In the first year after the sudden removal of a requirement that prescribers get special permission to prescribe medication for opioid addiction, a study finds more prescribers started providing it, but the number of patients receiving it didn’t rise very much.
Tag: Health Policy
University of Maryland, Baltimore Researchers Call for Regulation of Direct-to-Consumer Microbiome Tests
Burgeoning interest in the microbiome has led to a growing demand for direct-to-consumer (DTC) microbiome testing services.
Braidwood Management v Becerra Puts Over a Decade of Progress in Preventive Health Care At Risk
A brief filed on behalf of 111 public health and health law and policy Deans and Scholars, the American Public Health Association, the Robert Wood Johnson Foundation, Trust for America’s Health, and ChangeLab Solutions highlights new findings on the preventive health gains at stake in Braidwood Management v Becerra.
ISPOR Europe 2023 Plenaries and Speakers Announced
ISPOR—The Professional Society for Health Economics and Outcomes Research announced the plenary sessions and speakers for ISPOR Europe 2023. The conference is scheduled for 12-15 November in Copenhagen, Denmark with the theme, “Health Economics and Outcomes Research at the Nexus of Policy and Science.”
Real-world examples demonstrate how systems science can address health inequities
As researchers increasingly recognize that causes for health issues are structural and interrelated, real-world, innovative case studies demonstrate the value of applying systems science to evaluate health interventions and address health inequities as seen in a special supplement, supported by the W.K. Kellogg Foundation, in the October/December issue of Family & Community Health. The journal is published in the Lippincott portfolio by Wolters Kluwer.
Mapping the changing landscape of gender-affirming care for teens
Many families whose transgender children need gender-affirming care will need to drive much further than before because of laws and other actions passed since 2021 in 20 states, a new study shows. Half will need to drive an hour or more; 25% four hours each way.
Deep-dive on telehealth use in Michigan shows importance for mental, rural & out-of-state care
A new single-state report looks at patterns of telehealth use by people with different forms of insurance before and during the pandemic, and could inform post-pandemic health policy.
Expanding Medicaid improved care without crowding out other patients
People with low incomes who live in states that expanded Medicaid got more of the kind of health care that can keep them healthier in the long run, compared with similar people in non-expansion states.
NHS policies on patient’s weight and access to hip replacement surgery are inappropriate, study finds
Weight and body mass index (BMI) policies introduced by NHS commissioning groups in England are inappropriate and worsening health inequalities, according to a new study published in BMC Medicine today [13 June] that analysed nearly 490,000 hip surgeries. With one in ten people likely to need a joint replacement in their lifetime, many thousands of patients are directly affected by these policies.
Joint Statement on Behalf of Health Policy Deans, Scholars, and the American Public Health Association
On June 8, in a 7-2 decision authored by Justice Jackson, the US Supreme Court upheld the legal rights of millions of Medicaid beneficiaries, preserving those rights against unlawful action by state officials and thereby preserving access to health care for millions of vulnerable Americans. The nation’s largest public insurer, Medicaid entitles the poorest and most vulnerable children and adults to comprehensive health coverage and represents the nation’s single largest health care investment in public health.
New book sheds light on adult mortality in India
A new book provides an in-depth analysis of adult mortality patterns in India and addresses crucial issues related to public health and policy.
A freeze, or a fix? Preventive care coverage at a crossroads
Many types of preventive care have been available for years with no cost to the patient. But that provision now hangs in the balance, because of a court case. Two professors explain what’s at stake and why.
GW Experts Available to Discuss Key Issues for Pride Month
WASHINGTON (May 26, 2023)–June is designated as Pride Month in the United States to commemorate the 1969 Stonewall Uprising in Manhattan. The protests marked the beginning of the gay pride movement and helped launch a civil rights movement for LGBTQ+…
Widespread staff shortages exacerbate pressures facing radiation oncology clinics; ASTRO Advocacy Day calls for action
More than 9 in 10 radiation oncologists report that their practices face clinical staff shortages, according to a new national survey from the American Society for Radiation Oncology (ASTRO). More than half (53%) of the doctors said the shortages are creating treatment delays for patients, and 44% say they are causing increased patient anxiety.
