MD Anderson and Summit Therapeutics announced a strategic five-year collaboration to accelerate the development of ivonescimab, a novel PD-1/VEGF bispecific antibody.
Tag: Glioblastoma
MD Anderson Research Highlights for June 19, 2024
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention. These advances are made possible through seamless collaboration between MD Anderson’s world-leading clinicians and scientists, bringing discoveries from the lab to the clinic and back.
Sylvester Cancer Launches New Brain Tumor Institute to Personalize Brain Cancer Treatment
Sylvester Comprehensive Cancer Center today announced establishment of the Sylvester Brain Tumor Institute. It will focus on personalized medicine approaches for treating all patients with brain tumors.
MD Anderson Research Highlights for October 25, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention. These advances are made possible through seamless collaboration between MD Anderson’s world-leading clinicians and scientists, bringing discoveries from the lab to the clinic and back.
Recent developments at MD Anderson include positive results from a Phase I trial for patients with TP53-mutant acute myeloid leukemia, a novel machine learning platform to identify cancer biomarkers from liquid biopsies, a tumor-specific multi-microRNA delivery system to improve treatment outcomes in glioblastoma, a combination strategy to overcome treatment resistance in KRAS-mutated pancreatic cancer, and a new target for improving treatment response in patients with stomach cancer that has metastasized to the peritoneal cavity.
Embargoed Sylvester Comprehensive Cancer Center ASTRO 2023 Tip Sheet
Many physician-scientists and other researchers from Sylvester Comprehensive Cancer Center will make oral or poster presentations and participate in panel discussions at the American Society of Radiation Oncology (ASTRO) 2023 annual meeting in San Diego, Oct. 1-4.
True Progression or Pseudoprogression in Glioblastoma Patients?
EMBARGOED ASTRO PRESENTATION: Is it true progression or pseudoprogression in tumor growth? That’s the critical question for radiation and medical oncologists treating patients with glioblastoma. Sylvester researchers will present results from two recent studies at ASTRO 2023.
MD Anderson Research Highlights for September 21, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention. These advances are made possible through seamless collaboration between MD Anderson’s world-leading clinicians and scientists, bringing discoveries from the lab to the clinic and back.
Researchers awarded $2.5 million to develop brain cancer treatment
A multidisciplinary team of investigators from the UCLA Jonsson Comprehensive Cancer Center was awarded a $2.5 million Translational Team Science Award from the Department of Defense to develop a tailored treatment for glioblastoma, a deadly brain tumor with limited treatment options.
Study could help explain why certain brain tumors don’t respond well to immunotherapy
A study led by researchers at the UCLA Jonsson Comprehensive Cancer Center sheds new light on why tumors that have spread to the brain from other parts of the body respond to immunotherapy while glioblastoma, an aggressive cancer that originates in the brain, does not.
MD Anderson Research Highlights for August 16, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention.

Sylvester Research: Remnants of ancient retrovirus may drive aggressiveness and resilience of malignant brain cancers
A new, EMBARGOED study suggests that reactivation of an ancient retrovirus from 6 million years ago may be at least partly to blame for the aggressiveness and treatment resistance of some glioblastomas.
Awake surgery for cancerous brain tumor brings referee back to the mat
After an awake surgery to remove a cancerous brain tumor, a Michigan man is living “more deliberately” than ever — officiating a high school wrestling state championship and participating in research for a potential cure.
Cancerous brain tumor cells may be at ‘critical point’ between order and disorder, study suggests
Glioblastoma cells are poised near a “critical point” of order and disorder — meaning, the cells possess some form of large-scale coordination throughout the whole tumor that allows them to respond in practical unison to attempts to kill tumor cells, such as chemotherapy or radiation, a study suggests. Researchers say disrupting the large-scale organization of brain tumors may result in more powerful ways to treat and one day eliminate brain tumors.

Breakthrough in Glioblastoma Treatment with the Help of a Virus
Howard Colman, MD, PhD, was recently featured as an author on a publication in Nature Medicine describing the results of a recent clinical trial – a breakthrough in glioblastoma treatment with the help of a modified cold virus injected directly into the tumor. When combined with an immunotherapy drug, the authors observed a subset of patients that appeared to be living longer as a result of this therapy.
