A study of more than 15,000 Hispanic/Latino adults of Central American, Cuban, Dominican, Mexican, Puerto Rican, and South American backgrounds found that the patterns of all-cause mortality among these groups were altered during the COVID-19 pandemic, persons of Central American and Mexican backgrounds may have been particularly affected. The study is published in Annals of Internal Medicine.
Tag: health disparaties
New Method Can Improve Assessing Genetic Risks For Non-White Populations
A team led by researchers at Johns Hopkins Bloomberg School of Public Health and the National Cancer Institute has developed a new algorithm for genetic risk-scoring for major diseases across diverse ancestry populations that holds promise for reducing health care disparities.
Fred Hutch to serve as national coordinating center for new Asian American, Native Hawaiian and Pacific Islander health studies
Fred Hutchinson Cancer Center will serve as the national coordinating center for a new epidemiological cohort study among Asian Americans, Native Hawaiians and Pacific Islanders (AsA-NHPI). Fred Hutch was awarded a seven-year, $38.7 million National Institutes of Health (NIH) grant to coordinate the effort to gather important health information on these populations, which are underrepresented in biomedical research.
Race-Neutral Testing Could Have Given Access to Life-Saving Lung Transplants for More Black Patients
Race-neutral lung function interpretation could increase access to lung transplants for Black patients with respiratory disease, according to new research published in the Annals of the American Thoracic Society online ahead of print.
Impact of racism and inequities on African Americans’ sleep and well-being
UCI professor of environmental and occupational health, Karen Lincoln, PhD, shares her expertise in health disparities affecting African Americans built upon the lived experience as an African American woman and through her interdisciplinary training at the Program for Research on African…
Disparities in Kidney Transplant Access Can Be Reduced Through a Multilevel Quality Improvement Effort
An academic medical center in Charleston, South Carolina, was able to significantly improve access to kidney transplants for African Americans by streamlining and standardizing the evaluation process, according to research published in the Journal of the American College of Surgeons.
KidneyX Launches New Artificial Kidney Prize with $10.5 Million in Funding
Today, the US Department of Health and Human Services (HHS) and the American Society of Nephrology (ASN) announced a new prize competition from the Kidney Innovation Accelerator (KidneyX) that seeks to further the development of a fully functional bioartificial kidney.
50 Years of Progress in Women’s Health
Debates over women’s health have long been contentious, but have also resulted in significant improvements in areas like equitable access to health care and survivorship. But the overall picture remains far from perfect. For example, the United States still has…
Researchers find COVID-19 mother-to-newborn infection rates are low, but indirect risks exist
Study reveals that, while mother-to-newborn transmission of the virus is rare, newborns of expectant mothers with COVID-19 can suffer indirect adverse health risks as a result of worsening maternal COVID-19 illness.

Exploring Racial and Ethnic Disparities in Colorectal Cancer Screening among Patients with Diabetes
Researcher at Rutgers Cancer Institute of New Jersey and Rutgers Robert Wood Johnson Medical School has received $400,000 in awards to help identify and overcome multi-level factors such as patient, health professionals and clinic systems affecting optimal use of colorectal cancer preventative screening options for patients with elevated medical and social risks throughout the United States.
Survey reveals racial, political differences in COVID-19 responses
A study from Michigan State University that found in spite of Black Americans’ attitudes toward proper precautions, they are disproportionately impacted by the pandemic and White people are less likely to fall ill.
Leading Health and Cancer Advocacy Groups Unite to Reduce Racial Disparities in Cancer Care
The National Comprehensive Cancer Network (NCCN), American Cancer Society Cancer Action Network (ACS CAN) and the National Minority Quality Forum (NMQF) presented new ideas for overcoming inequality in oncology. The recommendations address how medical systems often disproportionately fail minority patients.

Black dean of UAB School of Medicine able to discuss COVID health inequities, vaccine hesitancy in minority populations
Selwyn Vickers, M.D., dean of the University of Alabama at Birmingham School of Medicine and leading expert in health disparities and inequities, is able to comment on: Why minority populations are experiencing vaccine hesitancy How minority populations have disproportionately been…
Health Disparities and COVID-19, Toxicity of E-cigarette Generated Aerosols, and More Featured in February 2021 Toxicological Sciences
Toxicological Sciences continues to feature leading toxicology research in the areas of developmental and reproductive toxicology; endocrine toxicology; neurotoxicology; molecular, biochemical, and systems toxicology; and more.