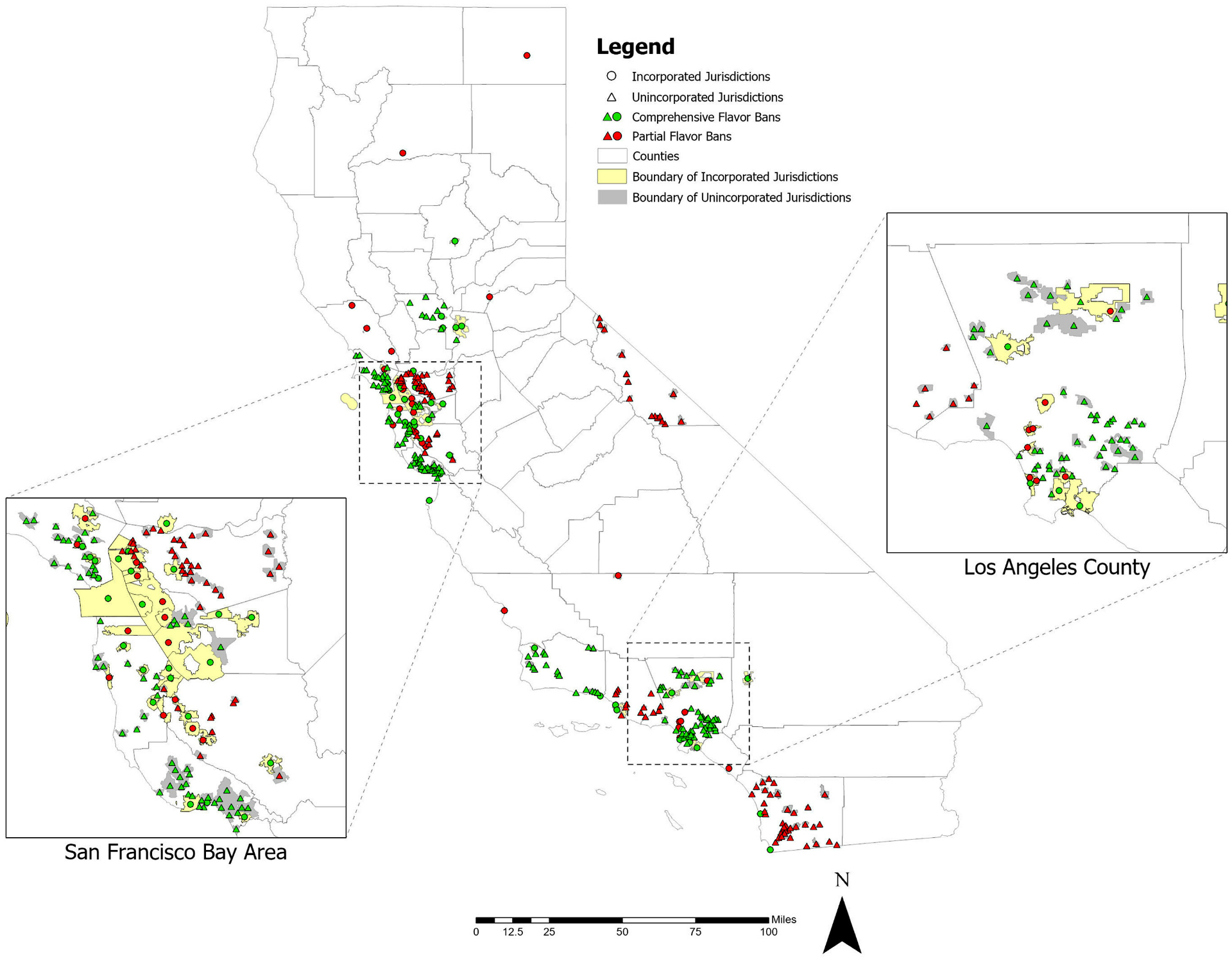
Study shows usage is lower in California areas that have a full ban on the sale of flavored tobacco products
Researchers from the University of California, Irvine found that residents of jurisdictions with a comprehensive sales ban have a 30% reduced odds of using flavored tobacco relative to those living in a jurisdiction without a ban. In contrast, lower use was not observed for residents of jurisdictions that enacted a partial sales ban.
Study Finds Hospitals’ Cash Prices for Uninsured Often Lower Than Insurer-Negotiated Prices
Two new studies led by researchers at the Johns Hopkins Bloomberg School of Public Health shed light on current U.S. hospital practices.
