A UCLA-led team has developed a machine-learning model that can predict with a high degree of accuracy the short-term survival of dialysis patients on Continuous Renal Replacement Therapy (CRRT).
Tag: Outcomes
MedStar Washington Hospital Center Again Named the Most Socially Responsible Hospital in the District
MedStar Washington Hospital Center is again the most socially responsible hospital in Washington, D.C. and is among the best in the nation, according to the Lown Institute, an independent think tank. It is ranked #1 in D.C., and is one of 154 hospitals to earn Honor Roll status with “A” grades in all top categories: Social Responsibility, Equity, Value, and Outcomes — key performance metrics that contribute to the overall rating.
After body contouring, bariatric surgery patients regain more weight than non-bariatric patients
Patients with previous bariatric surgery who undergo body contouring (BC) regain more weight at long-term follow-up, compared to BC patients who did not have bariatric surgery, reports a study in the November issue of Plastic and Reconstructive Surgery®, the official medical journal of the American Society of Plastic Surgeons (ASPS).
Study Reveals Patients Hospitalized with COVID-19 Faced Nearly Twice the Rates of Death After Discharge As Patients with Flu
Researchers demonstrate that among individuals who were admitted to the hospital with COVID-19 and were discharged alive, the risk of post-discharge death was nearly twice that observed in those who were discharged alive from an influenza-related hospital admission.
First-of-its-Kind Study Examines the Impact of Cannabis Use on Surgical Patients’ Post-Procedure Healthcare Needs
In patients who underwent non-cardiac surgery in Boston between 2008 and 2020, those with a diagnosed cannabis use disorder more often required advanced postprocedural healthcare compared to non-users. However, patients whose use of cannabis was not classified as a disorder had lower odds of requiring advanced healthcare after surgery compared to patients who never use cannabis.
Today’s Pediatric Heart Transplantations Involve Sicker Children, but Have Better Outcomes
A study of 323 pediatric heart transplants over 36 years at the University of Florida found that in recent years, more infants with serious congenital heart disease were offered heart transplants, but they had improved outcomes compared to patients in previous decades.
Academic medical centers are linked to better health outcomes at neighboring hospitals, researchers find
A new study suggests that the presence of academic medical centers within a healthcare market is linked to better outcomes for patients treated at nearby community hospitals.
New Method of Donor-Lung Distribution Expected to Decrease Deaths Among Those on Transplant Waiting List
A new method of donor-lung distribution is projected to decrease the number of candidate deaths who are on the waitlist for lung transplant, according to a study by Cleveland Clinic and the U.S. Scientific Registry of Transplant Recipients (SRTR) published in The American Journal of Transplantation.
Patients Believe in Psychotherapy More When Practitioners Demonstrate Warmth and Competence
Therapy is a collaborative process informed not just by a practitioner’s expertise but also by the patient’s expectations about that expertise and how likely they are to benefit from it. Research in Clinical Psychological Science suggests that therapists who demonstrate both warmth and competence can shape those expectations by inspiring more positive beliefs about the effectiveness of therapy.
Asian American / Pacific Islander Nurses Association and JMIR Publications Announce New Partnership to Publish Asian / Pacific Island Nursing Journal
Dr. Gunther Eysenbach, founder and CEO of JMIR Publications, says,
“Asian / Pacific Island Nursing Journal is an important addition to what we can offer as a publisher. I am thrilled to support the important voices and issues highlighted in the journal, and look forward to working with the Editor-in-Chief and editorial board to propel the title to the forefront of research on health disparities in minority patients.”
High risk of divorce after TBI? Not necessarily, study suggests
Traumatic brain injury (TBI) has a major impact on the lives of affected patients and families. But it doesn’t necessarily lead to an increased risk of marital instability, as two-thirds of patients with TBI are still married to the same partner 10 years after their injury, reports a study in the July/August issue of the Journal of Head Trauma Rehabilitation (JHTR). The official journal of the Brain Injury Association of America, JHTR is published in the Lippincott portfolio by Wolters Kluwer.

