Wren Laboratories announced executive leadership for commercial operations and market expansion. Dr. Abdel Halim is appointed CEO and CSO. Troy Tremaine Appointed to CCO, Dr. Eva Szarek Head of Marketing, and Melissa Ferone director of quality. Expansion includes AI-driven mRNA liquid biopsy genomic assays for biopharma and diagnostics.
Tag: Blood Test
Signs of Multiple Sclerosis Show Up in Blood Years Before Symptoms
In a discovery that could hasten treatment for patients with multiple sclerosis (MS), UC San Francisco scientists have discovered a harbinger in the blood of some people who later went on to develop the disease.
A standard blood test can predict a heart attack
Using the results of a standard blood test and an online tool, you can find out if you are at increased risk of having a heart attack within six months.
A blood test shows MS worsening 1 to 2 years before it happens
Multiple sclerosis patients whose blood tests reveal elevated NfL, a biomarker of nerve damage, could see worsening disability one to two years later, according to a new study spearheaded by researchers at UC San Francisco.
MD Anderson Research Highlights for October 4, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention. These advances are made possible through seamless collaboration between MD Anderson’s world-leading clinicians and scientists, bringing discoveries from the lab to the clinic and back. Recent developments at MD Anderson include a computer game that helps breast cancer survivors improve symptoms of peripheral neuropathy, a publicly available single-cell atlas of CD19 chimeric antigen receptor (CAR) T cells, new targets for TP53-mutant acute myeloid leukemia (AML), a preclinical target for preventing chemobrain, a blood test to help identify patients at higher risk of developing pancreatic cancer, and genomic insights to predict the risk of outcomes in patients with bone cancer.
New blood test for noncoding RNA significantly improves cancer detection
Cancer is most treatable in its early stages, so finding innovative and non-invasive methods to diagnose cancer early on is crucial for fighting the disease.
Early findings suggest clinical and lab-based approach critical to tracking head and neck cancer recurrence
Early findings of two studies from the University of Michigan Rogel Cancer Center shed light on new ways to anticipate recurrence in HPV-positive head and neck cancer sooner.
Studying the Blood Transcriptome May Improve Understanding of Variability in Exercise Response
Article title: Novel whole blood transcriptome signatures of changes in maximal aerobic capacity in response to endurance exercise training in healthy women Authors: Thomas J. LaRocca, Meghan E. Smith, Kaitlin A. Freeberg, Daniel H. Craighead, Timothy Helmuth, Matthew M. Robinson,…

Blood test aids in predicting lung cancer mortality risk
A blood-based four-protein panel (4MP), when combined with a lung cancer risk model (PLCOm2012), can better identify those at high risk of dying from lung cancer than the current U.S. Preventive Services Task Force (USPSTF) criteria.
Could low iron be making your mental health symptoms worse?
A review of the evidence regarding iron deficiency, iron supplementation, and mental health symptoms.
Chula Medicine Reveals Innovative Detection of Latent Dementia A 10-Year Awareness May delay Alzheimer’s Onset in Elderly
Thai Red Cross Emerging Infectious Diseases Health Science Center, Faculty of Medicine, Chulalongkorn University has researched a blood test for markers of Alzheimer’s that can give a 10-year warning, so people can be prepared to slow down the development of dementia in old age.
New blood test can detect ‘toxic’ protein years before Alzheimer’s symptoms emerge, study shows
Researchers can detect small “toxic” aggregates of a particular protein in the blood of individuals with Alzheimer’s disease and in individuals who showed no signs of cognitive impairment at the time the blood sample was taken, but who developed it at a later date.
A blood test could predict survival odds for patients with metastatic cancer
Measuring the amount of DNA that’s been shed by a tumor compared to the body’s typical amount of DNA may be a new tool to predict survival and guide treatment discussions for patients whose cancer has spread from the breast, prostate, lung or colon, a new study finds.
New Data Shows 85% Reduction in One-Year Mortality for Medicare Heart Failure Patients With BVA-Guided Care
New data validate the benefits of the BVA-100 blood volume measurement test for Medicare heart failure patients. Data were presented at the Heart Failure Society of America (HFSA) Annual Scientific Meeting (ASM) 2022 – which brought together the world’s leading experts in heart failure.