JMIR Research Protocols | What is the Role of Human Decision-making in an AI–driven Future in Health?
Australian researchers have established a set of protocols for a research project in JMIR Research Protocols that aims to explore whether humans will continue in meaningful decision-making roles in an AI-driven future.
Three Penn Medicine Faculty Members Named Hastings Center Fellows
Three faculty from the Perelman School of Medicine at the University of Pennsylvania have been named 2023 Hastings Center Fellows. Emily Largent, PhD, RN, Peter Reese, MD, PhD, and Dominic Sisti, PhD, are among 12 new Fellows joining an elected group of over 200.
Conference to tackle scope of health care uncertainties
With the aim to address key challenges impacting U.S. and global health care organizations, leaders representing every facet of the industry will converge for the 2023 “The Business of Health Care Conference,” to be held Feb. 24 at the University of Miami Coral Gables Campus.
What was the true human cost of the pandemic in Russia?
A new study assesses the number of lives lost to the COVID-19 pandemic in Russia and introduces a novel methodology that will help to get a clearer view of pandemics in the future.
Organ Donations, Transplants Increase on Days of Largest Motorcycle Rallies
Analysis shows steep increases in organ donations, transplantations during large motorcycle rallies. The increase in organ donations and transplantations appears to be driven by well-documented increases in crash-related deaths during large motorcycle rallies.
Medically Tailored Meals Could Save U.S. Nearly $13.6 Billion Per Year
Expanding programs that make and deliver medically tailored meals to people with serious, diet-sensitive diseases could lead to fewer hospitalizations nationally and a net cost savings of approximately $13.6 billion each year, according to a new study led by Tufts University researchers.
New report highlights need for recruitment, retention of interventional radiologists to small and rural practices
A new report from a joint task force of the American College of Radiology and the Society of Interventional Radiology recommends improved access to interventional radiologists in small and rural areas.
Lessons learned from COVID-19 mitigation measures
Researchers analyzed how the expectation of a vaccine influences optimal lockdown measures during a pandemic.

Disparities in United States COVID-19 Vaccine Distribution
Health care facilities in Black metropolitan counties, Hispanic rural counties and hardest-hit counties were less likely to administer COVID-19 vaccines during initial rollout, UC San Diego study finds.
Telehealth by phone & video proves a lifeline for veterans with opioid addiction
Phone-based and video-based telehealth visits both helped veterans with opioid addiction stay on buprenorphine medication to treat their opioid use disorder during the pandemic. The findings could inform telemedicine policy.
UCSF Dermatologist Inaugurated as AMA President
Jack S. Resneck Jr., MD, was inaugurated today as the 177th president of the American Medical Association (AMA). Resneck is a dermatologist, professor and vice-chair of the Department of Dermatology at UC San Francisco. Following a year-long term as president-elect of the nation’s premier physician organization, Resneck today assumed the office of AMA president.
The US reaches 1 Million Deaths from COVID-19: GW Experts Available to Comment
The United States has reached 1 million reported deaths from COVID-19 and that number is likely an undercount, according to the Centers for Disease Control and Prevention. The George Washington University has a number of experts to comment on the…
Analysis: California Malpractice Cap on Noneconomic Losses Associated with 16% More Adverse Events
A new analysis suggests California’s cap on noneconomic losses in malpractice cases has fallen far behind present-day values, and may even be associated with an increase in malpractice cases over the past five decades.
UCI-led study investigates saliva testing for medication monitoring among patients with psychiatric disorders
Lithium is a common medication prescribed to patients with psychiatric disorders, namely bipolar disorder, schizophrenia, and depression. It is used as a mood stabilizer and lessens the intensity of manic episodes, with particular benefit in reducing suicidality. While highly effective, the drug requires routine blood monitoring, which can be uncomfortable, expensive, and inconvenient for patients who must travel to clinical labs for frequent blood testing.
Data collection, reporting gaps harm Native Hawaiian, Pacific Islander health, UCI-led study says
Despite Native Hawaiians and Pacific Islanders being one of the fastest growing populations, according to the 2020 U.S. Census count, the collection and reporting of their health data at the federal and state levels is virtually non-existent, according to a study led by the University of California, Irvine.
