A brief filed on behalf of 111 public health and health law and policy Deans and Scholars, the American Public Health Association, the Robert Wood Johnson Foundation, Trust for America’s Health, and ChangeLab Solutions highlights new findings on the preventive health gains at stake in Braidwood Management v Becerra.
Tag: Affordable Care Act
Medicaid Expansion Associated with Increased, But Not High Quality, Screening for Alcohol Use
People living in states with expanded Medicaid access were more likely to be screened by their doctor for alcohol use compared to people who lived in states that did not expand Medicaid access, but they did not necessarily receive effective interventions. A study published in Alcohol: Clinical and Experimental Research found that living in a state with expanded Medicaid access was associated with a higher prevalence of lower-income adults’ receiving some alcohol screening at a recent checkup but not receiving higher quality screening or brief counseling. The authors suggest that expanded Medicaid access may increase screening via increased access to primary care but that policies that target healthcare provider constraints are also needed to increase high-quality, evidence-based screening and counseling around alcohol use.
A freeze, or a fix? Preventive care coverage at a crossroads
Many types of preventive care have been available for years with no cost to the patient. But that provision now hangs in the balance, because of a court case. Two professors explain what’s at stake and why.
IU expert can discuss potential impact of Texas judge’s ruling on the Affordable Care Act
Last month, a federal judge in Texas ruled against a part of the Affordable Care Act that requires most insurers to cover preventive services that include screenings for cancer, diabetes and mental health. Kosali Simon, an expert on the Affordable…
Study Finds Persistent Disparities in Access to Prenatal Care Among Pregnant People Based on Citizenship Status and Education Level
Findings suggest exclusions to Medicaid because of immigration status may increase risk for maternal health care disparities in some immigrant populations
Expert on out-of-pocket health costs available to comment on Texas court ruling overturning free preventive care
For more than two decades, A. Mark Fendrick, M.D., has studied how the amount of money a patient has to pay out of their own pocket for health care affects the amount and type of care they receive. He is…
@MTSU Healthcare Operations Expert Richard Tarpey Breaks Down SCOTUS Decision to Dismiss Challenge to the #AffordableCareAct
Richard Tarpey, assistant professor of management, in Middle Tennessee State University’s Jones College of Business, examines the U.S. Supreme Court recent decision to dismiss a challenge to the Affordable Care Act. In turning away a challenge from Republican-led states and the former…
Law, health economics experts available to comment on U.S. Supreme Court decision to uphold the ACA
This morning, the U.S. Supreme Court ruled 7-2 that the red states and two individuals who challenged the Affordable Care Act do not have legal standing to dispute the constitutionality of the law’s individual mandate to buy health insurance and…
Endocrine Society celebrates Supreme Court decision to uphold the Affordable Care Act
The Endocrine Society today praised the U.S. Supreme Court’s decision to uphold the Affordable Care Act, which makes health care accessible to millions of individuals nationwide, including those with hormone health conditions such as diabetes, osteoporosis, thyroid conditions, and breast and prostate cancer.
A few hundred dollars makes a difference in use of long-lasting birth control
Getting a birth control implant used to cost some women hundreds of dollars, especially if they had a high-deductible health plan. A new study shows the impact of the Affordable Care Act’s no-cost birth control provision, and the potential impact of a Supreme Court ruling allowing employers to opt out.
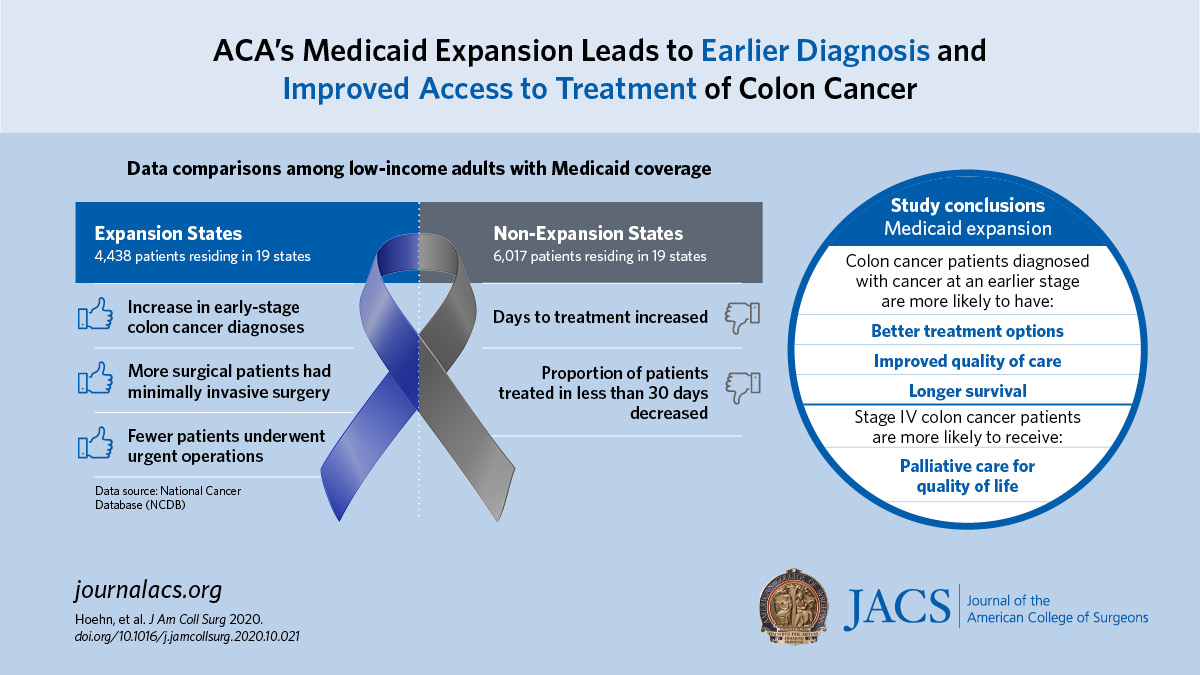
Medicaid expansion may result in earlier diagnosis and improved access to treatment of colon cancer
The Affordable Care Act’s Medicaid expansion for low-income people appears to lead to earlier diagnosis of colon cancer, enhanced access to care, and improved surgical care for patients with this common cancer.
Medicaid Expansion Increased Early Cancer Detection, New Study Finds
States where Medicaid was expanded under the Affordable Care Act have seen a measurable increase in the early detection of cancer and reduced late-stage cancer incidence, according to the results of a new study published in the current issue of the American Journal of Preventive Medicine.

