MedStar Washington Hospital Center is tied for the #1 hospital in the Washington metro region in the 2024-2025 edition of U.S. News & World Report’s Best Hospitals. Additionally, two of MedStar Washington’s clinical programs are nationally ranked. Cardiology, Heart & Vascular Surgery again ranked at #38 in the country.
Tag: Geriatrics
UC San Diego Receives $5M to Support Geriatrics Workforce Enhancement Program
The San Diego Imperial Geriatric Education Center has received renewed funding from the Health Resources and Services Administration, allowing the center to relocate to UC San Diego.
In the Resuscitation Discussion, Do Words Matter Between Doctors and Patients?
Adults 65 and older, who were hospitalized for a variety of medical conditions, had highly satisfying conversations about whether they wanted CPR, regardless of whether doctors used the terms “allow a natural death” or “do not resuscitate” for indicating no CPR, according to a pilot study by Rutgers Health researchers.
The study, which found 83 percent wished to be resuscitated, is the first to report on the resuscitation preferences for general inpatients older than age 65.
Measuring communication experiences of families of inpatients unable to make decisions for themselves
Researcher-clinicians to measure the experience of communication with hospital staff from the perspective of family members of seriously ill patients unable to make decisions for themselves.
Baylor Scott & White Health Again the Most-Awarded Health System in Texas for Clinical Care and Patient Experience
Baylor Scott & White Health once again leads the state of Texas in the number of accolades earned in U.S. News & World Report’s 2023-24 Best Hospitals, released today. A total of 26 Baylor Scott & White hospitals were recognized, including four facilities with a nationally ranked specialty – more than any other health system in Texas.
Baylor Scott & White Health Again the Most-Awarded Not-for-Profit Health System in Texas for Clinical Care and Patient Experience
Baylor Scott & White Health once again leads the state of Texas in the number of accolades earned in U.S. News & World Report’s 2023-24 Best Hospitals, released today. A total of 26 Baylor Scott & White hospitals were recognized, including four facilities with a nationally ranked specialty – more than any other health system in Texas.
UC San Diego Health Ranks No. 1 in San Diego, Makes National Honor Roll
U.S. News & World Report ranks 10 medical and surgical specialties at UC San Diego Health among the nation’s best.
A Generous Gift for the Future of Aging: Parker Health Group Gives $18.8 Million to Rutgers University’s Robert Wood Johnson Medical School
A gift of $18.8 million was announced today from Parker Health Group—a Piscataway, New Jersey-based leader in aging services—to the Rutgers Robert Wood Johnson Medical School. This gift will create the Parker Health Group Division of Geriatrics in the medical school’s Department of Family Medicine and Community Health, which will focus on improving care for seniors through applied research, education, and interdisciplinary collaboration.
Renowned Expert on Aging and Brain Health Available to Comment on Study Finding Regular Internet Usage Associated with Decreased Risk of Dementia
A new study by NYU School of Global Health published in the Journal of the American Geriatrics Society reports that regular Internet usage was associated with approximately half the risk of dementia compared to non-regular usage.
AI can spot early signs of Alzheimer’s in speech patterns, study shows
New technologies that can capture subtle changes in a patient’s voice may help physicians diagnose cognitive impairment and Alzheimer’s disease before symptoms begin to show, according to a UT Southwestern Medical Center researcher who led a study published in the Alzheimer’s Association publication Diagnosis, Assessment & Disease Monitoring.
On pandemic’s third anniversary, loneliness and isolation are down, but still high, among older adults
After three years of pandemic living, loneliness, isolation and lack of social contact have finally started to decline among older adults, a new poll shows.
UT Southwestern’s nationally ranked geriatric care receives international exemplar status
UT Southwestern Medical Center has received exemplar status by the Nurses Improving Care for Healthsystem Elders (NICHE) – an international designation that indicates a hospital’s commitment to achieving the highest level of geriatric care excellence.
Cedars-Sinai Ranked #2 Hospital in Nation by U.S. News & World Report
Cedars-Sinai has been named the #2 hospital in the nation and #1 in California in U.S. News & World Report’s “Best Hospitals 2022-23” rankings.
U.S. News & World Report Again Names University Hospitals Cleveland Medical Center Among Nation’s Best Hospitals for 2022-2023
Announcement of annual hospital ranking from US News & World Report, which recognized University Hospitals Cleveland Medical Center as a Best Hospital for 2022-2023. UH Cleveland Medical Center ranked in four of 15 adult specialties, and is ranked third among all hospitals in Ohio.
UC San Diego Health Ranks #1 Regionally by U.S. News & World Report
UC San Diego Health top ranked in 10 medical and surgical specialties, among the nation’s best.
Palo Alto University Addresses Mental Health Needs of Senior Living Communities While Providing Training Opportunities for Beginning Clinicians
Palo Alto, CA – In response to the impact COVID-19 is having on the mental health of individuals in aging communities, a team of psychologists and counselors at Palo Alto University (PAU) developed a tele-mental health outreach program that partners…
Gold Ribbon Not Necessary—Healthy Brain and Body Function Are the Rewards in This Game
As human lifespans increase, new societal challenges arise. In a “superaging society,” in which young people are few and older people are many, caring for the older adult population adequately with limited resources is a difficult balancing act to perform.

