The uninsured rate in Missouri has dropped significantly, according to a new analysis by the Center for Advancing Health Services, Policy & Economics Research at Washington University in St. Louis.
Tag: Medicaid
20-Week Ultrasound in Pregnancy is a Key Driver of Disparities in Prenatal Diagnosis of Congenital Heart Defects
Patients insured by Medicaid are less likely to get prenatal diagnosis of heart defects than those with private insurance, and this disparity can be partly attributed to lower rates of 20-week ultrasound in pregnant people with public insurance, according to a study led by Ann & Robert H. Lurie Children’s Hospital of Chicago in collaboration with Advocate Christ Children’s Hospital. The study was published in the journal Prenatal Diagnosis.
UC Irvine-led study finds inconsistent state-by-state vision care coverage
UC Irvine led study delves into the state-by-state Medicaid policies during the calendar year 2022, examining how these policies affect adult vision care coverage. Providing comprehensive vision care could have big benefits in terms of health, quality of life, and even employment and productivity.
UCLA selected by Centers for Medicare & Medicaid Services to test Medicare dementia care model
UCLA has been selected by the Centers for Medicare & Medicaid Services (CMS) to participate in a new Medicare alternative payment model designed to support people living with dementia and their caregivers.
Machine learning algorithm identifies individuals who experience the largest reduction in depression risk from Medicaid coverage
Previous research has demonstrated that Medicaid coverage reduces the risk for developing depression among recipients, but the question is who benefits most from coverage. Using a tool called machine learning causal forest to analyze data from the Oregon Health Insurance…
As Medicaid ‘unwinding’ continues and more states expand eligibility, Michigan report provides key insights
At a pivotal time for Medicaid health coverage for Americans with low incomes, a report on the impacts of Michigan’s Medicaid expansion shows very positive effects, as well as opportunities for continued improvements.
Few children – especially those with safety-net insurance – get vision checked at checkups
Less than a third of children have gotten their vision checked in the past year at their regular primary care clinic, a new study finds. Rates of eyesight screening in kids vary widely by insurance status.
Research Explores Patient Experience of North Carolina’s Medicaid Transition
In 2021, 1.6 million Medicaid beneficiaries in North Carolina moved from a fee-for-service Medicaid model to a managed care system known as N.C. Medicaid Managed Care. What impact did the transition have on Medicaid enrollees who live in Forsyth County?
George Washington University Launches Medicaid Workforce Tracker
To improve access to high-quality Medicaid services, experts must first locate the gaps in healthcare providers available to patients who rely on this health insurance. Researchers at the George Washington University today launched an interactive online tracking system that identifies states and counties in the United States that suffer from a shortage of primary care providers who see Medicaid patients.
Expanding Medicaid improved care without crowding out other patients
People with low incomes who live in states that expanded Medicaid got more of the kind of health care that can keep them healthier in the long run, compared with similar people in non-expansion states.
New Study Shows Medicaid Expansion Associated With Increase in Palliative Care for Patients With Advanced Cancers
More people with advanced cancers in the United States received critical palliative care services, according to new findings by researchers at the American Cancer Society. Medicaid expansion under the ACA was associated with the largest increases in palliative care use.
Patients With Alzheimer Disease, Dementia Face 2x Risk of Dying After ICU Discharge
Older adults with Alzheimer disease and related dementia who were admitted to an ICU were much less likely to be discharged home and faced almost twice the risk of dying soon after discharge and within the 12 months afterward.
Joint Statement on Behalf of Health Policy Deans, Scholars, and the American Public Health Association
On June 8, in a 7-2 decision authored by Justice Jackson, the US Supreme Court upheld the legal rights of millions of Medicaid beneficiaries, preserving those rights against unlawful action by state officials and thereby preserving access to health care for millions of vulnerable Americans. The nation’s largest public insurer, Medicaid entitles the poorest and most vulnerable children and adults to comprehensive health coverage and represents the nation’s single largest health care investment in public health.
UC Irvine-led study finds Medicaid telemedicine coverage boosted use, healthcare access
Medicaid telemedicine coverage between 2013 and 2019 was associated with significant growth in telemedicine use and improved healthcare access, while private policies did not have such an association, according to a study led by the University of California, Irvine. An analysis of 20,000 records of U.
Medicaid Reform Lies at the Heart of Efforts to Address the US Maternal Health Crisis
Medicaid must be part of any solution to address the current maternal mortality crisis and racial inequities in the United States, according to a new analysis by researchers at the George Washington University.
