Background: Cancer-related hospitalizations constitute one of the primary drivers of cancer-related healthcare expenses. Understanding the burden and characteristics of these hospitalizations is essential to appropriately direct resources, improve outcomes, and avoid unnecessary hospitalizations. Our study sought to evaluate the national…
Tag: Hospitalization
Antipsychotic Injections Linked to a Sharp Drop in Hospital Readmissions
A Rutgers Health study supports long-acting shots over daily pills for patients with schizophrenia or schizoaffective disorder.
Analysis suggests access to primary care could play an important role in reducing hospitalizations
A secondary analysis of a randomized encouragement study found that Medicare patients who received social needs case management had a 3% increase in primary care visits and an 11% reduction in inpatient hospitalizations. These findings suggest that increased access to primary care could play an important role in reducing acute care use. A brief research report is published in Annals of Internal Medicine.
Medicaid Expansion Reduced Black-White Disparities in Preventable Hospital Visits
Improving access to care for underserved communities improved a crucial health measure.
High-Dose Anticoagulation Can Reduce Intubations and Improve Survival for Hospitalized COVID-19 Patients
High-dose anticoagulation can reduce deaths by 30 percent and intubations by 25 percent in hospitalized COVID-19 patients who are not critically ill when compared to the standard treatment, which is low-dose anticoagulation.
Transcatheter Mitral Valve Repair in Heart Failure Patients Significantly Reduces Hospitalizations and Improves Survival
Breakthrough findings from study led by Mount Sinai researcher could improve outcomes for high-risk patients
Nanoparticle Therapy May Help Patients Hospitalized with Severe COVID-19 Infections
Johns Hopkins Medicine researchers say that an experimental dendrimer nanoparticle treatment called OP-101 substantially reduced the risk of death and need for a ventilator in a study of 24 severely ill adults hospitalized with COVID-19.
Vitamin D supplement ‘overdosing’ is possible and harmful, warn doctors
‘Overdosing’ on vitamin D supplements is both possible and harmful, warn doctors in the journal BMJ Case Reports after they treated a man who needed hospital admission for his excessive vitamin D intake.
COVID-19 vaccine protects people of all body weights from hospitalization and death, study of 9 million adults in England suggests
COVID-19 vaccines greatly reduced the number of cases of severe COVID-19 disease for everyone regardless of their body size, according to a new study published in The Lancet Diabetes & Endocrinology. Vaccine effectiveness was similar for those with a higher BMI and of a healthy weight, but slightly lower in the underweight group, who were also the least likely to have been vaccinated.