A shortage with a silver lining: A chance to reduce unneeded blood tests
A pandemic-related shortage of a mundane item – tubes to collect blood samples from patients — has caused headaches for health systems worldwide. But it may also have a silver lining: A lesson in how to reduce unneeded medical tests, whether or not there’s a shortage, according to a new study.
Grail and Ochsner Health Launch New Initiatives to Improve Cancer Detection Rates in Louisiana
Multi-Cancer Early Detection Health Equity Demonstration Three-Year Program Aims to Improve Cancer Outcomes Among Underserved Populations and Develop Best Practices for Deployment of Innovative Technologies in Community Settings
Higher Antioxidant Levels Linked to Lower Dementia Risk
People with higher levels of antioxidants in their blood may be less likely to develop dementia, according to a study published in the May 4, 2022, online issue of Neurology®, the medical journal of the American Academy of Neurology.
COVID-19 pandemic shifted patient attitudes about colorectal cancer screening
For people hesitant to come into the hospital or an outpatient center to get a colonoscopy, home-administered fecal occult blood tests (FOBT) may provide a useful workaround tool.
NUS researchers develop world’s first blood test for real-time monitoring of cancer treatment success
A team of researchers from the NUS Department of Biomedical Engineering and Institute for Health Innovation & Technology has developed a novel blood test called ExoSCOPE that could tell doctors whether cancer treatment is working for a patient, within 24 hours after the treatment. This will enable doctors to customise the treatment plan to improve patients’ chances of recovery.
Immunomics: A Conversation on the Future of Diagnostics with Ramy Arnaout
In a recent perspective article, pathologists outline how the immunome — all of the genes collectively expressed by an individual’s immune cells — holds the potential to provide researchers and physicians with unprecedented insight into an individual’s health. Collecting that information from large numbers of patients could one day facilitate diagnostics via a near-universal blood test and pave the way to targeted therapies for a wide variety of conditions.
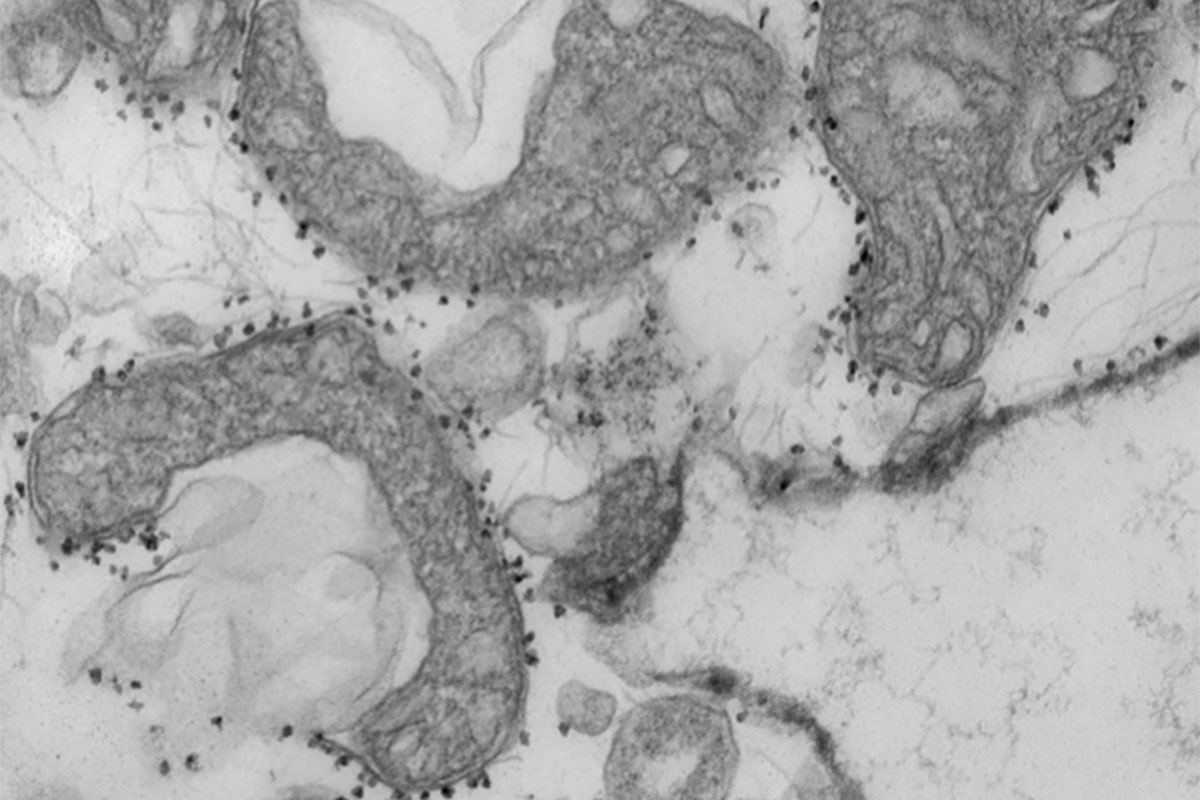
Rapid blood test identifies COVID-19 patients at high risk of severe disease
Scientists at Washington University School of Medicine in St. Louis have shown that a relatively simple and rapid blood test can predict which patients with COVID-19 are at highest risk of severe complications or death. The blood test measures levels of mitochondrial DNA, which normally resides inside the energy factories of cells. Mitochondrial DNA spilling out of cells and into the bloodstream is a sign that a particular type of violent cell death is taking place in the body.