Looking at the Legal Ins and Outs of Vaccine Mandates
Johns Hopkins Carey Business School Associate Professor Stacey Lee, an expert in business law, health law, and negotiation, addresses some of questions raised by President Biden’s recent plans for increasing COVID-19 vaccinations.
Study finds recent change in EMS transport policy could improve stroke outcomes
A new EMS transport policy implemented in Chicago showed that sending patients suspected of experiencing large vessel occlusion directly to comprehensive stroke centers led to an increase in the use of endovascular therapy, an important treatment for acute ischemic stroke.
Hackensack Meridian School of Medicine and Seton Hall University Opioid Conference to Feature Addiction Experts Working to Combat National Crisis
The July 30 virtual conference is part of a three-year grant to train clinicians to prescribe medications to treat addiction.
Tracking COVID-19 across Europe
A COVID tracker developed by IIASA researcher Asjad Naqvi, aims to identify, collect, and collate various official regional datasets for European countries, while also combining and homogenizing the data to help researchers and policymakers explore how the virus spreads.
@MTSU Healthcare Operations Expert Richard Tarpey Breaks Down SCOTUS Decision to Dismiss Challenge to the #AffordableCareAct
Richard Tarpey, assistant professor of management, in Middle Tennessee State University’s Jones College of Business, examines the U.S. Supreme Court recent decision to dismiss a challenge to the Affordable Care Act. In turning away a challenge from Republican-led states and the former…
Though ‘unsurprising,’ U.S. Supreme Court decision on Affordable Care Act a relief for many
The United States Supreme Court’s decision to uphold the Affordable Care Act, also known as Obamacare, should not come as a total surprise despite the conservative efforts to invalidate the law, according to West Virginia University policy and legal experts.…
NCCN Policy Summit Explores How COVID-19 Pandemic Can Lead to Improvements in Cancer Care
NCCN Policy Summit examines the impact of the past year on oncology policy in the U.S., such as resuming recommended screening and clinical trials, applying health innovations from the COVID-19 pandemic to cancer treatment, and addressing systemic inequalities that lead to disparities in outcomes.
Scott Lee, MD, PhD, among group to earn Kenneth J. Arrow Award for health economics research
Scott Lee, MD, PhD, MPA, MPhil, assistant professor of Medicine at Vanderbilt University Medical Center, has received the Kenneth J. Arrow Award for health economics research given by the International Health Economics Association.
Community Health Centers Move to the COVID-19 Immunization Frontline
A new analysis from the Geiger Gibson/RCHN Community Health Foundation Research Collaborative provides current information on the number of community health center staff members and patients who have received COVID-19 vaccines, using data from the latest published Health Resources and Services Administration’s Health Center COVID-19 Survey. The Geiger Gibson/RCHN Community Health Foundation Research Collaborative is based at the George Washington University Milken Institute School of Public Health (GW Milken Institute SPH).

American Chiropractic Association Elects New Leadership
The American Chiropractic Association (ACA) installed a new leadership team on Feb. 5 during its annual meeting. Michele Maiers, DC, MPH, PHD, of Minneapolis, Minn., is the first woman elected as ACA president in the association’s 58-year history.
Paid maternity leave has long-term health benefits
A study of women who were new mothers in the late 1970s found that those who were given longer, paid maternity leave lived healthier lives as they entered middle age.
Adults with Cerebral Palsy Need Better Access to Health Care
Once viewed as a pediatric condition, patients with cerebral palsy are aging, but the health care system is not prepared to offer them the care they need.
