A new “armored” form of CAR T cell therapy may be able to help patients with non-Hodgkin lymphoma whose cancers do not respond to currently available CAR T cell therapies. The Phase I clinical trial was presented at the 2024 ASCO Annual Meeting.
Tag: CAR T cell therapy
Moffitt Treats First Clinical Trial Patient with Gamma Delta CAR T for Bone Metastatic Prostate Cancer
Moffitt Cancer Center has treated its first patient in an investigator-initiated, phase 1 clinical trial investigating the safety and efficacy of a chimeric antigen receptor T-cell (CAR T) therapy for prostate cancer that has metastasized to the bone.
CHOP, Stanford Researchers Identify Protein That Controls CAR T Cell Longevity
CAR T cell therapy has revolutionized the way certain types of cancer are treated, and the longer those CAR T cells live in a patient’s body, the more effectively they respond to cancer. Now, researchers have found that a protein called FOXO1 improves the survival and function of CAR T cells, which may lead to more effective CAR T cell therapies and could potentially expand its use in difficult-to-treat cancers.
AACR: Novel immunotherapies show promise for patients with kidney cancer and for solid organ transplant recipients with skin cancer
Researchers from The University of Texas MD Anderson Cancer Center presented encouraging findings today from two clinical trials in a plenary session highlighting advances in novel immunotherapy approaches at the American Association for Cancer Research (AACR) Annual Meeting 2024.
Promising target for CAR T-cell therapy leads to potent antitumor responses against cutaneous and rare melanomas
Scientists at the UCLA Health Jonsson Comprehensive Cancer Center have built and demonstrated the potential efficacy of a new chimeric antigen receptor (CAR) T-cell-based immunotherapy specifically designed to treat patients with cutaneous and rare subtypes of melanoma.
Scientists engineer potent immune cells for ‘off-the-shelf’ cancer immunotherapy
UCLA scientists have developed a new method to engineer more powerful immune cells that can potentially be used for “off-the-shelf” cell therapy to treat challenging cancers.
Researchers identify ‘switch’ to activate cancer cell death
A research team from the UC Davis Comprehensive Cancer Center has identified a crucial epitope (a protein section that can activate the larger protein) on the CD95 receptor that can cause cells to die.
MD Anderson Research Highlights for October 4, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention. These advances are made possible through seamless collaboration between MD Anderson’s world-leading clinicians and scientists, bringing discoveries from the lab to the clinic and back. Recent developments at MD Anderson include a computer game that helps breast cancer survivors improve symptoms of peripheral neuropathy, a publicly available single-cell atlas of CD19 chimeric antigen receptor (CAR) T cells, new targets for TP53-mutant acute myeloid leukemia (AML), a preclinical target for preventing chemobrain, a blood test to help identify patients at higher risk of developing pancreatic cancer, and genomic insights to predict the risk of outcomes in patients with bone cancer.
MD Anderson Research Highlights for August 30, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention. These advances are made possible through seamless collaboration between MD Anderson’s world-leading clinicians and scientists, bringing discoveries from the lab to the clinic and back.
Recent developments include a novel computational tool to detect single base pair DNA changes in single-cell sequencing data, a potential target to treat hypertension caused by drugs commonly used in organ transplants, further insights into the steps involved in genetic recombination, a novel treatment target for a subset of adenoid cystic carcinoma (ACC), a combination therapy that improves outcomes in certain patients with acute myeloid leukemia (AML), and a target for treating prolonged cytopenia in patients with relapsed/refractory large B cell lymphoma treated with chimeric antigen receptor (CAR) T cell therapy.
Cancer Research Institute Hosts 11th Annual Cancer Immunotherapy Month™ Showcasing Lifesaving Breakthroughs in Immuno-Oncology
Global celebration of 11 years of discovery and lifesaving innovation in immuno-oncology
MD Anderson Research Highlights for March 29, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention.
