Researchers at Washington University School of Medicine in St. Louis, with collaborators at the University of Florida and Stanford University, identified a compound that, in mice, makes naloxone much more effective at counteracting a drug overdose.
Tag: Overdose
CDC report on drug overdose deaths: Johns Hopkins experts available
Experts from the Johns Hopkins Bloomberg School of Public Health will be available for interviews around the upcoming CDC Data Brief on Drug Overdose Deaths in the United States, 2002-2022, scheduled to be released on Thursday, March 21. Kenneth Feder,…
Medical Bioethics Expert Available – Philadelphia Lawmakers Vote to Prohibit Safe Injection Sites
What: According to The Philadelphia Inquirer, the Philadelphia City Council voted to prohibit supervised drug consumption sites across most of the city, greatly imperiling the future of such a facility if the legislation becomes law. Peter Clark, S.J., PhD, director…
Easier Access to Opioid Painkillers May Reduce Opioid-Related Deaths
Treatment medications are too stigmatized, costly and racially prescribed to stem the surge in overdoses, Rutgers researchers find.
Bloomberg American Health Initiative at the Johns Hopkins Bloomberg School of Public Health Announces Seventh Cohort of Bloomberg Fellows
The Bloomberg American Health Initiative at the Johns Hopkins Bloomberg School of Public Health announces the 2023 Bloomberg Fellows, each selected from organizations working to improve one of five critical public health challenges facing the country: addiction and overdose, adolescent health, environmental challenges, food systems for health, and violence.
Rutgers Poison Control Expert Available to Discuss Dangers of TikTok “Challenges”
Diane Calello, Executive and Medical Director of the New Jersey Poison Center based at Rutgers University, is available to discuss the dangers of the TikTok “challenges,” like the “Benedryl challenge,” which recently killed a 13-year-old. The following quotes from Dr.…

How to Get Narcan: The Lifesaving Drug for Opioid Overdose
Ochsner Health Doctor of Pharmacy discusses Narcan use and availability.
New Jersey Regulation Not Associated With Curbed Opioid Prescriptions or Shortened Usage
Rutgers research shows that it is difficult to dictate physician behavior, but that may be a good thing.
How AI Can Help Design Drugs to Treat Opioid Addiction
ROCKVILLE, MD – Approximately three million Americans suffer from opioid use disorder, and every year more than 80,000 Americans die from overdoses. Opioid drugs, such as heroin, fentanyl, oxycodone and morphine, activate opioid receptors. Activating mu-opioid receptors leads to pain relief and euphoria, but also physical dependence and decreased breathing, the latter leading to death in the case of drug overdose.
Fentanyl overdoses are on the rise. Here’s what to know and how you can help.
Community awareness is critical to preventing overdoses
Researchers Endorse Widespread Naloxone Over the Counter to Prevent Drug Overdose Deaths
Naloxone is an opioid receptor antagonist that rapidly reverses or blocks the effects of opioids, restores normal respiration and heart rhythm, and reverses the potentially fatal effects of an overdose. Although naloxone is included in U.S. CDC recommendations, the drug is currently prescribed to less than 1 in 70 patients prescribed high-dose opioid prescriptions. Researchers propose a call to action for all health providers and state medical societies to ensure the widest distribution and easy availability of naloxone, including over the counter, which is likely to be FDA-approved very soon.
Drug Used for Sleep Disorders Is Linked to Higher Risk of Overdose in Teens, Young Adults
Researchers found young people using benzodiazepines for common sleep conditions had an increased risk of overdose during the six months after starting treatment compared with other prescription sleep medications.
Rutgers Medical Toxicologist and Addiction Expert Available to Discuss Fentanyl Vaccine’s Impacts
Lewis Nelson, a medical toxicologist and chair of the Department of Emergency Medicine at Rutgers New Jersey Medical School, is available to discuss the possible benefits and many uncertainties of the experimental fentanyl vaccine. “Vaccines against other noninfectious agents, such…
At overdose events, arrests by police and combative behavior are rare, study finds
While police officers are often dispatched alongside other first responders when drug overdoses are reported, an analysis of hundreds of overdose events in one Rhode Island city found that there were scant incidents that actually needed involvement from law enforcement.
‘Years of Life Lost’ to unintentional drug overdose in adolescents spikes during pandemic
COLUMBUS, Ohio – The first year of the COVID-19 pandemic saw a 113% increase in the “Years of Life Lost” among adolescents and young people in the United States due to unintentional drug overdose, according to researchers at The Ohio State University Wexner Medical Center and College of Medicine.

