UCLA has been selected by the Centers for Medicare & Medicaid Services (CMS) to participate in a new Medicare alternative payment model designed to support people living with dementia and their caregivers.
Tag: Alzheimer’s
Racial disparities in dementia determined by social factors
A study conducted in four Latin American countries by researchers at Washington University School of Medicine in St. Louis reveals that racial disparities in brain health are due to social factors, with genetic ancestry playing no role.

Expert available: FDA approval of new Alzheimer’s drug, Kisunla
Aaron Burberry, Assistant Professor, Department of Pathology, School of Medicine https://case.edu/medicine/pathology/faculty/aaron-burberry
Activating molecular target reverses multiple hallmarks of aging
Researchers at The University of Texas MD Anderson Cancer Center have demonstrated that therapeutically restoring ‘youthful’ levels of a specific subunit of the telomerase enzyme can significantly reduce the signs and symptoms of aging in preclinical models. If these findings are confirmed in clinical studies, there may be therapeutic implications for age-related diseases such as Alzheimer’s, Parkinson’s, heart disease and cancer.
Alzheimer’s Awareness Month: Virginia Tech researchers work toward better treatments
Alzheimer’s disease, a deadly brain disease than can cause loss of memory and mobility, affects millions of lives daily. June marks Alzheimer’s and Brain Awareness Month, and Virginia Tech researchers are engaged in research meant to advance treatment for Alzheimer’s disease and assist caregivers of loved ones with dementia.
Rutgers Research Bridging Gaps in Alzheimer’s Risk Among South Asian Populations
Researchers at the Krieger Klein Alzheimer’s Research Center at Rutgers Brain Health Institute are launching a pioneering study to better understand the characteristics that place South Asian populations at heightened risk for Alzheimer’s disease.
Subtle cognitive decline precedes end to driving for older adults
Even slight cognitive changes can affect an older person’s decision to stop driving, according to a new study by researchers at Washington University School of Medicine in St. Louis. The findings suggest that routine cognitive testing — in particular, the kind of screening designed to pick up the earliest, most subtle decline — could help older adults and their physicians make decisions about driving that maximizes safety while preserving independence as long as possible.
Scientists aim to stop harmful gut bacteria triggering Alzheimer’s
Australian scientists are exploring how harmful gut bacteria from a poor diet can access the brain and trigger early onset Alzheimer’s disease.
Simulation reveals new mechanism for membrane fusion
An intricate simulation performed by UT Southwestern Medical Center researchers using one of the world’s most powerful supercomputers sheds new light on how proteins called SNAREs cause biological membranes to fuse.
Human brains are getting larger. That may be good news for dementia risk
A new study published in JAMA Neurology found human brains are getting bigger. The increased size may lead to a brain reserve, potentially reducing the risk of dementia.
Nanoparticles activated by ultra-low-energy X-rays effectively halt the aggregation and toxicity of amyloid beta in preclinical models
A collaborative effort between Israeli and Italian researchers has led to the development of a new treatment strategy targeting the early-stage aggregation of A-beta before the formation of toxic oligomers.
Abdominal Fat Can Impact Brain Health and Cognition in High Alzheimer’s Risk Individuals
The impact of abdominal fat on brain health and cognition is generally more pronounced in middle-aged men at high risk of Alzheimer’s disease as opposed to women, according to researchers at Rutgers Health.
Dr. Claudia Padilla discusses Alzheimer’s and a new treatment.
Claudia Padilla, MD, at Baylor Scott & White Health, discusses Alzheimer’s and a new treatment. What You Need to Know: Alzheimer’s disease is a type of dementia. The most common sign is short-term memory loss. New medication targets the protein…
A Decade of Progress: Addressing Humanity’s Shared Challenges
Ten years after the creation of Rutgers Biomedical and Health Sciences, new university institutes and centers are bringing the world’s best medical ideas to New Jersey and beyond

Cerebral amyloid angiopathy, seizures, and epilepsy: Dr. Brin Freund
Sixty percent of patients with dementia on autopsy studies have cerebral amyloid angiopathy (CAA) pathology. This episode discusses the relationship between CAA and epilepsy through the lens of a recent publication. Dr. Alina Ivaniuk talks with Dr. Brin Freund.
