A thin film that combines an electrode grid and LEDs can both track and produce a visual representation of the brain’s activity in real-time during surgery–a huge improvement over the current state of the art.
Tag: Brain Cancer
Bypassing the blood-brain barrier to improve brain tumor diagnosis
A collaborative team of NIH-funded researchers is developing a way to obtain DNA shed from brain tumors using focused ultrasound. Their first-in-human study could be an important step towards improving the way brain tumors are diagnosed.
The Wistar Institute Announces New Caspar Wistar Fellow, Dr. Irene Bertolini
Wistar Institute is pleased to announce the recruitment of Irene Bertolini, Ph.D., to pursue research in breast and brain cancers.
Moderate to severe brain injuries significantly increase risk for brain cancer in post-9/11 veterans
Service members who have had a moderate, severe, or penetrating traumatic brain injury, or TBI, are at a greater risk for subsequently developing brain cancer, according to a collaborative study led by researchers at the Uniformed Services University (USU) published February 15, 2024, in JAMA Open Network. On the other hand, those who have suffered mild TBI, or concussion – which is much more common – may not be associated with later brain cancer diagnoses, the study finds.
NIH grant expands UIC brain bank into citywide effort to study epilepsy, brain cancer
$5 million grant expands UIC’s network of brain tissue research to 4 new Chicago sites.
Metabolite tells cells whether to repair DNA
Findings from researchers at the University of Michigan Health Rogel Cancer Center, published in Cancer Discovery, show how a specific nucleotide metabolite called GTP controls responses to radiation and chemotherapy in an unexpected way.

Study shows how brain tumors make certain immune cells turn traitor
A Ludwig Cancer Research study has for the first time exhaustively analyzed neutrophils that reside in brain tumors, detailing how the immune cells support brain cancer survival and how they’re turned by the tumor microenvironment into enablers of malignant growth.
$50 million gift to expand health sciences research at Virginia Tech
The Richmond, Virginia-based Red Gates Foundation recently committed $50 million to the Fralin Biomedical Research Institute at VTC to accelerate health sciences research at Virginia Tech. The gift is among the largest ever made to the university.
Study could help explain why certain brain tumors don’t respond well to immunotherapy
A study led by researchers at the UCLA Jonsson Comprehensive Cancer Center sheds new light on why tumors that have spread to the brain from other parts of the body respond to immunotherapy while glioblastoma, an aggressive cancer that originates in the brain, does not.
Gene therapy for brain tumor shows promising early results in humans
A new study from the University of Michigan Department of Neurosurgery and Rogel Cancer Center shows promising early results that a therapy combining cell-killing and immune-stimulating drugs are safe and effective in extending survival for patients with gliomas, a highly aggressive form of brain cancer.
Study finds improved survival for incurable brain tumor, providing ‘a crack in the armor’
For the first time, researchers have found a potential drug candidate that improved outcomes for patients with a type of childhood brain tumor for which there are no effective treatments. The compound, called ONC201, nearly doubled survival for patients with diffuse midline glioma (DMG) or diffuse intrinsic pontine glioma (DIPG), compared to previous patients.
Awake surgery for cancerous brain tumor brings referee back to the mat
After an awake surgery to remove a cancerous brain tumor, a Michigan man is living “more deliberately” than ever — officiating a high school wrestling state championship and participating in research for a potential cure.
Cancerous brain tumor cells may be at ‘critical point’ between order and disorder, study suggests
Glioblastoma cells are poised near a “critical point” of order and disorder — meaning, the cells possess some form of large-scale coordination throughout the whole tumor that allows them to respond in practical unison to attempts to kill tumor cells, such as chemotherapy or radiation, a study suggests. Researchers say disrupting the large-scale organization of brain tumors may result in more powerful ways to treat and one day eliminate brain tumors.
New drug delays progression of glioma, a deadly brain cancer
In an international study co-led by UCLA, scientists have shown that a new targeted therapy drug can extend the amount of time people with a subtype of glioma are on treatment without their cancer worsening. The finding suggests a possible new treatment option for people with the slow-growing but deadly brain tumor.
Study using novel approach for glioblastoma treatment shows promising results, extending survival
A new international study published in and presented as a late-breaking abstract at the American Association of Neurological Surgeons (AANS) annual conference, shows great promise for patients with glioblastoma. Drs. Farshad Nassiri and Gelareh Zadeh, neurosurgeons and scientists at the University Health Network (UHN) in Toronto, published the results of a Phase 1/2 clinical trial investigating the safety and effectiveness of a novel therapy which combines the injection of an oncolytic virus – a virus that targets and kills cancer cells – directly into the tumour, with intravenous immunotherapy.
New research may hold key to better treatments for aggressive brain cancer
For decades, researchers have marveled at the ability of glioblastoma, a particularly aggressive brain cancer, to turn off a patient’s cancer-fighting immune cells, thereby allowing tumors to grow freely.
March Tip Sheet From Sylvester Comprehensive Cancer Center
A new study reported in JAMA Network Open unveils disparities in Mesothelioma survival, a grant to help construction workers nail quitting smoking, a new AI algorithm that offers insights into deadly cancer, a newly launched Neuroendocrine Tumors Program, a cancer researcher chosen to co-lead Tumor Biology Program and more are in this month’s tip sheet from Sylvester Comprehensive Cancer Center.

