Forty eighth grade students — many originally from Mexico, Colombia, Venezuela and elsewhere — learned firsthand how scientists of Hispanic/Latino heritage contribute to science during the 18th annual Hispanic/Latino Education Outreach Day at Argonne.
Tag: personal protective equipment
Pilot study finds computer vision technology effective at determining proper mask wearing in a hospital setting
In early 2020, before COVID-19 vaccines and effective treatments were widely available, universal mask wearing was a central strategy for preventing the transmission of COVID-19. But hospitals and other settings with mask mandates faced a challenge.
New study proves correct dosage for ultraviolet disinfection against COVID
A new study from Binghamton University, State University of New York proves the correct dosage for ultraviolet disinfection against COVID.
University of Kentucky Students Creating Safer PPE for Frontline Workers
University of Kentucky students in the Textile Testing Laboratory are helping develop durable, reusable personal protective equipment (PPE) for health care workers.
Genome sequencing reveals widespread COVID-19 infection in white-tailed deer
Houston Methodist’s SARS-CoV-2 genome sequencing team has partnered on a study led by Penn State that revealed 80% of white-tailed deer sampled across Iowa at the height of the 2020-2021 deer-hunting season tested positive for the SARS-CoV-2 virus. Analysis of the virus genome sequences revealed infections were likely the result of multiple human-to-deer transmission “spillover” events followed by deer-to-deer transmission from April 2020 through January 2021.
During COVID-19, nurses face significant burnout risks, reports American Journal of Nursing
Early in the COVID-19 pandemic, more than 40 percent of nurses and other health care workers had risks associated with an increased likelihood of burnout, reports a survey study in the August issue of the American Journal of Nursing (AJN). The journal is published in the Lippincott portfolio by Wolters Kluwer.
Research Update: Cleaning & Disinfecting PPE for Reuse
The COVID-19 pandemic has caused an unprecedented disruption in supply chains across multiple sectors including the shortage of critical personal protective equipment (PPE). In addition to hand washing and social distancing, various PPE items are used to prevent contact with…