Study Finds Increased Risk of Dementia After Hospitalization for Major TBI
People who have been hospitalized for a major traumatic brain injury (TBI) may have a higher risk of developing dementia when compared to people who do not have a TBI, according to a new study published in the May 11, 2022, online issue of Neurology®, the medical journal of the American Academy of Neurology.
New Oral Antiviral Drug Reduces Death in Early COVID-19
Researchers note that health care providers are now able to add to their armamentarium against COVID-19 their prescription of this new antiviral drug for high-risk, newly-infected patients as soon as possible following diagnosis or within five days of the onset of symptoms.
UCI-led study finds disparities in severe illness and lengthy hospitalizations between undocumented and Medi-Cal patients
Lithium is a common medication prescribed to patients with psychiatric disorders, namely bipolar disorder, schizophrenia, and depression. It is used as a mood stabilizer and lessens the intensity of manic episodes, with particular benefit in reducing suicidality. While highly effective, the drug requires routine blood monitoring, which can be uncomfortable, expensive, and inconvenient for patients who must travel to clinical labs for frequent blood testing.
Chance of postoperative complications after hospital discharge increases with shorter hospitalization
New study results suggest the national trend toward decreasing length of hospitalization after surgical procedures may come at the expense of an increasing proportion of complications occurring after patients leave the hospital.
As COVID-19 and Online Misinformation Spread, Children and Teens Were Poisoned with Hand Sanitizer and Alcoholic Drinks
During the early months of the COVID-19 pandemic, as false health information spread on social media, the number of children and teens poisoned with hand sanitizer or alcoholic beverages surged in Iran. These poisonings resulted in hundreds of hospitalizations and 22 deaths. Misinformation circulating on social media included the false suggestion that consuming alcohol (methanol) or hand sanitizer (ethanol or isopropyl alcohol) protected against COVID-19 infection (it does not). A major alcohol poisoning outbreak sickened nearly 6,000 Iranian adults, of whom 800 died. It was not known, however, to what extent children and adolescents were affected. For the study in Alcoholism: Clinical & Experimental Research, investigators compared pediatric hospitalizations for ethanol and methanol poisoning during the early COVID-19 pandemic in Iran with the same period the previous year. They also looked at types of exposure and how those were linked to the children’s ages and clinical outcomes.
