A thin film that combines an electrode grid and LEDs can both track and produce a visual representation of the brain’s activity in real-time during surgery–a huge improvement over the current state of the art.
Tag: Brain Tumors
NIH grant expands UIC brain bank into citywide effort to study epilepsy, brain cancer
$5 million grant expands UIC’s network of brain tissue research to 4 new Chicago sites.
DNA organization influences the growth of deadly brain tumors in response to neuronal signals
A pioneering study at Umeå University, Sweden, has unveiled that the 3D organization of DNA can influence the progression of the aggressive brain tumour known as glioblastoma. Having identified the factors that glioblastoma uses to respond to neurons by growing and spreading, this discovery paves the way for further research into new treatments for brain tumours.
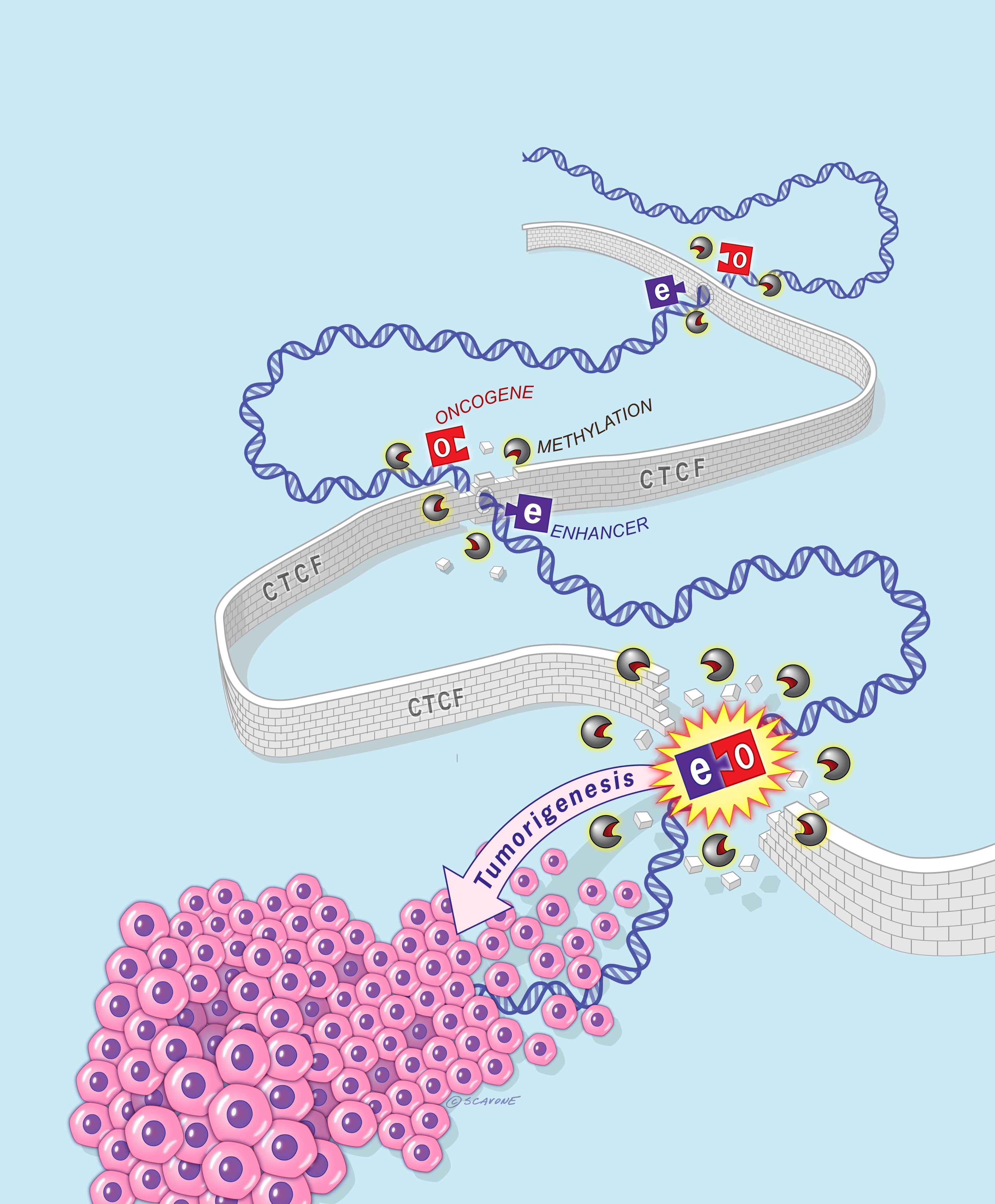
Understanding Epigenetic Changes in Glial Cells May be Key to Combatting Brain Tumors
Gliomas are incurable brain tumors. Researchers are trying to unlock the mysteries of how they originate from normal cells, which may lead to better treatments.
Hackensack Meridian Neuroscience Institute Set To Debut First-In-The-World ZAP-X Gyroscopic Radiosurgery® For The Brain Combined With Synaptive MRI To Shorten The Time From Diagnosis To Treatment
New first in the world Zap-X Gyroscopic radiosurgery equipment paired with brain only Synaptive MRI for treatment of brain tumors and other conditions
Cancerous brain tumor cells may be at ‘critical point’ between order and disorder, study suggests
Glioblastoma cells are poised near a “critical point” of order and disorder — meaning, the cells possess some form of large-scale coordination throughout the whole tumor that allows them to respond in practical unison to attempts to kill tumor cells, such as chemotherapy or radiation, a study suggests. Researchers say disrupting the large-scale organization of brain tumors may result in more powerful ways to treat and one day eliminate brain tumors.
Study using novel approach for glioblastoma treatment shows promising results, extending survival
A new international study published in and presented as a late-breaking abstract at the American Association of Neurological Surgeons (AANS) annual conference, shows great promise for patients with glioblastoma. Drs. Farshad Nassiri and Gelareh Zadeh, neurosurgeons and scientists at the University Health Network (UHN) in Toronto, published the results of a Phase 1/2 clinical trial investigating the safety and effectiveness of a novel therapy which combines the injection of an oncolytic virus – a virus that targets and kills cancer cells – directly into the tumour, with intravenous immunotherapy.
Reshaping the anti-tumor CD4 T-cell repertoire contributes to oncolytic virus therapeutic efficacy in malignant glioma
Malignant gliomas are deadly brain tumors with no cure. We engineered herpes simplex virus (HSV)-1 and developed oncolytic HSV (oHSV) to treat brain tumors, given its potential to selectively kill tumor cells while sparing normal brain cells, and to boost…
Scientists Develop Novel Approach to Enhance Drug Delivery for Brain Tumors in Children
Mount Sinai Health System and Memorial Sloan Kettering Cancer Center researchers have developed a new drug delivery approach that uses nanoparticles to enable more effective and targeted delivery of anti-cancer drugs to treat brain tumors in children.
Using machine learning to predict brain tumor progression
Researchers at the University of Waterloo have created a computational model to predict the growth of deadly brain tumours more accurately.
New method eradicates deadly brain tumors by ‘starving’ them of energy source
Dramatic results in glioblastoma research: eliminating the astrocytes (a major class of brain cells) surrounding the tumors or inhibiting their ability to supply energy to the glioblastoma cells resulted in cancer cell death, and tumor regression within several days.
National Comprehensive Cancer Network Shares New Recommendations for Treating Children with Brain Tumors
Newly-published NCCN Guidelines for Pediatric Central Nervous System Cancers synthesize latest evidence to help care teams ensure children with high-grade gliomas have best possible outcomes; available free at NCCN.org.

