The highly infectious bird flu, also known as avian influenza H5N1, primarily spreads among birds. However, there have been rare cases of infection to humans. According to the Centers for Disease Control and Prevention, two human cases of H5N1 have…

news, journals and articles from all over the world.

The highly infectious bird flu, also known as avian influenza H5N1, primarily spreads among birds. However, there have been rare cases of infection to humans. According to the Centers for Disease Control and Prevention, two human cases of H5N1 have…
In a first, the study published in the journal Emerging Microbes and Infections demonstrated the team’s patented therapeutic candidate, an HIV-virus-like-particle (HLP), is 100 times more effective than other candidate HIV cure therapeutics for people living with chronic HIV on combined antiretroviral therapy (cART).
Research co-led by an investigator at Johns Hopkins Children’s Center shows that four children born with HIV who were safely removed from antiretroviral therapy (ART) continued to have undetectable levels of the virus for about a year or more without treatment. The children were among 54 newborns who were given very early treatment within the first 48 hours of life — rather than within weeks or months, as is typical.
[email protected]
KINGSTON, R.I. – Feb. 26, 2024 – In the 1980s, as a poetry student in Italy, Peter Covino was introduced to the work of acclaimed Italian poet Dario Bellezza. It’s a moment he still remembers.“It was a big deal to learn at that time that there was this really wild, irreverent writer exploring ideas that I didn’t realize would speak to me so directly,” says Covino, associate professor of English at the University of Rhode Island.
As the Measles outbreak continues to grow in Florida, Francesca Torriani, MD, infectious disease specialist with UC San Diego Health is available to discuss symptoms to look out for, when to seek medical care, and the importance of vaccination. Biography…
Since 2017, the lab of Rahima Benhabbour, PhD, MSc, associate professor in the UNC/NCSU Joint Department of Biomedical Engineering, has been working with a research team at the Centers for Disease Control and Prevention (CDC) and others at UNC to develop an injectable implant that can release HIV pre-exposure prophylaxis (PrEP) medications into the body for a long period of time.
Their latest research, published in Nature Communications, shows that the team’s latest formulation can provide up to six months of full protection.