Rutgers Receives $4.2 Million to Develop Center for Alzheimer’s and Dementia Research in Asian and Pacific Americans
The Resource Center for Alzheimer’s and Dementia Research in Asian and Pacific Americans will work to advance behavioral, social and economic research related to Alzheimer’s disease and other dementias especially in older Asian and Pacific Americans.
UCLA Health Tip Sheet September 2023
Below is a brief roundup of news and story ideas from the experts at UCLA Health. For more information on these stories or for help on other stories, please contact us at [email protected].
Alerta para los expertos: avances en el tratamiento para el alzhéimer mediante un enfoque integral
El lecanemab ha llamado la atención en todo el mundo por ser el medicamento aprobado recientemente para la enfermedad de Alzheimer y el primer tratamiento aprobado por la FDA para el alzhéimer en más de 20 años.
Alerta do especialista: o avanço no tratamento do Alzheimer por meio de uma abordagem abrangente
O lecanemabe recebeu atenção mundial depois de ter sido o medicamento mais recente aprovado para a doença de Alzheimer e o primeiro tratamento aprovado para Alzheimer pela Administração de Alimentos e Medicamentos (Food and Drug Administration, FDA) dos EUA em mais de 20 anos.
New Anti-amyloid Drugs are Providing Hope for People with Alzheimer’s Disease – Now What?
Newly approved anti-amyloid therapies that slow Alzheimer’s disease progression offer new hope for people with the disorder.
$50 million gift to expand health sciences research at Virginia Tech
The Richmond, Virginia-based Red Gates Foundation recently committed $50 million to the Fralin Biomedical Research Institute at VTC to accelerate health sciences research at Virginia Tech. The gift is among the largest ever made to the university.
Neuroscientists create new resource to improve Alzheimer’s disease research models
A new study by Indiana University School of Medicine researchers uses more genetically diverse mouse models to study the accumulation and spread of abnormal tau protein deposits in the brain.
Stem Cell Therapy Rescues Symptoms of Alzheimer’s Disease
Promising preclinical results from UC San Diego show hematopoietic stem cell therapy was effective in rescuing memory loss, neuroinflammation and beta amyloid build-up in a mouse model of Alzheimer’s disease.

New study reveals why defense against brain corrosion declines in people with Alzheimer’s disease
A new study by researchers at Case Western Reserve University revealed that the progression of Alzheimer’s disease (AD) can be slowed by suppressing a specific protein in the brain that causes corrosion.
Volunteering in late life may protect the brain against cognitive decline and dementia
Volunteering in late life is associated with better cognitive function — specifically, better executive function and episodic memory, according to a new UC Davis study.
Dr. Liana Apostolova is available to comment on new results of a phase III clinical trial of Donanemab, an Alzheimer’s disease medication for patients with early symptoms of the disease.
Liana Apostolova, MD is the associate dean of Alzheimer’s disease research at Indiana University School of Medicine. Dr. Apostolova and others presented results of the phase 3 clinical trial of Donanemab at the Alzheimer’s Association International Conference. The study, also published…
Lecanemab FDA Approval: U-Mich Alzheimer’s disease expert available and quote #lecanemab
On July 6, the U.S. Food and Drug Administration granted full approval to the new Alzheimer’s disease drug lecanemab (brand name Leqembi). The medication was granted accelerated approval in January. With the landmark decision, University of Michigan Health, Michigan Medicine,…
Ahead of Lecanemab FDA Decision: University of Michigan #Alzheimers expert available for interview
The U.S. Food and Drug Administration is considering full approval of the new Alzheimer’s disease drug Lecanemab (brand name Leqembi), with a decision expected by July 6. University of Michigan Health, Michigan Medicine, has an expert available to talk about…
Research Group Calls for Consensus, Collaboration to Improve Understanding of how Infections Drive Alzheimer’s
A research consortium, including a Philadelphia College of Osteopathic Medicine neuroscientist and his research coordinator, are calling for a consensus on how scientists identify and evaluate how infections contribute to or cause cognitive impairment and dementias, including Alzheimer’s disease.
