kantor, MBBCh, MSc, FRCPC.
Loyola Medicine cardiologists are available to discuss Lebron James’ 18-year-old son’s cardiac arrest.
MAYWOOD, IL – Loyola Medicine cardiologists, including Caroline Ball, MD, are available today to discuss Lebron James’ 18-year-old son’s cardiac arrest. According to a spokesman, USC freshman Bronny James, the eldest son of Lakers superstar LeBron James, was hospitalized Monday after suffering a…
Bronny James #cardiacarrest: University of Michigan cardiology experts available for interview
It was announced today that Bronny James, son of NBA great LeBron James, experienced a cardiac arrest Monday (July 24) and is in stable condition after treatment. While details are few, the University of Michigan Health Frankel Cardiovascular Center has experts…

University Hospitals Launches Program to Determine Need/Distribute Lifesaving Cardiac Defibrillators in Northeast Ohio Schools
University Hospitals (UH) is partnering with the Cleveland Browns, Make Them Know Your Name Foundation (MTKYN) and Kaulig Companies to ensure every school in Northeast Ohio is equipped with the latest life-saving technology and training in case an athlete suffers cardiac arrest.
Learning to save lives can start as early as age 4, according to new scientific statement
Building the skills for cardiopulmonary resuscitation (CPR) can begin as early as age 4 and layer on as children get older, so that by age 10 they may be able to perform effective chest compressions on training manikins, according to a new scientific statement from ILCOR, the American Heart Association and the European Resuscitation Council.
Predicting how CPR will work minutes ahead
Every year, between 1,200 and 1,500 patients suffer a cardiac arrest in Norwegian hospitals. Rapid and sound treatment is absolutely essential in helping these patients survive. Even if a patient suffers a cardiac arrest within the hospital’s four walls, the prognosis is poor. Only one in four survives. However, a new study suggests that easily available informaiton from the patient’s own ECG could change the outcome.
Communication may guide family members’ decisions after sudden cardiac death
Surviving family members of a person who died from sudden cardiac death rely on information from death investigators and health care professionals to process their relative’s death and understand their own risk of inherited heart conditions.
Older, Black, and low-income pregnant patients more likely to suffer cardiac arrest when hospitalized for delivery
A study of pregnant women hospitalized during delivery found that cardiac arrest occurred in about 1 in 9,000 deliveries, a rate that is higher than previously reported estimates. Cardiac arrest was more common among patients who were older, were non-Hispanic Black, had Medicare or Medicaid, or had underlying medical conditions. The findings are published in Annals of Internal Medicine.
Flu vaccination rate holds steady but misinformation about flu and Covid-19 persists
Although the public had been alerted that this winter could be a potentially bad flu season, barely half of Americans said in January that they had received a flu shot, a vaccination level unchanged in a representative national panel from the comparable period last year.
Learn CPR and Lower Your Stress: Mount Sinai Cardiologists Emphasize Their Importance During American Heart Month
Doctors warn about lack of knowledge of administering CPR, especially in high-risk groups, and the rise of stress-related heart issues
Should parents be concerned about their kids in sports in the wake of Damar Hamlin’s injury?
Dr. Olujimi A. Ajijola, an associate professor of medicine at the UCLA Cardiac Arrhythmia Center, is available to discuss what parents should know Amid Buffalo Bills safety Damar Hamlin’s ongoing recovery from a cardiac arrest, parents may wonder how to…
The Medical Minute: Hamlin’s cardiac arrest highlights need for equipment, training
The medical emergency suffered by Damar Hamlin of the Buffalo Bills underscores the importance of speed when responding to cardiac arrest. Two Penn State Health physicians offer guidance.
Cardiac Arrest: What Happened to Buffalo Bills Player Damar Hamlin?
Buffalo Bills safety Damar Hamlin, 24, remains hospitalized in “critical condition” after experiencing cardiac arrest when he collapsed mid-game against the Cincinnati Bengals on Monday night.
U-Mich Health experts able to comment on cardiac arrest – #Bills #DamarHamlin #cardiology
During the Jan 2. Monday Night Football game, Buffalo Bills safety Damar Hamlin, 24, collapsed after experiencing a cardiac arrest. This condition occurs when the heart suddenly stops beating because of a problem with its electrical system. When this occurs,…
Top cardiologists with the University of Miami are available to provide expert perspective on cardiac arrest among athletes. #DamarHamlin
Good morning, if your media outlet is following Damar Hamlin, the Buffalo Bills player who collapsed on the field last night due to cardiac arrest, Dr. Robert Myerburg and Dr. Jeffrey Goldberger, both nationally renowned cardiologists and cardiac electrophysiologists with…
New screening test for those at risk of sudden cardiac arrest
New research from the Victor Chang Cardiac Research Institute will allow families around the world to discover if they are carrying genetic mutations that cause sudden cardiac arrest – a condition that kills nine out of 10 victims.
Story Tips from Johns Hopkins Experts on COVID-19
Vaccines take time to work. After getting a COVID-19 vaccine, it takes a while for the immune system to fully respond and provide protection from the virus. For the Moderna and Pfizer COVID-19 vaccines, it takes up to two weeks after the second shot to become appropriately protected.
Women At Higher-Risk of Fatal, Nightime Cardiac Arrest
New research from the Center for Cardiac Arrest Prevention in the Smidt Heart Institute at Cedars-Sinai has found for the first time that during nighttime hours, women are more likely than men to suffer sudden death due to cardiac arrest. Findings were published in the journal Heart Rhythm.