UT Southwestern participating in national initiative to sequence pediatric brain tumors
UT Southwestern is joining with medical centers around the nation to apply advanced sequencing to pediatric brain tumors as part of the National Cancer Institute’s new Molecular Characterization Initiative, a subset of the Cancer Moonshot Childhood Cancer Initiative.
CHOP-led Pediatric Hospital Network Receives Critical Government Support for Genetic Research of Pediatric Tumors
The Center for Data Driven Discovery at CHOP will procure molecular characterization for thousands of these brain tumor samples providing an unprecedented level of insight into devastating cancers and paving the way for future therapeutic interventions.
Hopkins Med News Update
Hopkins Med News Update
Targeting Abnormal Cell Metabolism Shows Promise for Treating Aggressive Pediatric Brain Tumors
Two experimental drug approaches that target vulnerabilities in cancer cell metabolism may extend survival and enhance the effectiveness of standard chemotherapies for a highly aggressive type of pediatric brain cancer.
Understanding Brain Tumors
To better understand brain cancer, neuro-oncologist Michael E. Salacz, MD, director of the Neuro-Oncology Program at Rutgers Cancer Institute of New Jersey and associate professor of medicine at Rutgers Robert Wood Johnson Medical School, shares some basic information on types of brain tumors, risk factors and treatment options.

Study finds high tumor mutation burden predicts immunotherapy response in some, but not all, cancers
A high rate of genetic mutations within a tumor, known as high tumor mutation burden, was only useful for predicting immunotherapy responses in a subset of cancer types, suggesting that this may not reliably be used as a universal biomarker.

Chênevert Family Brain Tumor Center Launched at Yale
Yale School of Medicine announces a gift to establish the Chênevert Family Brain Tumor Center at Yale Cancer Center. The Chênevert Family Brain Tumor Center will be a leading center in Neuro-Oncology research worldwide, bringing ground-breaking solutions and hope to patients with brain tumors.

