Thomas M. Priselac, whose leadership over the last 30 years as Cedars-Sinai’s president and CEO significantly expanded the scope and quality of its clinical, educational, research and community benefit programs, has announced his plans to retire.

news, journals and articles from all over the world.

Thomas M. Priselac, whose leadership over the last 30 years as Cedars-Sinai’s president and CEO significantly expanded the scope and quality of its clinical, educational, research and community benefit programs, has announced his plans to retire.
The three-year, $1.3 million grant from the Administration for Community Living’s Alzheimer’s Disease Program Initiative will support a groundbreaking project designed to advance health equity and improve quality of life for individuals living with or at high risk for Alzheimer’s disease and related dementias and their family caregivers.
The University of Pennsylvania School of Nursing (Penn Nursing) has named its second cohort of Fellows for the Leonard A. Lauder Community Care Nurse Practitioner Program (LLCCNPP).

The study finds utilization of annual screening mammograms suboptimal among low-income Black women with several reported perceived and actual barriers. Most had a low breast cancer risk perception. Interestingly, participants perceived mammograms as very beneficial: 80 percent believed that ‘if breast cancer is found early, it’s likely that the cancer can be successfully treated;’ 90 percent indicated that ‘having a mammogram could help find breast cancer when it is first getting started.’
New UCLA-led research suggests that patient mortality rates, readmissions, length of stay, and health care spending were virtually identical for elderly hospitalized patients who were treated by physicians with Doctor of Medicine (MD) or Doctor of Osteopathic Medicine (DO) degrees.
After hundreds of thousands of miles and 20 years of service, UTHealth Houston School of Dentistry has a new set of wheels for its Mobile Dental Van program to continue providing care to underserved communities.

FAU researchers from the Christine E. Lynn College of Nursing have received a four year, $3.9 million grant from the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services for a nurse-led mobile health unit to create healthier populations in rural and medically underserved regions.
Yvette Calderon, MD, MS, Chair of Emergency Medicine at Mount Sinai Beth Israel and Professor of Emergency Medicine at the Icahn School of Medicine at Mount Sinai, has been elected to the National Academy of Medicine (NAM). Election to the NAM is considered one of the highest honors in health and medicine, recognizing individuals who have demonstrated outstanding professional achievement and commitment to service. With her election, Mount Sinai has 26 faculty members in the NAM.
Researchers evaluated a remotely supervised online chair yoga intervention targeted at older adults with dementia and measured clinical outcomes virtually via Zoom under the remote guidance. Results showed that remotely supervised online chair yoga is a feasible approach for managing physical and psychological symptoms in socially isolated older adults with dementia based on retention (70 percent) and adherence (87.5 percent), with no injury or other adverse events.

Kimberly Strauch, PhD, MSN, ANP-BC, has been appointed the inaugural Executive Director of Leonard A. Lauder Community Care Nurse Practitioner Program (LLCCNPP) at Penn Nursing. This program was announced in February 2022 as a first-of-its-kind, tuition-free program dedicated to building a nurse practitioner workforce committed to working in and with underserved communities, both rural and urban. LLCCNPP was borne of a $125 million gift—the largest ever to an American nursing school—by Penn alumnus Leonard A. Lauder, Chairman Emeritus of The Estee Lauder Companies.
A unique Mount Sinai study focused on a multi-ethnic, underserved community in New York City shows that young Black adults are twice as likely to have atherosclerosis as similarly situated young Hispanic adults.
Dr. Ortega’s newest role as associate dean of clinical practice now places her at the helm of clinical care for both the Green Memory and Wellness Center and the FAU and Northwest Community Health Alliance’s Community Health Center (FAU/NCHA CHC), operated by the Christine E. Lynn College of Nursing. She will collaborate with FAU/NCHA CHC executive director Karethy Edwards, Dr.PH, APRN, professor and associate dean for academic programs; and clinical director Desiree’ T. Weems, APRN, a certified nurse practitioner.
Washington University School of Medicine in St. Louis has received a $17 million grant from the National Institutes of Health (NIH) to address disparities in cancer research, treatment and outcomes in underrepresented populations. The research, funded through the National Cancer Institute’s Cancer Moonshot program, will focus on African American patients with colorectal cancer and multiple myeloma, as well as patients of any race or ethnicity with cholangiocarcinoma, a rare cancer of the bile ducts.
Florida Atlantic University and Northwest Community Health Alliance’s Community Health Center, operated by FAU’s Christine E. Lynn College of Nursing, together with the West Palm Beach YWCA, recently received the “2021 Community Collaborators Award” from Nonprofits First, Inc., for their untiring efforts to mitigate health care disparities among women from minority groups with limited access to quality care.
The RCHN Community Health Foundation has awarded $7 million to the Geiger Gibson Program in Community Health at the George Washington University Milken Institute School of Public Health, the nation’s leading academic program focusing on community health centers and the communities and populations they serve.
The FAU/NCHA Community Health Center is the first university in Florida to be designated by the U.S. Health Resources and Services Administration (HRSA), as a “Federally Qualified Health Center (FQHC) Look-Alike. To receive this designation, organizations must operate and provide services consistent with HRSA’s Health Center Program requirements to ensure health care for underserved communities and vulnerable populations in the U.S. through service provision to all, regardless of ability to pay.
How Can Scientists Predict a COVID-19 Outbreak? There’s an App for that; Johns Hopkins Medicine Collaborates with the City and Faith Organizations to Offer Guidance on Safely Reopening Houses of Worship; Johns Hopkins Hospital Patient ‘Grateful to Still Be Alive’ After Two-Month Hospitalization with COVID-19; “12 Things You Need To Know” Infographic…