FAU Awarded $1 Million to Help Prevent Injury, Death from Falls in Older Adults
Every second, an older person in the U.S. falls and injures themselves, and every 20 minutes one of them dies from the fall. The Geriatric Emergency Department Fall Injury Prevention Project will investigate several emergency department-based prevention strategies in older patients at high risk for recurrent falls and injury. The tailored multicomponent intervention will identify effective fall prevention strategies that target limited resources to high-risk individuals who come to the emergency department to improve patient outcomes, improve safety, and reduce overall costs of health care.
Music to Our Patients’ Ears
When Noel Thompson was sent to the Emergency Trauma Department at Hackensack University Medical Center by his podiatrist on April 4, with a possible infection in his right foot, the 96 year old was nervous. It was a violinist who…
Hero’s Encounter: Leading Geriatrician and World War II Veteran Share Bond
An internationally renowned geriatrician and advocate for seniors and a 98-year-old World War II veteran hero are a dynamic duo whose paths recently crossed. They have a common bond: to improve care and quality of life for Americans and people throughout the world.
Older Adults Need More Than Clichés Like ‘Exercise is Good for You’ to Stay Active
More than 80 percent of adults get the recommended 150 minutes of moderate intensity or 75 minutes of vigorous-intensity physical activity per week. Moreover, 40 percent of Americans 75 and older are entirely inactive. Little is known about factors associated with increasing, sustaining, or declining physical activity levels over time. A study explored what drives older adults from diverse backgrounds to start or sustain physical activity and what stops them. The bottom line: knowledge and old clichés alone aren’t enough to keep them moving.
UC San Diego Health Ranked #1 by U.S. News & World Report
UC San Diego Health, the region’s only academic health system, is ranked #1 in San Diego and #5 in California, placing it among the nation’s best hospitals, according to the 2021-2022 U.S. News & World Report survey. UC San Diego Health was ranked in the top 50 in 10 specialties.
Older Adults with Functional Impairments Linked to Prescription Drug Use/Misuse
Researchers at University of California San Diego School of Medicine found that functional impairments among adults aged 50 and older are associated with a higher risk of medical cannabis use; and prescription opioid and tranquilizer/sedative use and misuse.

How Does Your Brain Process Emotions? Answer Could Help Address Loneliness Epidemic
In a study published in the March 5, 2021 online edition of Cerebral Cortex, researchers at University of California San Diego School of Medicine found that specific regions of the brain respond to emotional stimuli related to loneliness and wisdom in opposing ways.
Geriatric Emergency Departments Associated with Lower Medicare Expenditures
As the U.S. population ages, more hospitals are implementing geriatric emergency department (GED) programs with specialized staff focused on transitional care for older adults. A new study finds that providing specialized geriatric emergency care results in lower Medicare expenditures up to $3,200 per beneficiary.
American College of Surgeons verifies first hospital that meets its standardized quality criteria for geriatric surgery
The American College of Surgeons Geriatric Surgery Verification Program (ACS GSV) has announced that Unity Hospital, Rochester, N.Y., has achieved Level 1—Comprehensive Excellence verification status, which recognizes its commitment to providing optimal care for its older adult surgical patients by meeting the GSV’s program standards.

Study: Loneliness Highest in the 20s and Lowest in the 60s
Seeking to develop effective interventions, researchers at University of California San Diego School of Medicine examined the psychological and environmental factors that lead to patterns of loneliness in different age groups.

Is Spirituality a Component of Wisdom?
In a recent study, researchers at University of California San Diego School of Medicine found a seventh component of wisdom: spirituality.