Rutgers University’s Resilient, Innovative Year Confronting COVID-19
The last year, which has been unlike any other in Rutgers’ 254-year history, has centered on keeping the Rutgers community safe, providing top-notch health care, developing the first saliva test for the coronavirus and helping society cope with the biggest global public health crisis since the 1918 influenza pandemic.
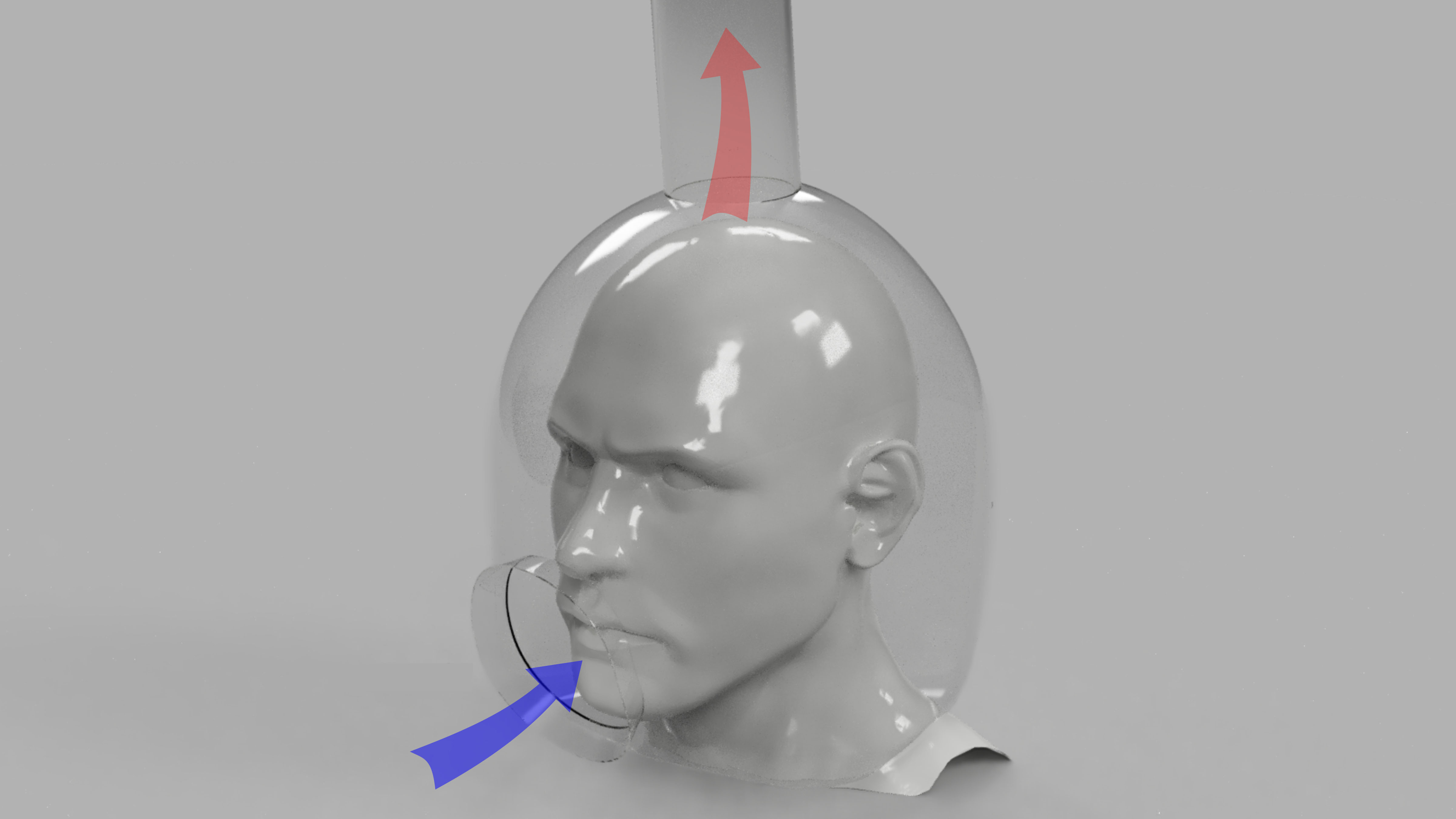
Disposable Helmet Retains Cough Droplets, Minimizes Transmission to Dentists, Otolaryngologists
Dentists and otolaryngologists are at particular risk of infection of COVID-19, since they need direct access to the mouth, nose, and throat of patients. The current solutions are expensive, not highly effective, and