Implementing a standardized quality verification program in hospitals can significantly enhance surgical care, as demonstrated by a review study published in the Journal of the American College of Surgeons (JACS). This review provides comprehensive evidence on the positive impact of team-based and disease-based clinical programs, compliance with hospital-level regulatory metrics, and their effect on patient outcomes.
Tag: Patient Safety
MedStar Washington Hospital Center Again Named the Most Socially Responsible Hospital in the District
MedStar Washington Hospital Center is again the most socially responsible hospital in Washington, D.C. and is among the best in the nation, according to the Lown Institute, an independent think tank. It is ranked #1 in D.C., and is one of 154 hospitals to earn Honor Roll status with “A” grades in all top categories: Social Responsibility, Equity, Value, and Outcomes — key performance metrics that contribute to the overall rating.
Insurers Set to Ignore Sicker, More Complex Patients Starting July 15
The American Society of Anesthesiologists (ASA) calls on Aetna and Blue Cross Blue Shield of Illinois, Montana, New Mexico, Oklahoma and Texas to reverse their profit-driven plans to cease payments for anesthesia care provided to sicker, more complex patients based on the ASA Physical Status Classification System (ASA PS).
More hospitals than ever require staff to get flu shots
Flu vaccination mandates for hospital staff have increased in recent years, especially at hospitals serving veterans, the latest in a series of surveys shows.
Keck Hospital of USC earns an ‘A’ hospital safety grade from The Leapfrog Group
Keck Hospital of USC earned an “A” Hospital Safety Grade from The Leapfrog Group, an independent national watchdog organization.
American Association of Critical-Care Nurses Honors 18 Acute and Critical Care Nurses With Circle of Excellence Award
AACN recognizes 18 exceptional nurses — each nominated by colleagues — with the 2024 Circle of Excellence award. They will be honored during AACN’s 50th National Teaching Institute, to be held in Denver, May 20-22.
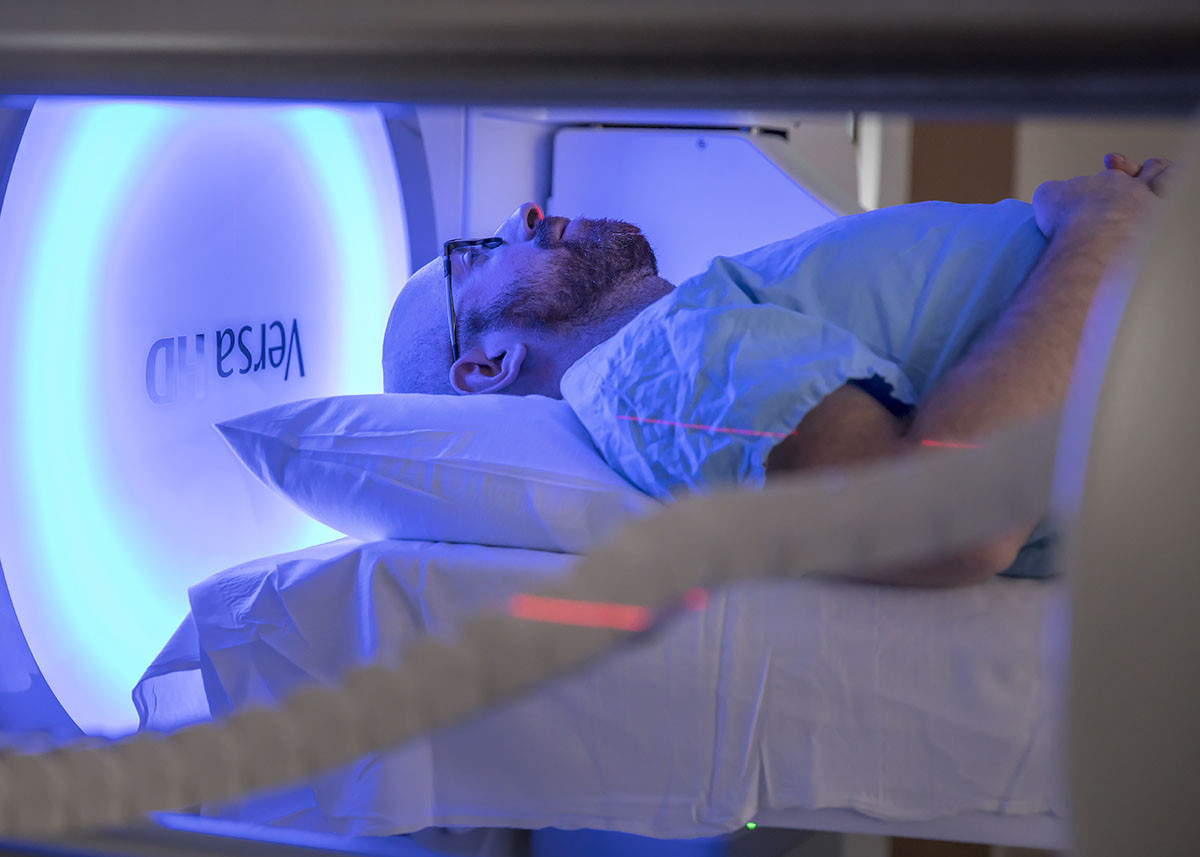
Cedars-Sinai Radiation Oncology Earns Top Accreditation
The Department of Radiation Oncology at Cedars-Sinai Cancer has earned accreditation from the American Society for Radiation Oncology (ASTRO) Accreditation Program for Excellence.
Embargoed Sylvester Comprehensive Cancer Center ASTRO 2023 Tip Sheet