The Midwest AIDS Training and Education Center at the University of Illinois Chicago will expand its services nationwide with the help of a new $3 million grant.
An embargoed study published in the Aug. 22, 2022 issue of Nature Medicine identifies a new biomarker that appears effective as a surrogate endpoint to reliably predict the ability of broadly neutralizing monoclonal antibodies to prevent acquisition of HIV-1, the most common type of the virus that causes AIDS. Broadly neutralizing antibodies (bnAbs) are defined by their ability to neutralize multiple genetically distinct viral strains.
A University of Utah Health-led multi-institutional research center that studies the inner workings and vulnerabilities of HIV, the human immunodeficieny virus that causes AIDS, recently received a five-year, $28 million grant renewal from the National Institutes of Health.
Special issue includes research and commentary addressing important considerations for national PrEP program that would lower prices and expand access.
HIV has an “early and substantial” impact on aging in infected people, accelerating biological changes in the body associated with normal aging within just two to three years of infection.
Article title: Wonder of Wonders, Miracle of Miracles: The Unprecedented Speed of COVID-19 Science Author: Michael Saag From the author: “Although a wide variety of scientific disciplines established the platform upon which the remarkable response to COVID-19 was based, the study…
Conforme as famílias se reúnem para as festas de final de ano, é importante que os pacientes imunocomprometidos tomem medidas extras para ajudar a se proteger da COVID-19. Pessoas com o sistema imunológico enfraquecido correm maior risco de adoecer gravemente com a COVID-19.
The new study provides valuable insights into the genetic variants associated with HIV-1C infection and AIDS progression in sub-Saharan Africa, potentially paving the way for new therapies.
Researchers at Albert Einstein College of Medicine and the City University of New York Graduate School of Public Health and Health Policy (CUNYSPH) have been awarded a five-year, $14.5 million grant from the National Institutes of Health (NIH) to continue leading and expand their research on HIV treatment and care in five Central African nations.
A team led by Dan H. Barouch, MD, PhD, has been awarded $4.9 million in annual funding over the next five years to find a cure for HIV. Barouch was one of ten primary investigators to receive a 2021 National Institutes of Health (NIH) Martin Delaney Collaboratories for HIV Cure Research award, which aims to expedite human immunodeficiency virus (HIV) cure research by bringing together research partners in academia, government, the private sector and the community; coordinating complex research studies, and mentoring the next generation of HIV cure researchers.
A team of researchers co-led by UCLA Fielding School of Public Health epidemiology professor Dr. Matthew Mimiaga has received more than $5.2 million in grants from the U.S. National Institutes of Health (NIH) to develop and test interventions in the U.S. and Brazil.
A new study by researchers at Penn State College of Medicine indicates that people living with human immunodeficiency virus (HIV) and acquired immune deficiency syndrome (AIDS) — approximately 38 million worldwide — are more likely to have suicidal thoughts and die from suicide than members of the general population.
O mês de junho marca o 40º aniversário do primeiro relatório científico descrevendo a pneumocistose, que depois passou a ser conhecida como síndrome da imunodeficiência adquirida (AIDS).
A groundbreaking study found that stem cells reduce the amount of virus causing AIDS, boost the body’s antiviral immunity, and restore the gut’s lymphoid follicles damaged by HIV. It provided a roadmap for multi-pronged HIV eradication strategies.
A comprehensive health-screening program in rural northern KwaZulu-Natal, South Africa, has found a high burden of undiagnosed or poorly controlled non-communicable diseases, according to a study published in The Lancet Global Health.
Mount Sinai Health System has recruited an internationally recognized expert in the management of breast cancer and HIV-associated malignancies, Joseph A. Sparano, MD, FACP, as Chief of Hematology and Medical Oncology and Deputy Director of The Tisch Cancer Institute (TCI). Dr. Sparano will also hold the Ezra M. Greenspan, MD Professorship in Clinical Cancer Therapeutics at the Icahn School of Medicine at Mount Sinai and will oversee the expansion of clinical and research capacities of the Division and TCI.
SEATTLE — June 2, 2021 — Below are summaries of recent Fred Hutch research findings and other news. If you are covering news at the annual meeting of the American Society of Clinical Oncology (June 4-8), check out our ASCO page highlighting Fred Hutch presentations and feel free to reach out to our media team for help sourcing experts: media@fredhutch.
Saturday, June 5, marks the 40th anniversary of the first official reported cases of what became known as AIDS. The University of Michigan has experts who can discuss. Celeste Watkins-Hayes is a professor of public policy and sociology as well…
On June 5, it will be 40 years since the CDC published an article in their Morbidity and Mortality Weekly Report which described Pneumocystis pneumonia in previously healthy, gay men in LA. The report was the first official reporting of…
Laurie Garrett, a Pulitzer-Prize-winning journalist, has been named the 2021 Senator Frank R. Lautenberg Awardee by the Rutgers School of Public Health. She will serve as the School’s speaker at their 38th graduation ceremony, which will virtually launch on May 14, 2021.
A UCLA research team has shown that using a truncated form of the CD4 molecule as part of a gene therapy to combat HIV yielded superior and longer-lasting results in mouse models than previous similar therapies using the CD4 molecule.

Dr. Matthew Mimiaga, director of the UCLA Center for LGBTQ Advocacy, Research & Health (C-LARAH), leads $8.8 million project HIV prevention project funded by the National Institutes of Health
A study led by researchers at the Johns Hopkins Bloomberg School of Public Health found that just under 20 percent of HIV-uninfected patients visiting Baltimore sexual health clinics were aware of pre-exposure prophylaxis medication (PrEP), a daily regimen that decreases a person’s risk of contracting HIV from sex by more than 90 percent.
The AIDS Clinical Trials Group (ACTG), the largest global HIV research network, will present four oral and 20 scientific spotlight sessions at the Conference on Retroviruses and Opportunistic Infections (CROI 2021) held virtually, March 6-10.
New research out of the University at Albany and the AIDS Institute at the New York State Department of Health found that through the middle of 2020, people diagnosed with HIV infection were significantly more likely to contract, be hospitalized with and die from COVID-19.
The AIDS Clinical Trials Group (ACTG), the largest global HIV research network, has been re-funded for the next seven years by the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health (NIH), and collaborating NIH Institutes.