The Other Dementia Breakthrough—Comprehensive Dementia Care
Most patients with Alzheimer’s disease or other types of dementia will not be eligible for the new disease modifying drugs approved by the FDA for mild cognitive impairment or mild dementia. But an op-ed co-written by UCLA’s Dr. David Reuben,…
Deep-brain stimulation during sleep strengthens memory
This study provides provides the first physiological evidence from inside the human brain supporting the dominant scientific theory on how the brain consolidates memory during sleep. Further, deep-brain stimulation during a critical time in the sleep cycle appeared to improve memory consolidation.
Alzheimer’s Drug Development Pipeline: Promising Therapies, Pharma Investment Drive Momentum in Clinical Trials
According to the newly released “Alzheimer’s Disease Drug Development Pipeline: 2023,” there are currently 187 clinical trials in the Alzheimer’s drug development pipeline – the most ever on record. This momentum is driven in part by greater investment from the pharma industry and a bump in biologic therapies – particularly monoclonal antibodies – that were central to the success of both recent FDA-approved drugs.
The annual report spots trends in clinical trial design and outcome measures, and also investigate the types of agents and biological targets that are being pursued.
Managing epilepsy in older adults
What special considerations must physicians make when managing epilepsy in older adults? Who is considered an “older adult,” anyway? Dr. Anca Arbune interviews two authors of a recent critical review by an ILAE task force.

Special Mother’s Day Cards will Fund Research To Help Find a Cure for Alzheimer’s Disease in Women
In honor of Mother’s Day, American Greetings and the Women’s Alzheimer’s Movement at Cleveland Clinic have partnered to encourage the celebration of women everywhere and raise critical research funds in the process.
High blood pressure in your 30s is associated with worse brain health in your 70s
New research from the UC Davis School of Medicine shows high blood pressure in early adulthood is associated with worse brain health in late life — especially for men. The results suggest that treating hypertension in young and middle-aged adults may help prevent dementia and Alzheimer’s disease.
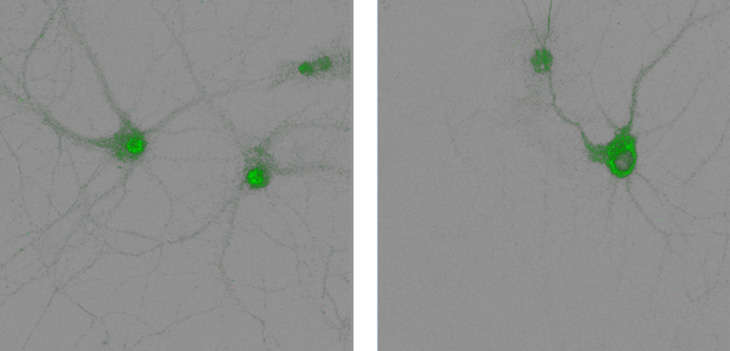
New mouse study reveals a key process in how the brain forms memories
A study from the UC Davis School of Medicine has identified a gene-enzyme interaction that appears to play a key role in how the brain forms memories. The findings provide insights into how PDE inhibitor medications may help diseases like Alzheimer’s. The research was published in Science Signaling.
UTHealth Houston expert available to discuss VA’s coverage of Alzheimer’s drug
Paul E. Schulz, MD, neurologist with UTHealth Houston and Memorial Hermann, is available over the next few days to comment on recent news that the Veterans Health Administration will provide coverage for Leqembi, which recently received accelerated approval from the…
MIND and Mediterranean Diets Associated with Fewer Alzheimer’s Plaques and Tangles
People who eat diets rich in green leafy vegetables as well as other vegetables, fruits, whole grains, olive oil, beans, nuts and fish may have fewer amyloid plaques and tau tangles in their brain—signs of Alzheimer’s disease—than people who do not consume such diets, according to a study published in the March 8, 2023, online issue of Neurology®, the medical journal of the American Academy of Neurology.