Many physician-scientists and other researchers from Sylvester Comprehensive Cancer Center will make oral or poster presentations and participate in panel discussions at the American Society of Radiation Oncology (ASTRO) 2023 annual meeting in San Diego, Oct. 1-4.
UC San Diego Health Ranks No. 1 in San Diego, Makes National Honor Roll
U.S. News & World Report ranks 10 medical and surgical specialties at UC San Diego Health among the nation’s best.
Majority of Nurses Attribute Well-Being Struggles to Staffing Shortages
With projected national shortages of 63,720 registered nurses in 2030 and 141,580 licensed practical nurses in 2035, a new survey finds one-third of nurses plan to leave the profession in the next two years.
USC Verdugo Hills Hospital nationally recognized with first ‘A’ hospital safety grade
For the first time, USC Verdugo Hills Hospital (USC-VHH) earned an “A” Hospital Safety Grade from The Leapfrog Group, an independent national watchdog organization, for achieving the highest national standards in patient safety. This achievement places USC-VHH among top tier hospitals in the nation for safety and quality.
Georgia Governor Signs Law Protecting Patients from Medical Title Misappropriation
Today, Georgia Gov. Brian P. Kemp signed into law Senate Bill 197, a vital patient safety measure that prevents the use of medical and medical specialty titles, including “anesthesiologist,” by health care practitioners who are not physicians.
Center for Health Innovation Expands with $22 Million in Gifts
With a generous $22 million in gifts from Joan and Irwin Jacobs, UC San Diego Health will bring its Center for Health Innovation into full reality.
The American Thoracic Society Wants to Improve Patient Safety and Equity at the Time of ICU Discharge
The American Thoracic Society, together with six sites across the U.S., is launching the ATS ICU Pause Initiative to educate health care providers about patient safety and equity in diagnosis at the time of ICU discharge.
Identifying individuals who require higher doses of anaesthetic
Brain structures which could predict an individual’s predisposition to accidental awareness under anaesthetic have been identified for the first time by neuroscientists in Trinity College Dublin.
American Society of Anesthesiologists’ Neuromuscular Blockade Guidelines Will Improve Patient Safety and Satisfaction
The latest guidance in addressing proper monitoring and reversal of neuromuscular blockade drugs during general anesthesia – a major advance in patient safety and satisfaction – was published today in Anesthesiology, the American Society of Anesthesiologist’s (ASA) peer-reviewed medical journal.
