Amanda Butler and Isabella Bugatti, both just entering their 30s, were blindsided by a diagnosis that is on the rise among women their age: breast cancer.
Tag: Radiation Therapy
Using recent diagnostic scans can substantially cut time to treatment for patients needing urgent palliation
Using previously taken diagnostic computed tomography (CT) scans in place of CT simulation scans to plan simple palliative radiation treatments can substantially reduce the time some people spend waiting for urgent treatment, improving the patient experience, a new study suggests.
Accelerated radiation treatment could reduce head and neck cancer patient burden in low- and middle-income countries
A type of head and neck cancer predominantly diagnosed in people who reside in low- and middle-income countries may be treated effectively with fewer, but higher doses of radiation, a large new international study suggests.
Precision medicine navigators increase genomic testing rates for Black patients with prostate cancer
The presence of a clinical navigator to act as a liaison between people with prostate cancer and the health care system greatly increases the likelihood that patients, especially Black patients, will receive advanced testing that can help predict the severity of their disease and guide treatment, a new study suggests.
Short-course radiation as effective as standard treatment for patients who opt for breast reconstruction after mastectomy
In a first-of-its-kind study, people with breast cancer who underwent implant-based breast reconstruction immediately following a mastectomy reported that getting fewer, higher doses of radiation was just as effective as standard radiation, did not increase side effects and saved them time and money.
High-dose radiation offers new treatment option for older patients with inoperable kidney tumors
Older adults diagnosed with kidney tumors that are not suitable for surgery may benefit from targeted, high-dose radiation, a new study from Australian and Dutch researchers suggests.
Sexual activity and vaginal dilation associated with fewer side effects after cervical cancer treatment
People who engage in sexual activity or vaginal dilation after chemoradiation treatment for cervical cancer are at lower risk for long-term side effects, according to a new study from researchers in Austria.
Liquid biopsies can rapidly detect residual disease following cervical chemoradiation, study finds
Two liquid biopsy tests that look for the presence of human papillomavirus (HPV) in the blood accurately identified patients with a high risk of cervical cancer recurrence after the completion of chemoradiation, a new study confirms.
High cure rate, low toxicity maintained with shortened radiation treatment for intermediate risk prostate cancer, study finds
People with intermediate risk, localized prostate cancer can be treated as effectively using fewer and higher doses of radiation therapy delivered over five treatment sessions as they can with lower doses delivered over several weeks, a new phase III randomized trial suggests.
Winners of the ASTRO-Sumitomo Pharma-Pfizer Alliance new combination therapy challenge announced
The American Society for Radiation Oncology (ASTRO) today announced the three winning research proposals for the 2022 ASTRO-Myovant Sciences (now known as Sumitomo Pharma)-Pfizer Alliance New Combination (Relugolix-Radiation) Therapy Challenge.
Radiation oncology research and clinical trial results to be featured at ASTRO’s Annual Meeting in San Diego
The American Society for Radiation Oncology (ASTRO) announced today the 10 studies to be highlighted in the 2023 ASTRO Annual Meeting press program. Researchers will discuss their findings in news briefings held October 2 and 3 at the San Diego Convention Center and via live webcast.
PSA levels after treatment may not be reliable predictor of survival for patients with prostate cancer
A UCLA-led study found treatments that reduce the risk of being diagnosed with a cancer recurrence based on rising prostate-specific antigen (PSA) levels after radiotherapy, commonly referred to as biochemical recurrence, do not necessarily improve a patient’s long-term overall survival.
Transforming Cancer Diagnosis and Treatment with Cerium/Lanthanum-134
Actinium-targeted alpha radiotherapy is a promising approach for treating metastatic cancers, including prostate cancer. However, therapeutic substances labeled with actinium-225 have limits on how they can be imaged, a step that allows doctors to plan treatments. This study examined the performance of cerium/lanthanum-134 as a surrogate imaging material for Ac-225.
Radiation therapy clinical trial at UCLA Health is right approach for Oakland business owner
In June 2021, Bob McCarrick and his wife Stacey headed out to Los Angeles to enroll in the MIRAGE trial and start radiation therapy.