Gut Microbiome Influences How Lymphoma Patients Respond to CAR T Therapy
In a new study published in Nature Medicine, Moffitt Cancer Center physician-scientists, in collaboration with four cancer centers in the United States and Germany, reveal how microorganisms in the gut influence non-Hodgkin lymphoma patient outcomes to a type of cellular immunotherapy called chimeric antigen receptor T-cell therapy, or CAR T.
St. Jude scientists create more efficient CAR immunotherapies using a molecular anchor
St. Jude scientists added a small physical structure called an anchor domain to the CAR molecule. The anchor domain connects the CAR to the internal infrastructure of the immune cell. It augments and helps organize the immune synapse
Penn Medicine at the 2022 ASH Meeting
Researchers from the Abramson Cancer Center and Perelman School of Medicine at the University of Pennsylvania will be presenting data on the latest advances in blood cancer research and treatment at the 2022 American Society of Hematology (ASH) Annual Meeting from December 10-13.
MD Anderson Research Highlights for August 24, 2022
The University of Texas MD Anderson Cancer Center’s Research Highlights provides a glimpse into recent basic, translational and clinical cancer research from MD Anderson experts. Current advances include confirmation of improving response rates in Phase I trials over the last 20 years, a novel targeted therapy combination and biomarkers of response for chimeric antigen receptor (CAR) T cell therapy in B-cell lymphomas, a combination therapy for patients with melanoma brain metastases, and new treatment options for metastatic sarcomas, HPV-driven cancers and uterine cancer.
MD Anderson Research Highlights for July 13, 2022
The University of Texas MD Anderson Cancer Center’s Research Highlights provides a glimpse into recent basic, translational and clinical cancer research from MD Anderson experts. Current advances include new targets involved in protecting DNA replication forks and preventing inflammatory responses, a new treatment option for elderly patients with late-stage acute myeloid leukemia, insights into the breast cancer tumor microenvironment, biomarkers of response to targeted and immune therapies, a novel cellular therapy option for osteosarcoma and a new target for inducing ferroptosis in cancer cells.
Pushing T cells down “memory lane” may improve cancer therapy
Scientists at St. Jude Children’s Research Hospital identified proteins that help decide T cell fate and used the finding to improve CAR-T cell therapy in a solid tumor model.
MD Anderson researchers present cellular therapy advances at the 2022 ASCO Annual Meeting
Promising clinical results with cellular therapies for patients with blood cancers highlight advances being presented by researchers from The University of Texas MD Anderson Cancer Center at the 2022 American Society of Clinical Oncology (ASCO) Annual Meeting.
These findings include long-term outcomes of patients receiving an infusion of brexucabtagene autoleucel (KTE-X19) for mantle cell lymphoma, efficacy of gamma delta CAR T therapy for aggressive B-cell lymphoma and responses of umbilical cord blood-derived expanded natural killer cells when given together with combination therapy before stem cell transplant.
MD Anderson and Resilience launch joint venture to accelerate development and manufacturing of innovative cell therapies for cancer
MD Anderson and Resilience today announced the launch of a joint venture, the Cell Therapy Manufacturing Center, which unites the strengths of both parties to accelerate the development and manufacturing of cell therapies for patients with cancer.
MD Anderson Research Highlights for June 1, 2022
Current advances include new biomarkers to predict chimeric antigen receptor (CAR) T cell therapy outcomes and neurotoxicities, novel treatment targets for pre-cancerous pancreatic lesions and T-cell acute lymphoblastic leukemia, a new approach to improve immunotherapy responses in cold tumors, a profile of synthetic lethal targets for cancers with tumor suppressor loss, and promising clinical data for acute myeloid leukemia and cancers of unknown primary.
