A multidisciplinary team of neurosurgeons and neuroscientists from the Icahn School of Medicine at Mount Sinai are the first in New York to study a new brain-computer interface that’s engineered to map a large area of the brain’s surface, in real time, at resolutions hundreds of times more detailed than typical arrays used in neurosurgical procedures.
Tag: Neurological Disorders
A New Study Shows How Neurochemicals Affect fMRI Readings
A landmark study, led by Yen-Yu Ian Shih, PhD, at the UNC School of Medicine, shows how neurochemicals can influence blood vessels. The new findings may alter how researchers interpret results from functional magnetic resonance imaging.
New study reveals breakthrough in understanding brain stimulation therapies
For the first time, researchers at the University of Minnesota Twin Cities showed that non-invasive brain stimulation can change a specific brain mechanism that is directly related to human behavior.
Revolutionary brain stimulation technique shows promise for treating brain disorders
The human brain’s adaptability to internal and external changes, known as neural plasticity, forms the foundation for understanding cognitive functions like memory and learning, as well as various neurological disorders.
UC Irvine-led research team creates novel rabies viral vectors for neural circuit mapping
Irvine, Calif., Feb. 14, 2024 — A research team led by the University of California, Irvine has created 20 new recombinant rabies viral vectors for neural circuit mapping that offer a range of significant advantages over existing tools, including the ability to detect microstructural changes in models of aging and Alzheimer’s disease brain neurons.
NIH grant expands UIC brain bank into citywide effort to study epilepsy, brain cancer
$5 million grant expands UIC’s network of brain tissue research to 4 new Chicago sites.
Physicists overturn common assumptions regarding brain activity
For the last 75 years a core hypothesis of neuroscience has been that the basic computational element of the brain is the neuronal soma, where the long and ramified dendritic trees are only cables that enable them to collect incoming signals from its thousands of connecting neurons.
New clues to early development of schizophrenia
Schizophrenia is a severe neuropsychiatric disease that remains poorly understood and treated. Schizophrenia onset is typically in adolescence or early adulthood, but its underlying causes are thought to involve neurodevelopmental abnormalities.
Siblings with autism share more of dad’s genome, not mom’s
Cold Spring Harbor Laboratory (CSHL) researchers have flipped the script on autism spectrum disorder (ASD) genetics.

FAU and Insightec Partner to Use Focused Ultrasound to Treat Neurological Disorders
This agreement will enable FAU and Insightec to collaborate to advance scientific knowledge about the use of focused ultrasound to treat brain diseases, including Parkinson’s disease and Alzheimer’s disease. By harnessing acoustic energy, Insightec’s innovative technology uses focused ultrasound to treat diseases in different ways.
Researchers discover how some brain cells transfer material to neurons in mice
A UC Davis study is the first to report on a material transfer mechanism from cells, known as oligodendrocytes, to neurons in the brain of a mouse model. This discovery opens new possibilities for understanding brain maturation and finding treatments for many neurological conditions.
‘Carb’ Treatment for Stroke Receives New U.S. Patent
A new twist on a drug used to treat alcohol use disorder could double up as a treatment for stroke. Called “Carb” for short, this new formulation is designed to treat ischemic stroke, protect brain tissue against injury and minimize the size of a brain infarct.
Bariatric surgery may reverse diabetes complications for people with obesity
For more than 100 million Americans who are obese, bariatric surgery may reverse complications related to diabetes, including regenerating damaged nerves, a Michigan Medicine study shows. Researchers say the findings suggest that bariatric surgery likely enables the regeneration of the peripheral nerves and, therefore, may be an effective treatment for millions of individuals with obesity who are at risk of developing diabetes and peripheral neuropathy.
Physical exercise helps to improve symptoms of Parkinson’s Disease
Physical exercise can help to improve the severity of movement-related symptoms and the quality of life in people with Parkinson’s Disease. Findings from the first Cochrane review of the available evidence found that any type of structured exercise is better than none.