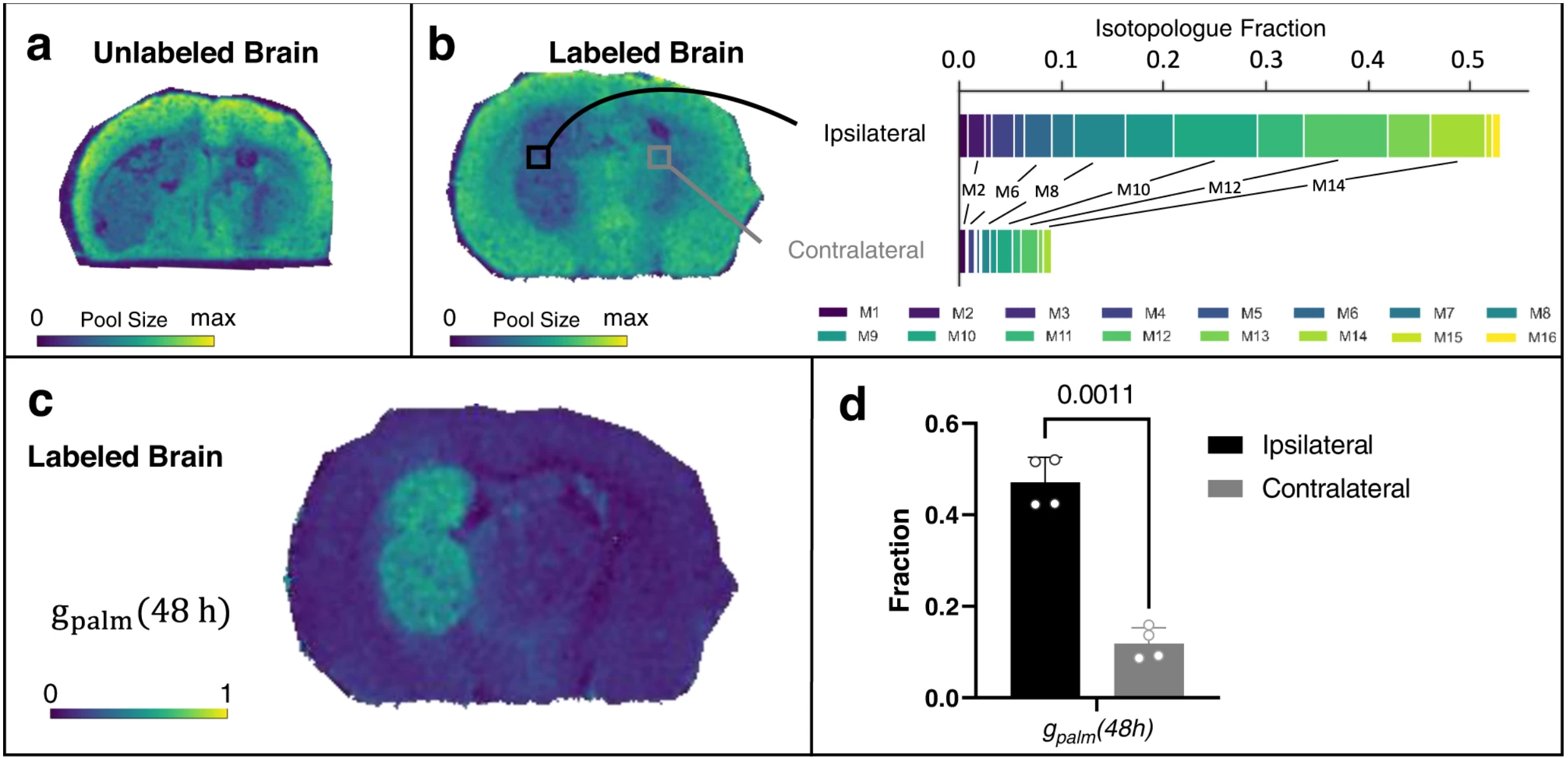
Cancer cells rev up synthesis, compared with neighbors
Tumors are composed of rapidly multiplying cancer cells. Understanding which biochemical processes fuel their relentless growth can provide hints at therapeutic targets. Researchers from Washington University in St. Louis have developed a technology to study tumor growth in another dimension — literally. The scientists established a new method to watch what nutrients are used at which rates spatially throughout a tissue.
Study using novel approach for glioblastoma treatment shows promising results, extending survival
A new international study published in and presented as a late-breaking abstract at the American Association of Neurological Surgeons (AANS) annual conference, shows great promise for patients with glioblastoma. Drs. Farshad Nassiri and Gelareh Zadeh, neurosurgeons and scientists at the University Health Network (UHN) in Toronto, published the results of a Phase 1/2 clinical trial investigating the safety and effectiveness of a novel therapy which combines the injection of an oncolytic virus – a virus that targets and kills cancer cells – directly into the tumour, with intravenous immunotherapy.