The Arnhold Institute for Global Health at the Icahn School of Medicine Mount Sinai will host a virtual event on World AIDS Day.
World AIDS Day During COVID-19: AU Experts Offer Insights What: How have lessons from the HIV/AIDS pandemic inform our response to COVID-19? What has been the impact of COVID-19 on people living with HIV/AIDS and HIV research? AU experts are…

Rutgers School of Public Health instructor, Stephanie Shiau, has been awarded a Eunice Kennedy Shriver National Institute of Child Health & Human Development of the National Institutes of Health R21 grant to examine the effect of HIV infection and/or exposure during pregnancy on epigenetic patterns in children.
Untreated HIV infection is linked with epigenetic changes suggesting rapid aging. A new study by UCLA researchers shows that antiretroviral therapy given over two years was unable to completely restore age-appropriate epigenetic patterns, leaving patients more susceptible to aging-related illnesses.
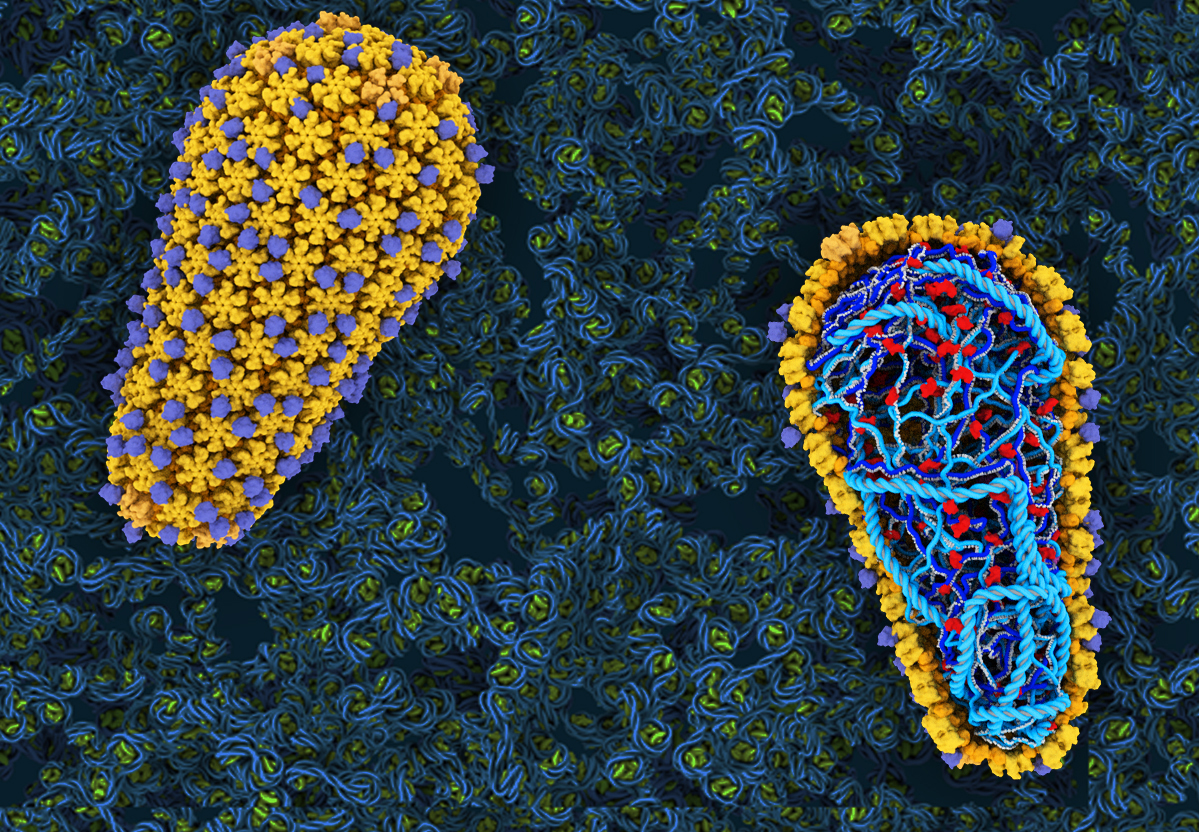
Accomplishing a feat that had been a pipe dream for decades, scientists at University of Utah Health and University of Virginia have recreated in a test tube the first steps of infection by HIV (human immunodeficiency virus), the virus that causes AIDS (acquired immunodeficiency syndrome). Doing so has provided up-close access to the virus—which is otherwise obstructed from view deep within the cell—and enabled identification of essential components that HIV needs to replicate within its human host. The research publishes in the journal, Cell.