NJ Medicaid Reforms Tied to Increased Use of Opioid Addiction Treatment
Rutgers study shows higher number of caregivers prescribing buprenorphine
11 things to know now that COVID-19 isn’t an “emergency” anymore
Life has changed forever because of COVID-19. And the virus is still spreading, and still causing serious illness or significant disruption of ‘normal’ life. But when the clock strikes 11:59 p.m. on May 11, some of the special rules and programs put in place during the past three years will end. Here’s a guide.

Pandemic-era Medicaid benefits expire, expert explains economic impact
Medicaid benefits were expanded during the COVID-19 pandemic to cover low-income patients without a need for them to prove their eligibility or to reapply. At the end of March, those benefit expansions expired, and states have begun reviewing the Medicaid rolls to remove those who do not qualify, a process that could create new hardships for millions of Americans.
Achieving Prevention and Health, Rather Than More Healthcare
If more people have access to health insurance, we have to be sure the death rates of those with certain chronic conditions are decreasing.
Medicaid Expansion Reduced Black-White Disparities in Preventable Hospital Visits
Improving access to care for underserved communities improved a crucial health measure.
Paying Family Members for At-Home Medical Care of Their Children Found to Be a Viable Answer to Healthcare Worker Shortage
A recent study found that a Medicaid program in Colorado can help address the shortage of home healthcare workers for children with complex medical needs by offering family members certified nursing assistant (CNA) training and paying them for at-home medical care their child requires. Results show that children who received family-CNA care were not more likely to be hospitalized than children cared for by a non-family CNA. Children with family-CNA caregivers also experienced greater care continuity since turnover was not an issue as it tends to be with traditional home healthcare workers. Findings were published in the Journal of Pediatrics.
Medicaid expansion improves childhood cancer survival
Medicaid expansion may improve outcomes for children with cancer, finds a new analysis from the Brown School and Washington University School of Medicine in St. Louis.
Nearly Half of Children on Medicaid Lack Outpatient Follow-up Within a Month After Emergency Care for Mental Health
Only 56 percent of Medicaid-enrolled children received any outpatient follow-up within 30 days after discharge from the Emergency Department (ED) for a mental health concern, according to a large study published in the journal Pediatrics. Rates of timely follow-up among Black children were particularly low, with 10 percent fewer receiving an outpatient mental health appointment within 30 days compared to white children.
Medicaid Expansion in Southern States Associated with Earlier and More Comprehensive Breast Cancer Treatment
Patients in Southern states that expanded Medicaid were less likely to be uninsured and diagnosed with stage IV cancer.
Health insurance changes are coming – don’t get caught without coverage
Now that the pandemic has eased up, and jobs are easier to find, an emergency order regarding Medicaid and CHIP enrollment will end on March 31, 2023. Some people are calling it an “unwinding.” This means that everyone in these programs will have to prove they are still eligible for their coverage if they want to keep it.
American College of Rheumatology: Proposed Rule Will Bring Great Transparency to Medicare Advantage Prior Authorization
The American College of Rheumatology said the Centers for Medicare and Medicaid Services’ Advancing Interoperability and Improving Prior Authorization Proposed Rule will bring greater transparency, reduce administrative burden, & make turnaround on prior authorization more predictable for payers.
“Sandwich generation” study shows challenges of caring for both kids and aging parents
Their older parents need care. Their kids are still under 18. And they probably have a job, too. They’re the “sandwich generation” – a longtime nickname for the mostly female, mostly middle-aged group of Americans who serve as caregivers for both older and younger family members at once. A new study estimates there are at least 2.5 million of them, while giving a detailed view into who they are, and which older adults rely on them.
Medicaid used as primary source of insurance coverage for more than half of participants
A study of more than one million Medicaid beneficiaries has found that more than half were enrolled in Medicaid for at least a decade and experienced substantial lapses in coverage.
Homelessness, hospitals and mental health: Study shows impacts and costs
A new study that harnesses a new form of data on hospital patients’ housing status reveals vast differences in diagnoses between patients with and without housing issues who are admitted to hospitals. This includes a sharp divide in care for mental, behavioral and neurodevelopmental conditions.
Study compares adverse events after two types of bariatric surgery in adolescents
Adolescents who underwent sleeve gastrectomy, a type of weight-loss surgery that involves removing part of the stomach, were less likely to go the emergency room in the five years after their operations than those who had their stomachs divided into pouches through gastric bypass surgery, according to new research.