UK HealthCare neurologist working to improve access to MS treatments
Together with Multiple Sclerosis (MS) experts, biostatisticians and clinicians from across the globe, a UK HealthCare neurologist has helped compile an essential list of MS medications for patients in resource-poor settings. Jagannadha “Jay” Avasarala, M.D., Ph.D., director of the Comprehensive Care Center for MS and Neuroimmunology at the Kentucky Neuroscience Institute, currently serves as a panel member of the Multiple Sclerosis International Foundation (MSIF) and previously served as chair of the American Academy of Neurology (2020-22).
Study finds how our brains turn into smarter disease fighters
Irvine, Calif., Jan. 30, 2023 — Combating Alzheimer’s and other neurodegenerative diseases by inserting healthy new immune cells into the brain has taken a leap toward reality. Neuroscientists at the University of California, Irvine and the University of Pennsylvania have found a way to safely thwart the brain’s resistance to them, vaulting a key hurdle in the quest.
Ketamine found to increase brain noise
An international team of researchers including Sofya Kulikova, Senior Research Fellow at the HSE University-Perm, found that ketamine, being an NMDA receptor inhibitor, increases the brain’s background noise, causing higher entropy of incoming sensory signals and disrupting their transmission between the thalamus and the cortex.
Research shows fatty liver disease endangers brain health
In a study examining the link between non-alcoholic fatty liver disease (NAFLD) and brain dysfunction, scientists at the Roger Williams Institute of Hepatology, affiliated to King’s College London and the University of Lausanne, found an accumulation of fat in the liver causes a decrease in oxygen to the brain and inflammation to brain tissue – both of which have been proven to lead to the onset of severe brain diseases.
Multilevel brain atlases provide tools for better diagnosis
The multilevel Julich Brain Atlas developed by researchers in the Human Brain Project, could help in studying psychiatric and aging disorders by correlating brain networks with their underlying anatomical structure.
New flexible, steerable device placed in live brains by minimally invasive robot
The early-stage research tested the delivery and safety of the new implantable catheter design in two sheep to determine its potential for use in diagnosing and treating diseases in the brain.
An Environmental Wake-Up Call for Neurology
The Presidential Symposium at the American Neurological Association’s 2022 Annual Meeting (ANA2022) in Chicago will shine a spotlight on the role of environmental exposures — air pollution, pesticides, microplastics, and more — in diseases like dementias and developmental disorders.
Study finds different comorbidities have different impacts on COVID outcomes
A new paper in Biology Methods & Protocols, published by Oxford University Press, indicates that some pre-existing conditions—including degenerative neurological diseases, dementia, and severe disabilities—matter a lot more than once thought when assessing who is at risk for death due to COVID-19.
University of Washington joins industry-academia alliance to accelerate research in neuroscience
The University of Washington has joined the Alliance for Therapies in Neuroscience (ATN), a long-term research partnership between UC San Francisco, UC Berkeley, Genentech (a member of the Roche group) and Roche Holding AG geared to transform the fight against brain diseases and disorders of the central nervous system.
Elucidating the molecular targets of “eicosapentaenoic acid”: A natural remedy for chronic pain
Eicosapentaenoic acid (EPA) is an essential nutrient belonging to the omega-3 group of polyunsaturated fatty acids (PUFAs). As the human body cannot synthesize PUFAs, dietary supplements containing EPA are required for normal physiological functions.
New research provides insight into Long COVID and ME
Researchers have uncovered how post-viral fatigue syndromes, including Long COVID, become life-changing diseases and why patients suffer frequent relapses.
Black Nursing Home Residents, Those Under Age 65 More Likely to Have Repeat Transfers to Hospital
Nursing homes transfer roughly 25% of their residents to the hospital at least once, at a cost of $14.3 billion to Medicare, according to a federal report by the Office of Inspector General.
Organoids Reveal Similarities Between Myotonic Dystrophy Type 1 & Rett Syndrome
Using brain organoids, UC San Diego researchers discover mutational commonalities between muscular dystrophy type 1 and Rett syndrome, suggesting the potential of a similar treatment for both.
Biochemists Use Enzymes to Change How Brain Cells Communicate with Each Other
As you’re reading this sentence, the cells in your brain, called neurons, are sending rapid-fire electrical signals between each other, transmitting information.