not very accessible. In Physics of Fluids, researchers discuss their design of an open-faced helmet for patient use that is connected to a medical-grade air filtration pump from the top that creates a reverse flow of air to prevent cough droplets from exiting the helmet.
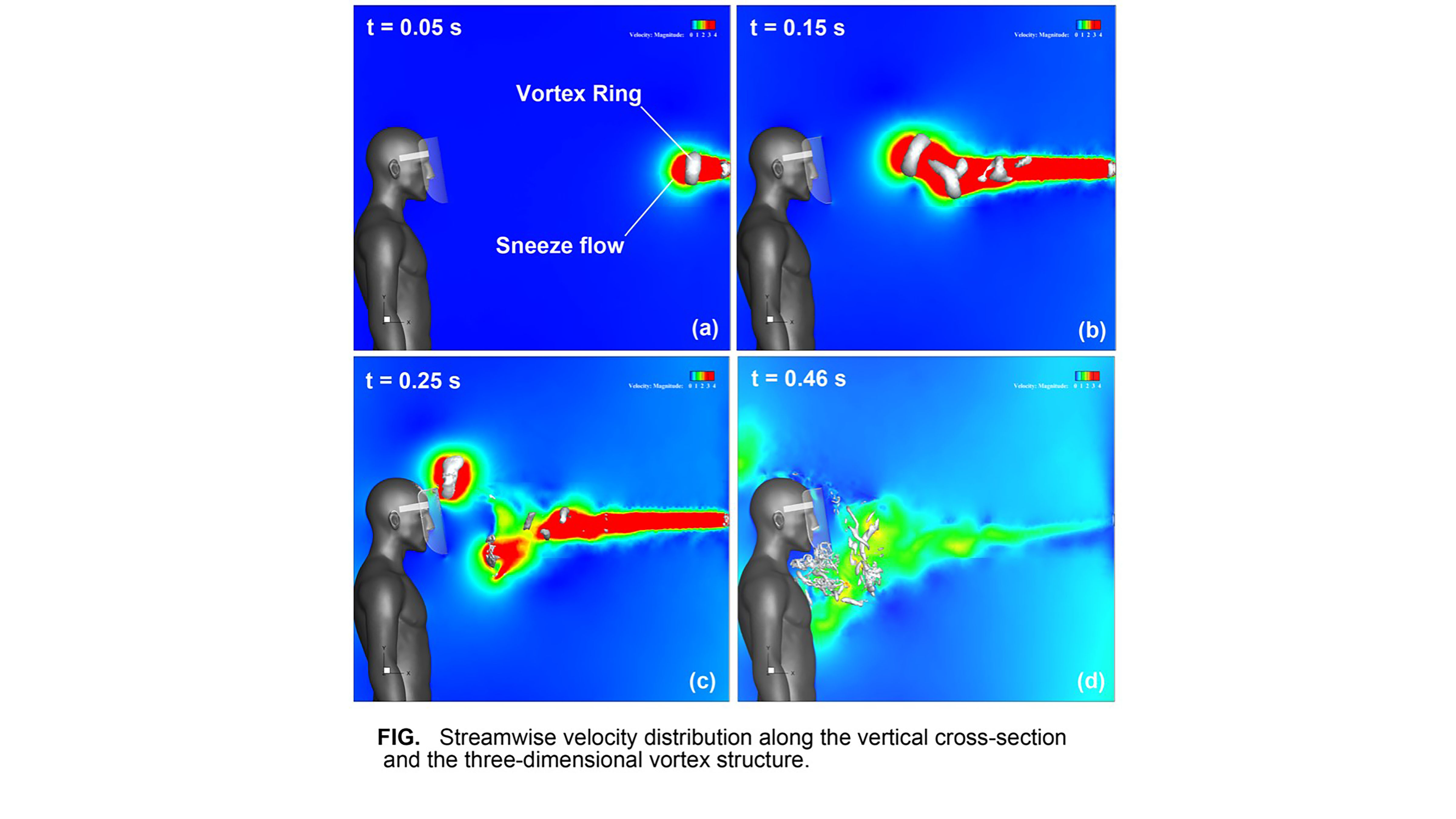
Face Shields No Match for Sneeze Vortex Rings
Do face shields provide enough protection to the wearers against COVID-19 if they don’t also wear a mask? No. But researchers in Japan are working to create face shields safe enough to be worn alone. In Physics of Fluids, Fujio Akagi and colleagues describe their work to gain a better understanding of what happens to the airflow around a face shield when someone nearby sneezes.