Cornell College students accepted into top health programs
The staff and faculty with Cornell College’s Dimensions Program for Health Professions are all smiles as they continue to hear the good news that many students have been accepted into top-tier graduate programs.
Pregnant Women Hospitalized for Covid-19 Infection Do Not Face Increased Risk of Death
Pregnant women who develop severe COVID-19 infections that require hospitalization for pneumonia and other complications may not be more likely to die from these infections than non-pregnant women. In fact, they may have significantly lower death rates than their non-pregnant counterparts.

Study: Race Made No Difference in ICU Outcomes of COVID-19 Patients
In a study that looked at racial differences in outcomes of COVID-19 patients admitted to the intensive care unit, researchers at Henry Ford Hospital in Detroit found that patients of color had a lower 28-day mortality than white patients.
Race, however, was not a factor in overall hospital mortality, length of stay in the ICU or in the rate of patients placed on mechanical ventilation, researchers said.
The findings, published in Critical Care Medicine, are believed to be one of the first in the United States to study racial differences and outcomes specific to patients hospitalized in the ICU with COVID-19.
American College of Surgeons verifies first hospital that meets its standardized quality criteria for geriatric surgery
The American College of Surgeons Geriatric Surgery Verification Program (ACS GSV) has announced that Unity Hospital, Rochester, N.Y., has achieved Level 1—Comprehensive Excellence verification status, which recognizes its commitment to providing optimal care for its older adult surgical patients by meeting the GSV’s program standards.
Life after COVID-19 hospitalization: Statewide study shows major lasting effects on health, work and more
Outcomes for COVID-19 patients two months after a stay in one of 38 Michigan hospitals include high rates of death, rehospitalization, lingering physical and mental health issues, problems with everyday activities and issues with work and finances.
Better Outcomes after Epilepsy Surgery in Kids with Poor Seizure Control
Epilepsy surgery in children with refractory epilepsy, who have poor seizure control with medications, results in better outcomes, according to a study published in the journal Neurosurgery.
New Study Reveals 75% of Multiple Sclerosis Patients Face Financial Toxicity
A new study from Harvey L. Neiman Health Policy Institute finds that over ¾ of Multiple Sclerosis (MS) patients face financial toxicity that often results in non-adherence to follow up care. This Multiple Sclerosis Journal study is the first of its kind to evaluate financial toxicity in MS patients and whether financial hardship is linked to patients foregoing the therapy and imaging follow-up prescribed in their treatment plan.
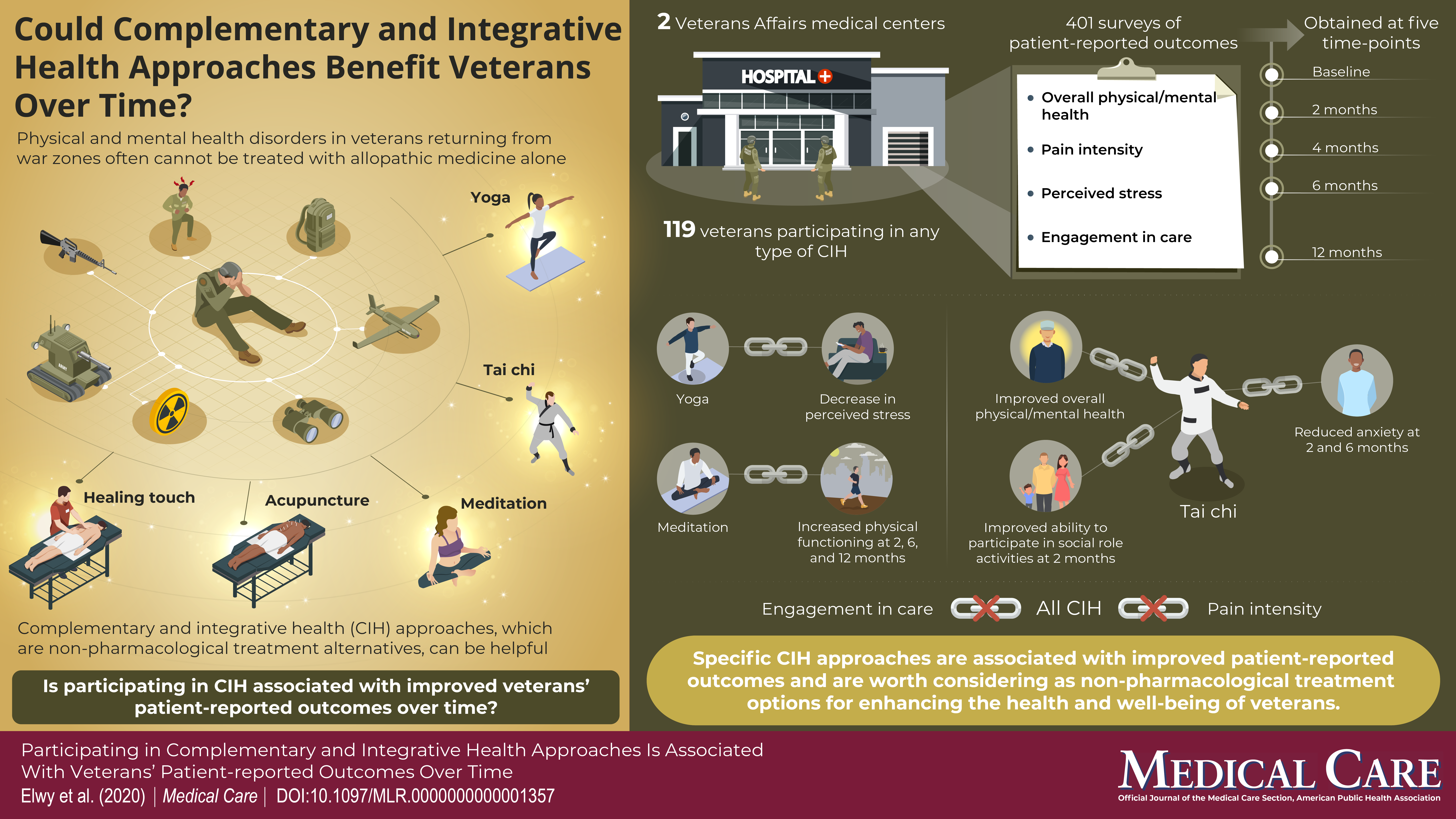
Yoga, Tai Chi, and Meditation Bring Specific Benefits for Veterans
Three popular complementary and integrative health (CIH) therapies – yoga, tai chi, and meditation – lead to significant improvements in key outcomes perceived by Veterans receiving care in the Veterans Health Administration (VA) system, suggests a study in a special September supplement to Medical Care. The journal is published in the Lippincott portfolio by Wolters Kluwer.