New research may hold key to better treatments for aggressive brain cancer
For decades, researchers have marveled at the ability of glioblastoma, a particularly aggressive brain cancer, to turn off a patient’s cancer-fighting immune cells, thereby allowing tumors to grow freely.

Cedars-Sinai Cancer Experts To Present Clinical Findings at AACR Conference
Cedars-Sinai Cancer oncologists and researchers are available to comment on late-breaking topics and research throughout the American Association for Cancer Research (AACR) Annual Meeting 2023, happening April 14-19 in Orlando.
Researchers Leverage Cell Self-Destruction to Treat Brain Tumors
Dominique Higgins, MD, PhD, an assistant professor in the Department of Neurosurgery, and a team of researchers at Columbia University have found that glioblastoma tumor cells are particularly sensitive to ferroptosis – a type of cell death that can be triggered by removing certain amino acids from the diet.
March Tip Sheet From Sylvester Comprehensive Cancer Center
A new study reported in JAMA Network Open unveils disparities in Mesothelioma survival, a grant to help construction workers nail quitting smoking, a new AI algorithm that offers insights into deadly cancer, a newly launched Neuroendocrine Tumors Program, a cancer researcher chosen to co-lead Tumor Biology Program and more are in this month’s tip sheet from Sylvester Comprehensive Cancer Center.
MD Anderson Research Highlights for February 22, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention. These advances are made possible through seamless collaboration between MD Anderson’s world-leading clinicians and scientists, bringing discoveries from the lab to the clinic and back. Recent developments include a new understanding of how HPV drives cancer development, a combination therapy to overcome treatment resistance in mantle cell lymphoma, novel insights into memory T cell formation and potential therapeutic strategies for brain cancers, improved survival outcomes for metastatic colorectal cancer, targeting myeloperoxidase to improve immunotherapy responses in melanoma, and preclinical results of a combination therapy that could effectively treat a subset of acute myeloid leukemia.
Sylvester Comprehensive Cancer Center Scientists, Collaborators Develop Powerful AI Algorithm to Gain New Insights into Deadly Glioblastoma
(MIAMI, FL, EMBARGOED UNTIL FEB. 2, 2023 AT 11 A.M. EST) — Scientists at Sylvester Comprehensive Cancer Center at the University of Miami Miller School of Medicine, collaborating with international researchers, have developed a sophisticated AI algorithm that performs advanced…
NIH Grant Funds Efforts to Improve Glioblastoma Detection
Collaborative project with Emory University will refine groundbreaking spectroscopic MRI technology to make it easier to use. Researchers at Sylvester Comprehensive Cancer Center at the University of Miami Miller School of Medicine will share a five-year, $3.3 million National Institutes…
Rethinking How Cancer Cells Evade Targeted Therapy
In a study publishing December 20 in Nature Cancer, UCSF researchers found that phenotype switching, as opposed to genetic evolution, may be the escape mechanism that explains the failure of precision therapies to date. They found that some cells shift to a mesenchymal, radiation-resistant phenotype (state) as a stress response following standard therapy.
Making Glioblastoma More Vulnerable to Treatment
In the tough war against glioblastoma, scientists are taking a cue from viruses on how to make the aggressive cancer more vulnerable to treatment.
UCLA researchers identify a gene as a potential target in treatment-resistant brain cancer glioblastoma multiforme
Research led by doctors and scientists at UCLA Jonsson Comprehensive Cancer Center and the UCLA Jane & Terry Semel Institute for Neuroscience & Human Behavior have identified a gene that may provide a therapeutic target for the deadly, treatment-resistant brain cancer glioblastoma multiforme (GBM).
Researchers discover how deadly brain cancer evades treatments
The researchers found the cancer cells that survive the first round of radiotherapy or chemotherapy do so by mutating during the post-treatment minimal residual disease (MRD) or dormant state.
New Radiation Therapy Delays Brain Cancer Regrowth, Protects Healthy Tissue
UC San Diego Health now offers a novel therapy option shown to extend the lifespan and improve quality of life for certain patients.
New research could lead to simple blood test for brain tumours
Bristol-led research, published in the journal The Royal Society Interface, involved the development of mathematical models to assess the current use of biomarkers in the detection of GBMs and how such biomarker-based strategies can be improved.