Increase in Early-Stage Cancer Diagnoses Tied to ACA’s Medicaid Expansion, Pitt Study Finds
The study showed that health insurance expansions increased early-stage cancer diagnoses, while rates of late-stage cancer decreased.
Legal challenge to Affordable Care Act threatens women’s reproductive health care
The Affordable Care Act has improved women’s reproductive health care, but a looming legal challenge threatens those gains. On Nov. 10, the Supreme Court is scheduled to hear arguments in California v. Texas, which challenges the constitutionality of the ACA.
Biden focuses on health care, but pharma firms have upper hand
President-elect Joe Biden began transition planning with the announcement of a COVID-19 task force, continuing a focus on health care that was a hallmark of the Obama-Biden era, culminating in the passing of the Affordable Care Act. Colleen Carey,…
Underinsured Transgender Americans More Likely to Turn to Riskier Sources for Gender-Affirming Hormones
People who are transgender and lack access to insurance coverage for gender-affirming hormone therapy are more likely to turn to sources other than a licensed health care provider, a new Michigan Medicine-led study finds.
Expanded Birth Control Coverage May Help Reduce Disparities in Unplanned Pregnancies
Removing out-of-pocket costs for contraception may help reduce the income-related disparities that play such a significant role in unintended pregnancies, a new Michigan Medicine-led study suggests.