Bipartisan House and Senate Majorities and Health Care Providers Urge Action to Stop Medicare Provider Cuts
Medicare cuts to a million health care providers, many reeling from the economic impact of COVID-19, may cause practice closings, service reductions, job losses and decreased access to care. With the cuts to start Jan. 1, nearly 400 medical organizations and 329 members of Congress are calling to #StopTheCuts

Penn Medicine mRNA Vaccine Technology Pioneer and Health Policy Experts Join Together to Discuss COVID Vaccine Emergency Use Authorization Plans
**All experts also available for interviews prior to event and EUA Advisory Committee Meetings**
**B-roll and lab photos of Drs. Weissman and Wherry shot this month, headshots of the others, and photos from Penn’s Moderna vaccine trial participants getting vaccinated, are available for use**
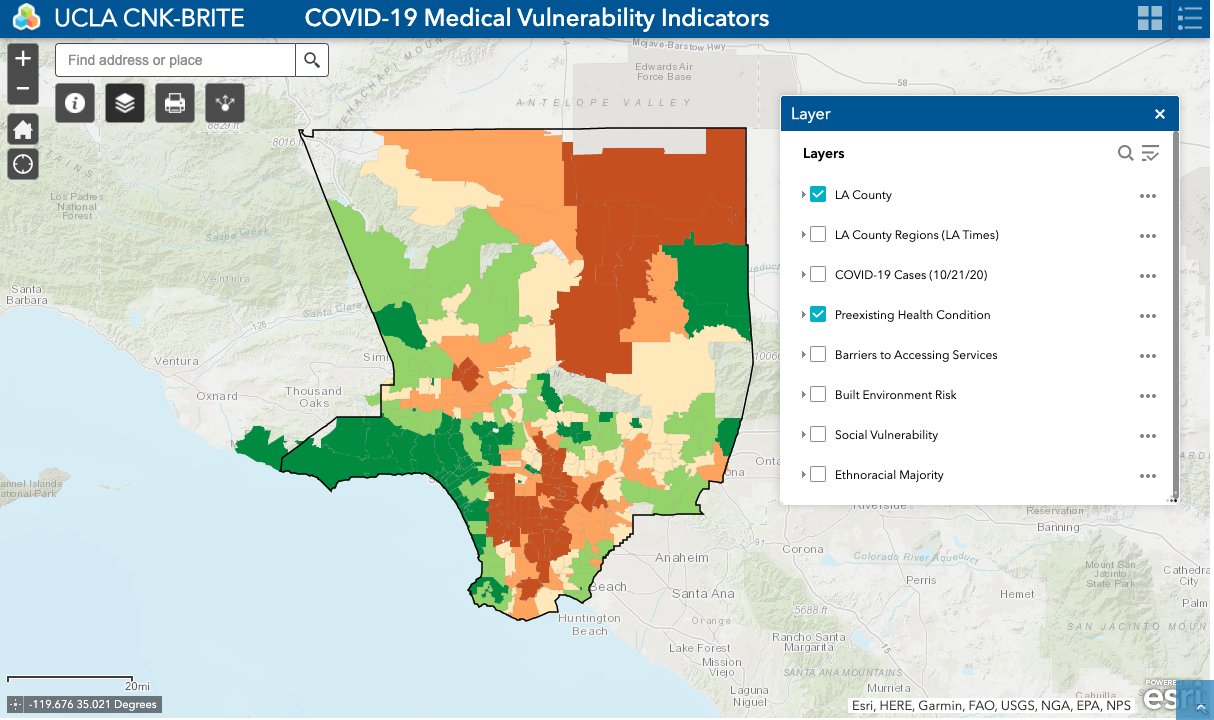
UCLA Model Identifies Neighborhoods That Should Have Priority for Vaccine, Other COVID-19 Help
To help slow the spread of COVID-19 and save lives, UCLA public health and urban planning experts have developed a predictive model that pinpoints which populations in which neighborhoods of Los Angeles County are most at risk of becoming infected.
Mount Sinai Researchers Find That Where People Live Can Impact Their Risk for Common Chronic Conditions Including High Blood Pressure and Depression
The researchers found that a persons’ place of residence substantially influences their risk of uncontrolled chronic disease including high blood pressure and depression

UCLA Fielding School of Public Health to host conference on addressing health care inequities
Health care leaders from across the United States will speak at an Oct. 14 event focusing on the critical intersection between social justice and health equity, including bridging gaps in the U.S. health care system and focusing on lessons learned from the COVID-19 pandemic response.
NCCN Policy Summit Explores How to Lower Costs for Cancer Care
NCCN Virtual Policy Summit features congressional staffers and representatives from CMS, COA, BIO, and others, discussing legislative and regulatory approaches for reducing health care costs.
Study examines racial and ethnic disparities among COVID-19 cases in Massachusetts
In a new study published in Health Affairs, researchers at Beth Israel Deaconess Medical Center (BIDMC) and the Harvard T.H. Chan School of Public Health examines the association between community-level factors and COVID-19 case rates across 351 cities and towns in Massachusetts between January 1 and May 6, 2020.