Cancer Research Institute Hosts 10th Annual Cancer Immunotherapy Month™ Celebrating Lifesaving Discovery in Immuno-Oncology
Global celebration of 10 years of discovery and lifesaving innovation in immuno-oncology
Emily Whitehead, First Pediatric Patient to Receive CAR T-Cell Therapy, Celebrates Cure 10 Years Later
Ten years ago, Tom and Kari Whitehead came to Children’s Hospital of Philadelphia (CHOP) looking for a miracle. Their 6-year-old daughter, Emily, had relapsed in her battle with acute lymphoblastic leukemia (ALL), after many months of unsuccessful chemotherapy and a disease that had progressed so rapidly that she was ineligible for a bone marrow transplant to treat it. Her family came to CHOP in the hopes that Dr. Stephan Grupp, a pioneer in the field of cellular immunotherapy, could provide the miracle they were looking for.
MD Anderson Research Highlights for May 4, 2022
Featured studies include clinical advances with a new combination therapy targeting angiogenesis in platinum-resistant ovarian cancer and a promising immunotherapy combination for kidney cancer, plus laboratory studies that focus on targeting ferroptosis in specific lung cancers, developing chimeric antigen receptor (CAR) T cell therapies for blastic plasmacytoid dendritic cell neoplasms, and characterizing racial and ethnic disparities in breast cancer early detection.
CHOP Researchers Develop a New Class of CAR-T Cells that Target Previously Untargetable Cancer Drivers
In a breakthrough for the treatment of aggressive solid cancers, researchers at Children’s Hospital of Philadelphia (CHOP) have developed a novel cancer therapy that targets proteins inside cancer cells that are essential for tumor growth and survival but have been historically impossible to reach. Using the power of large data sets and advanced computational approaches, the researchers were able to identify peptides that are presented on the surface of tumor cells and can be targeted with “peptide-centric” chimeric antigen receptors (PC-CARs), a new class of engineered T cells, stimulating an immune response that eradicates tumors.
UCLA researchers awarded $1M from DOD to advance CAR T cell therapy for rare melanomas