American Society for Radiation Oncology (ASTRO) to host Annual Meeting in San Diego, October 1-4
Registration opens today for the American Society for Radiation Oncology’s (ASTRO) 65th Annual Meeting, which will be held at the San Diego Convention Center, October 1-4, 2023. Media registration is available at www.astro.org/astro2023press, and general registration is available at www.astro.org/annualmeeting.

A Simple Antibacterial Treatment Solves a Severe Skin Problem Caused by Radiation Therapy
Acute radiation dermatitis (ARD)—characterized by red, sore, itchy or peeling skin—affects up to 95% of people undergoing radiation treatment for cancer. Severe cases can cause significant swelling and painful skin ulcers that can severely impair quality of life, yet little is known about why this condition occurs and no standardized treatments for preventing severe ARD have been widely adapted.
Study finds large gap in breast cancer treatment recommendations for patients aged 70 vs 69
Age-based heuristics can lead to large differences in breast cancer treatment based on small differences in chronologic age, according to a new analysis of more than 500,000 patient records. Patients aged 70 were nearly twice as likely to be passed over for standard-of-care radiation as those aged 69. There were no similar gaps between other age pairs. The study is among the first to demonstrate an age cutoff heuristic in oncology.
ASTRO issues updated guideline on radiation therapy for endometrial cancer
A newly updated clinical guideline from the American Society for Radiation Oncology (ASTRO) provides recommendations on the use of radiation therapy and systemic therapy after surgery to treat patients with endometrial cancer. The guideline also considers the role of surgical staging and molecular profiling techniques in determining whether a patient should receive post-operative therapy. The guideline is published in the January/February 2023 issue of Practical Radiation Oncology.
Simultaneous radiation and immunotherapy are beneficial for a subset of lung cancer patients
In a recently published Nature Cancer paper, UChicago Medicine researchers have identified the first biomarker – aneuploidy – that predicts response to the radiation therapy and immune checkpoint blockade treatment combination.
Shorter course of radiation therapy yields comparable results for patients with non-metastatic soft tissue sarcoma
Patients with non-metastatic soft tissue sarcoma (STS) who need pre-operative radiation therapy can safely receive hypofractionated treatment over three weeks instead of five, with comparable tumor control and no increased risk of major complications in wound healing, according to researchers at The University of Texas MD Anderson Cancer Center.
November 2022 Issue of Neurosurgical Focus: “Evolution of Radiation Therapy Technique”
Announcement of contents of the November 2022 issue of Neurosurgical Focus
Radiation-hormone therapy combination may slow growth of oligometastatic prostate cancer
A new study offers a new option to patients with oligometastatic prostate cancer who want relief from hormone therapy without compromising the risk of their disease spreading. In the study, patients who received radiation in addition to intermittent hormone therapy lived longer without their disease progressing, and they were able to take longer breaks from the drug treatments. Results of the phase II trial (EXTEND; NCT03599765) will be presented today at the American Society for Radiation Oncology (ASTRO) Annual Meeting.
Adding radiation to systemic therapy extends overall survival for patients with advanced liver cancer
Adding radiation therapy to systemic therapy for patients with advanced liver cancer can extend overall survival and delay tumor progression without compromising patients’ quality of life, a randomized phase III clinical trial shows.
AI model using daily step counts predicts unplanned hospitalizations during cancer therapy
An artificial intelligence (AI) model developed by researchers can predict the likelihood that a patient may have an unplanned hospitalization during their radiation treatments for cancer. The machine-learning model uses daily step counts as a proxy to monitor patients’ health as they go through cancer therapy, offering clinicians a real-time method to provide personalized care. Findings will be presented today at the American Society for Radiation Oncology (ASTRO) Annual Meeting.