Using neuropsychology to heal from cancer treatment
Ken Kessler had been diagnosed with glioblastoma, a rare and aggressive brain tumor. In April 2022, he had his first procedure at the University of Michigan Rogel Cancer Center to remove as much of the tumor as possible.
MD Anderson Research Highlights for February 22, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention. These advances are made possible through seamless collaboration between MD Anderson’s world-leading clinicians and scientists, bringing discoveries from the lab to the clinic and back. Recent developments include a new understanding of how HPV drives cancer development, a combination therapy to overcome treatment resistance in mantle cell lymphoma, novel insights into memory T cell formation and potential therapeutic strategies for brain cancers, improved survival outcomes for metastatic colorectal cancer, targeting myeloperoxidase to improve immunotherapy responses in melanoma, and preclinical results of a combination therapy that could effectively treat a subset of acute myeloid leukemia.
Unemployment Due to Brain, Spine Cancer Linked to More Pain, Depression
People who are unemployed due to brain or spine cancer may experience more severe symptoms of pain, discomfort, anxiety and depression than people with these cancers who are employed, according to a study published in the February 8, 2023, online issue of Neurology®, the medical journal of the American Academy of Neurology.
New drug for effective treatment of childhood brain tumor
Researchers at the University of Colorado Anschutz Medical Campus have discovered a drug combination that may offer a better prognosis for children diagnosed with MYC amplified Medulloblastoma, an often deadly form of brain cancer.
Unraveling the biology behind aggressive pediatric brain tumor reveals potential new treatment avenue
Researchers at the University of Michigan Rogel Cancer Center have identified a novel treatment approach to an aggressive type of pediatric brain cancer, using therapies already approved to treat cancer. The team developed a mouse model of pediatric glioma with a histone mutation called H3.3-G34, which allowed them to study the tumor’s biology in the presence of a functional immune system, revealing a promising outlook for long-term survival.
Researchers discover how deadly brain cancer evades treatments
The researchers found the cancer cells that survive the first round of radiotherapy or chemotherapy do so by mutating during the post-treatment minimal residual disease (MRD) or dormant state.
ASTRO issues clinical guideline on radiation therapy for IDH-mutant glioma
A new clinical guideline from the American Society for Radiation Oncology (ASTRO) provides recommendations on the use of radiation therapy to treat patients with isocitrate dehydrogenase (IDH)-mutant grade 2 and grade 3 diffuse glioma. Evidence-based recommendations outline the multidisciplinary planning and delivery techniques to manage this subset of central nervous system (CNS) tumors.
A Survivor’s Guide to Brain Cancer
Sheri Saenz is enjoying everyday pleasures as a Laguna Niguel grandmother, crafting and camping with her granddaughter and grandson and vacationing with her husband of 34 years.
Henry Ford Health + MSU Health Sciences Funds Five Cancer Research Grants to Advance Cancer Medicine, Combat Health Disparities
Henry Ford Health + Michigan State University Health Sciences today announced its funding of five cancer research grants of up to $100,000 each. These five grants follow an initial wave of funding from the partnership, in which 18 pilot grants of up to $25,000 each were funded in May 2022.