Scientists Dr. Cristina Puig-Saus and Dr. Daniel Shin from the UCLA Jonsson Comprehensive Cancer Center have received a $1 million Translational Research Award from the U.S. Department of Defense Melanoma Research Program to help advance the use of chimeric antigen receptor, or CAR, T cell therapy as a treatment for people with acral, mucosal and uveal melanomas.
Less is More for the Next Generation of CAR T Cells
Penn Medicine researchers discovered that less is more when it comes to the length of what is known as the single-chain variable fragment in CAR T cells.
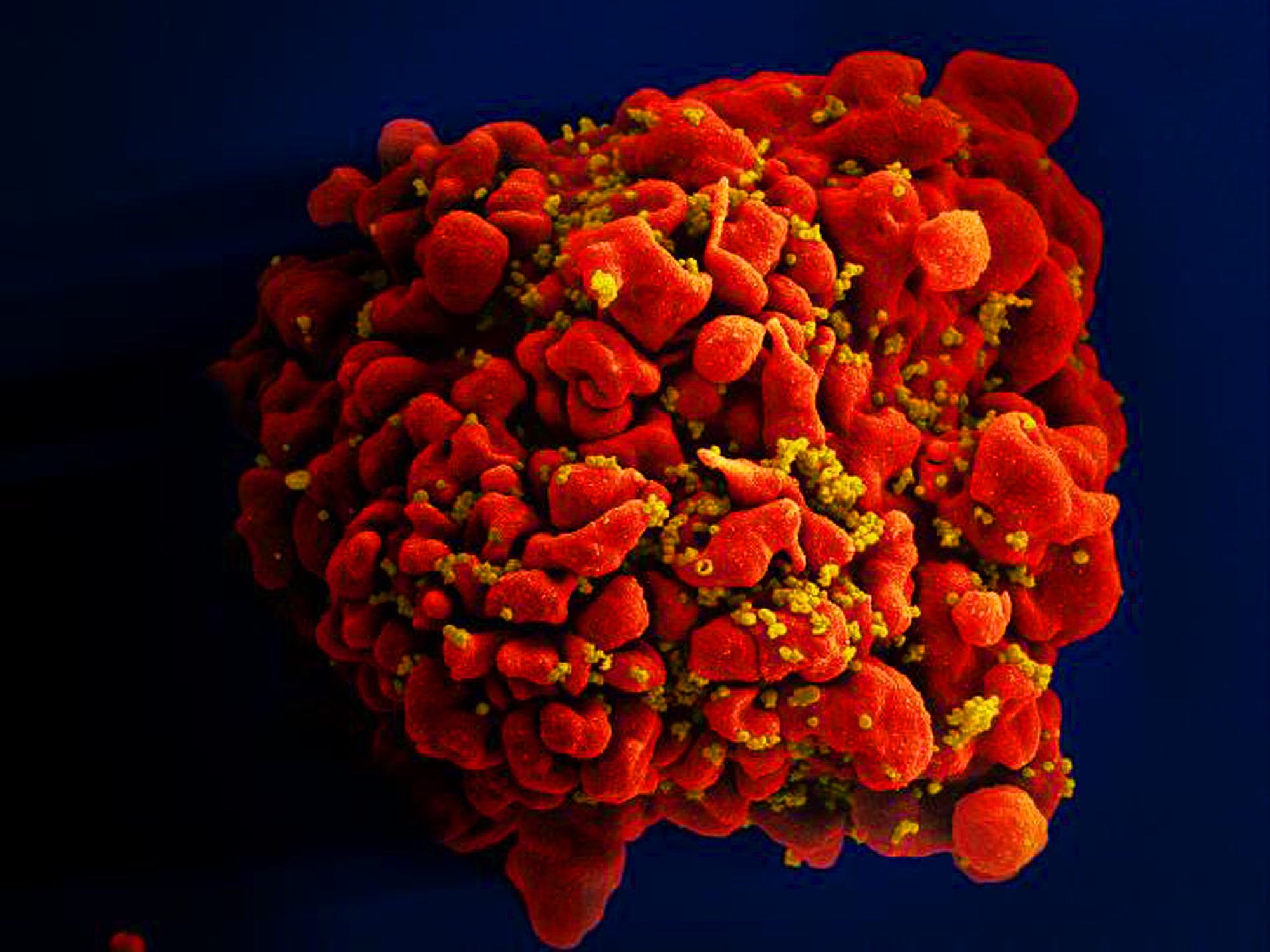
Researchers devise more efficient, enduring CAR gene therapy to combat HIV
A UCLA research team has shown that using a truncated form of the CD4 molecule as part of a gene therapy to combat HIV yielded superior and longer-lasting results in mouse models than previous similar therapies using the CD4 molecule.
Moffitt Researchers Use Mathematical Modeling to Analyze Dynamics of CAR T-Cell Therapy
In an article published in Proceedings of the Royal Society B, Moffitt Cancer Center researchers use mathematical modeling to help explain why CAR T cells work in some patients and not in others.

CAR T-cell therapy generates lasting remissions in patients with multiple myeloma
In a major advance in the treatment of multiple myeloma, a CAR T-cell therapy has generated deep, sustained remissions in patients who had relapsed from several previous therapies, an international clinical trial has found.
Moffitt Researchers Identify Why CAR T Therapy May Fail in Some Lymphoma Patients
In a new study published in Blood, the official journal of the American Society of Hematology, Moffitt researchers show that immune dysregulation can directly affect the efficacy of CAR T therapy in patients with diffuse large B-cell lymphoma.
CRISPR-edited CAR T Cells Enhance Fight Against Blood Cancers
Knocking out a protein known to stifle T cell activation on CAR T cells using the CRISPR/Cas9 technology enhanced the engineered T cells’ ability to eliminate blood cancers.
CAR T cell therapy effective as first-line treatment for high-risk large B-cell lymphoma
A study led by researchers at The University of Texas MD Anderson Cancer Center found that axi-cel, an autologous anti-CD19 chimeric antigen receptor (CAR) T cell therapy, is a safe and effective first-line therapy for patients with high-risk large B-cell lymphoma (LBCL), a group with an urgent need for new and effective treatments.