WVU pharmaceutical experts caution ‘one pill can kill’ as new forms of fentanyl become more prevalent
Faculty members with the West Virginia University School of Pharmacy are issuing warnings about the rise of fentanyl in Mountain State communities and elsewhere following the recent seizure of a large amount of “rainbow fentanyl,” potent illegal pills resembling candy, by law enforcement officers in Monongalia County.
Increased overdose and mental health risks persist two years after opioid dose reduction
A new UC Davis Health study suggests that the increased rates of overdose and mental health crisis observed during the first year after opioid dose tapering persist through the second year. The study was published in JAMA Network Open.
Opioids: 4 ways to reduce harm, overdose and death
As America sees a record number of overdose deaths, taking action to reduce harm and tragedy due to opioids is vital. Here, three providers with expertise in substance use disorder care share ways individuals, communities and health care providers can help save lives.
IU study explored how people’s beliefs impact overdose education and naloxone distribution programs
A new study by Indiana University researchers, published in the journal BMC Public Health, explored people’s beliefs about overdose and naloxone as a step to understanding why some communities are not using the reversal medication.
IU study explored how people’s beliefs impact overdose education and naloxone distribution programs
A new study by Indiana University researchers explored people’s beliefs about overdose and naloxone as a step to understanding why some communities are not using the reversal medication.
Medication that lowers risk of overdose underused
Researchers at Washington University School of Medicine in St. Louis and Saint Louis University found that less than half of Americans who received treatment for opioid use disorder over a five-year period were offered a potentially lifesaving medication. The numbers were even lower for those with what’s known as polysubstance use disorder — when opioid users also misuse other substances.
Overdose Deaths Involving Cocaine or Meth Tripled in Shadow of Opioid Crisis
Even as the opioid epidemic dominated national attention over the past decade, the rate of overdose deaths involving cocaine, methamphetamine and other stimulants tripled, a new study in veterans suggests.
As Cocaine Overdose Deaths Increase, New Study @UCSDMedSchool Offers Potential Cocaine Addiction Treatment
Robert Anthenelli, MD, professor and director, Pacific Treatment and Research Center, UC San Diego School of Medicine, is available to talk about a new study that is investigating the potential use of a novel medication for cocaine addiction. UC San…
Study identifies possible antidote for club drug GHB overdose
Diclofenac and other NSAIDs may limit the passage of narcolepsy medication and illicit party drug GHB to the brain, decreasing the potential for fatal overdose, University at Buffalo researchers find.
First-time opioid prescriptions got shorter, less potent after CDC guidelines
Five years ago, CDC released an evidence-based guideline to help doctors treat their patients’ pain while balancing the risks and benefits of prescription opioid medications. A new study suggests it may have started to have an effect in the first two years after its launch.
Is reducing opioids for pain patients linked to higher rates of overdose and mental health crisis?
A UC Davis Health study published in JAMA found a 68% increase in overdose events and a doubling of mental health crises among patients who were on stable opioid therapy but saw their doses tapered.
Emergency department visits related to opioid overdoses up significantly during COVID-19 pandemic
Emergency department visit rates because of an opioid overdose increased by 28.5% across the U.S. in 2020, compared to 2018 and 2019, recent Mayo Clinic research finds. Emergency visits overall decreased by 14% last year, while visits because of an opioid overdose increased by 10.5%. The result: Opioid overdoses were responsible for 0.32 out of 100 visits, or 1 in every 313 visits, which is up from 0.25, or 1 in every 400 visits, the previous two years.
Carrying Naloxone Can Save Lives but Newly Abstinent Opioid Users Resist
UC San Diego School of Medicine researchers report that opioid users who participated in a 12-step abstinence program and recently stopped using drugs refused to take home naloxone, even if having it on hand might save lives.
Arkansas Society of Anesthesiologists and American Society of Anesthesiologists Applaud Arkansas Senate Public Health Committee on Passing SB 505 Giving Protection to Patients Prescribed Opioids
The Arkansas Society of Anesthesiologists (ARSA) and the American Society of Anesthesiologists (ASA) today applaud bill sponsor Sen. Cecile Bledsoe and the Arkansas Senate Public Health, Labor and Welfare Committee for helping to ensure the safety of patients prescribed opioids. Arkansas State Drug Director Kirk Lane and Jonathan Goree, M.D., a physician anesthesiologist and pain medicine specialist, testified for the bill.
Recommendations for the Overdose Epidemic in the COVID-19 Pandemic
A new report from researchers at the Johns Hopkins Bloomberg School of Public Health offers recommendations aimed at federal, state, and local policymakers to address the opioid epidemic during the pandemic.
