Children’s Hospital Los Angeles has received a multi-year $6 million award from the California Institute for Regenerative Medicine (CIRM) to develop innovative stem cell approaches to treat children and adolescents with recurrent solid tumors. The Cancer and Blood Disease Institute (CBDI) is a recognized leader in pediatric cancer care and research.
Tag: CAR T-cell therapy
A Leading-Edge Lymphoma Program
Less than three years after joining the Cedars-Sinai Cancer faculty, hematologist-oncologists Justin Darrah, MD, and Akil Merchant, MD, are pioneering new research and bringing a new, comprehensive set of treatment options to patients in the recently established Lymphoma Program.
NCCN Annual Congress on Hematologic Malignancies™ Returns to In-Person October 14–15, 2022 in New York City
The 2022 NCCN Annual Congress on Hematologic Malignancies™ (#NCCNhem22) is taking place Friday, October 14–Saturday, October 15, 2022 in New York City. All live sessions will also stream remotely through a virtual event platform.
Emily Whitehead, First Pediatric Patient to Receive CAR T-Cell Therapy, Celebrates Cure 10 Years Later
Ten years ago, Tom and Kari Whitehead came to Children’s Hospital of Philadelphia (CHOP) looking for a miracle. Their 6-year-old daughter, Emily, had relapsed in her battle with acute lymphoblastic leukemia (ALL), after many months of unsuccessful chemotherapy and a disease that had progressed so rapidly that she was ineligible for a bone marrow transplant to treat it. Her family came to CHOP in the hopes that Dr. Stephan Grupp, a pioneer in the field of cellular immunotherapy, could provide the miracle they were looking for.
Ultrasound remotely triggers immune cells to attack tumors in mice without toxic side effects
A new cancer immunotherapy pairs ultrasound with specially engineered CAR T cells to destroy malignant tumors while sparing normal tissue. The new experimental therapy significantly slowed down the growth of solid cancerous tumors in mice.
John Theurer Cancer Center Investigators Participated in ZUMA-7 Study Showing Value of CAR T-Cell Therapy as Second-Line Treatment for Relapsed Large B-Cell Lymphoma
new study has found that using CAR T-cell therapy as the second line of treatment for diffusing large B-cell lymphoma (DLBCL) that has returned or continued to grow after initial treatment was more effective than the standard second-line regimen of care for improving event-free survival (EFS / defined as disease progression, needing to start a new lymphoma treatment, or death from any cause). Investigators from Hackensack Meridian/Hackensack University Medical Center’s John Theurer Cancer Center (JTCC), a part of Georgetown Lombardi Comprehensive Cancer Center, participated in the multicenter international study, called ZUMA-7.