Seeking the Most Effective Polymers for Personal Protective Equipment
Personal protective equipment, like face masks and gowns, is generally made of polymers. But not much attention is typically given to the selection of polymers used beyond their physical properties. To help with the identification of materials that will bind to a virus and speed its inactivation for use in PPE, researchers have developed a high-throughput approach for analyzing the interactions between materials and viruslike particles. They report their method in the journal Biointerphases.
The Strategic Stockpile Failed; Experts Propose New Approach to Emergency Preparedness
A panel of academic and military experts is calling for a more dynamic, flexible approach to emergency preparedness at the national level.

Plant-Based Spray Could be Used in N95 Masks and Energy Devices
Engineers have invented a way to spray extremely thin wires made of a plant-based material that could be used in N95 mask filters, devices that harvest energy for electricity, and potentially the creation of human organs. The method involves spraying methylcellulose, a renewable plastic material derived from plant cellulose, on 3D-printed and other objects ranging from electronics to plants, according to a Rutgers-led study in the journal Materials Horizons.

American Academy of Dermatology honors Detroit physician Iltefat H. Hamzavi with national “Patient Care Hero” award
The American Academy of Dermatology has named board-certified dermatologist Iltefat H. Hamzavi, MD, FAAD, a Patient Care Hero for his innovative use of light therapy to sanitize masks needed by frontline health care workers.
FDA Guidance Fails to Ensure Security of 3D-Printed Masks and PPE
New Brunswick, N.J. (Sept. 16, 2020) – FDA guidelines for making 3D-printed masks, face shields and other personal protective equipment (PPE) in the COVID-19 era fail to defend against cyberattacks, according to Rutgers and Georgia Tech engineers. Due to the…
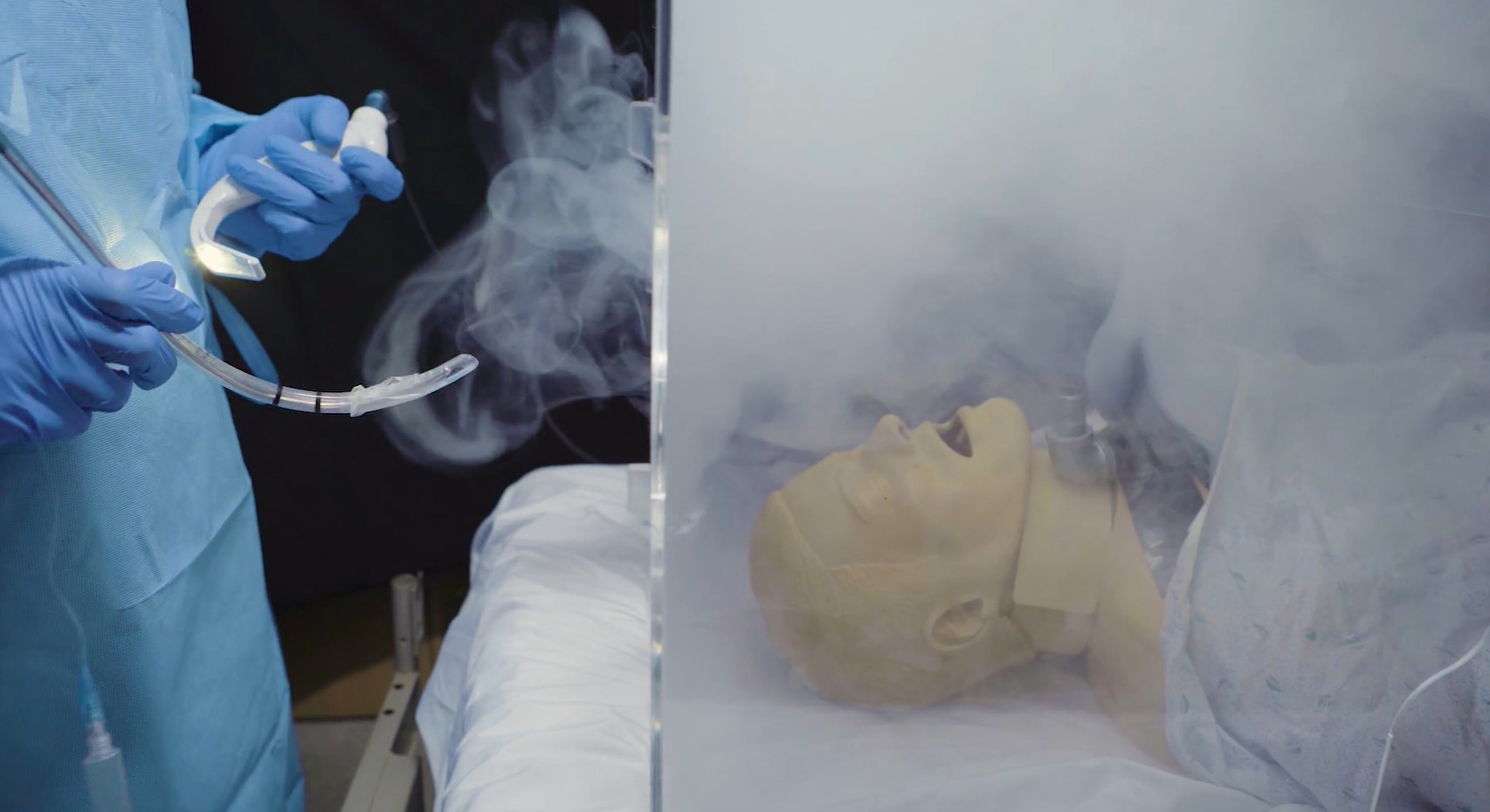