Real-time opioid overdose tracking system shows rise in the time of COVID-19
An epidemic that was already raging before COVID-19 arrived has flared up in recent months, according to a real-time tracking system in Michigan. It shows a 15 percent rise in suspected opioid overdose deaths since March, compared with the same time last year, and a 29% rise in first responders’ use of the rescue drug naloxone.
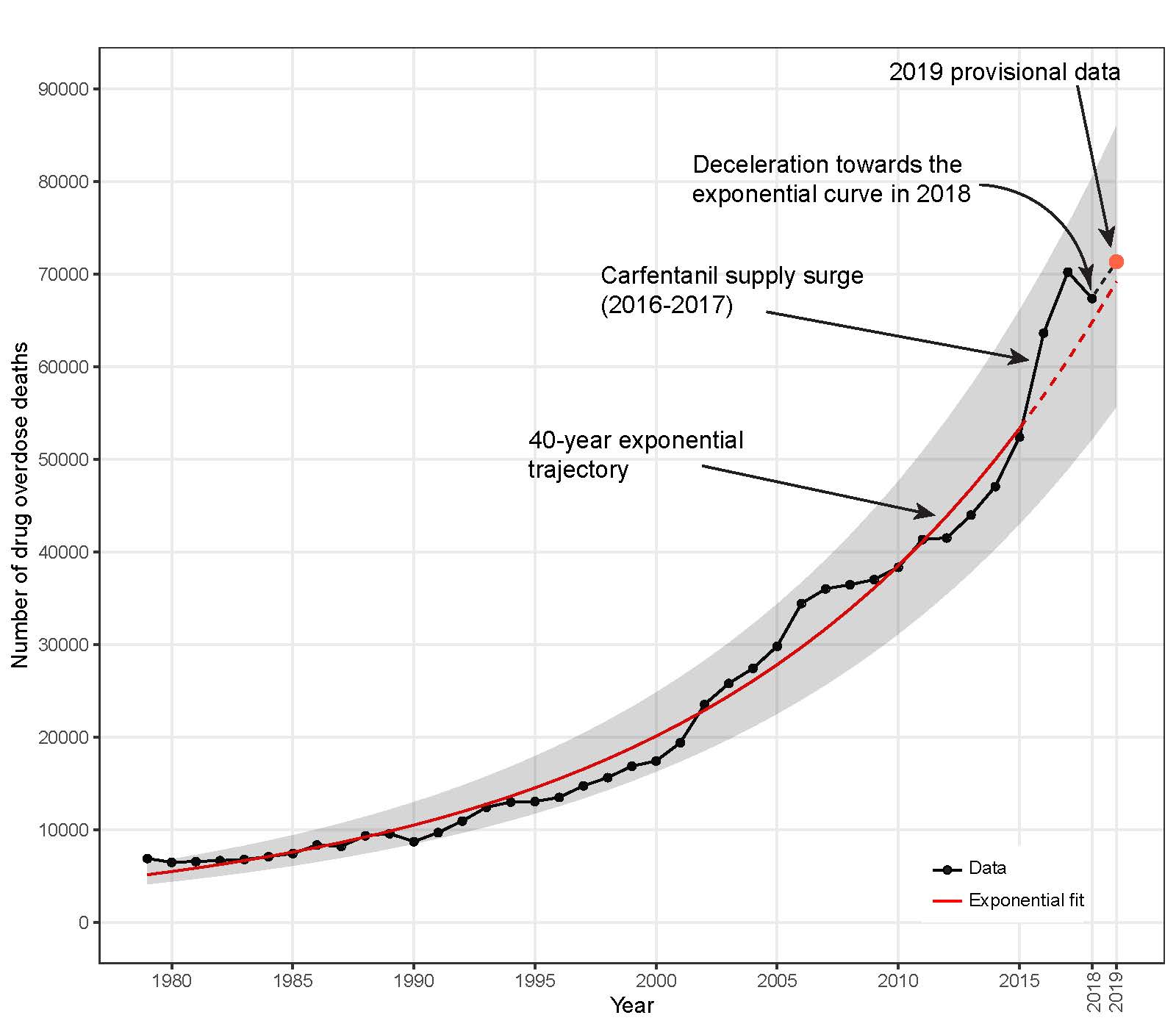
Potent Drug Supply Drop, Not U.S. Domestic Drug Policies, Likely Behind 2018’s Overdose Death Downturn
The slight decline in drug overdose deaths in 2018 coincides with Chinese regulations on the powerful opioid carfentanil, rather than the result of domestic U.S. efforts to curb the opioid epidemic, a University of Pittsburgh Graduate School of Public Health analysis revealed today.