Mount Sinai Launches Neural Epigenomics Research Center
The Icahn School of Medicine at Mount Sinai has launched a new research center devoted to understanding how epigenomics influences the nervous system under both healthy and disease conditions. The Center for Neural Epigenome Engineering aims to dramatically expand Mount Sinai’s ability to conduct research in this field, facilitating new discoveries and the development of long-sought treatments for a variety of neurological and psychiatric disorders. Areas of expansion include chromatin biochemistry, chemical biology, protein engineering, and single-cell “omics.”
New study reveals the effect of extended space flight on astronauts’ brains
Long-duration space flight alters fluid-filled spaces along veins and arteries in the brain, according to new research from Oregon Health & Science University and scientists across the country.
Does autism begin in the womb?
An international research group led by Professor Toru Takumi (Senior Visiting Scientist, RIKEN Center for Biosystems Dynamics Research) and Researcher Chia-wen Lin at Kobe University Graduate School of Medicine has shown that idiopathic autism*1 is caused by epigenetic*2 abnormalities in hematopoietic cells during fetal development, which results in immune dysregulation in the brain and gut.

‘Eye-catching’ smartphone app could make it easy to screen for neurological disease at home
UC San Diego researchers developed a smartphone app that could allow people to screen for Alzheimer’s disease, ADHD and other neurological diseases and disorders—by recording closeups of their eye. The app uses a smartphone’s built-in near-infrared camera and selfie camera to track how a person’s pupil changes in size. These pupil measurements could be used to assess a person’s cognitive condition.
Differences in human, mouse brain cells have important implications for disease research
A UCLA-led study comparing brain cells known as astrocytes in humans and mice found that mouse astrocytes are more resilient to oxidative stress, a damaging imbalance that is a mechanism behind many neurological disorders.
The way mice lick could reveal origins of neurological disorders
For the first time, Cornell University researchers have developed a technique for studying the neuroscience of motor control in mice ¬– by focusing on a mouse’s tongue when it licks a water spout.
World’s first: Drug guides stem cells to desired location, improving their ability to heal
Scientists at Sanford Burnham Prebys Medical Discovery Institute have created a drug that can lure stem cells to damaged tissue and improve treatment efficacy—a scientific first and major advance for the field of regenerative medicine. The discovery, published in the Proceedings of the National Academy of Sciences (PNAS), could improve current stem cell therapies designed to treat such neurological disorders as spinal cord injury, stroke, amyotrophic lateral sclerosis (ALS) and other neurodegenerative disorders; and expand their use to new conditions, such as heart disease or arthritis.
New Grant Seeks to Fill Knowledge Gaps Regarding Spina Bifida
Researchers at UC San Diego School of Medicine and Rady Children’s Institute for Genomic Medicine have been awarded a five-year, $8.3 million grant from the National Institutes of Health to investigate the causes of spina bifida, the most common structural defect of the central nervous system.

New Study on Development of Parkinson’s Disease is ‘On the Nose’
Scientists suggest that the initial impact of environmental toxins inhaled through the nose may induce inflammation in the brain, triggering the production of Lewy bodies that can then be spread to other brain regions. However, the relationship linking olfactory dysfunction and Parkinson’s disease development remains unclear. New findings from a study add weight to this theory and identify a critical signaling molecule that may be key to the domino effect kicked off by nasal inflammation.
Study Reveals New Way to Treat Stroke Using an Already FDA-Approved Drug
Granulocyte colony-stimulating factor (GCSF) is currently used to treat neutropenia due to chemotherapy and has been successfully used for patients who require bone marrow transplants. The study is the first to report on the neuroprotective effect of GCSF in vivo and showed that it improved neurological deficits that occur in the first few days following cerebral ischemia. GCSF improved long-term behavioral outcomes while also stimulating a neural progenitor recovery response in a mouse model.