Addressing health disparities in diabetes requires a broader look at systemic racism
Poor social conditions caused by systemic racism contribute to health disparities in people with diabetes, according to a paper published in the Endocrine Society’s Journal of Clinical Endocrinology & Metabolism.

Dean Appointed to Committee on Health Equity
Rutgers School of Public Health dean, Perry N. Halkitis, has been appointed to the American Psychological Association’s inaugural Ad Hoc Committee on Health Equity.
Closing the Racial Disparity Gap in Survival After In-Hospital Cardiac Arrest
In-hospital cardiac arrests (IHCA) represent catastrophic and often terminal events. Despite investments to improve the quality of resuscitation efforts, fewer than 25% of all patients that experience cardiac arrests in hospitals survive to discharge, and survival varies significantly across hospitals and by race. Until now, few have been able to specify reasons for the between-hospital differences.
Found: a genetic link to molecular events that precede symptoms in Alzheimer’s disease
Tufts researchers find a key mutation causing abnormal transport of BACE1, the enzyme responsible for processing the Alzheimer’s disease-linked amyloid protein. Identification of this mutation, which is more common among African Americans with Alzheimer’s, may allow early intervention.

Study Compares Racial Disparities in Unilateral Vs. Bilateral Knee Replacement
Analyzing data from the NIS – Healthcare Cost and Utilization Project database, HSS researchers found that African Americans were much less likely to undergo bilateral knee replacement compared to white patients. With respect to in-hospital complication rates, there was no significant difference.
Black individuals bear heavy burden of COVID-19 mortality, but key geographic disparities in health determinants exist
A new study published in the Mayo Clinic Proceedings: Innovations, Quality & Outcomes by University of Alabama at Birmingham researchers showed that Black individuals have a disproportionately higher COVID-19 mortality burden across all of the United States, which is driven by a high incidence of COVID-19 infection. They found that there are key geographic differences in the distribution of health determinants and COVID-19 mortality patterns.

Dr. Taison Bell Honored for Working to Transform Healthcare
For his work battling COVID-19 and his efforts to address racial health disparities, Business Insider has named UVA Health’s Taison Bell, MD, MBA, one of “30 Leaders Under 40 Changing Healthcare.”
Effects of poverty on childhood development seen in children as young as 5
How kindergarten teachers helped UCLA researchers highlight the impact of socioeconomic barriers on children’s health and development.
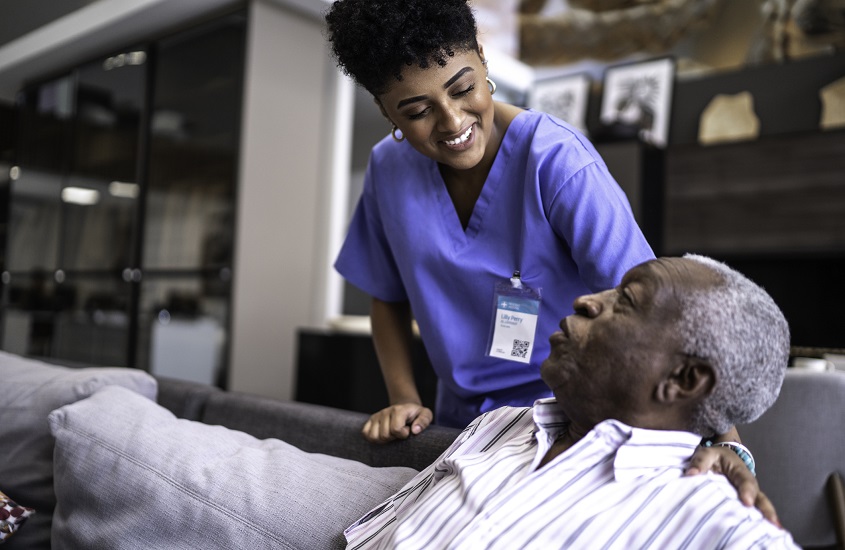
Rush Receives $3.5 Million in Funding to Address Behavioral Health Disparities in Older Adults
As the Rush Center for Excellence in Aging continues its commitment to improving the health of older adults, others are taking notice. Rush was designated a Center of Excellence Behavioral Health Disparities in Older Adults by the federal Substance Abuse and Mental Health Services Administration.