UC Davis study uncovers age-related brain differences in autistic individuals
Differences in genes involved in inflammation, immunity response and neural transmissions begin in childhood and evolve across the lifespan in brains of people with autism, a UC Davis MIND Institute has found.
Dementia: University of Michigan neurologists available to speak on frontotemporal dementia #FTD after Bruce Willis diagnosis
On Feb. 16, the family of Bruce Willis announced that the celebrated actor has been diagnosed with frontotemporal dementia, or FTD. It was announced in 2022 that Willis had aphasia, which can be an early sign of FTD. In wake…
Eartest by Eartone Application Detects Dementia Risk by Checking the Hearing of Words in Thai language
The Faculties of Medicine and Science, Chulalongkorn University, in collaboration with University College London (UCL), the United Kingdom, together with industrial partner have developed Eartest by Eartone Application that examines hearing with Thai words processing that the public can use to screen dementia by themselves before consulting physicians to help prevent and reduce future risk of dementia.
FSU psychologist receives $3.7 million grant to combat anxiety in older adults with Alzheimer’s, cognitive impairment
For the more than 6 million Americans living with Alzheimer’s disease, related dementias, or mild cognitive impairment, anxiety is often an accompanying challenge. A Florida State University psychologist has received a five-year, $3.7 million grant from the National Institute on Aging to study intervention techniques that aim to combat anxiety in these groups and improve quality of life.
U-M Health neurologists available to discuss Lecanemab, Alzheimer’s drug FDA approval #lecanemab #alzheimers
The U.S. Food and Drug Administration granted accelerated approval Friday for lecanemab, an Alzheimer’s disease drug for which studies showed the promising biological effect of removal of the brain’s amyloid buildup that occurs in the disease. University of Michigan Health,…
Study Shows African Americans and Hispanics Have Greater Vulnerability to Alzheimer’s Because of Vascular Risks, Socioeconomic Factors
African Americans and Hispanics face higher risk for Alzheimer’s disease than whites in the United States, but the reason may not be solely race or ethnicity, new research shows. Instead, those minority groups are more vulnerable because of lifelong inequities in socioeconomic factors such as income, health insurance, and access to medical care that lead to an accumulation of vascular risk factors in midlife and late life, including diabetes, hypertension, and obesity.
Study Shows African Americans and Hispanics Have Greater Vulnerability to Alzheimer’s Because of Vascular Risks, Socioeconomic Factors
James E. Galvin, M.D., M.P.H., a professor of neurology, psychology and behavioral sciences and founding director of the Comprehensive Center for Brain Health at the University of Miami Miller School of Medicine. His team recently published a study titled, “Exploring…
UCI-led study shows cognitively impaired degu is a natural animal model well suited for Alzheimer’s research
Led by researchers from the University of California at Irvine, a new study reveals that a long-lived Chilean rodent, called Octodon degus (degu), is a useful and practical model of natural sporadic Alzheimer’s Disease.
Researchers Identify the Role of an Alzheimer’s Disease Risk Gene in the Brain
Inflammatory response linked to amyloid plaque buildup
Rutgers Researchers Discover How Immune Cells Prevent Cognitive Decline
Mice altered to prevent the production of a certain type of immune cell struggled to form new memories.
Study yields clues to why Alzheimer’s disease damages certain parts of the brain
A study by researchers at Washington University School of Medicine in St. Louis yields clues to why certain parts of the brain are particularly vulnerable to Alzheimer’s damage. It comes down to the gene APOE, the greatest genetic risk factor for Alzheimer’s disease. The parts of the brain where APOE is most active are the areas that sustain the most damage, they found.
Rejuvenated immune cells can improve clearance of toxic waste from brain
Rejuvenating the immune cells that live in tissues surrounding the brain improves fluid flow and waste clearance from the brain — and may help treat or even prevent neurodegenerative diseases such as Alzheimer’s and Parkinson’s, according to a study by researchers at Washington University School of Medicine in St. Louis.