A real life “Superman” celebrates 5 years of survival from one of the deadliest cancers
Story of a man who celebrated his five-year survival with GBM. He received 5-ALA prior to surgery, which helps the surgeon see more of the tumor for removal, and he was in a Phase 1 clinical trial.
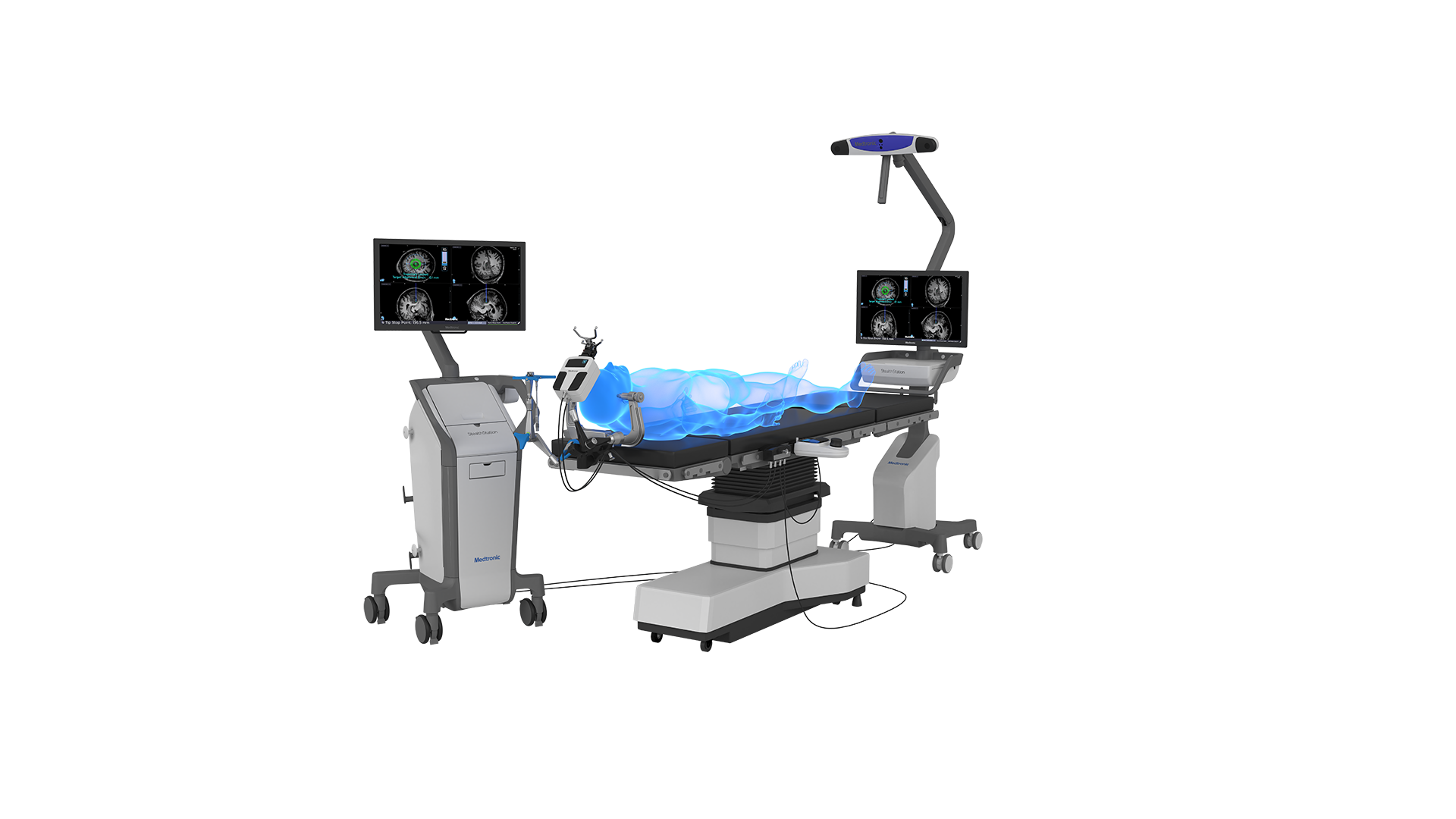
Medtronic selects UH Cleveland Medical Center for Stealth Autoguide precision robotic platform for brain surgery
Announcement of University Hospitals Cleveland Medical Center and UH Seidman Cancer Center obtaining the Medtronic Stealth Autoguide cranial robotic guidance platform for neurosurgery.

Brain Cancer: UVA IDs Gene Responsible for Deadly Glioblastoma
The discovery of the oncogene responsible for glioblastoma could be the brain tumor’s Achilles’ heel, one researcher says.

Focused ultrasound shows promise against deadliest brain tumor
An innovative use of focused ultrasound is showing promise against glioblastoma, the deadliest brain tumor, and could prove useful against other difficult-to-treat cancers.
Combination Drug Therapy For Childhood Brain Tumors Shows Promise In Laboratory Models
In experiments with human cells and mice, researchers at the Johns Hopkins Kimmel Cancer Center report evidence that combining the experimental cancer medication TAK228 (also called sapanisertib) with an existing anti-cancer drug called trametinib may be more effective than either drug alone in decreasing the growth of pediatric low-grade gliomas. These cancers are the most common childhood brain cancer, accounting for up to one-third of all cases. Low grade pediatric gliomas arise in brain cells (glia) that support and nourish neurons, and current standard chemotherapies with decades-old drugs, while generally effective in lengthening life, often carry side effects or are not tolerated. Approximately 50% of children treated with traditional therapy have their tumors regrow, underscoring the need for better, targeted treatments.