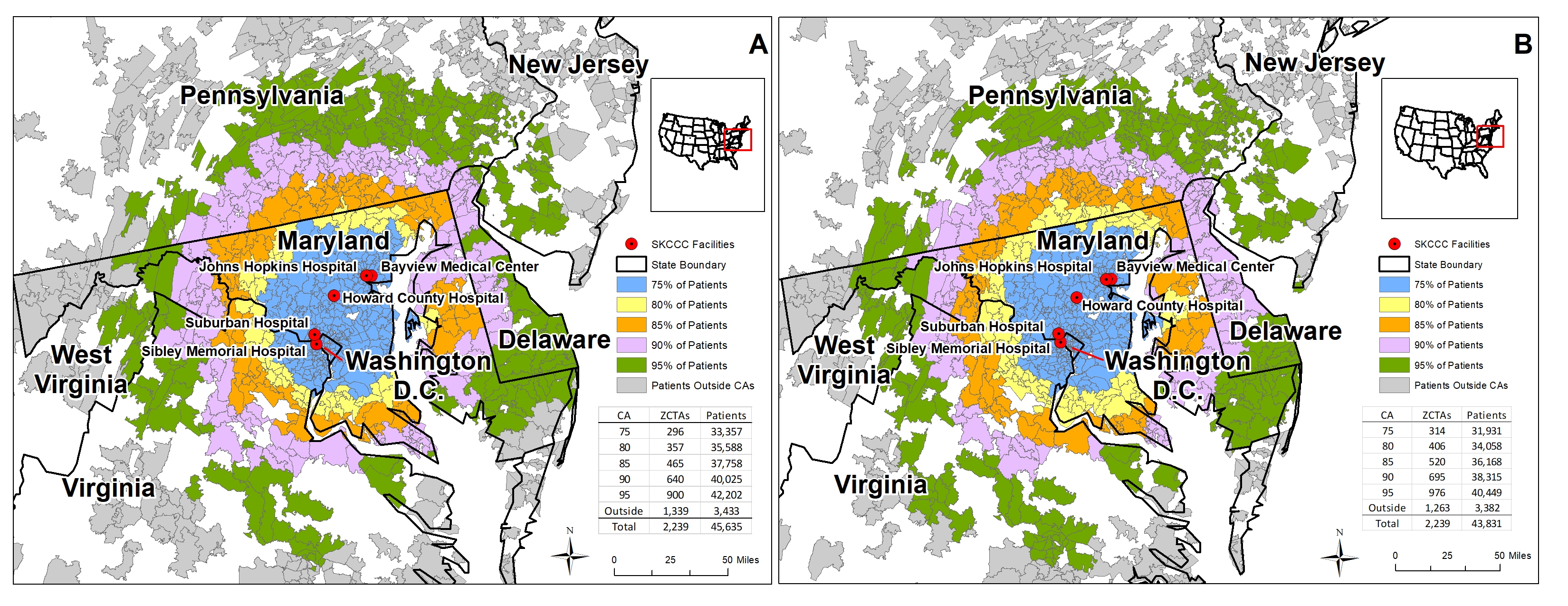
Location, race and insurance status play a significant part in the odds of a patient being diagnosed with early-stage or late-stage cancer, according to a detailed medical records analysis of more than 94,000 patients with cancer by researchers at the Johns Hopkins Bloomberg School of Public Health and the Johns Hopkins Kimmel Cancer Center.