In a new study, infectious disease researchers show that HIV viremia isn’t always nonadherence to medication or resistance to the drugs. Instead, the patients are victims of what the scientists have dubbed “repliclones” – large clones of HIV-infected cells that produce infectious virus particles.
The Chicago Center for HIV Elimination, housed at the University of Chicago, has been awarded $5 million over two years through the National Institute of Health’s (NIH) RADx Underserved Populations program to support a COVID-19 testing project to engage two disenfranchised populations.

The widespread use of antiretroviral therapy to suppress the HIV virus has helped tens of millions of people with HIV live healthier, longer lives—but an unfortunate consequence of people living longer with HIV is an increased risk of cancer. For 25 years, the AIDS Malignancy Consortium (AMC) has led national and international efforts to prevent and treat of HIV-related cancers. Now, Montefiore Health System and Albert Einstein College of Medicine have received a five-year, $111 million grant from the National Cancer Institute (NCI) to lead this research consortium.
For Black women in the southern United States, mistrust of the health care system that is grounded in structural and systemic racism is a key factor affecting participation in HIV prevention and treatment services, reports a study in the September/October issue of The Journal of the Association of Nurses in AIDS Care (JANAC). The official journal of the Association of Nurses in AIDS Care, JANAC is published in the Lippincott portfolio by Wolters Kluwer.
IHV announced today that Shenghan Lai, MD, MPH and Hong Lai, PhD, MPH, in addition to three staff members, and two more to add, have joined the Institute of Human Virology. The faculty began their positions on April 1 with Professor and Associate Professor academic appointments in the UMSOM’s Department of Epidemiology & Public Health.
A multiple sclerosis drug may be used to block HIV infection and reduce the latent reservoir, according to research published in PLOS Pathogens by a team at the RGeorge Washington University.

Men at particular risk for HIV are very likely to consistently take prevention medication during vacations when their odds of contracting the virus are higher, according to a new study.
New Brunswick, N.J. (Aug. 3, 2020) – Rutgers University–New Brunswick Professor Robert E. Kopp is available to discuss a major study released today on the global consequences of climate change on death rates. The study by the Climate Impact Lab,…
The new Center for Collaborative HIV Research in Practice and Policy at the University at Albany will address the public health and social justice challenges of persons placed at risk for, or living with, HIV and related diseases.

Nurses Alison Moëd and Cliff Morrison will receive AACN Pioneering Spirit Awards for their efforts to transform treatment for patients with AIDS in the early 1980s. Together, they created the San Francisco Model, a patient-centered approach that improved the care for their patients and countless others around the world.
Scientists at Sanford Burnham Prebys Medical Discovery Institute have created a next-generation drug called Ciapavir (SBI-0953294) that is effective at reactivating dormant human immunodeficiency virus (HIV). The research, published in Cell Reports Medicine, aims to create a functional HIV cure by activating and then eliminating all pockets of dormant HIV—an approach called “shock and kill.”
Topics include the efficacy and safety of third-line treatment regimens in resource-limited settings, viral rebound rates after treatment interruption of modern ART, and whether a standardized frailty score can improve clinicians’ ability to estimate cardiovascular risk among older people with HIV.

Satya Dandekar, professor of microbiology and chairperson of the Department of Medical Microbiology and Immunology at UC Davis, honored by Prestigious NIH MERIT award for her illustrious journey in HIV research.