MD Anderson to host virtual Cancer Neuroscience Symposium
MD Anderson will host the virtual Cancer Neuroscience Symposium Sept. 22-23, 2022, in collaboration with the journal Advanced Biology. The symposium is free to attend and gathers leading experts in the field to discuss a variety of topics on the relationship between cancer biology and neuroscience. Registration includes the opportunity to participate in an abstract competition and to view sessions following the event.
Studies reveal new insights into gut microbiome impact on immunotherapy response in multiple cancers, including glioblastoma
Two studies led by The University of Texas MD Anderson Cancer Center that shed new light on the potential of the gut microbiome as a targetable biomarker to improve responses to immunotherapy were presented today at the 2022 American Society for Clinical Oncology (ASCO) Annual Meeting.
Path to Remission for a Brain Cancer That Is Usually Fatal
Recently, Michael Wulfe, who is 61 and lives in West Hollywood, was on the phone with his sister, Stephanie Wulfe, in Dallas. They talk at least once a day, but that day, something wasn’t right. “I was talking, and then I didn’t have the words,” Wulfe said. “My sister immediately said, ‘Call Cedars-Sinai!’”
Experiencia con los mentores inspira a los becarios de Mayo Clinic a ayudar a otros médicos residentes
Cuando era estudiante de medicina en México, la Dra. Paola Suarez-Meade quería una carrera que comprendiera la investigación y el trabajo clínico. Entre sus profesores, sin embargo, las trayectorias profesionales más comunes implicaban hacer una elección: tratar a los pacientes o estudiar las enfermedades.
Fast-tracked: First in-human trial for aggressive brain tumours
A novel technology designed to precisely image aggressive brain cancers and guide treatment is being developed by the University of South Australia and Australian cancer diagnostic company, Ferronova, potentially helping thousands of people who are diagnosed with the deadly condition each year.
Engineered NK cells can eliminate glioblastoma stem cells
Preclinical research finds that glioblastoma stem cells can be targeted by NK cells, but they are able to evade immune attack by releasing TFG-β. Deleting the TFG-β receptor in NK cells renders them resistant to this and restores their anti-tumor activity.
Glioblastoma study discovers protective role of metabolic enzyme, revealing a novel therapeutic target
MD Anderson researchers have discovered a new role for the metabolic enzyme, MCAD, in glioblastoma. The enzyme prevents toxic fatty acid accumulation, in addition to its normal role in energy production, and targeting MCAD led to irreversible damage and cell death specifically in cancer cells.
Ingredient in Indian Long Pepper Shows Promise Against Brain Cancer in Animal Models
Piperlongumine, a chemical compound found in the Indian Long Pepper plant, is known to kill cancerous cells in many tumor types. Now an international team including researchers from Penn has illuminated one way in which the piperlongumine works in animal models against glioblastoma.
Chemo for glioblastoma may work better in morning than evening
An aggressive type of brain cancer, glioblastoma has no cure. Patients survive an average of 15 months after diagnosis, with fewer than 10% of patients surviving longer than five years. While researchers are investigating potential new therapies via ongoing clinical trials, a new study from Washington University in St. Louis suggests that a minor adjustment to the current standard treatment — giving chemotherapy in the morning rather than the evening — could add a few months to patients’ survival.

Cancer discovery up for year’s biggest biomedical advance in a different kind of March Madness
The public can vote in STAT Madness, which is like the scientific version of the NCAA basketball tournament.

New immunotherapy target discovered for malignant brain tumors
Scientists say they have discovered a potential new target for immunotherapy of malignant brain tumors, which so far have resisted the ground-breaking cancer treatment based on harnessing the body’s immune system. The discovery, reported in the journal CELL, emerged from laboratory experiments and has no immediate implications for treating patients.

Promising new approach to stop growth of brain cancer cells
Stand Up to Cancer Canada Dream Team is combining strengths of Princess Margaret, SickKids, University of Toronto researchers, and other unique partnerships, to accelerate new cures for hard-to-treat cancers, such as glioblastoma.

Molecular Details Reveal New Clues about Common Brain Tumor
The largest and most detailed molecular analysis yet of an aggressive brain cancer, called glioblastoma, reveals fundamental details that drive its growth. The
Aggressive brain tumor mapped in genetic, molecular detail
A new study led by Washington University School of Medicine in St. Louis has revealed a detailed map of the genes, proteins, infiltrating cells and signaling pathways that play key roles in driving glioblastoma. The study, of 99 tumors from patients, is the largest and most detailed schematic of this deadly brain tumor.