Number of Hospitalizations Can Be Important Clinical Indicator for Head, Neck Cancer Patients
Patients who were unexpectedly hospitalized for dehydration, fever or other ailments while undergoing radiation treatment for head and neck cancers were at a higher risk for less favorable outcomes, a new study from Roswell Park Comprehensive Cancer Center reports.

Genetics Researchers Find Easy Way to Improve Cancer Outcomes
By mining a vast trove of genetic data,researchers at the University of Virginia School of Medicine are enhancing doctors’ ability to treat cancer, predict patient outcomes and determine which treatments will work best for individual patients. The researchers have identified inherited variations in our genes that affect how well a patient will do after diagnosis and during treatment.

Class of 2019: 99% of Graduates Employed in Major or Chosen Field
According to a newly published report, 99 percent of recent Augustana University graduates seeking employment are employed in their major or chosen field.
Primary Care Declines in America
National analysis reveals alarming decline in primary care use. Primary care is associated with better health outcomes than episodic, inconsistent care.

Artificial Intelligence Tool Predicts Life Expectancy in Heart Failure Patients
Researchers at University of California San Diego School of Medicine, as well as a diverse team of cardiologists and physicists, developed a machine learning algorithm to predict the life expectancy in heart failure patients.
Retrospective study suggests emergency department physicians are improving both outcomes and efficiency of care
In a new study published today in JAMA Internal Medicine, a team of researchers led by Laura Burke, MD, MPH, an emergency medicine physician at BIDMC, found that among Medicare beneficiaries receiving ED care in the United States, mortality within 30 days of an ED visit has declined in recent years, particularly for the highest-severity patients.