University of Chicago Medical Center earns 22nd consecutive ‘A’ grade for patient safety, retains 10-year run in elite group
The University of Chicago Medical Center has earned its 22nd consecutive ‘A’ grade in hospital and patient safety from The Leapfrog Group, extending a 10-year run of scoring top honors from the independent watchdog organization. Of the thousands of acute-care facilities nationwide, the 811-bed University of Chicago Medical Center is one of only 22 hospitals in the country to have earned the top grade in all 22 of The Leapfrog Group’s semiannual report cards, which began in 2012.
Keck Hospital of USC nationally recognized with seventh consecutive ‘A’ hospital safety grade
For the seventh consecutive time, Keck Hospital of USC earned an “A” Hospital Safety Grade from The Leapfrog Group, an independent national watchdog organization, for achieving the highest national standards in patient safety.
UC San Diego Health Awarded Advanced Certification in Spine Surgery
UC San Diego Health has earned The Joint Commission’s Gold Seal of Approval for Advanced Certification in Spine Surgery by meeting or exceeding the highest level of national performance standards.
Ochsner Health Quality & Safety Experts Offer Playbook for Managing Widely Reported Hospital Metrics
Ochsner Health professionals team up to provide playbook for managing widely reported hospital metrics
American Society of Anesthesiologists Welcomes GE Healthcare as Industry Supporter
The American Society of Anesthesiologists (ASA) today announced GE Healthcare, a global medical technology and digital solutions company, as a new ASA Industry Supporter, bolstering the work of the Society in improving patient safety and the delivery of high-quality care before, during, and after surgery.
UC San Diego Health Recognized by Vizient as 2022 Top Performer
UC San Diego Health has been recognized as a top performer in the 2022 Bernard A. Birnbaum, MD, Quality Leadership Ranking by Vizient, Inc.
Patient Education and Feedback to Nurses Help Improve Administration Of Clot-Busting Drugs
Johns Hopkins Medicine study suggests strategies may prevent dangerous post-surgery condition
AACN Study Underscores Pandemic Damage and the Benefits of Healthy Work Environments
Results from the American Association of Critical-Care Nurses’ national survey of 9,000-plus nurses underscore the ongoing impact of the COVID-19 pandemic on nurses and the benefits of creating healthy work environments to support nurse staffing, retention and optimal patient care.
Anesthesia Patient Safety Foundation Calls on Health Care Systems to Make Systemic Changes to Stop Medical Errors: Criminalization Not the Answer
The Anesthesia Patient Safety Foundation (APSF), a related organization of the American Society of Anesthesiologists (ASA), released a statement on the criminalization of medical errors with a call to action to all health care systems and organizations to establish comprehensive mechanisms to mitigate the risk of future errors.
Keck Hospital of USC nationally recognized with sixth consecutive ‘A’ hospital safety grade
The Leapfrog Group awards Keck Hospital of USC with sixth consecutive ‘A’ hospital safety grade, illustrating the hospital’s high standards and commitment to the highest quality patient care.

AACN Rounds with Leadership – Sustaining a Culture of Safety
The joy connected with hosting an in-person AACN Deans Annual Meeting last month was tempered by the news of the criminal conviction of former nurse RaDonda Vaught for making a fatal medication error. Despite numerous system failures contributing to this tragic accident, the individual nurse was held responsible for this terrible outcome, even though she was forthcoming about the unintentional errors made.
Accreditation in healthcare quality and safety: First standards for graduate programs
Initial standards for accreditation of graduate programs in the burgeoning professional discipline of healthcare quality and safety (HQS) are presented in the November/December issue of American Journal of Medical Quality (AJMQ), official journal of the American College of Medical Quality (ACMQ). The journal is published in the Lippincott portfolio by Wolters Kluwer.
8 Mayo Clinic hospitals receive ‘A’ grade for patient safety
Eight Mayo Clinic hospitals scored high marks for safety. These hospitals earned an “A” grade for patient safety from The Leapfrog Group, a nonprofit organization run by employers and other large purchasers of health benefits.