Radiation therapy for high-risk, asymptomatic bone metastases may prevent pain and prolong life
Treating high-risk, asymptomatic bone metastases with radiation may reduce painful complications and hospitalizations and possibly extend overall survival in people whose cancer has spread to multiple sites, a phase II clinical trial suggests. Results of the multicenter, randomized trial (NCT03523351) will be presented today at the American Society for Radiation Oncology (ASTRO) Annual Meeting.
Medical physicist consults with patients can help reduce anxiety and increase satisfaction with radiation care
Meeting with a medical physicist who can explain how radiation therapy is planned and delivered reduces patient anxiety and increases patient satisfaction throughout the treatment process, according to a new study published today in the International Journal of Radiation Oncology • Biology • Physics. Findings of the randomized, prospective phase III clinical trial also will be presented at the American Society for Radiation Oncology (ASTRO) Annual Meeting.
FLASH radiation therapy shows promise in first-in-human trial
FLASH radiation treatment – which delivers therapeutic doses of radiation in a fraction of a second – may hold promise as a potential treatment for tough-to-kill tumors, a first-in-human study in a small number of people with bone cancer suggests.
Shortened course of radiation therapy safe and effective for men with high-risk prostate cancer
A new randomized study confirms that men with high-risk prostate cancer can be treated with five versus eight weeks of radiation therapy.
Sexual side effects of cancer treatment often unaddressed with female patients
A new study finds that sexual side effects of cancer treatment are discussed far less frequently with female patients than with male patients, even when the treatment directly affects sex organs.
Radiation oncology research and clinical trial results to be featured at ASTRO’s Annual Meeting in San Antonio
The American Society for Radiation Oncology (ASTRO) announced today the 10 studies that will be highlighted in the 2022 ASTRO Annual Meeting press program. Researchers will discuss their findings in two news briefings to be held October 24 and 25 in the Henry B. Gonzalez Convention Center in San Antonio and via live webcast. Reporters can register for the meeting at astro.org/annualmeetingpress.
Cleveland Clinic Receives $7.9 Million Grant from National Institutes of Health to Form Radiation Oncology-Biology Integration Network (ROBIN)
Cleveland Clinic received a $7.9 million five-year grant from the National Cancer Institute at the National Institutes of Health to form one of three national centers as part of the newly established Radiation Oncology-Biology Integration Network (ROBIN).
ASTRO issues clinical guideline on radiation therapy for IDH-mutant glioma
A new clinical guideline from the American Society for Radiation Oncology (ASTRO) provides recommendations on the use of radiation therapy to treat patients with isocitrate dehydrogenase (IDH)-mutant grade 2 and grade 3 diffuse glioma. Evidence-based recommendations outline the multidisciplinary planning and delivery techniques to manage this subset of central nervous system (CNS) tumors.
Betamethasone could improve outcomes for prostate cancer radiation therapy
A new study published by University of Kentucky Markey Cancer Center researchers suggests that the common steroid betamethasone could be used to reduce unwanted side effects of radiation treatments for prostate cancer.
MD Anderson and Empyrean announce agreement to develop novel radiation therapy technologies
MD Anderson and Empyrean announced an exclusive license and joint development agreement to advance new technologies and products in radiation oncology.
Radiation Therapy as Effective as Surgery for Prostate Cancer
Radiation is an effective treatment for prostate cancer. Ronald D. Ennis, MD,Professor and Vice Chair of Network Integration and Quality, Department of Radiation Oncology at Rutgers Cancer Institute, along with Lara Hathout, MD, FRCPC, radiation oncologist and director of Brachytherapy at Rutgers Cancer Institute and associate Professor of radiation oncology at Rutgers Robert Wood Johnson Medical School share more
Henry Ford Health is First in the World to Offer Latest Advancement in MR-Guided Radiation Therapy
Henry Ford Health is the first in the world to complete a full course of patient treatments using the latest advancement in magnetic resonance (MR)-guided radiation therapy, which integrates real-time magnetic resonance imaging (MRI) and linear acceleration to deliver precise and accurate radiation treatment more rapidly than ever before.