Combination therapy with radiation shows promise in treating glioblastoma
In a study of mice, researchers at the UCLA Jonsson Comprehensive Cancer Center have identified a new approach that combines an anti-psychotic drug, a statin used to lower high cholesterol levels, and radiation to improve the overall survival in mice with glioblastoma.

Henry Ford Cancer Institute is First in the World to Activate Two New Treatments in GBM AGILE Trial for Glioblastoma
Henry Ford Cancer Institute is the first site in the world to activate two new treatments for glioblastoma (GBM), the deadliest form of brain cancer, as part of a patient-centered adaptive platform trial known as GBM AGILE (Glioblastoma Adaptive Global Innovative Learning Environment).
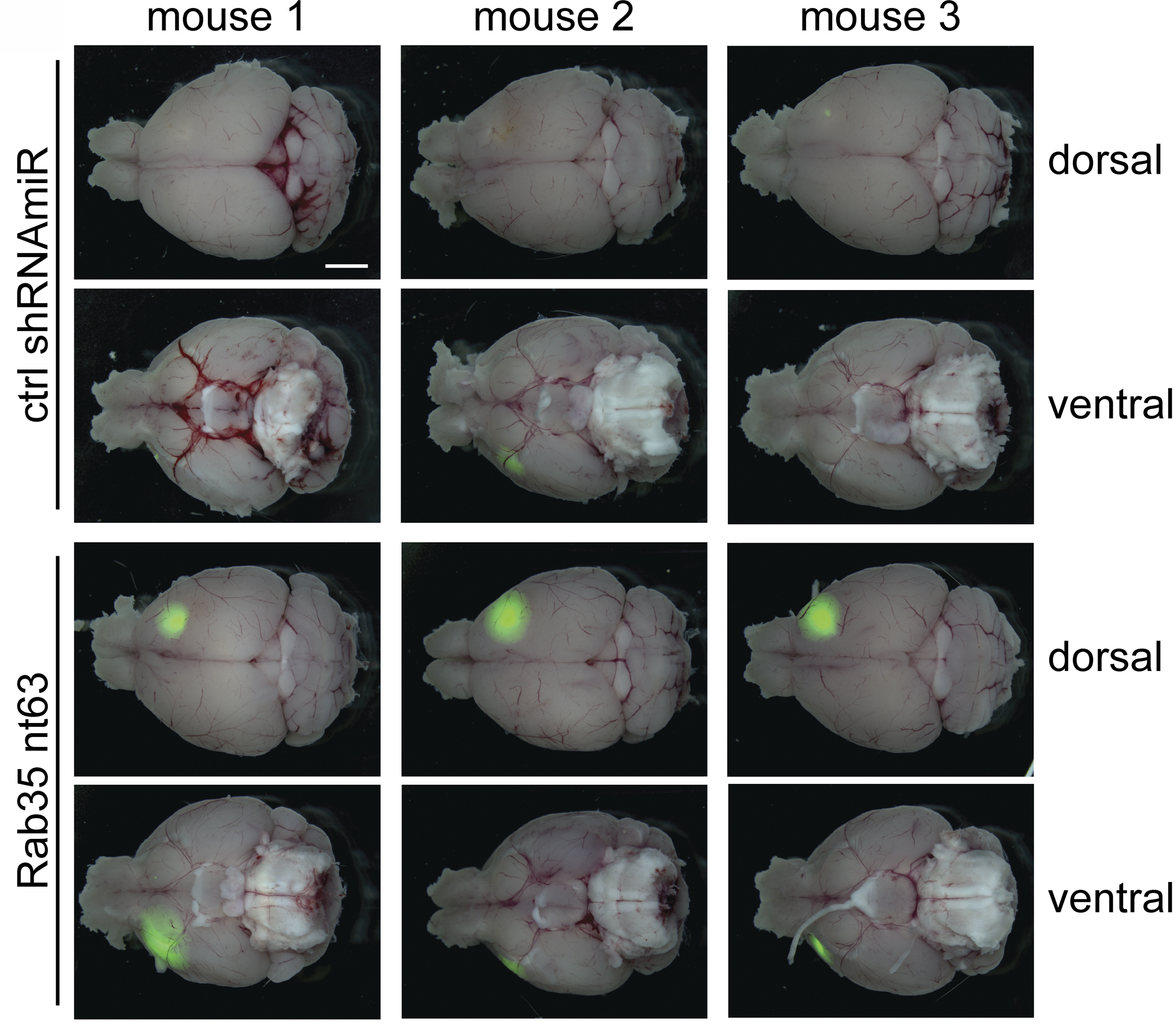
Researchers link cellular transport pathway to aggressive brain cancer
Researchers at McGill University have identified a new cellular pathway that limits the growth and spread of brain tumors by controlling the recycling of cell surface receptor proteins. The study, which will be published January 14 in the Journal of Cell Biology (JCB), suggests that the pathway, which involves a protein called Rab35, is defective in many patients with glioblastoma and that restoring Rab35’s activity could be a new therapeutic strategy for this deadly form of brain cancer.