In a Race to Cure Childhood Brain Cancer, Leading Experts Unveil the Mount Sinai Children’s Brain and Spinal Tumor Center
In a race against time to cure childhood brain cancer, the leading cause of cancer deaths among children, Mount Sinai Kravis Children’s Hospital is forming the Mount Sinai Children’s Brain and Spinal Tumor Center.
Dynamic cells linked to brain tumor growth and recurrence
Tumors are made up of many types of cells, both cancerous and benign. The specific complexity of the cells inside brain tumors has been a trademark of the disease, one that makes treatment extremely difficult. While scientists have long known about the variety of cells within a brain tumor, the ways these tumors grow has relied on the understanding that the cells are static, unmoving and relatively fixed.
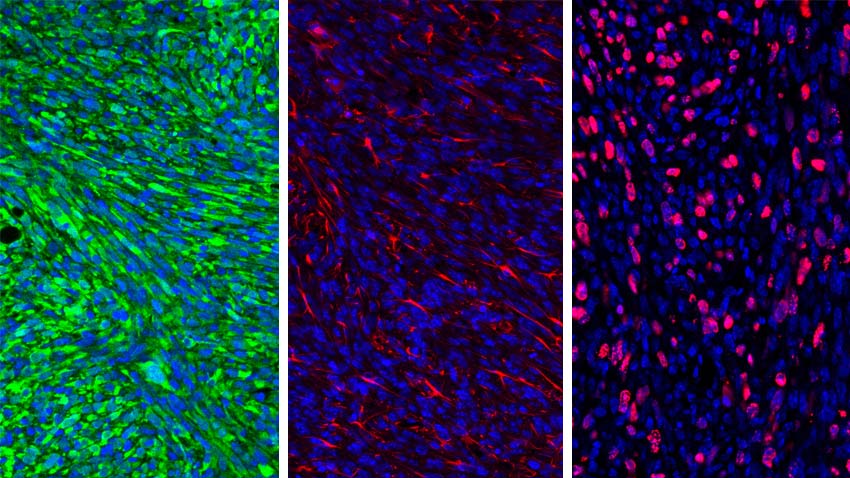
A nanoparticle and inhibitor trigger the immune system, outsmarting brain cancer
Scientists at the University of Michigan fabricated a nanoparticle to deliver an inhibitor to brain tumor in mouse models, where the drug successfully turned on the immune system to eliminate the cancer. The process also triggered immune memory so that a reintroduced tumor was eliminated—a sign that this potential new approach could not only treat brain tumors but prevent or delay recurrences.
Fast-tracked: First in-human trial for aggressive brain tumours
A novel technology designed to precisely image aggressive brain cancers and guide treatment is being developed by the University of South Australia and Australian cancer diagnostic company, Ferronova, potentially helping thousands of people who are diagnosed with the deadly condition each year.
Hopkins Med News Update
Hopkins Med News Update
NREF and AANS/CNS Tumor Section Announce StacheStrong and NREF Research Grant Recipients
The Neurosurgery Research and Education Foundation (NREF) and the American Association of Neurological Surgeons (AANS) and Congress of Neurological Surgeons (CNS) Section on Tumors are pleased to announce Jacob Young, MD, and Daniel Green Eichberg, MD, as the recipients of the StacheStrong and NREF Research Grants on behalf of the AANS/CNS Section on Tumors. These grants were funded by the NREF through a partnership with StacheStrong, a 501(c)3 not-for-profit charity focused on raising funds and awareness for brain cancer research.
Brain Cancer: Hunting What’s Left
Like a mystery detective, Sara G.M. Piccirillo, PhD, is hunting deadly bad actors by studying the crime scene and questioning bystanders one by one. But these bad actors are cells in the brain. She is using two grants to study tumor cells and cells in the surrounding area, one by one.
Could Ketogenic Diet Be Helpful with Brain Cancer?
A modified ketogenic diet may be worth exploring for people with brain tumors, according to a new study published in the July 7, 2021, online issue of Neurology®, the medical journal of the American Academy of Neurology. The diet is high in fat and low in carbohydrates.
Yale Cancer Center Study Reveals New Pathway for Brain Tumor Therapy
In a new study led by Yale Cancer Center, researchers show the nucleoside transporter ENT2 may offer an unexpected path to circumventing the blood-brain barrier (BBB) and enabling targeted treatment of brain tumors with a cell-penetrating anti-DNA autoantibody.
A Heroic Reunion
At just 8 years old, Benjamin Gordon’s life was flipped upside down when his father, Greg, was diagnosed with an aggressive type of brain cancer.