Abandoned Buildings, Fear of Calling Police Contribute to High Rate of Fatal Overdoses in Philadelphia, New Study Shows
Abandoned Buildings, Fear of Calling Police Contribute to High Rate of Fatal Overdoses in Philadelphia, New Study Shows
Rutgers Expert Available to Comment on the Rise of Methamphetamine Use and Deaths
Perry N. Halkitis, PhD, MS, MPH, is dean and professor of the Rutgers School of Public Health and director of the Center for Health, Identity, Behavior and Prevention Studies (CHIBPS). Halkitis, author of Methamphetamine Addiction: Biological Foundations, Psychological Factors, and…
Most Youths Surviving Opioid Overdose Not Getting Timely Treatment to Avoid Recurrence
A study of more than 4 million Medicaid claims records during a recent seven-year period concludes that less than a third of the nearly 3,800 U.S. adolescents and young adults who experienced a nonfatal opioid overdose got timely (within 30 days) follow-up addiction treatment to curb or prevent future misuse and reduce the risk of a second overdose.
This drug could save their lives, but less than 2% of them get it
Only a tiny minority of people at risk for an opioid overdose actually are prescribed a drug that could save their lives, a new study suggests. And the odds of having a dose of the rescue drug were very low among some of the most at-risk groups, including those who had already survived a previous opioid overdose.
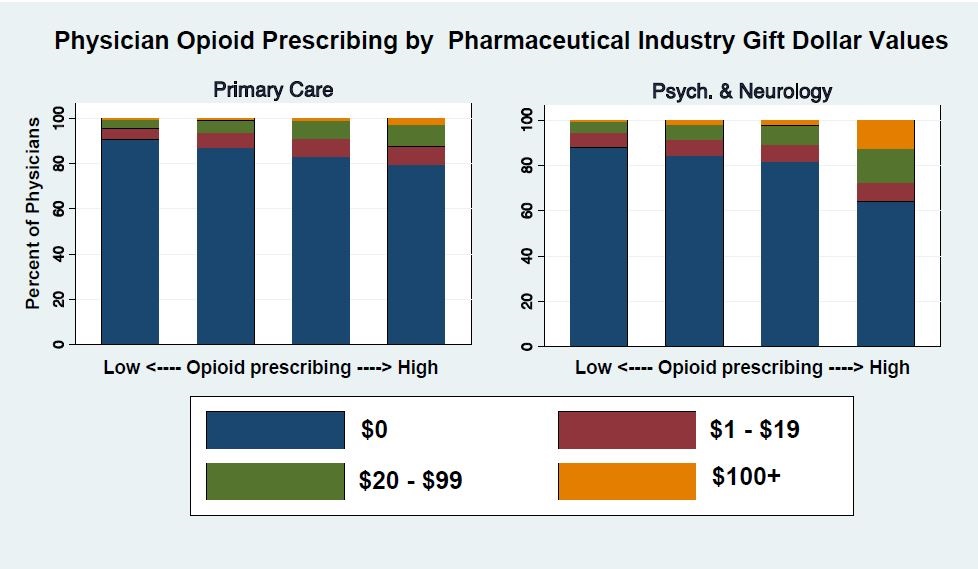
Opioid-Related Gifts from Pharma Companies Linked to Physician Prescribing by Specialty
Physicians who received gifts from pharmaceutical companies related to opioid medications were more likely to prescribe opioids to their patients in the following year, according to a new analysis.
National focus on overdose prevention should include alcohol too, study suggests
The need to prevent and rapidly treat opioid overdoses is in the spotlight. But a new study suggests more focus is needed on the risk of alcohol overdoses among people who use opioids of all kinds, and other drugs. Ninety percent of residential recovery center patients surveyed had overdosed on alcohol at least once, and 80 percent of them said that at the time of their overdose, they had also been taking other drugs.
Study highlights overdose risks of alcohol used with other drugs
Only one in five non-fatal alcohol overdoses results from use of alcohol alone, according to a study of patients in a large addiction treatment facility, with most alcohol overdoses involving concomitant use of other drugs. Alcohol can interact with other drugs ─ including marijuana, central nervous system depressants such as opioids, and stimulants such as cocaine ─ in various ways, and using them together is known to increase the likelihood and severity of overdose. Despite this, there is limited research examining the characteristics of alcohol overdose in the context of concomitant drug use. The new study, published in the journal Alcoholism: Clinical & Experimental Research, provides a clearer understanding of role of other drug use and its impact on outcomes of alcohol overdose.