New Combined Therapy Helps Extend Lives of Men With Prostate Cancer
Practice-changing research from Cedars-Sinai Cancer shows that a combination of androgen deprivation therapy—a commonly used hormone injection—plus pelvic lymph node radiation, kept nearly 90% of clinical trial patients’ prostate cancer at bay for five years. The findings were published in the peer-reviewed journal The Lancet.
MD Anderson Research Highlights: ASTRO 2021 Special Edition
This special edition features oral presentations by MD Anderson researchers at the 2021 American Society for Radiation Oncology (ASTRO) Annual Meeting (Oct. 24-27) on novel therapeutic and diagnostic approaches, including partial breast irradiation, evaluating PD-L1 levels as biomarkers to better predict response to immunotherapy, and deep learning and biomechanical models.
Intervention eliminates Black-white gaps in survival from early-stage breast and lung cancer
A new study shows that system-level changes to the way cancer care is delivered can also eliminate Black-white disparities in survival from early-stage lung and breast cancer. By identifying and addressing obstacles that kept patients from finishing radiation treatments for cancer, the intervention improved five-year survival rates for all patients and erased the survival gap between Black and white patients. Findings will be presented today at the American Society for Radiation Oncology (ASTRO) Annual Meeting.
Shortened course of radiation therapy offers similar long-term side effects following prostate removal surgery
Using fewer—but higher—doses of radiation to treat men with prostate cancer who had their prostates removed does not increase long-term side effects or lower their quality of life compared to conventional radiation treatment, a new, multi-institutional clinical trial shows.
Genetic biomarker test predicts recurrence and survival outcomes for men with high-risk prostate cancer
A new meta-analysis finds that a genetic biomarker test accurately predicts how men with high-risk prostate cancer will respond to treatment with radiation and hormone therapy. The study, which examined biopsy samples collected from three large, randomized clinical trials, indicates that physicians potentially can use genetic test scores to personalize treatment for men with the most aggressive form of prostate cancer. Findings will be presented today at the American Society for Radiation Oncology (ASTRO) Annual Meeting.
High-dose radiation thwarts tumor growth in patients with advanced lung cancer
High-dose radiation therapy can be used to lengthen progression-free survival for people with advanced lung cancer when systemic therapy has not fully halted the growth or spread of metastases, according to a new study. Findings will be presented today at the American Society for Radiation Oncology (ASTRO) Annual Meeting.
External-beam radiation therapy underused for people with liver cancer awaiting transplant
People with liver cancer awaiting transplantation could benefit from non-invasive radiation treatments but are rarely given this therapy, according to a new analysis of U.S. national data. Findings will be presented today at the American Society for Radiation Oncology (ASTRO) Annual Meeting.
Radiation therapy reprograms heart muscle cells to younger state
New research from Washington University School of Medicine in St. Louis suggests that radiation therapy can reprogram heart muscle cells to what appears to be a younger state, fixing electrical problems that cause a life-threatening arrhythmia without the need for a long-used, invasive procedure.
The Medical Minute: Real-time tumor tracking delivers high cure rates, decreased side effects for cancer patients
Think of it like radio making way for television. Image-guided radiation therapy has evolved to include the ability to track tumors in real time during treatment. It’s improving cure rates and limiting side effects for a growing number of cancer patients.
Study Confirms Effectiveness of New Personalized Approach for Radiation Therapy
Researchers from Cleveland Clinic, Case Western Reserve University School of Medicine, and Moffitt Cancer Center have found that the genomic adjusted radiation dose (GARD) may be used to personalize radiotherapy (RT) to maximize the therapeutic effect of a given physical RT dose. This research was published Aug. 4 in The Lancet Oncology journal.
ASTRO issues clinical guideline on radiation therapy for soft tissue sarcoma in adults
A new clinical guideline from the American Society for Radiation Oncology (ASTRO) provides guidance on radiation therapy for soft tissue sarcoma. Recommendations outline optimal radiation dosing, techniques and treatment planning, with a focus on preserving long-term functionality through individualized care.