Studies Find Even Minimal Physical Activity Measurably Boosts Health
Two research teams at UC San Diego School of Medicine sought to understand sedentary lifestyles, with one study finding that even light physical activity, including just standing, can benefit health, and the other that Americans are sitting too much.

From San Diego to Italy, Study Suggests Wisdom can Protect Against Loneliness
Researchers at UC San Diego School of Medicine and University of Rome La Sapienza examined middle-aged and older adults in San Diego and Cilento, Italy and found loneliness and wisdom had a strong negative correlation. The wiser the person, the less lonely they were.

Research News Tip Sheet: Story Ideas From Johns Hopkins Medicine
During the COVID-19 pandemic, Johns Hopkins Medicine Media Relations is focused on disseminating current, accurate and useful information to the public via the media. As part of that effort, we are distributing our “COVID-19 Tip Sheet: Story Ideas from Johns Hopkins” every other Tuesday.

Talking Alone: Researchers Use Artificial Intelligence Tools to Predict Loneliness
A team led by researchers at University of California San Diego School of Medicine has used artificial intelligence technologies to analyze natural language patterns to discern degrees of loneliness in older adults.
The Mount Sinai Hospital Ranked Among Top in the Nation by U.S. News & World Report; Brookdale Department of Geriatrics and Palliative Medicine Claims No. 1 Spot in Specialty Rankings
The Mount Sinai Hospital, the flagship hospital of Mount Sinai Health System, was listed among the nation’s top hospitals for care excellence in U.S. News and World Report, marking the fifth straight year the hospital has been listed among the top 20 in the country while landing on the distinctive “Honor Roll” list.
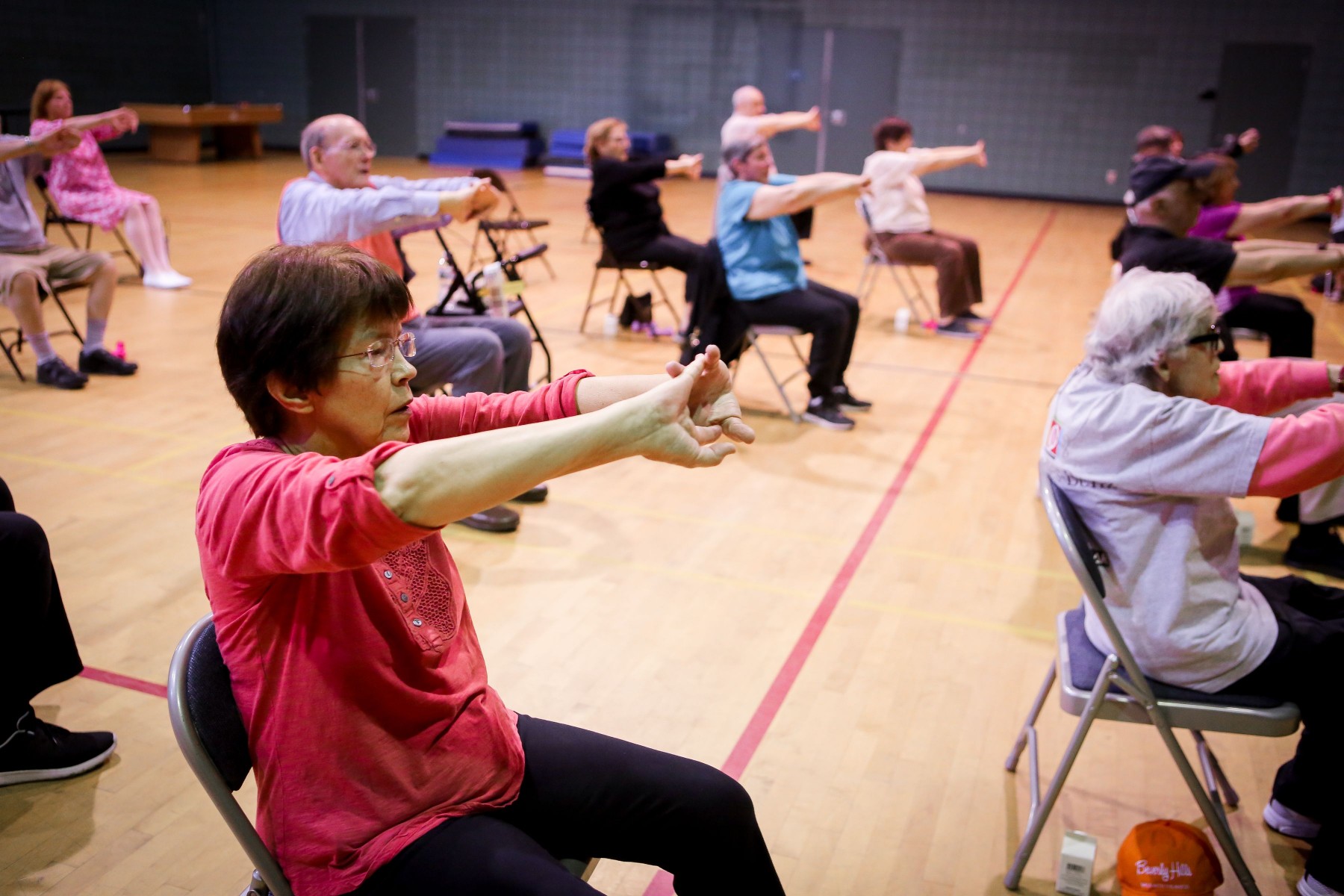
Nurse Scientists to Study Preventive Care of Low-Income Seniors
People age 80 and older account for 19% of patients at Cedars-Sinai, a figure that is expected to increase in the coming years as the general U.S. population ages. The proportion of these patients who are low-income also is growing. Nurse scientists from the Nursing Research Department at Cedars-Sinai are now studying how best to address preventive health services among older patients like these while reducing the potential strain on long-term care, hospitals and the healthcare system.