From Glioblastoma to Endurance Races: A Story of Tenacity
Anyone who sees Colin Clark, 57, running, cycling or swimming around the Big Island of Hawaii, likely notices his athleticism and the smile permanently adorning his face.
Penn Medicine Researchers Unlock the Door to Tumor Microenvironment for CAR T Cells
Combining chimeric antigen receptor (CAR) T cell therapy with a PAK4 inhibitor allowed the engineered cells to punch their way through and attack solid tumors, leading to significantly enhanced survival in mice.
Medtronic selects UH Cleveland Medical Center for Stealth Autoguide precision robotic platform for brain surgery
Announcement of University Hospitals Cleveland Medical Center and UH Seidman Cancer Center obtaining the Medtronic Stealth Autoguide cranial robotic guidance platform for neurosurgery.
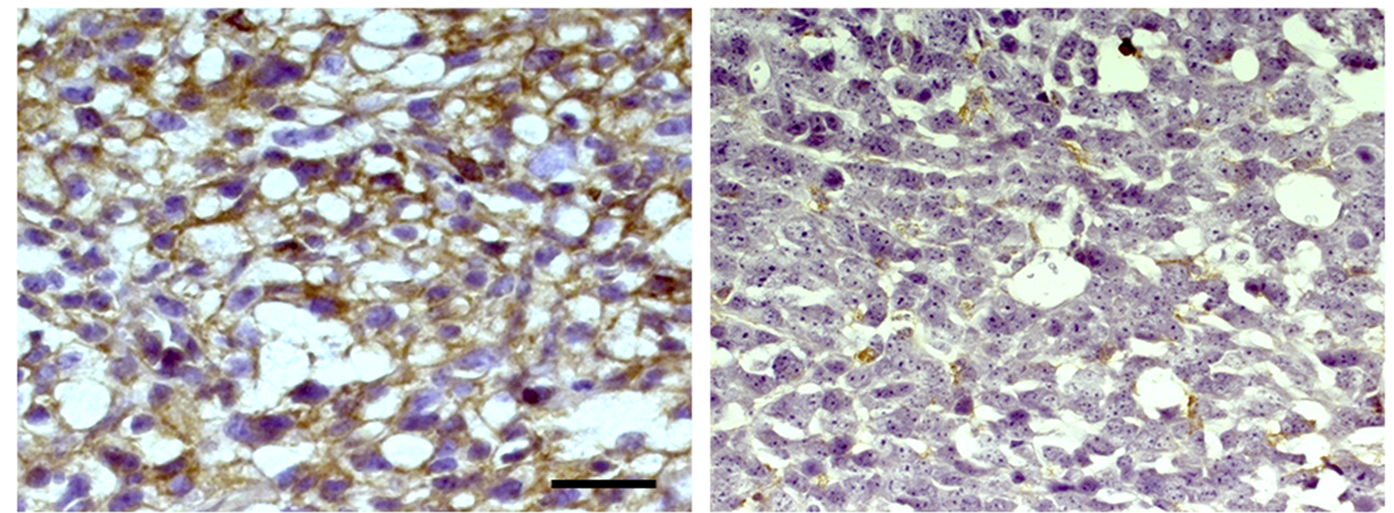
Researchers identify mechanism underlying cancer cells’ immune evasion
Researchers in China have discovered how brain cancer cells increase production of a key protein that allows them to evade the body’s immune system. The study, which will be published August 27 in the Journal of Experimental Medicine (JEM), suggests that targeting this cellular pathway could help treat the deadly brain cancer glioblastoma, as well as other cancers that are resistant to current forms of immunotherapy.