Study Finds Persistent Disparities in Access to Prenatal Care Among Pregnant People Based on Citizenship Status and Education Level
Findings suggest exclusions to Medicaid because of immigration status may increase risk for maternal health care disparities in some immigrant populations
Ochsner Health Reveals New Findings: Digital Health Pilot Dramatically Improves Outcomes for Medicaid Patients Battling Chronic Diseases, Among First to Do So
The statistically and clinically significant results of the pilot program– one of the first in the country – showed that enrollment in Ochsner Digital Medicine brought nearly half of all out-of-control Hypertension patients under control at only 90 days.
Amicus Brief Urges High Court to Preserve Legal Rights for Medicaid Beneficiaries
WASHINGTON (October 10, 2022)–A case that could bar Medicaid beneficiaries from access to the federal courts when states violate their rights could put millions of beneficiaries at risk, according to a public health amicus brief submitted to the Supreme Court.…
New Transitional Care Clinical Pathway Improves Health Equity
People with multiple chronic conditions require complex care management and often experience significant challenges when transitioning from hospital to home. This is especially true for people insured by Medicaid who are disproportionately Black, Indigenous, People of Color (BIPOC) and experience higher chronic disease burdens and adverse outcomes following hospitalization. For them, comprehensive transitional care support is a paramount, yet often absent aspect of care delivery that may result in health inequities.
For Medicaid-Insured Patients with Cancer, Health Insurance Does Not Always Mean Health Access
Although there has been a significant increase in the number of U.S. residents insured through Medicaid since the expansion of the Patient Protection and Afforadble Care Act (ACA) in March 2010, the ability of Medicaid-insured patients to access cancer care services has not been well understood. In a study published today in the journal JAMA Network Open, researchers at Yale Cancer Center assessed the acceptance of Medicaid insurance among patients diagnosed with common cancers.
Interventions based on social needs may reduce hospitalizations, health care use
A randomized study of adult Medicaid patients suggests that social program-based interventions for housing, food security, and transportation may reduce inpatient admission rates by 11 percent and emergency department visits by 4 percent. However, health care savings based on these interventions may not cover the cost of social the social programs. The findings are published in Annals of Internal Medicine.
New Study Finds Medicaid Expansion Increases Survival in Newly Diagnosed Cancer Patients
A new large study led by researchers at the American Cancer Society (ACS) shows Medicaid expansion under the Affordable Care Act (ACA) was associated with an increase in two-year overall survival rates among patients newly diagnosed with cancer, especially among non-Hispanic Black people and people living in rural areas.
STUDY FINDS DECREASE IN RACIAL DISPARITY AND INCREASE IN SURVIVAL RATES IN METASTATIC BREAST CANCER PATIENTS DUE TO MEDICAID EXPANSION
Findings from Study Led by Susan G. Komen Scholars Published in JAMA Oncology
Medicaid health plan community health workers have positive impact on care
Community health workers employed by Medicaid health plans can help low-income people who face barriers to care rely less on the emergency room, and more on outpatient care, a new study finds.
Medicaid Expansion of Dental Care Can Increase Access
When Medicaid expands its dental coverage, by increasing the types of procedures it covers and the total amount a dentist can spend on an individual patient, more dentists will locate to the expansion areas, thereby increasing access.
Aging U.S. Immigrant Population Poses Challenges to State Health Care Systems
A team led by Dr. Arturo Vargas Bustamante, UCLA Fielding School of Public Health professor of health policy and management and director of faculty research at the UCLA Latino Policy and Politics Initiative (LPPI), has found the United States faces a potential crisis in terms of health care for documented, and undocumented immigrants.
New Report Offers National Blueprint for Strengthening Family Planning Services in Medicaid Managed Care
A new report by researchers at the George Washington University lays out a blueprint for policies that can strengthen family planning for millions of Medicaid beneficiaries enrolled in Medicaid managed care.

Health Policy Researchers Propose Filling Health Care Coverage Gap to Help ‘Near Poor’
“Near-poor” Americans – people just above the federal poverty level but still well below the average U.S. income – who rely on Medicare for health insurance face high medical bills and may forgo essential health care, according to new research.
Medicaid expansion made many mouths healthier, study finds
As the pandemic’s economic effects drive more people to enroll in Medicaid as safety-net health insurance, a new study suggests that the program’s dental coverage can improve their oral health in ways that help them seek a new job or do better at the one they have.