ATRT molecular groups: looking at the biology from the clinic
Scientists at St. Jude Children’s Research Hospital are learning more about what the molecular groups of a rare pediatric brain tumor mean for clinical care.

NYU Langone Brings Top Talent to Advance Cancer Care in Brooklyn
To help develop the latest treatment methods and expand cancer care service, Thomas Daniels, MD, has been appointed service chief of the Department of Radiation Oncology at Perlmutter Cancer Center–Sunset Park in Brooklyn.

Chênevert Family Brain Tumor Center Launched at Yale
Yale School of Medicine announces a gift to establish the Chênevert Family Brain Tumor Center at Yale Cancer Center. The Chênevert Family Brain Tumor Center will be a leading center in Neuro-Oncology research worldwide, bringing ground-breaking solutions and hope to patients with brain tumors.

Promising new approach to stop growth of brain cancer cells
Stand Up to Cancer Canada Dream Team is combining strengths of Princess Margaret, SickKids, University of Toronto researchers, and other unique partnerships, to accelerate new cures for hard-to-treat cancers, such as glioblastoma.

Molecular Details Reveal New Clues about Common Brain Tumor
The largest and most detailed molecular analysis yet of an aggressive brain cancer, called glioblastoma, reveals fundamental details that drive its growth. The
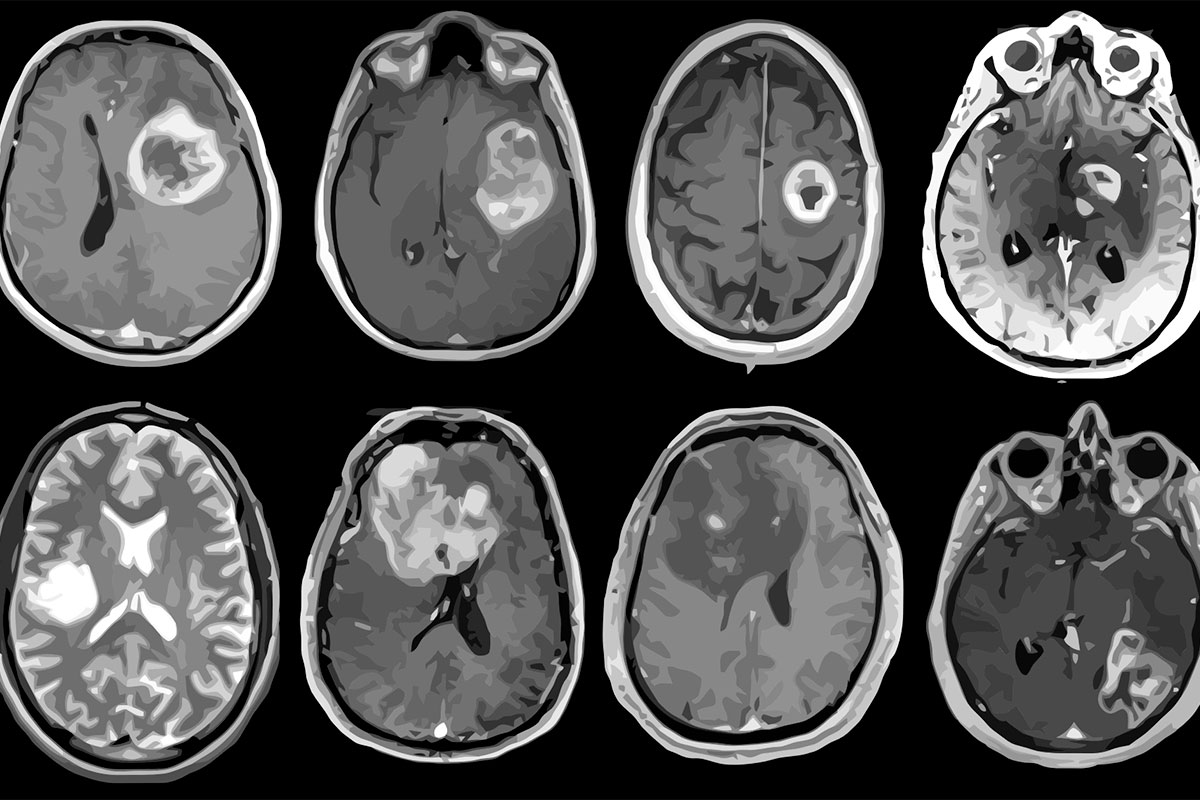
Aggressive brain tumor mapped in genetic, molecular detail
A new study led by Washington University School of Medicine in St. Louis has revealed a detailed map of the genes, proteins, infiltrating cells and signaling pathways that play key roles in driving glioblastoma. The study, of 99 tumors from patients, is the largest and most detailed schematic of this deadly brain tumor.