Income Tied to Health Disparities in Chicago Parents
In Chicago, only 36 percent of parents with low household income reported being in better health, compared to 57 percent of parents with low to middle income and 75 percent of parents with high income, according to a survey released by Ann & Robert H. Lurie Children’s Hospital of Chicago and the Chicago Department of Public Health (CDPH).
Historical Racial & Ethnic Health Inequities Account for Disproportionate COVID-19 Impact
A new Viewpoint piece published online in the Annals of the American Thoracic Society examines the ways in which COVID-19 disproportionately impacts historically disadvantaged communities of color in the United States, and how baseline inequalities in our health system are amplified by the pandemic. The authors also discuss potential solutions.
Center for Asian Health Equity awarded $4.25 million CDC grant to prevent colorectal cancer in Illinois
The University of Chicago Medicine’s Center for Asian Health Equity has received a five-year, $4.25 million federal grant to increase colorectal cancer screenings, particularly among underserved and rural Illinois communities.
COVID-19 and Health Equity: Time to Think Big
Authors of a new perspective on health inequities say that, in addition to health policy and individual-level efforts, social policy solutions are needed. They identify two key lessons from the pandemic: public policy enables public health and health equity requires big investments in public policy.
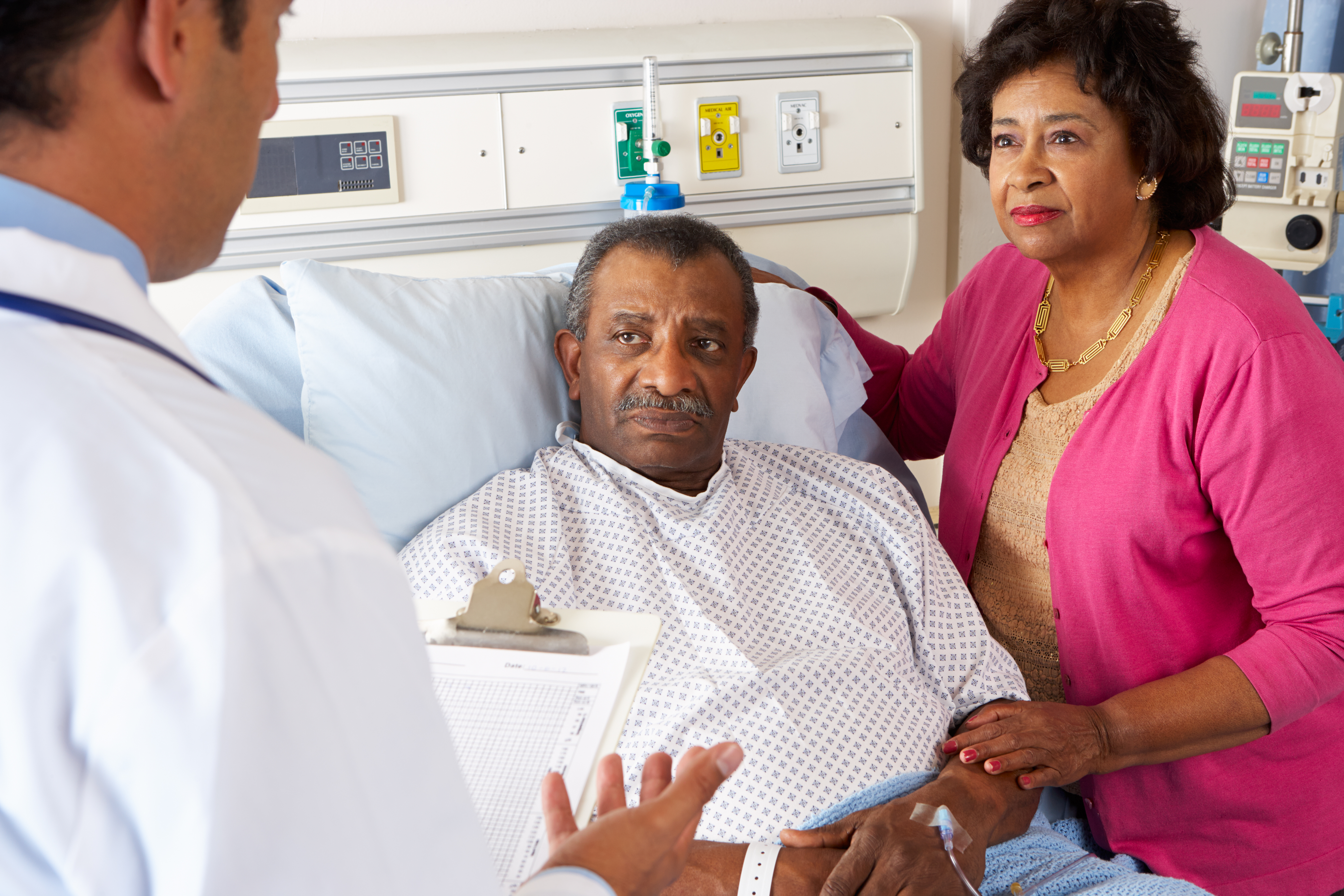
Black Individuals at Higher Risk for Contracting COVID-19, According to New Research
Results of an analysis published in the Annals of the American Thoracic Society found that Black individuals were twice as likely as White individuals to test positive for COVID-19. The average age of all participants in the study was 46. However, those infected were on average 52 years old, compared to those who tested negative, who were 45 years old on average.
Medicare’s Race, Ethnic Data Often Undercounts Minority Populations, Study Finds
Information critical to a nationwide priority of reducing health care disparities among minorities is incomplete and inaccurate, according to a new Rutgers study
Study: Identifying Optimal Points of Intervention to Address Racial and Ethnic Disparities in COVID-19 Fatality Rates in New York State
Results from a new COVID-19 epidemiological study have been released from the University at Albany in partnership with the New York State Department of Health (NYSDOH); the findings were published today in the peer-reviewed journal, Annals of Epidemiology.
CHOP’s Center for Applied Genomics Receives Funding to Study Risk of Disease Specifically in African Americans