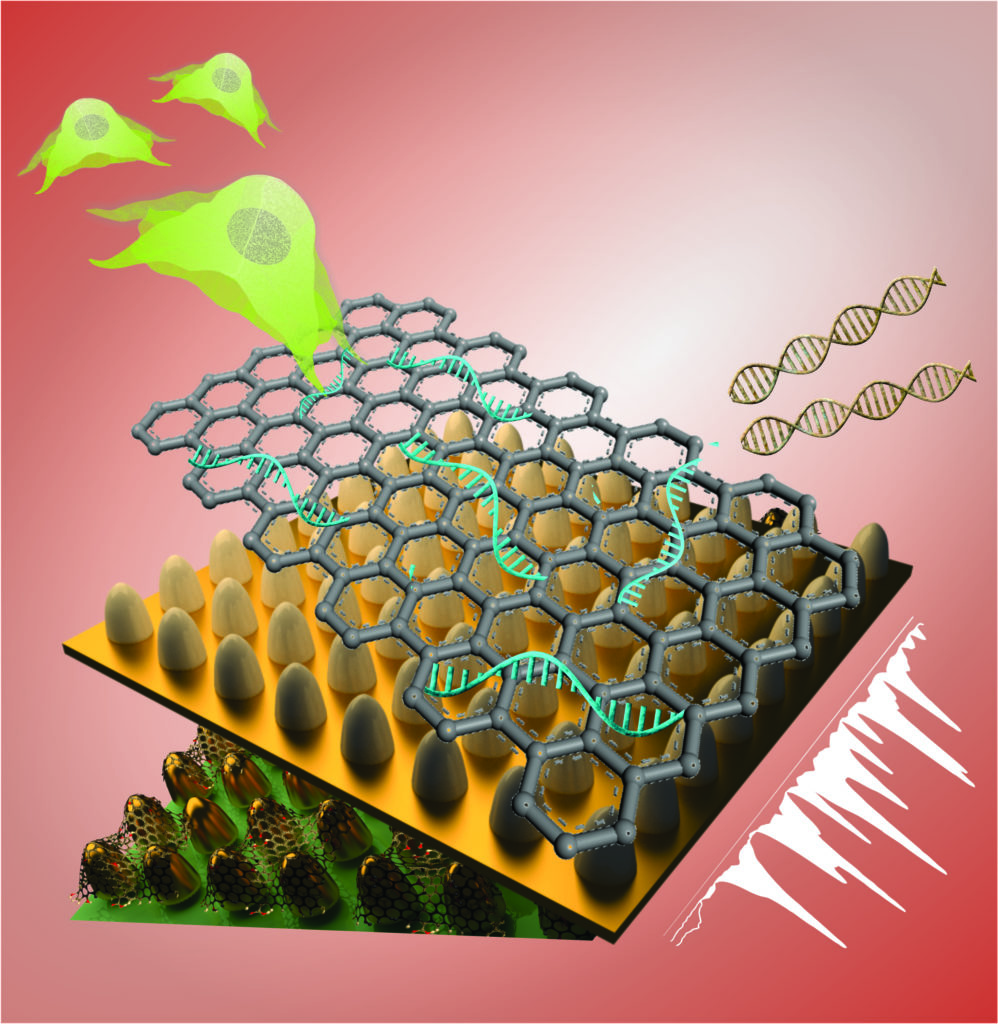
Better Biosensor Technology Created for Stem Cells
A Rutgers-led team has created better biosensor technology that may help lead to safe stem cell therapies for treating Alzheimer’s and Parkinson’s diseases and other neurological disorders. The technology, which features a unique graphene and gold-based platform and high-tech imaging, monitors the fate of stem cells by detecting genetic material (RNA) involved in turning such cells into brain cells (neurons), according to a study in the journal Nano Letters.

Machine Learning Leads to Novel Way to Track Tremor Severity in Parkinson’s Patients
Physical exams only provide a snapshot of a Parkinson’s patient’s daily tremor experience. Scientists have developed algorithms that, combined with wearable sensors, can continuously monitor patients and estimate total Parkinsonian tremor as they perform a variety of free body movements in their natural settings. This new method holds great potential for providing a full spectrum of patients’ tremors and medication response, providing clinicians with key information to effectively manage and treat their patients with this disorder.