CAR T-cell therapy found highly effective in patients with high-risk non-Hodgkin lymphoma
A CAR T-cell therapy known as axicabtagene ciloleucel (axi-cel) drove cancer cells to undetectable levels in nearly 80% of patients with advanced non-Hodgkin lymphoma (NHL) in a phase 2 clinical trial, Dana-Farber Cancer Institute investigators report at the virtual 62nd American Society of Hematology (ASH) Annual Meeting.
Dana-Farber to present more than 40 research studies at 2020 ASH Annual Meeting
Dana-Farber Cancer Institute researchers will present more than 40 research studies at the virtual 62nd American Society of Hematology (ASH) Annual Meeting on December 5-8, including two studies that were selected for inclusion in the official press program.
Fred Hutch at ASH: Fauci fireside chat, latest on cell therapies, repairing immune function, COVID and clots — and more
SEATTLE — Nov. 18, 2020 — Fred Hutchinson Cancer Research Center’s latest findings on cell therapies, repairing immune function, and more will be featured at the 62nd American Society of Hematology Annual Meeting & Exposition, to be held virtually Dec. 5 – 8.Dr. Stephanie Lee, ASH president and Fred Hutch physician-scientist will kick off the meeting with a fireside chat with Dr.
MD Anderson and Allogene Therapeutics announce strategic collaboration to accelerate advancement of allogeneic CAR T therapy (AlloCAR T)
MD Anderson and Allogene today announced a strategic five-year collaboration for preclinical and clinical investigation of allogeneic CAR T cell therapies.
Study identifies characteristics of infused CAR T cells associated with efficacy and toxicity in patients with large B-cell lymphoma
Researchers at The University of Texas MD Anderson Cancer Center have identified molecular and cellular characteristics of anti-CD19 CAR T cell infusion products associated with how patients with large B-cell lymphoma (LBCL) respond to treatment and develop side effects.