The National Institutes of Health (NIH) announced today that researchers from Children’s Hospital of Philadelphia (CHOP) are among the recipients of a multi-million dollar grant that focuses on the use of genomics to improve risk assessment for diverse populations and integrate the findings into clinical care.
NYC Subway Data Reveals Communities of Color Carry the Burden of Essential Work and COVID-19
A new study shows there was substantial social distancing inequalities throughout New York City during the COVID-19 pandemic. Researchers reported that areas with the lowest individual income and a greater percentage of non-white and/or Hispanic/Latino individuals, used the subway to a greater degree during the pandemic, and the strongest driver of subway use in communities of color was the percent of individuals in essential work. This is one of the first studies to assess the interrelationship between sociodemographic factors, mobility, and COVID-19. Findings are online in the preprint of medRxiv ahead of peer-reviewed publication.

New Georgetown Report Highlights Health Disparities and Calls for Racial Equity in the District of Columbia
Approximately three quarters of the deaths associated with COVID-19 in the nation’s capital have been among the African American community. A new Georgetown University report illuminates entrenched health and socioeconomic disparities that explain one reason this is occurring. Main points:
• 15-year difference in the life expectancy between residents in Ward 3 and Ward 8;
• Residents from Wards with more Black residents (5, 7, and 8) more likely hospitalized for preventable health conditions;
• Number of Blacks who are obese is 3x higher than Whites;
• Number of Blacks with diabetes is 7x higher than Whites;
• Number of Blacks who die from heart disease is 2.5 times higher than Whites;
• Median household income is 3x less for Blacks; and
• Blacks have the lowest percentage of bachelor degree attainment.
Study: Critical Care Improvements May Differ Depending on Hospital’s Patient Population
A new study led by researchers at Beth Israel Deaconess Medical Center reveals that while critical care outcomes in ICUs steadily improved over a decade at hospitals with few minority patients, ICUs with a more diverse patient population did not progress comparably.
Researchers begin major study aimed at improving health equity in New Jersey
The New Jersey Population Health Cohort Study, now in the design phase, will collect biometrics, survey responses and other granular data over time on major outcomes such as stress, resilience, trauma and cognitive function from a broad cross-section of the population across multiple generations, with additional targeting of low-income residents and diverse immigrant groups.