Monitoring daily activity patterns using a wrist-worn device may detect early warning signs of Alzheimer’s disease, according to a new study led by researchers at the Johns Hopkins Bloomberg School of Public Health.
Tag: Amyloid Beta
New blood test can detect ‘toxic’ protein years before Alzheimer’s symptoms emerge, study shows
Researchers can detect small “toxic” aggregates of a particular protein in the blood of individuals with Alzheimer’s disease and in individuals who showed no signs of cognitive impairment at the time the blood sample was taken, but who developed it at a later date.
Whole blood exchange could offer disease-modifying therapy for Alzheimer’s disease, study finds
A novel, disease-modifying therapy for Alzheimer’s disease may involve the whole exchange of blood, which effectively decreased the formation of amyloid plaque in the brains of mice, according to a new study from UTHealth Houston.
Research News Tip Sheet: Story Ideas from Johns Hopkins Medicine
NEWS STORIES IN THIS ISSUE:
– Study Says Failure to Rid Amyloid Beta Protein from Brain May Lead to Alzheimer’s Disease
– Johns Hopkins Medicine Team Discovers Novel Mediator of Once Mysterious Chronic Itch – Study Suggests Molecular Changes in Tissue Microenvironment May Promote Colorectal Cancer
– Researchers ID Anti-Inflammatory Proteins as Therapy Targets for Nasal and Sinus Problem
– Johns Hopkins Children’s Center Receives NIH Award to Study Dangerous Pediatric Disease

Protein That Can Be Toxic in The Heart And Nerves May Help Prevent Alzheimer’s
A protein that wreaks havoc in the nerves and heart when it clumps together can prevent the formation of toxic protein clumps associated with Alzheimer’s disease, a new study led by a UT Southwestern researcher shows. The findings, published recently in the Journal of Biological Chemistry, could lead to new treatments for this brain-ravaging condition, which currently has no truly effective therapies and no cure.
Alzheimer’s Association should reveal financial conflict of interest in urging FDA to approve Biogen drug, says Dr. Leslie Norins, CEO of Alzheimer’s Germ Quest
Biogen tried, and failed, to win FDA committee approval for its anti-amyloid Alzheimer’s drug. The Alzheimer’s Association supported the application but did not reveal significant monies received from the firm.
Protein Shapes Matter in Alzheimer’s Research
Even small changes may have big, long-term consequences. For amyloid beta peptides, a major hallmark of Alzheimer’s disease, a common chemical modification at a particular location on the molecule has a butterfly effect that leads to protein misfolding, aggregation and cellular toxicity.
Flickering Light Mobilizes Brain Chemistry That May Fight Alzheimer’s
The promise of flickering light to treat Alzheimer’s takes another step forward in this new study, which reveals stark biochemical mechanisms: The 40 Hertz stimulation triggers a marked release of signaling chemicals.

Pathogenic Alzheimer’s disease cascade is activated by faulty norepinephrine signaling
Preclinical research has revealed a key missing piece of the Alzheimer’s disease puzzle. That allowed proof-of-concept experiments — using an existing drug — that dramatically reduced Alzheimer’s pathology and symptoms in mouse models, potentially offering an immediate treatment for this disease.
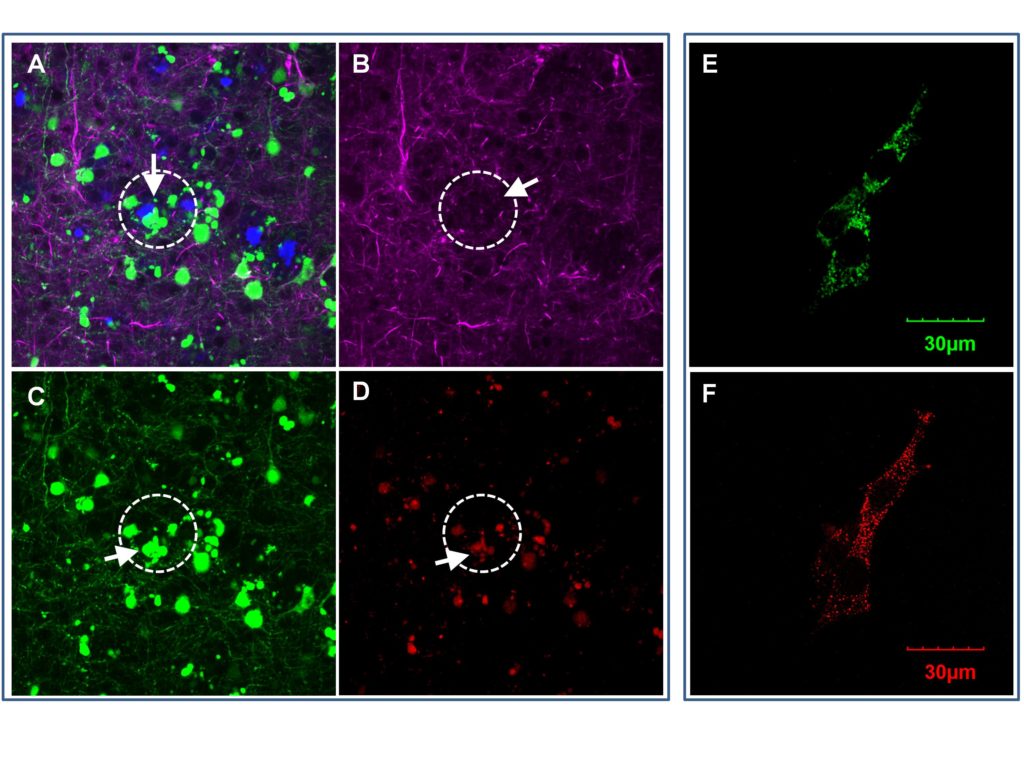
Scientists identify protein associated with ovarian cancer that exacerbates neurodegeneration in Alzheimer’s
Houston Methodist scientists identified a protein found in ovarian cancer that may contribute to declining brain function and Alzheimer’s disease, by combining computational methods and lab research.
Brain Guard
Israeli researchers have developed new technology for transporting drugs within silicon nanostructures to the brain. These nanostructures release an essential protein, which can inhibit the development of Alzheimer’s disease, and provide targeted delivery in the brain with the use of a “gene gun.”

Alzheimer’s missing link ID’d, answering what tips brain’s decline
Brain’s immune cells form nexus between two damaging Alzheimer’s proteins Years before symptoms of Alzheimer’s disease appear, two kinds of damaging proteins silently collect in the brain: amyloid beta and tau. Clumps of amyloid accumulate first, but tau is particularly…