Engagement Strategies for Safe Patient Handling in the Rehab Setting
Title: Engagement Strategies for Safe Patient Handling in the Rehab Setting Author: Elizabeth Mooney, MBA, BSN, RN, CRRN – Regional Chief Nursing Officer, Encompass Health Abstract: Safe patient mobility is crucial to maintain both patient and employee safety. As our…
American Society of Anesthesiologists Welcomes Medtronic as Industry Supporter for Seventh Year
The American Society of Anesthesiologists (ASA) today announced Medtronic plc (NYSE:MDT), a global leader in medical technology, as an ASA Industry Supporter for the seventh year, supporting the work of the Society and physician anesthesiologists to improve patient safety and brain health during and following surgical procedures.
Nurse Poll Suggests New Clinical Standards Cause Patient Harm
Drug titration is the process of adjusting the dose of a medication for maximum benefit. A pair of published surveys suggest the majority of responding nurses say mandated changes in management standards have negatively impacted their ability to do their…
American Society of Anesthesiologists and Anesthesia Patient Safety Foundation Say Preoperative Testing for COVID-19 is Essential, Regardless of Vaccination
All patients undergoing non-emergency surgeries or procedures should continue to have preoperative polymerase chain reaction (PCR) testing for SARS-CoV-2, irrespective of vaccination status, according to an updated guidance from the American Society of Anesthesiologists and Anesthesia Patient Safety Foundation.
Unit Culture, Safety Concerns Among Barriers to Patient Mobility
Research published in American Journal of Critical Care explores the barriers to out-of-bed patient mobility practices as identified by nurses in a medical ICU at Yale New Haven Hospital. In the study, all 105 patients met early mobility criteria, but none were mobilized for out-of-bed activities.
ACR Releases Position Statement on Patient Safety and Site of Service for Biologics
The American College of Rheumatology (ACR) has released an updated position statement on patient safety and site of service for biologics outlining several reasons why the ACR strongly believes infusions should be administered in a monitored health care setting with onsite supervision by a provider with appropriate training in biologic infusions.
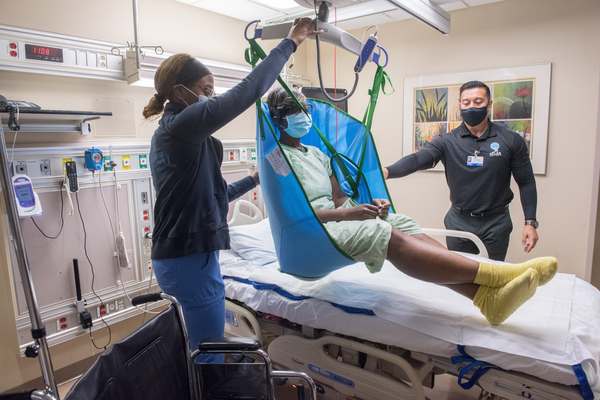
Henry Ford Hospital Launches Program to Enhance Patient Safety, Reduce Workplace Injuries
Henry Ford Hospital has partnered with Atlas Lift Tech, Inc. and Arjo Diligent Clinical Consultants to launch a program aimed at enhancing the safety of patients and team members. The program, named Project Mobility: How Motown Moves, was implemented with Henry Ford’s focus on safety, continual improvement, and innovation in mind.
AACN Critical Care Conference Brings Together Thousands of Nurses for Education, Inspiration
The American Association of Critical-Care Nurses expects 6,000+ progressive and critical care nurses to attend its virtual National Teaching Institute & Critical Care Exposition (NTI, #NTI2021) May 24-27.
Dental procedures during pandemic are no riskier than a drink of water
A new study’s findings dispel the misconception that patients and providers are at high risk of catching COVID-19 at the dentist’s office.
Morristown Medical Center Among 1st to Receive American College of Cardiology Transcatheter Valve Certification
Atlantic Health System’s Morristown Medical Center has received American College of Cardiology (ACC) Transcatheter Valve Certification, a designation of excellence that recognizes demonstrated expertise and commitment in treating patients undergoing transcatheter valve repair and replacement procedures, including transcatheter aortic valve replacement (TAVR).