Delivery for hospitalized pregnant women improves recovery outcome, study finds
Pregnant women hospitalized with COVID-19 had improved recovery outcomes after delivering their babies early, according to new research from The University of Texas Health Science Center at Houston (UTHealth).
New study suggests pregnant women hospitalized for COVID-19 do not face increased risk of death
Pregnant women who are hospitalized with COVID-19 and viral pneumonia are less likely than non-pregnant women to die from these infections, according to a new study by researchers with The University of Texas Health Science Center at Houston (UTHealth) and the University of Maryland School of Medicine (UMSOM).
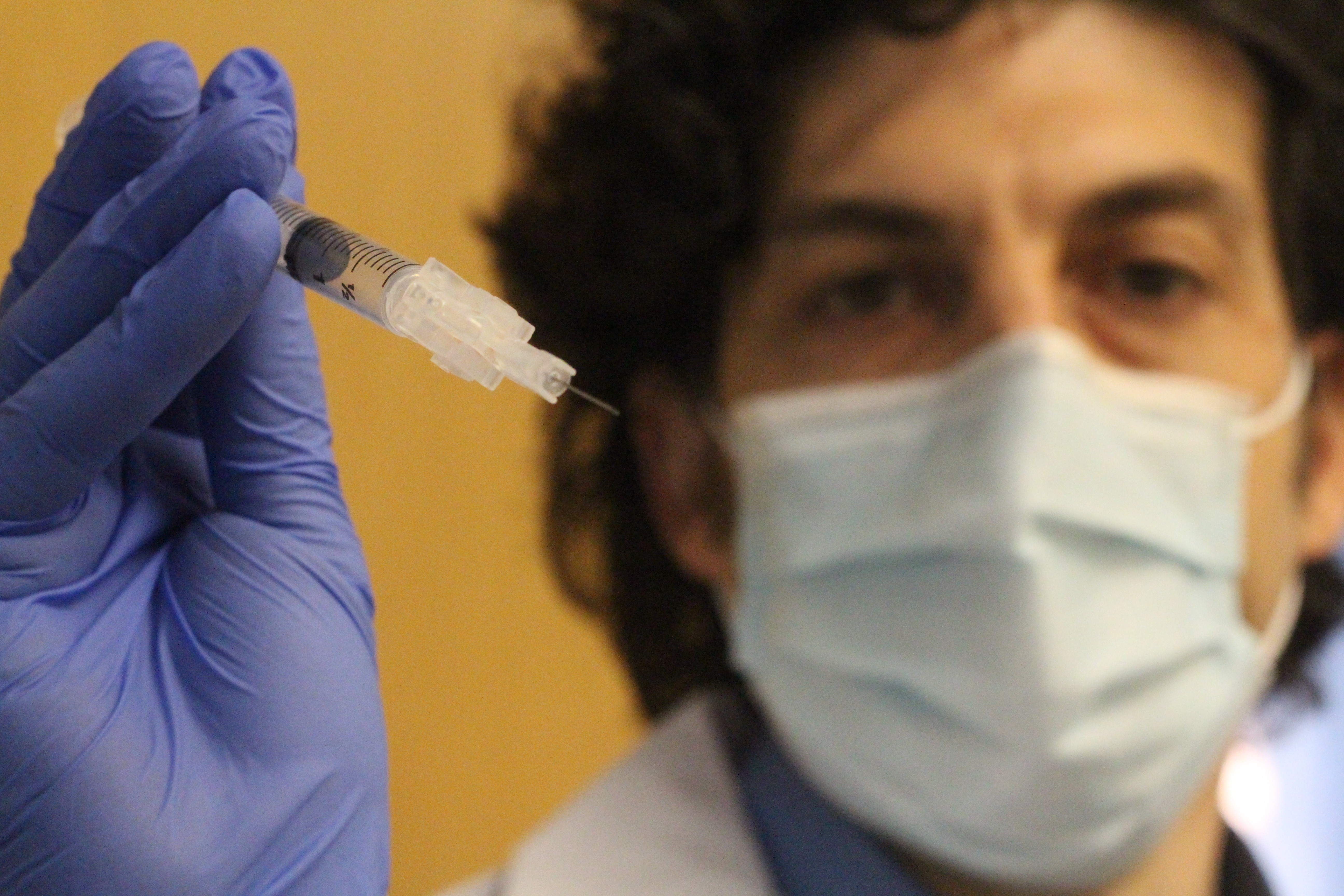
Peginterferon-lambda shows strong antiviral action to accelerate clearance of COVID-19
A clinical study led by Dr. Jordan Feld, a liver specialist at Toronto Centre for Liver Disease, University Health Network (UHN), showed an experimental antiviral drug can significantly speed up recovery for COVID-19 outpatients – patients who do not need to be hospitalized. This could become an important intervention to treat infected patients and help curb community spread, while COVID-19 vaccines are rolled out this year.
Research finds people diagnosed with HIV in New York State were more than twice as likely to die from COVID-19
New research out of the University at Albany and the AIDS Institute at the New York State Department of Health found that through the middle of 2020, people diagnosed with HIV infection were significantly more likely to contract, be hospitalized with and die from COVID-19.
Largest Study of Its Kind Identifies Which COVID-19 Patients Face the Greatest Risk of Mortality During Hospitalization
Hospitalized COVID-19 patients have a greater risk of dying if they are men or are obese or have complications from diabetes or hypertension, according to a new study conducted by University of Maryland School of Medicine (UMSOM) researchers. In a study published in the journal Clinical Infectious Diseases, the researchers evaluated nearly 67,000 hospitalized COVID-19 patients in 613 hospitals across the country to determine link between common patient characteristics and the risk of dying from COVID-19.
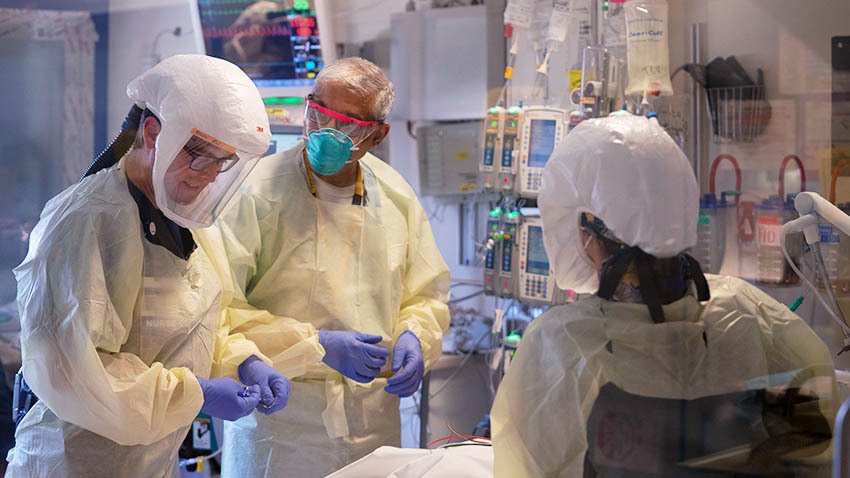
Life after COVID-19 hospitalization: Statewide study shows major lasting effects on health, work and more
Outcomes for COVID-19 patients two months after a stay in one of 38 Michigan hospitals include high rates of death, rehospitalization, lingering physical and mental health issues, problems with everyday activities and issues with work and finances.