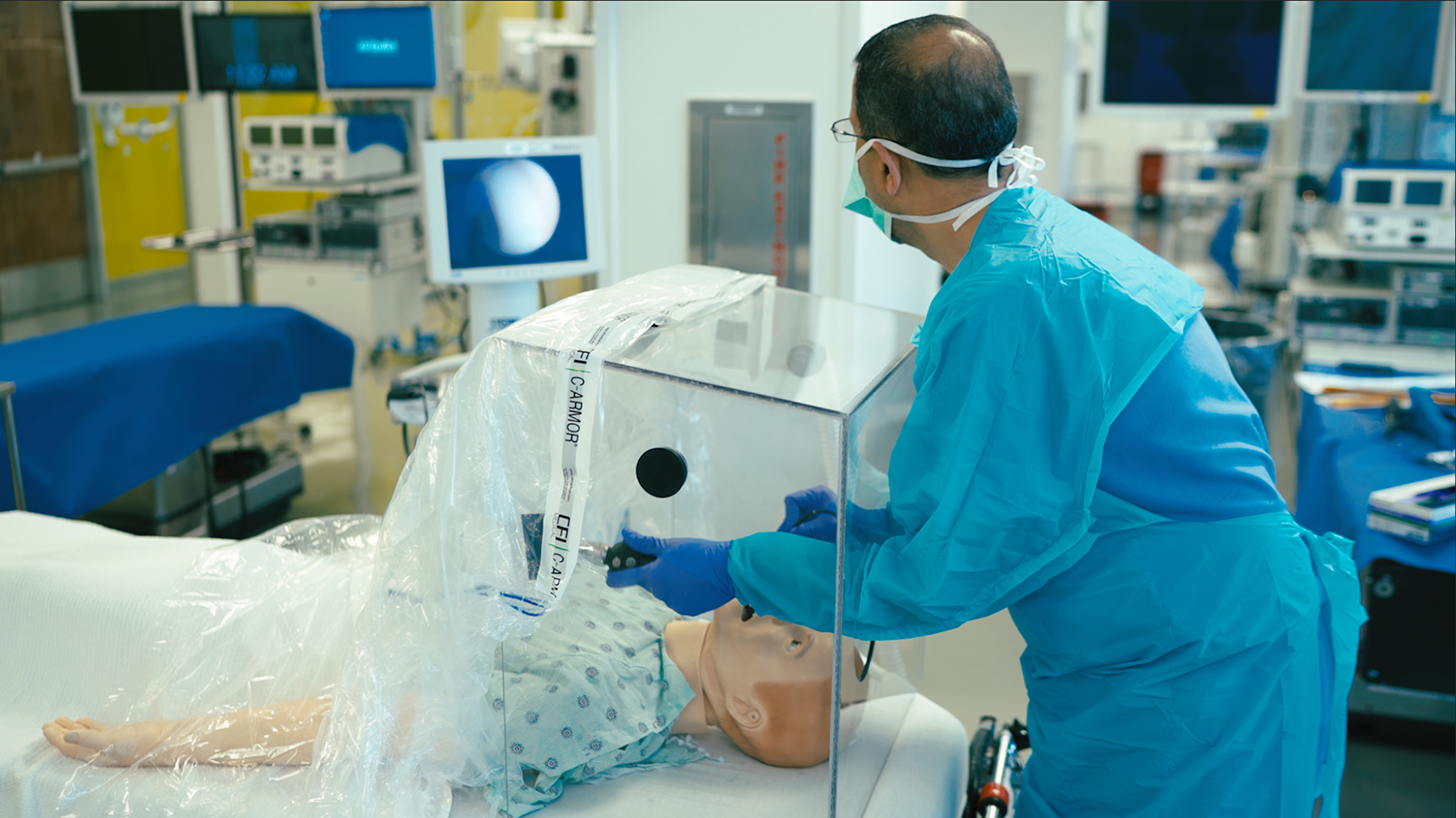
It Takes More than Plexiglass to Protect Against Aerosolized SARS-CoV-2
The FDA just revoked their EUA for intubation boxes – plastic shields that supposedly protect health care workers from becoming infected with SARS-CoV-2 – due to concerns over aerosol leaks. This study describes a better box, with negative pressure and filtration, that contains airborne virus.
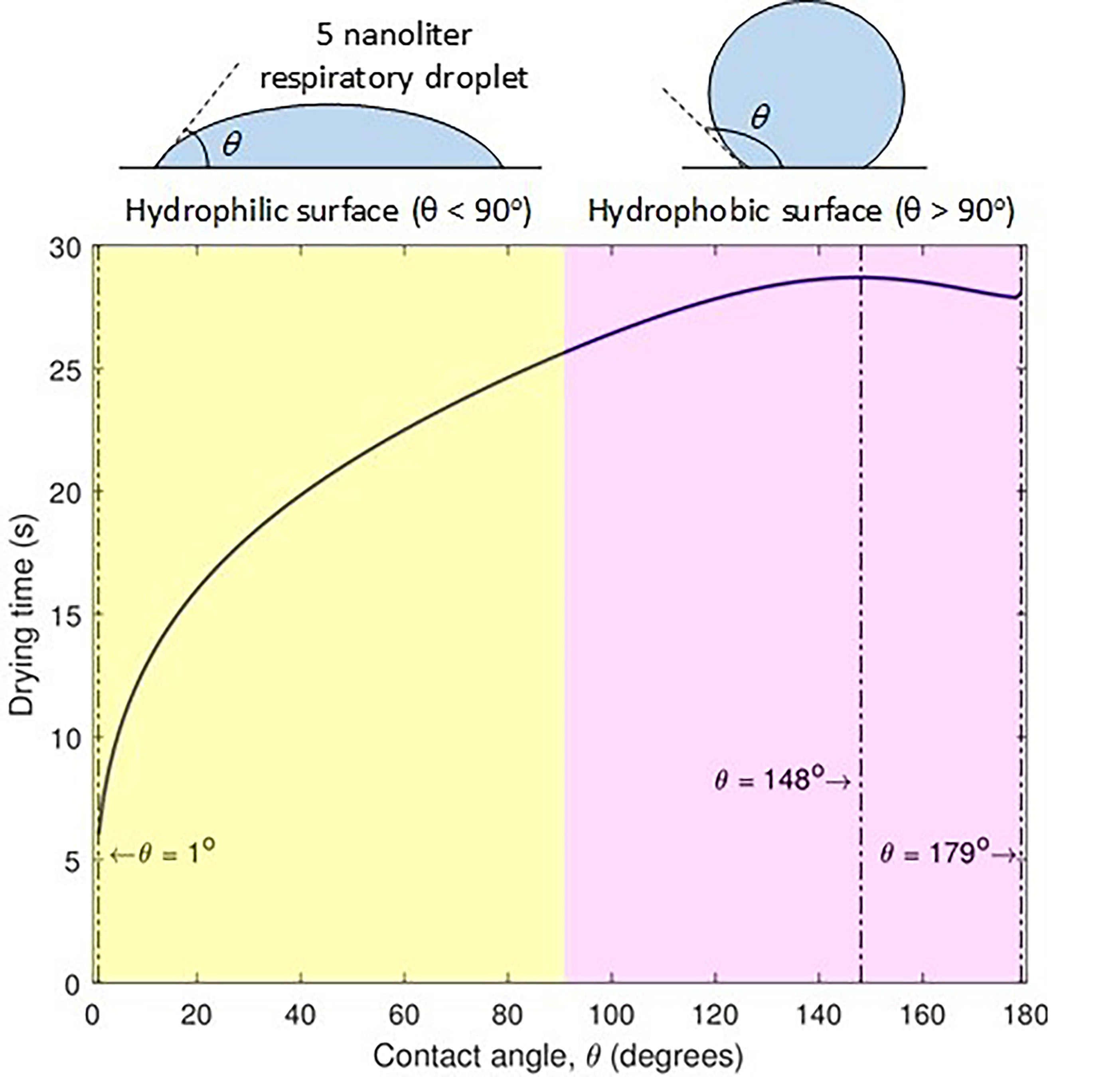
Masks, PPE Materials Should Be Hydrophilic
Since the COVID-19 virus spreads through respiratory droplets, researchers in India set out to explore how droplets deposited on face masks or frequently touched surfaces dry. Droplets can be expelled via the mouth or nose and studies have shown a substantially reduced chance of infection once they dry. In Physics of Fluids, the researchers publish their findings that surface wetting properties to reduce the drying time of droplets could help lessen the risk of infection from coronaviruses.