Cedars-Sinai Named Age-Friendly Health System
Shortly after COVID-19 was declared a pandemic, more than 450 older adults learned their weekly exercise classes offered through the Cedars-Sinai Geriatrics Program were on hold. But under the quick-thinking direction of geriatrician Allison Moser Mays, MD, the program pivoted, creating a way for seniors to access live classes over Zoom from the comfort of their homes. The online format has proved especially popular.
To Better Understand COVID-19, Researchers Review Aging, Immune Response to Viral Infections
As clinicians learn about a new disease in real-time, researchers are also investigating what lessons from other respiratory infections could apply to COVID-19.

Weekly Tip Sheet: Research News from Johns Hopkins Medicine NOT Related to COVID-19
Tip sheet with latest Johns Hopkins research news NOT related to COVID-19. Stories: more women & seniors needed in cholesterol drug trials, improving medical care quality for homebound seniors & 2020 JHM Science Writers Boot Camp goes virtual.

Caring for Those Most Vulnerable to COVID-19 Requires Vigilance
Early reports suggest the case fatality rate for those over 80, which constitutes nearly half of nursing home residents, is more than 15 percent. In areas where there is a shortage of ICU beds and respirators, even the most carefully thought out ethical approaches to rationing these resources will place older patients at a lower priority. Nursing homes must be prepared to manage patients who have had or have COVID-19 infection.

Novel Intervention in Senior Housing Communities Increases Resilience and Wisdom
Researchers at University of California San Diego School of Medicine, in collaboration with Mather Institute, developed a method to enhance resilience and reduce subjective stress in residents living in senior housing communities.

Lonely in a Crowd: Overcoming Loneliness with Acceptance and Wisdom
Researchers at University of California San Diego School of Medicine found the main characteristics of loneliness in a senior housing community and the strategies residents use to overcome it.
What Factors Influence the Decisions Older Adults Make About Their Care and Living Plans?
Northwestern Medicine Geriatrics receives nearly $4 million to better understand which factors influence older adults when making plans to age-in-place

New Diagnostic Criteria May Enable Earlier Detection of Cognitive Impairment in Women
Study finds when verbal memory test cut-offs were tailored to patient sex, more female patients and fewer male patients were considered to have amnesic mild cognitive impairment. This could change the way aMCI diagnoses are determined and make it easier to catch the condition in its early stages.
Rush University Medical Center Joins National Age-Friendly Health Systems Initiative
Rush University Medical Center has joined the national movement to improve health care for older adults by becoming the only hospital in Illinois to be part of the Age-Friendly Health Systems initiative.
Mount Sinai Ranked Among the Top in the Nation by U.S. News & World Report
The Hospital was ranked No. 14 nationally, up four spots from last year. Eight departments within the Hospital were ranked among the top 20 nationally in their specialties, up from five last year