The last year, which has been unlike any other in Rutgers’ 254-year history, has centered on keeping the Rutgers community safe, providing top-notch health care, developing the first saliva test for the coronavirus and helping society cope with the biggest global public health crisis since the 1918 influenza pandemic.
Richard Marlink, the director of Rutgers Global Health Institute who has worked extensively to confront issues of health equity both in the U.S. and around the world, discusses the complex obstacles facing low-income and minority communities during the pandemic and why it is important to help everyone recover.
A collaboration between eCornell and the nonprofit National Education Equity Lab is giving high school students in underserved communities the opportunity to develop skills in business analytics while gaining the confidence to recognize they can excel in college.
Nature is a tool to address deeply entrenched health disparities; health systems should work to increase nature access, as they have with other social determinants of health
A new artificial intelligence (AI) algorithm developed by researchers at New York Eye and Ear Infirmary of Mount Sinai (NYEE) can rapidly and accurately detect age-related macular degeneration (AMD), a leading cause of vision loss in the United States.
Study Shows Vascular Ultrasounds and Adhering to Interventional Education in Underserved Communities can Improve Health among Parents and School Staff
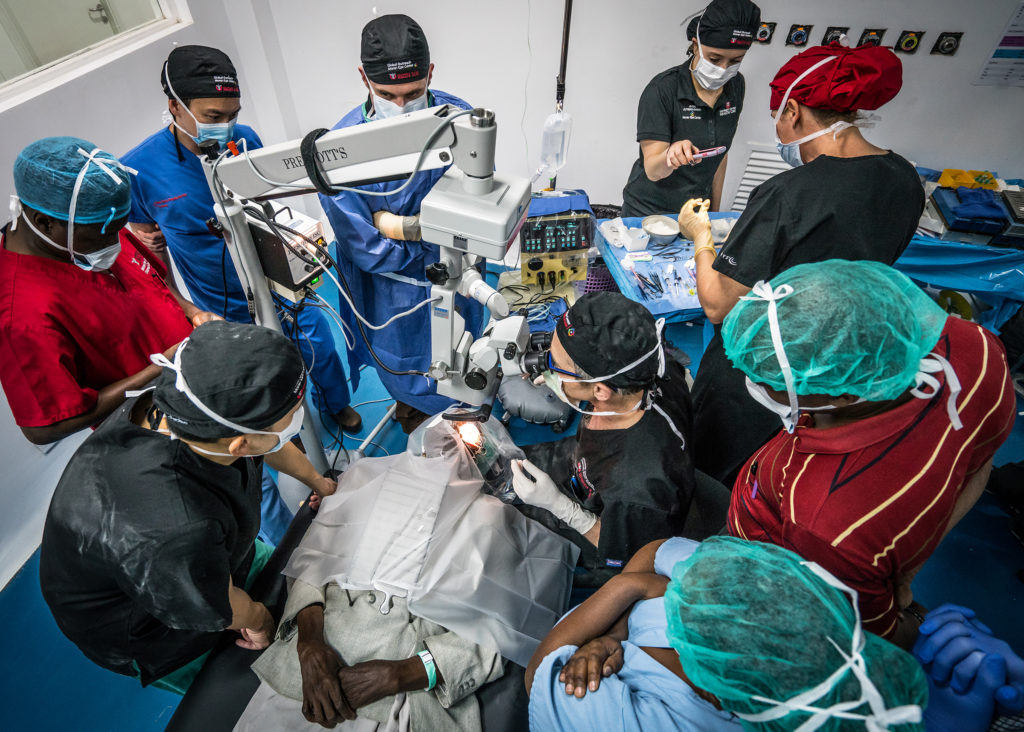
Staggering new statistics released by the World Health Organization (WHO) in its first World Report on Vision estimate more than 1 billion people are visually impaired because they don’t get the care they need—a finding that brings renewed urgency for sustainable global outreach efforts. The statistics underscore the need for programs like the donor-funded John A. Moran Eye Center Global Outreach Division at the University of Utah, which works to create sustainable eye care systems in developing nations and to reach underserved populations in Utah.