Dana-Farber to offer first CAR T-cell therapy for mantle cell lymphoma following FDA approval
Today’s Food and Drug Administration (FDA) approval of the first CAR T-cell therapy for mantle cell lymphoma (MCL) represents a key advance for patients with relapsed or treatment-resistant forms of the disease, say Dana-Farber Cancer Institute investigators who helped conduct the decisive clinical trial of the therapy.
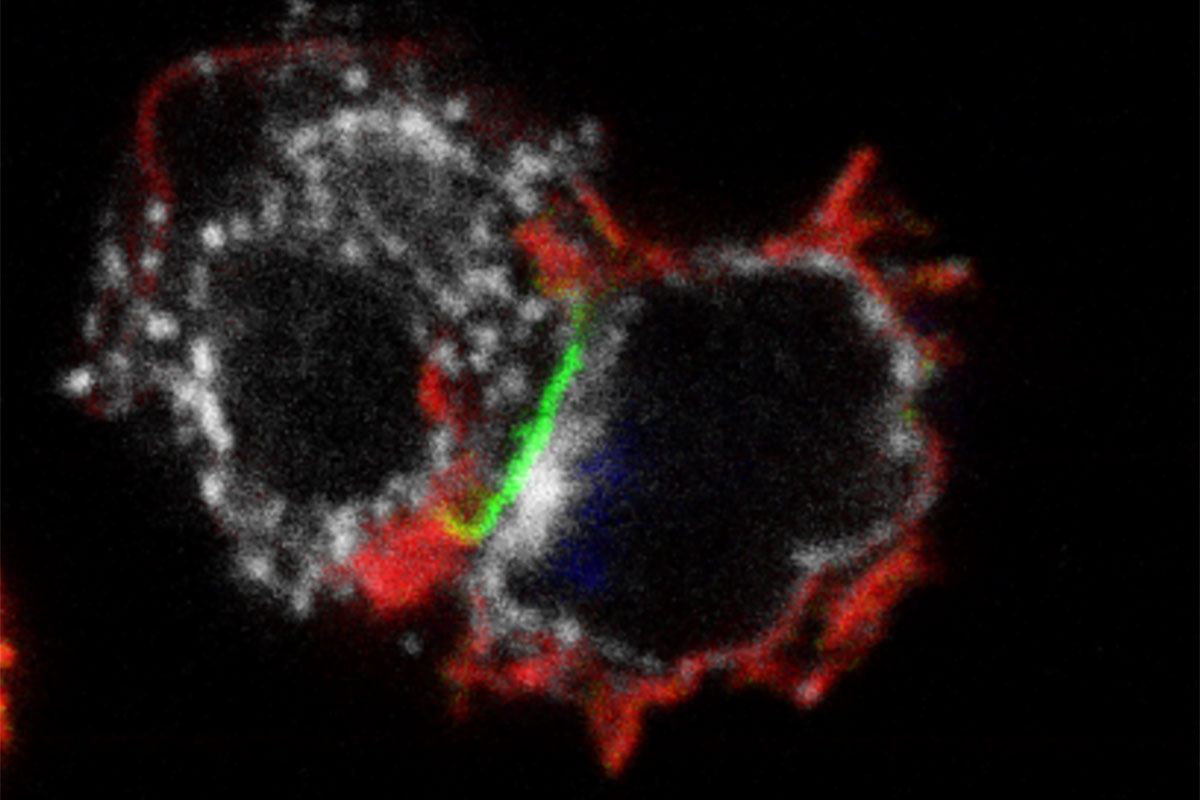
2 immunotherapies merged into single, more effective treatment
Researchers at Washington University School of Medicine in St. Louis have combined two immunotherapy strategies into a single therapy and found, in studies in human cells and in mice, that the two together are more effective than either alone in treating certain blood cancers, such as leukemia.
Moffitt Researchers Identify Factors to Predict Severe Toxicities in CAR T Patients
In a new study published in Clinical Cancer Research, Moffitt Cancer Center researchers identify possible factors that could help physicians know if patients are at higher risk for severe adverse events before they receive CAR T therapy.

NCCN: What People with Cancer and their Caregivers Need to Know about CAR T-Cell Therapy
The National Comprehensive Cancer Network (NCCN) has published a new NCCN Guidelines for Patients: Immunotherapy Side Effects focused on chimeric antigen receptor (CAR) T-cell therapy. This is book two in a series that includes another book on irAEs focused on immune checkpoint inhibitors.
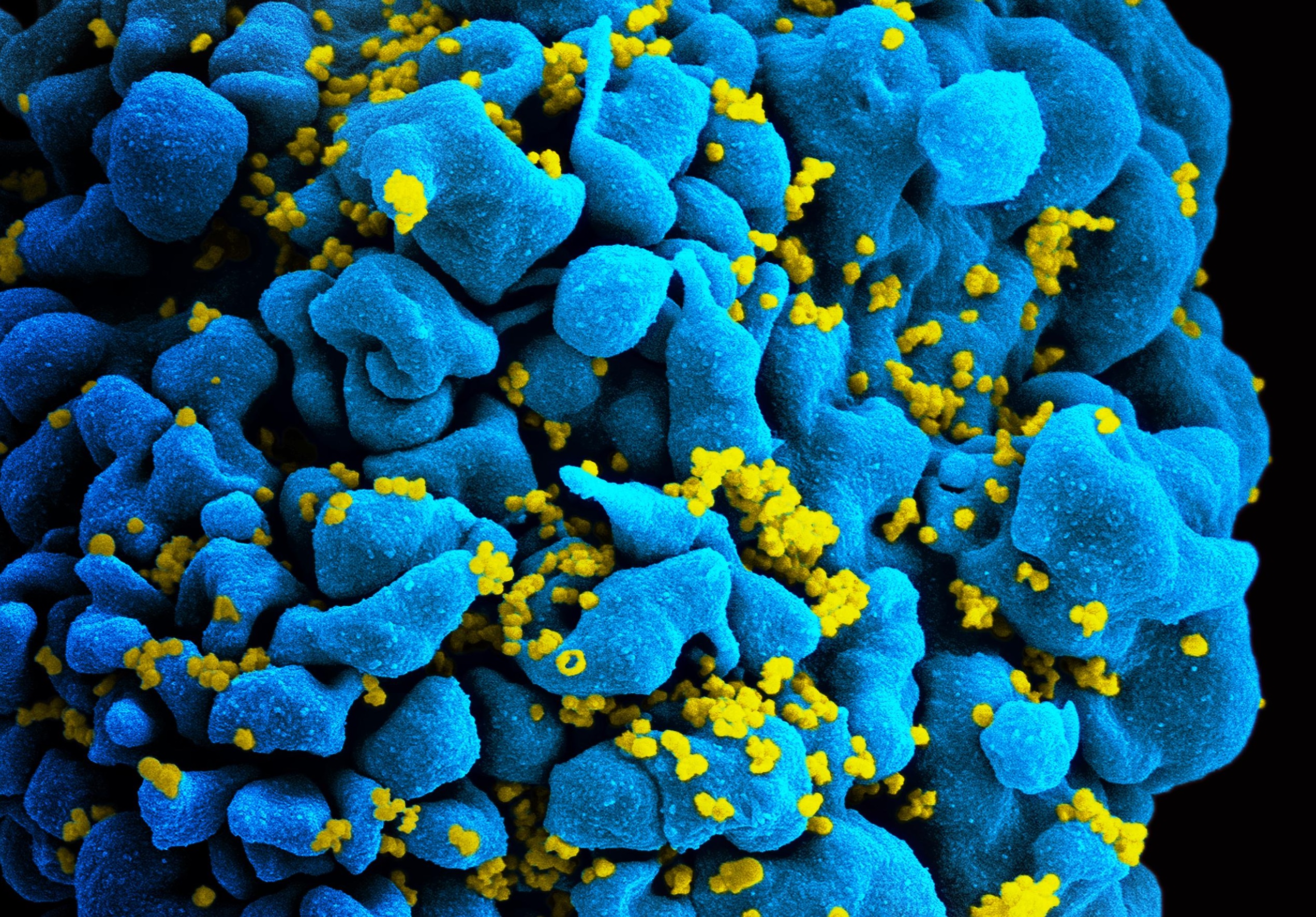
UCLA receives nearly $14 million from NIH to investigate gene therapy to combat HIV
UCLA researchers and colleagues have received a $13.65 million grant from the National Institutes of Health to investigate and further develop an immunotherapy known as CAR T, which uses genetically modified stem cells to target and destroy HIV.