Remdesivir for COVID-19: FDA Approved but Still Unproven
In a review of evidence from the most reliable data from randomized trials to find likely small-to-moderate effects of remdesivir, researchers say that totality of evidence compiled before the WHO trial results justifies compassionate use of remdesivir for severely ill patients. A smaller trial in China showed significantly decreased mean recovery time but no suggestion of a mortality benefit. ACTT-1 found the same mean recovery time and a suggestion of a mortality benefit that did not achieve statistical significance.

COVID-19 Recovery at Home Possible for Most Patients
A new study shows that the vast majority of patients who visited the Ruth and Harry Roman Emergency Department at Cedars-Sinai with suspected COVID-19 (novel coronavirus) symptoms, and who were treated and sent home to recuperate, recovered within a week.

Prevent Severe COVID Symptoms With Lifestyle Changes
Obesity is contributing to worse outcomes in people with COVID-19. Dr. Naomi Parrella, medical director of the Rush Center for Weight Loss and Bariatric Surgery, explains how managing your weight can lower your risk for severe COVID symptoms and help you prevent other chronic diseases.
COVID-19 may have been in L.A. as early as last December, UCLA-led study suggests
UCLA researchers and colleagues who analyzed electronic health records found that there was a significant increase in patients with coughs and acute respiratory failure at UCLA Health hospitals and clinics beginning in late December 2019, suggesting that COVID-19 may have been circulating in the area months before the first definitive cases in the U.S. were identified. This sudden spike in patients with these symptoms, which continued through February 2020, represents an unexpected 50% increase in such cases when compared with the same time period in each of the previous five years.

Number of Hospitalizations Can Be Important Clinical Indicator for Head, Neck Cancer Patients
Patients who were unexpectedly hospitalized for dehydration, fever or other ailments while undergoing radiation treatment for head and neck cancers were at a higher risk for less favorable outcomes, a new study from Roswell Park Comprehensive Cancer Center reports.
Homeless Patients Are More Likely to be Readmitted to a Hospital Within 30 Days of Discharge
Patients who are homeless are far more likely than housed individuals to be readmitted to a hospital within 30 or 90 days of their discharge, according to a new multi-center analysis of inpatient data from Florida, Massachusetts and New York.

Homeless people are more likely to be put on ventilators for respiratory infections than non-homeless
Researchers from UCLA, Harvard Medical School and the University of Tokyo found that during a recent six-year period, homeless people in New York state were more likely to hospitalized and treated with mechanical ventilators for respiratory infections than people who are not homeless. These findings have implications for the COVID-19 pandemic.

JNCCN: Many Hospitalized People with Advanced Cancer Struggle with Important Daily Tasks
New research from Mass General Cancer Center, published in the June 2020 issue of JNCCN—Journal of the National Comprehensive Cancer Network, found 40.2% of hospitalized patients with advanced, incurable cancer were functionally impaired at the time of admission.
Children Not Immune to Coronavirus; New Study from Pandemic Epicenter Describes Severe COVID-19 Response in Children
While most children infected with the novel coronavirus have mild symptoms, a subset requires hospitalization and a small number require intensive care. A new report from pediatric anesthesiologists, infectious disease specialists and pediatricians at the Children’s Hospital at Montefiore (CHAM) and Albert Einstein College of Medicine, describes the clinical characteristics and outcomes of children hospitalized with COVID-19, during the early days of the pandemic.

Vitamin D Boosts Chances of Walking After Hip Fracture
Senior citizens who are not vitamin D deficient have a better chance of walking after hip fracture surgery, according to a Rutgers-led study. The findings in The American Journal of Clinical Nutrition suggest that vitamin D deficiency could limit mobility in older adults, said senior author Sue Shapses, a professor in the Department of Nutritional Sciences at the School of Environmental and Biological Sciences at Rutgers University–New Brunswick.
Low-income older adults dually enrolled in Medicare and Medicaid have substantially higher mortality rates than adults solely enrolled in Medicare
In a new study published today in JAMA, a team of researchers at Beth Israel Deaconess Medical Center (BIDMC) evaluated how health outcomes for low-income older adults who are dually enrolled in both Medicare and Medicaid have changed since the early 2000s.