Study Shows Women Less Likely to Survive Out-Of-Hospital Cardiac Arrest Than Men
DALLAS – Dec. 15, 2020 – A study of patients resuscitated from out-of-hospital cardiac arrest shows that women have a lower likelihood of survival compared with men and are less likely to receive procedures commonly administered following cardiac arrest.
Closing the Racial Disparity Gap in Survival After In-Hospital Cardiac Arrest
In-hospital cardiac arrests (IHCA) represent catastrophic and often terminal events. Despite investments to improve the quality of resuscitation efforts, fewer than 25% of all patients that experience cardiac arrests in hospitals survive to discharge, and survival varies significantly across hospitals and by race. Until now, few have been able to specify reasons for the between-hospital differences.
COVID-19 Patients Survive In-Hospital Cardiac Arrest at Pre-Pandemic Rates
Resuscitation and survival rates for hospitalized COVID-19 patients who have cardiac arrest are much higher than earlier reports of near-zero; variation at the individual hospital level may have affected overall numbers
Cardiac Arrest, Poor Survival Rates Common in Sickest Patients with COVID-19
Study shows critically ill patients with the novel coronavirus have high rates of cardiac arrest and poor outcomes even after CPR, an effect most strongly seen in older patients.
Critically Ill Patients with COVID-19 Are More Likely to Develop Heart Rhythm Disorders Than Other Hospitalized Patients
Patients with COVID-19 who were admitted to an intensive care unit were 10 times more likely than other hospitalized COVID-19 patients to suffer cardiac arrest or heart rhythm disorders, according to a new study. .
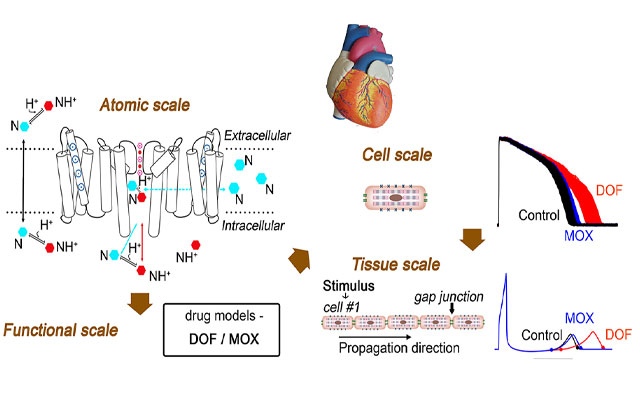
Supercomputing Drug Screening For Deadly Heart Arrhythmias
Using supercomputers, scientists have developed for the first time a way to screen drugs through their chemical structures for induced arrhythmias.
How Do Outcomes for In-Hospital Cardiac Arrest Differ in Patients Treated with Long-Term Dialysis?
• Among patients who experience cardiac arrest while in the hospital, those on dialysis were less likely to have a shockable rhythm and more likely to be outside of the intensive care unit at the time of arrest compared with patients not on dialysis.
• Patients on dialysis had lower scores for resuscitation quality, and they were less likely to have defibrillation within 2 minutes.
• Patients on dialysis had a similar likelihood of surviving to hospital discharge, and they had better neurological function at the time of discharge.
Bystander CPR Less Likely for People Living in Hispanic Neighborhoods Compared to Non-Hispanic Neighborhoods
People living in predominately Hispanic neighborhoods are less likely to receive CPR from a bystander following an out-of-hospital cardiac arrest compared to people living in non-Hispanic neighborhoods, researchers from Penn Medicine and the Duke University of School of Medicine reported in the journal Circulation. This same group also had a lower likelihood of survival.
CPR training kiosk comes to UChicago Medicine’s Center for Care and Discovery
The University of Chicago Medicine, in partnership with the American Heart Association, has installed a hands-only CPR kiosk in the Center for Care and Discovery. It’s one of three in Chicago.

How Effective is Body Cooling in Patients that Experience Cardiac Arrest?
A new nationwide clinical trial hopes to discover if patients that experience cardiac arrest survive more often and have a better recovery based on how long they have their body temperature cooled.

‘M-RISE’ Research Program Aims to Prevent Brain Damage Caused by Cardiac Arrest
ANN ARBOR, Mich. – For the more than 350,000 Americans that experience an out-of-hospital cardiac arrest each year, less than 1 in 10 of those treated will survive with good neurologic function. “Survival for these patients decreases with every minute there is a delay…