$10 million gift accelerates research to improve cancer therapies, extend benefits to more patients
The David and Etta Jonas Center for Cellular Therapy is being established at the University of Chicago Medicine to accelerate research in hard-to-treat cancers.
Controlling CAR T cells with light selectively destroys skin tumors in mice
UC San Diego bioengineers have developed a control system that could make CAR T-cell therapy safer and more powerful when treating cancer. By programming CAR T cells to switch on when exposed to blue light, the researchers controlled the cells to destroy skin tumors in mice without harming healthy tissue.
Tip Sheet: Mesh loaded with T cells shrinks tumors; second dose of CAR-T cells shows potential; and gene-edited cells stay safe as immunotherapy attacks cancer
Below are summaries of recent Fred Hutch research findings with links for additional background and media contacts.
Fred Hutch at ASH: Latest CAR T data – BCMA, CD19, CD20 – plus new insights on transplantation, gene therapy – and more
The 61st American Society of Hematology Annual Meeting and Exposition will take place Dec. 7–10 in Orlando, Florida

Three UCLA scientists receive grants totaling more than $18 million
Three researchers at the Eli and Edythe Broad Center of Regenerative Medicine and Stem Cell Research at UCLA have received awards totaling more than $18 million from the California Institute for Regenerative Medicine, the state’s stem cell agency.

National Cancer Institute awards UCLA prostate cancer program with Research of Excellence grant
The prostate cancer program at the UCLA Jonsson Comprehensive Cancer Center and UCLA Health has been awarded an $8.7 million Specialized Program of Research Excellence, or SPORE, grant from the National Cancer Institute.