Medicaid Compelled Work Experiments Represent an Abuse of Research Authority, Have Stripped Thousands of Eligible People of Coverage
A public health “friend of the court” brief filed with the U.S. Supreme Court urges the highest court of the land to uphold lower court decisions that blocked Medicaid work requirements in Arkansas and New Hampshire.
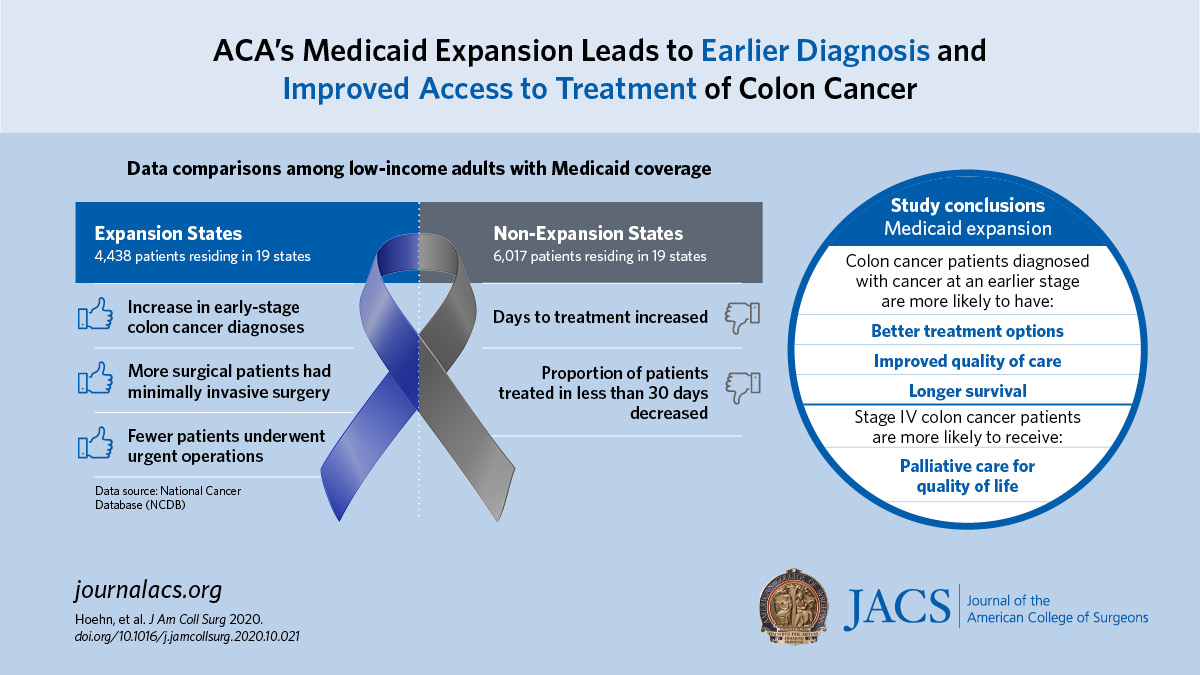
Medicaid expansion may result in earlier diagnosis and improved access to treatment of colon cancer
The Affordable Care Act’s Medicaid expansion for low-income people appears to lead to earlier diagnosis of colon cancer, enhanced access to care, and improved surgical care for patients with this common cancer.

Increase in Early-Stage Cancer Diagnoses Tied to ACA’s Medicaid Expansion, Pitt Study Finds
The study showed that health insurance expansions increased early-stage cancer diagnoses, while rates of late-stage cancer decreased.
What’s at stake in the Supreme Court’s ACA case? A quick explainer
Though the election and pandemic have eclipsed it in the news, there’s another event unfolding that could affect nearly all Americans: a Supreme Court case that will decide the future of the Affordable Care Act. A health policy researcher explains what would happen if it’s overturned.

Healthy Indiana Plan, shared data improve Medicaid enrollment, IUPUI study finds
In a new study published in Health Affairs, researchers at IUPUI and the Indiana Family and Social Services Administration found that Medicaid enrollment occurred more frequently and more quickly for individuals impacted by the justice system after the Healthy Indiana Plan…
Medicaid expansion linked to lower mortality rates for three major types of cancer
In states that have expanded Medicaid availability as part of the Affordable Care Act (ACA), mortality rates for three major forms of cancer are significantly lower than in states that have not expanded their Medicaid, a new study by researchers at Dana-Farber Cancer Institute, Brigham and Women’s Hospital, and Harvard University shows.