With Affordable Care Act’s future in the balance, U-M holds 10th anniversary discussion with national experts
A free online event featuring health policy experts will explore the past, present and future of the Affordable Care Act
Rutgers Expert Available to Discuss Supreme Court Ruling Limiting Birth Control Coverage Under Obamacare
Professor Lena Merjanian, a reproductive health expert and gynecologist at the Rutgers Robert Wood Johnson Medical School, is available to comment on the Supreme Court ruling that allows employers with religious or moral objections to deny women birth control coverage…
ASCO 2020: First National-Scale Study on the Impact of Medicaid Expansion on Cancer Mortality Rates Highlighted in Press Program
New data from researchers at Memorial Sloan Kettering Cancer Center (MSK) revealed the effects of Medicaid expansion on cancer death rates on a national scale. The landmark study found that states that adopted Medicaid expansion following the passage of the Affordable Care Act (ACA) in 2010 saw greater decreases in cancer mortality rates than states that did not. The findings were presented as part of the press program for this year’s virtual annual meeting of the American Society of Clinical Oncology (ASCO).
Endocrine Society opposes Administration’s effort to roll back protections for transgender health
The Endocrine Society is alarmed by the Administration’s proposed rule to roll back protections for transgender individuals and narrow the scope of the Affordable Care Act (ACA), especially during the COVID-19 pandemic, when everyone needs access to health care. The Society calls on the Administration to maintain access to care protections for all, particularly vulnerable populations.
Obamacare buffering bankruptcy risk, new study shows
A decade after President Barack Obama signed the Patient Protection and Affordable Care Act, more people are fully insured, fewer are uninsured and people who lose their insurance intermittently are no longer at greater risk of bankruptcy, according to a new University of Colorado Boulder study.
Medicaid expansion led to more insurance coverage and a higher rate of mammograms in seven states
In states that chose to expand Medicaid under the Affordable Care Act (ACA), lower-income women now have access to mammograms at a higher rate than in states that did not expand Medicaid coverage.
DePaul University experts available to discuss recovery, life after the COVID-19 pandemic
Recovery. Reentry. Reopen. Return. A new normal. Faculty experts at DePaul University are available for news media interviews about what comes next — after the COVID-19 pandemic. Does the world return to normal or will there be fundamental changes to how we live our lives, work, and travel; and how we are governed?

ACA has helped protect low-income patients from catastrophic spending for surgery
n the years after 2014, when the Affordable Care Act’s health insurance marketplaces were established, low-income patients who underwent a surgical procedure saved an average of $601 in out-of-pocket spending and $968 in premium spending per year, compared to before the marketplaces existed. Those low-income patients also had a 35% lower chance of having catastrophic levels of household medical spending.
However, for middle-income patients, spending levels were about the same before and after the marketplaces began.

Affordable Care Act helped make health insurance access more equal, but racial and ethnic gaps remain
As the Affordable Care Act turns 10, a new study shows it has narrowed racial and ethnic gaps in access to health insurance – but definitely not eliminated them.
Both the percentage of people 19-64 who lacked health insurance, and the size of the health insurance gap between white, African-American and Hispanic Americans, shrank. From 2013 to 2017, the gap between blacks and whites narrowed 45%, and the difference between Hispanics and whites narrowed 35%.
Study Finds ‘Far-Reaching’ Impact from Affordable Care Act
[Embargoed to March 2, 2020 @ 4 p.m. (ET). ] By 2008, when President Obama was first elected, the rate of uninsurance in the U.S. had been steadily deteriorating: nearly 56 million Americans reported they had no health insurance for…
White House health communications & ethics expert – COVID-19 response
Peter Loge is an expert in political communication relating to public health initiatives and is the director of the Project on Ethics in Political Communication at the George Washington University School of Media and Public Affairs. Loge can discuss the…
Visits to Pediatricians on the Decline
Commercially insured children in the U.S. are seeing pediatricians less often than they did a decade ago, according to a new analysis led by a pediatrician-scientist at the University of Pittsburgh and UPMC Children’s Hospital of Pittsburgh.

Medicaid expansion doubled access to primary care, increased attention to health risks in Michigan enrollees
When Michigan expanded its Medicaid program to cover more low-income residents, its leaders built in special features to encourage enrollees to understand their health risks, and incentivize them to prevent future health problems, or find them early. According to two new studies, that effort has paid off.