New experimental blood test determines which pancreatic cancers will respond to treatment
GRAND RAPIDS, Mich. (Oct. 22, 2020) — Scientists have developed a simple, experimental blood test that distinguishes pancreatic cancers that respond to treatment from those that do not. This critical distinction could one day guide therapeutic decisions and spare patients with resistant cancers from undergoing unnecessary treatments with challenging side effects.
Non-Fasting Blood Test Can Help Screen Youth for Prediabetes and Diabetes
A simple blood test that does not require overnight fasting has been found to be an accurate screening tool for identifying youth at risk for type 2 diabetes and heart disease risk later in life.
Cleveland Clinic Joins Study to Evaluate Blood Test Designed to Detect More Than 50 Cancers with Single Blood Draw
Cleveland Clinic has joined the PATHFINDER Study, a prospective, multi-center clinical trial that is evaluating the clinical use of an investigational blood test that has the ability to detect more than 50 cancers across stages I-IV with a single blood…

A blood test could predict who benefits from immunotherapy
A test which detects changing levels of tumour fragments in the blood may be an easy, non-invasive and quick way to predict who will benefit from immunotherapy, a treatment option for advanced cancers.

Researchers make significant step toward blood test for Alzheimer’s disease
Researchers at Washington University School of Medicine in St. Louis have developed a technique to detect minute amounts of a protein fragment linked to Alzheimer’s disease in the blood. The study, which will be published July 28 in the Journal of Experimental Medicine (JEM), shows that levels of p-tau-217 are elevated during the early stages of Alzheimer’s disease and could lead to a simple blood test capable of diagnosing the neurodegenerative disorder years before any symptoms begin to appear.
Mount Sinai Developing an “End-to-End” Diagnostics Solution for COVID-19 That Incorporates Diagnosis, Treatment Selection, and Monitoring of Disease Course
An expert team of researchers and clinicians have been working together to design, validate, and implement an “end-to-end” clinical pathology laboratory solution that will allow for the testing of approximately several hundred people per day in order to rapidly diagnose and help guide the selection of treatment and monitor disease course.
Carrots plus sticks: Study looks at what works to reduce low-value care
The old story of a farmer trying to get a stubborn mule to pull a wagon by dangling a carrot in front of its nose, or hitting its rump with a stick, may not seem to have much to do with the practice of medicine. But a new study suggests that when it comes to making the best use of health care dollars, it will take a combination of carrots and sticks to move things forward.
Blood test identifies risk of disease linked to stroke and dementia
A UCLA-led study has found that levels of six proteins in the blood can be used to gauge a person’s risk for cerebral small vessel disease, or CSVD, a brain disease that affects an estimated 11 million older adults in the U.S.

New blood test capable of detecting multiple types of cancer
A new blood test in development has shown ability to screen for numerous types of cancer with a high degree of accuracy, a trial of the test shows.
Blood Test Predicts Stroke Risk in Patients with Diabetes
ANN ARBOR, Mich. – Having diabetes is a risk factor for many other health conditions, including stroke. “Every 40 seconds an American has a stroke,” says Frederick Korley, M.D., Ph.D., an assistant professor of emergency medicine at Michigan Medicine. “To be…