Navigating the COVID-19 crisis to prevent pressure injuries: Learning health system helped one hospital adapt and update care in real time
Early in the COVID-19 pandemic, healthcare systems scrambled to modify patient care processes – particularly when it came to strategies aimed at reducing the risk of hospital-related complications. A look at how one hospital applied its learning health system (LHS) framework to respond to a COVID-19-related increase in hospital-acquired pressure injuries (HAPIs) is presented in the May/June Journal for Healthcare Quality (JHQ), the peer-reviewed journal of the National Association for Healthcare Quality (NAHQ). The journal is published in the Lippincott portfolio by Wolters Kluwer.

Nurse-Driven Initiative Cuts CAUTI Rates in the ICU
An initiative at UPMC Williamsport used education and practice-related interventions to quickly reduce CAUTI rates and lay the groundwork for hospital-wide implementation with long-term impact. The bundle included a daily checklist and nurse-driven removal protocol for discontinuing indwelling catheter use.

The Medical Minute: You + your doctor = patient safety
National Patient Safety Awareness Week is March 14-20, but in reality, it’s a year-round focus for hospital staff – and one that started long before COVID-19 made you think twice about it.

Hackensack Meridian Mountainside Medical Center Offers Tips to Help Patients Stay Safe: Patient Safety Awareness Week is March 14-20, 2021
In recognition of Patient Safety Awareness Week, Hackensack Meridian Mountainside Medical Center offers tips to help patients stay safe and take an active role in their care. Patient Safety Awareness Week, March 14 – 20, 2021, is observed annually to…

Patient Safety Week: Sleep Experts Available for Interviews to Discuss Sleep Center Safety, and Why Sleep is Essential to Health
Due to the COVID-19 pandemic, many patients are delaying or avoiding care for common, treatable sleep disorders, such as obstructive sleep apnea and insomnia. Putting off needed care for sleep disorders can have negative long-term consequences for overall health and…

In-Person Reviews of ICU Patient Deaths Led to Care Improvements
Data from five years of in-person rapid mortality reviews of 500+ ICU patient deaths at a Los Angeles hospital not only identified immediate concerns related to patient care but also yielded valuable insights on potentially preventable patient deaths and areas for hospital improvement initiatives.
American College of Surgeons verifies first hospital that meets its standardized quality criteria for geriatric surgery
The American College of Surgeons Geriatric Surgery Verification Program (ACS GSV) has announced that Unity Hospital, Rochester, N.Y., has achieved Level 1—Comprehensive Excellence verification status, which recognizes its commitment to providing optimal care for its older adult surgical patients by meeting the GSV’s program standards.

Johns Hopkins Medicine Hosts Briefing on COVID-19: One Year Later
A Woman’s Journey will host a 90-minute virtual event, “COVID-19: One Year Later,” during which Johns Hopkins Medicine experts will address important issues related to COVID-19 such as new and available treatments and vaccine safety and efficacy. Registrants will learn about the continued urgency of public health measures to mitigate the pandemic despite the introduction of vaccines, what distinguishes the leading vaccine contenders in their methodology, safety and effectiveness, and symptoms and insights surrounding lingering deficits in physical function, mental health and cognition among COVID-19 survivors.
AAPM Advances Best Practices for Patient Safety in X-Ray Imaging
Since April 2019, the American Association of Physicists in Medicine has championed a critical way to make X-ray imaging safer and more effective by discontinuing the long-standing practice of placing leaded shields over patient gonads. Today, the National Council on Radiation Protection and Measurements released a statement recommending the discontinuation of routine shielding of patient gonads during X-ray imaging exams and AAPM stands ready to help imaging providers, patients and caregivers to understand and adopt these new best practices – practices that will ensure safer and higher-quality X-ray exams.
Glaucoma Research Foundation Releases Video Encouraging Patients to Visit Their Eye Doctor for the Care They Need During COVID-19 Pandemic
The COVID-19 pandemic has presented many challenges including delayed eye doctor appointments. This video will discuss changes eye doctors have made to improve safety during every step of the office visit.
Gov. Ducey Ignores Nearly Two Thousand Letters from Physicians and the Public Demanding He Protect Patient Safety
Gov. Doug Ducey has ignored more than 1700 letters from the medical community and the public strongly urging he protect Arizona patients by making his decision to “opt-out” of the Centers for Medicare & Medicaid Services’ physician supervision requirement temporary.