Researchers Create Mask Filtration Effectiveness Hierarchy
Infection prevention experts at the UNC Medical Center set out to gather evidence on the fitted filtration efficiency of dozens of different types of masks and mask modifications, including masks sterilized for reuse, expired masks, novel masks sourced from domestic and overseas sources, and homemade masks.

Portable UV Disinfection Chambers Could Help Address PPE Shortage
Portable disinfection chambers that use ultraviolet (UV) light to inactivate virus particles could allow emergency medical technicians, police officers, healthcare workers, pharmacy technicians, and others to quickly disinfect their personal protective equipment (PPE) as they need it.

Helping protect medical professionals
A media comprised of a sandwich of materials, tested by Sandia National Laboratories, is being manufactured into N95-like respirators that could be used in local medical facilities. The project originated from the urgent need for personal protective equipment when the COVID-19 outbreak began.

Ozone Disinfection Could Allow Safe Reuse of Personal Protective Equipment (PPE)
A new study shows that ozone gas, a highly reactive chemical composed of three oxygen atoms, could provide a safe means for disinfecting certain types of personal protective equipment that are in high demand for shielding health care personnel from Covid-19.

Evidence shows cloth masks may help against COVID-19
The international research team examined a century of evidence including recent data, and found strong evidence showing that cloth and cloth masks can reduce contamination of air and surfaces.

UCLA leads CDC-funded project to reduce COVID-19 infection among emergency room workers
The David Geffen School of Medicine at UCLA is leading a project in collaboration with the University of Iowa Carver College of Medicine to study ways to reduce the risk for COVID-19 infection among emergency department workers.
Research and innovation as an essential function amid the COVID-19 pandemic
Necessity being the mother of invention, Houston Methodist clinicians, researchers and staff have collaborated on a number of clinical device and research innovations in response to COVID-19. Houston Methodist Academic Institute leadership has continually emphasized translational research in new technologies.

Engineers design UV sterilization stations to aid healthcare workers during coronavirus pandemic
Engineers at Binghamton University, State University of New York have designed sterilization stations that use ultraviolet light to kill the coronavirus on any contaminated personal protective equipment (PPE) such as N95 masks and face shields.

Healthcare safety expert: culture of PPE use and actively caring is critical
A Virginia Tech researcher and teacher who has spent decades studying the psychology of safety says it’s more important than ever for frontline workers such as healthcare providers to look out for one another, keeping each other accountable in an effort to…

New Rutgers Saliva Test for Coronavirus Gets FDA Approval
The FDA has granted emergency use authorization (EUA) to Rutgers’ RUCDR Infinite Biologics and its collaborators for a new collection approach that utilizes saliva as the primary test biomaterial for the SARS-CoV-2 coronavirus, the first such approval granted by the federal agency. The new saliva collection method, which RUCDR developed in partnership with Spectrum Solutions and Accurate Diagnostic Labs (ADL), will allow for broader population screening than the current method of nose and throat swabs.

Joint Statement: A Call to Action for America to Fight COVID-19
The American Association of Critical-Care Nurses, with other healthcare organizations, has released a statement calling upon the government, private sector and all other Americans to “uphold their moral obligation by joining us in fighting the battle against coronavirus and the resulting COVID-19 disease.”
Ad Astra Coalition created to help in the fight against COVID-19
A coalition of businesses and government partners, the Ad Astra Coalition has joined together to answer some of the challenges being created in Wichita and Kansas by the COVID-19 pandemic. The coalition is co-led by Airbus Americas Engineering, Spirit AeroSystems, Textron Aviation, Wichita State University and WSU Tech.