CAR T-cell therapy generates lasting remissions in patients with multiple myeloma
In a major advance in the treatment of multiple myeloma, a CAR T-cell therapy has generated deep, sustained remissions in patients who had relapsed from several previous therapies, an international clinical trial has found.
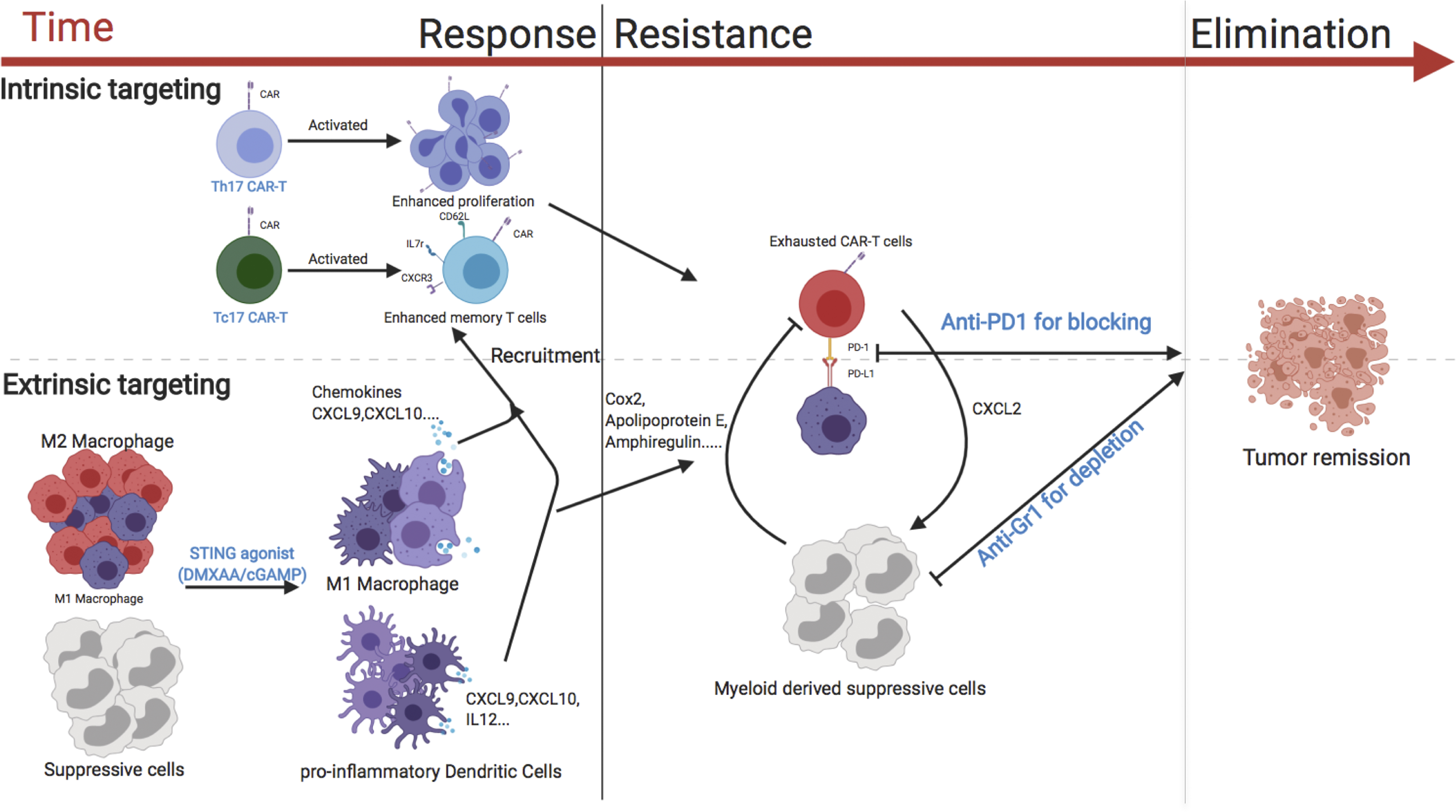
Combined approach could boost breast cancer immunotherapy, study suggests
Activating an immune signaling pathway best known for fighting viral and bacterial infections can boost the ability of genetically engineered T cells to eradicate breast cancer in mice, according to a new study by researchers at the University of North Carolina. The study, to be published December 31 in the Journal of Experimental Medicine (JEM), suggests that CAR T cells, which are already used to treat certain blood cancers in humans, may also be successful against solid tumors if combined with other immunotherapeutic approaches.

NCCN: What People with Cancer and their Caregivers Need to Know about CAR T-Cell Therapy
The National Comprehensive Cancer Network (NCCN) has published a new NCCN Guidelines for Patients: Immunotherapy Side Effects focused on chimeric antigen receptor (CAR) T-cell therapy. This is book two in a series that includes another book on irAEs focused on immune checkpoint inhibitors.
Moffitt Cancer Center Study Suggests More Could Benefit from CAR T-Cell Therapy
Moffitt Cancer Center organized a consortium of 16 cancer treatment facilities across the U.S. that offer Yescarta as a standard-of-care therapy for patients with relapsed/refractory large B cell lymphoma. They wanted to determine if the safety and effectiveness seen in the ZUMA-1 clinical trial were similar for patients treated with the now commercially available CAR T therapy. Their findings were published in the Journal of Clinical Oncology.
Drug-light combo could offer control over CAR T-cell therapy
UC San Diego bioengineers are a step closer to making CAR T-cell therapy safer, more precise and easy to control. They developed a system that allows them to select where and when CAR T cells get turned on so that they destroy cancer cells without harming normal cells. The system requires two “keys”—the drug Tamoxifen and blue light—to activate CAR T cells to bind to their targets. Just one key keeps the cells inactive.