Henry Ford Cancer Institute is First in the World to Activate Two New Treatments in GBM AGILE Trial for Glioblastoma
Henry Ford Cancer Institute is the first site in the world to activate two new treatments for glioblastoma (GBM), the deadliest form of brain cancer, as part of a patient-centered adaptive platform trial known as GBM AGILE (Glioblastoma Adaptive Global Innovative Learning Environment).

From the clinic to the lab, understanding medulloblastoma relies on molecular profiling
A pair of research papers from St. Jude Children’s Research Hospital report on a medulloblastoma clinical trial that provides insights to guide treatment and shed light on relapsed disease.
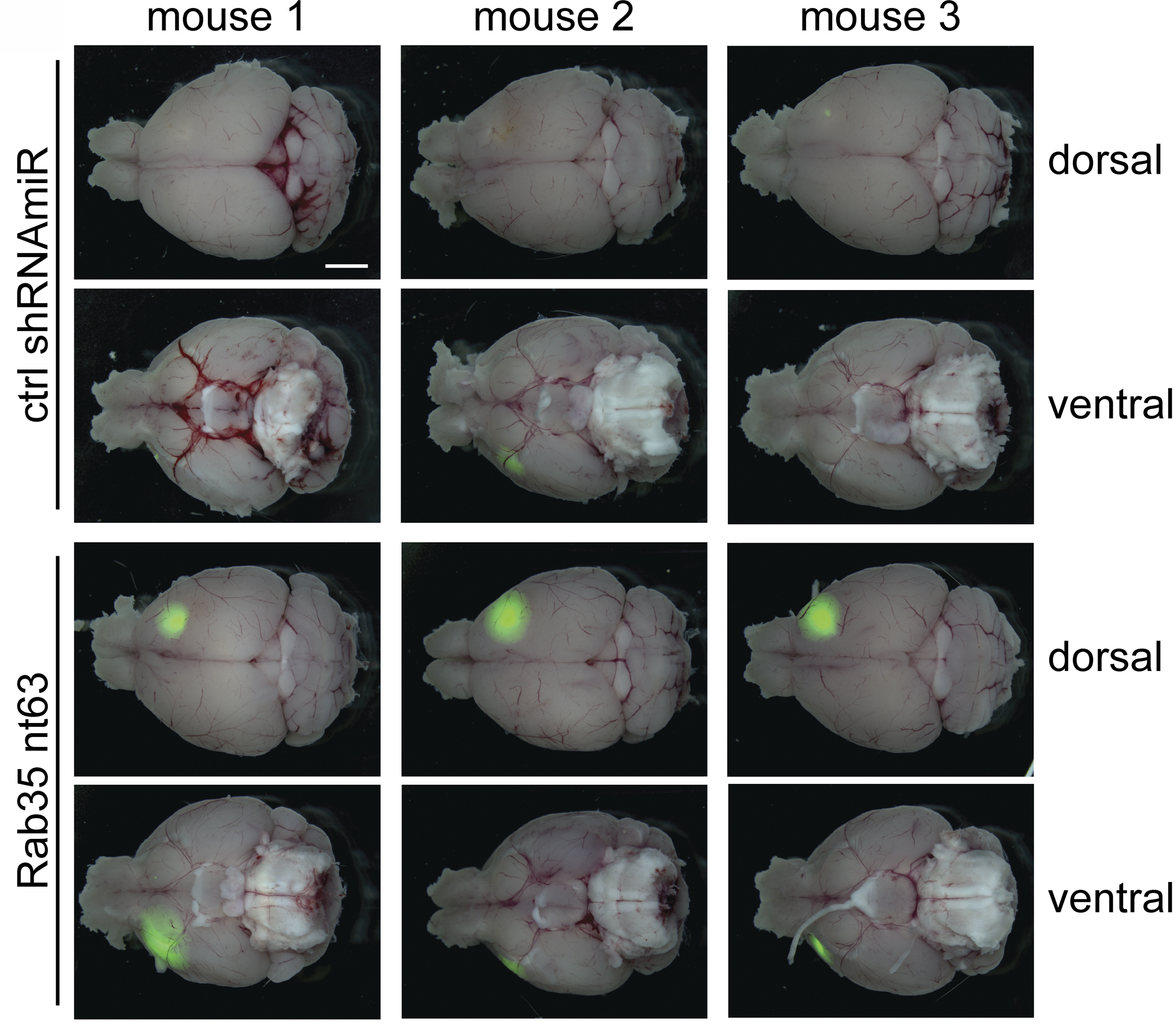
Researchers link cellular transport pathway to aggressive brain cancer
Researchers at McGill University have identified a new cellular pathway that limits the growth and spread of brain tumors by controlling the recycling of cell surface receptor proteins. The study, which will be published January 14 in the Journal of Cell Biology (JCB), suggests that the pathway, which involves a protein called Rab35, is defective in many patients with glioblastoma and that restoring Rab35’s activity could be a new therapeutic strategy for this deadly form of brain cancer.
From Glioblastoma to Endurance Races: A Story of Tenacity
Anyone who sees Colin Clark, 57, running, cycling or swimming around the Big Island of Hawaii, likely notices his athleticism and the smile permanently adorning his face.
New Treatment Approach for a Common Glioma Subtype Shows Promise in Animal Models
A combination approach to treating a common subtype of glioma — which includes metabolic reprogramming and immunotherapy — led to complete tumor regression in 60% of study mice.
Netflix to feature Mayo Clinic neurosurgeon in new documentary series
Netflix, a leading streaming entertainment service featuring TV series, documentaries and feature films across a wide variety of genres and languages, will soon begin airing a new documentary series, “The Surgeon’s Cut,” which features an episode about Alfredo Quinones-Hinojosa, M.D., a Mayo Clinic neurosurgeon.

A real life “Superman” celebrates 5 years of survival from one of the deadliest cancers
Story of a man who celebrated his five-year survival with GBM. He received 5-ALA prior to surgery, which helps the surgeon see more of the tumor for removal, and he was in a Phase 1 clinical trial.

New targeted therapy blocks metabolism in brain cancer cells with genetic vulnerability
Researchers at The University of Texas MD Anderson Cancer Center have developed a novel targeted therapy, called POMHEX, which blocks critical metabolic pathways in cancer cells with specific genetic defects. Preclinical studies found the small-molecule enolase inhibitor to be effective in killing brain cancer cells that were missing ENO1, one of two genes encoding the enolase enzyme.