West Virginia University partnerships help WVU Medicine community and beyond amidst personal protective equipment shortage
Josh Bintrim and Kelsey Crawford have worked in collaboration with Innovation Hub Director Gene Cilento, Assistant Director Kolin Brown and health care professionals at WVU Health Sciences Center to design surgical mask extenders, face shields and intubation boxes for use in medical facilities.
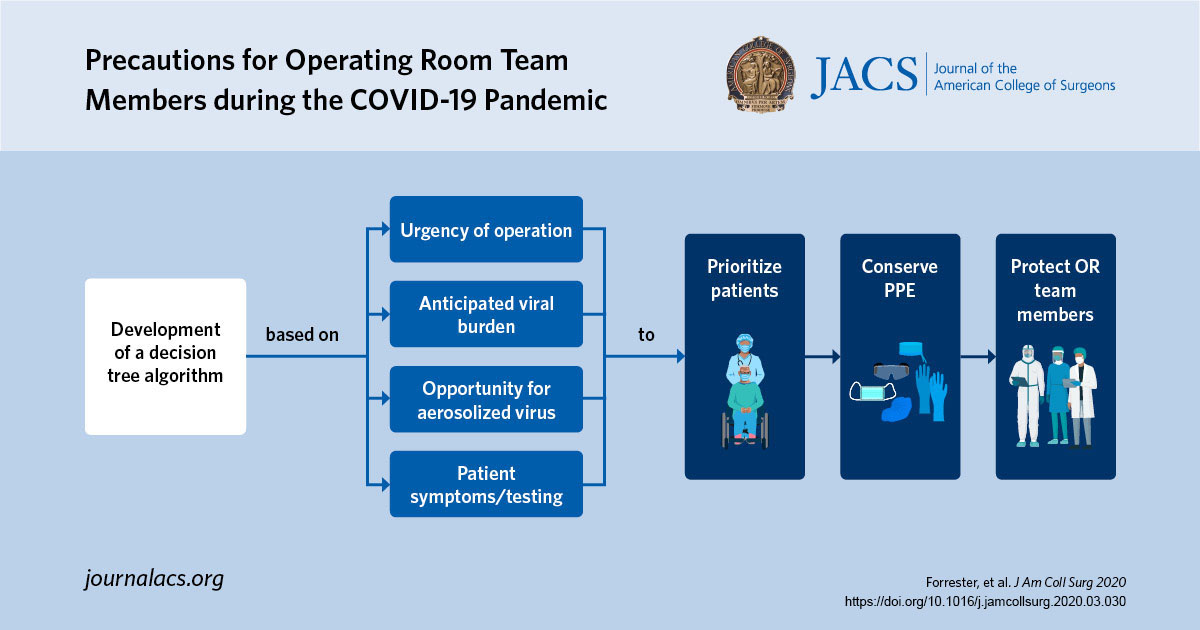
New algorithm aims to protect surgical team members against infection with COVID-19 virus
Researchers have created an algorithm that aims to protect operating room team members who perform urgent and emergency operations from COVID-19.
COVID-19: American College of Surgeons issues statement on personal protective equipment shortages
With many health care facilities facing shortages of personal protective equipment (PPE)—including face masks, gowns, and respirators—during the COVID-19 pandemic, the American College of Surgeons has released a statement on the issue.
ACADEMY OF NUTRITION AND DIETETICS URGES U.S. GOVERNMENT TO ADDRESS SHORTAGE OF PERSONAL PROTECTIVE EQUIPMENT DURING GLOBAL MEDICAL CRISIS
CHICAGO – During the novel coronavirus COVID-19 pandemic, the Academy of Nutrition and Dietetics, the world’s largest organization of food and nutrition professionals, urges the U.S. Department of Health and Human Services to address crucial personal protective equipment shortages for frontline health care workers and those providing access to food security programs.

Coronavirus relief dollars will help produce medical supplies, direct patient impact will take time, Notre Dame expert says
A $2 trillion coronavirus relief package that includes billions in aid for hospitals and medical facilities is on its way to President Donald Trump, but health care workers won’t feel its impact for weeks, according to a University of Notre…

Putting gloves into the right hands
Researchers across the Eberly College of Arts and Sciences at West Virginia University have moved quickly to donate personal protective equipment from their laboratories to healthcare workers on the front lines of the COVID-19 pandemic.

Nurses need protective equipment, but supplies are dwindling worldwide
Personal protective equipment is a nurse’s “protection and shield” against the novel coronavirus, said Benjamin Klos, an instructor in the West Virginia University School of Nursing and registered nurse with WVU Medicine. Yet as more people seek medical care for…

Do-It-Yourself Medical Devices, Protective Gear Fuel Battle Against COVID-19
The race is on to improvise ventilators, face shields, respirators, surgical gowns, and other health care gear to help the hundreds of thousands of people expected to swamp hospitals with waves of critical COVID-19 illness. Using 3D-printed parts, plastic-lined tablecloths, laser-cut gears and similar substitutions, a research team from the Georgia Institute of Technology is racing to develop “do-it-yourself” health care gear that can be assembled where it’s needed from components available locally.
AANA, ASA and APSF Issue Joint Statement on Use of Personal Protective Equipment During COVID-19 Pandemic
As anesthesia professionals are at an increased risk of exposure in caring for patients diagnosed with COVID-19, the AANA, the ASA, and APSF issued a joint statement today on the best use of personal protective equipment during the pandemic.

Study shows new surgical protective gear does not reduce surgical site infections
A study from UAB published in JAMA Surgery on Feb. 12 indicates that use of surgical jackets and head covers known as bouffants in operating rooms does not reduce the incidence of surgical site infections.