ASTRO responds to troubling Medicare cuts and Radiation Oncology Model update
In response to consecutive weeks of significant proposed Medicare payment cuts to radiation oncology cancer care, Thomas J. Eichler, MD, Chair of American Society for Radiation Oncology (ASTRO), issued the following statement.
American Society for Radiation Oncology (ASTRO) to host in-person Annual Meeting in Chicago, October 24-27
Registration opens today for the American Society for Radiation Oncology’s (ASTRO) 63rd Annual Meeting, which will return to an in-person conference at McCormick Place West in Chicago, October 24-27, 2021. Media resources and registration are available at www.astro.org/astro2021press, and general registration is available at www.astro.org/annualmeeting.
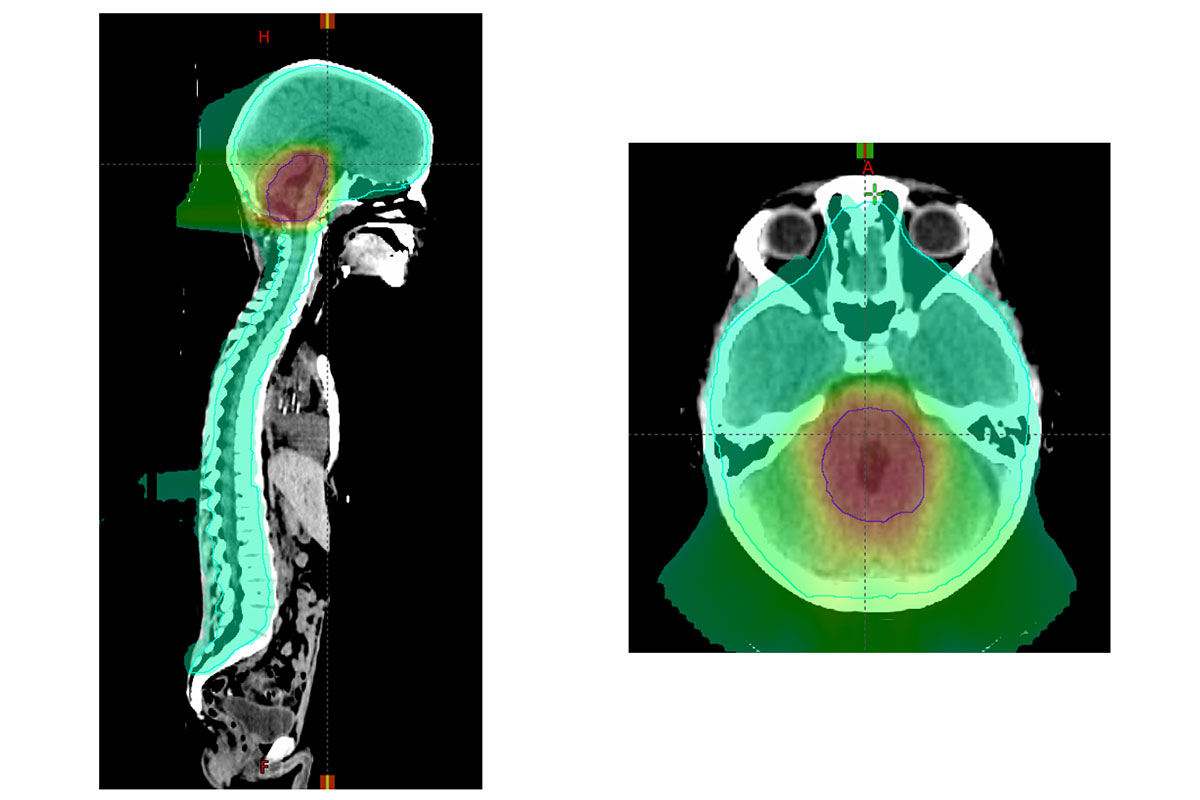
Study sheds light on treatment options for devastating childhood brain cancer
A new study led by Washington University School of Medicine in St. Louis provides new guidance on the treatment of medulloblastoma, a pediatric brain cancer. Some aspects of radiation therapy may be reduced while still providing effective treatment.