Inequities in pain medication treatment received postpartum, after giving birth, were found in a Cedars-Sinai study of 18,000 women. The disparities were observed even among patients reporting the highest pain levels.

news, journals and articles from all over the world.

Inequities in pain medication treatment received postpartum, after giving birth, were found in a Cedars-Sinai study of 18,000 women. The disparities were observed even among patients reporting the highest pain levels.
Complex Regional Pain Syndrome (CRPS) is a chronic and debilitating pain disorder, typically considered lifelong with limited treatment options. Now, groundbreaking research finds that early detection and effective treatment can lead to significant recovery within 18 months, offering hope to millions of people worldwide.
A new study from the University of South Australia is putting people’s experiences of pelvic pain at the front of pain education to develop better pain management strategies and improved outcomes.
When you’re an autistic teenager living with chronic pain, getting treatment for your pain can be a challenging experience.
A recent study led by Assistant Professor Lindsay Jibb of the Lawrence Bloomberg Faculty of Nursing and Scientist at The Hospital for Sick Children (SickKids) found that parents of young children with cancer, along with pediatric cancer clinicians are in favour of an app-based solution that Jibb and her team are creating, to help parents manage their child’s cancer pain at home.
A preoperative nerve block used in combination with other medications can reduce the need for opioids to manage pain following spinal surgery, UT Southwestern Medical Center researchers found. The findings, published in European Spine Journal, suggest a way to lessen the reliance on opioids to reduce postoperative pain and help patients become ambulatory sooner.

A study, led by University of Oregon neuroscientist Shawn Lockery, points to worms as a useful tool for understanding more about the many roles that cannabinoids naturally play in the body. And it could help researchers develop better drugs that target this system.
According to the Centers for Disease Control and Prevention (CDC) and The National Vital Statistics System, drug-related overdose deaths have been rising over the past two decades in the United States. In 2021, 106,699 drug overdose deaths occurred. Adults aged 65 and over…
A statewide effort to treat the pain of surgery patients without increasing their risk of long-term dependence on opioids has paid off in Michigan, a study shows.
Whether it’s headaches, abdominal pain, or unrelenting joint soreness, up to a third of young people in Australia experience chronic pain. Now, a world-first study from the University of South Australia is providing valuable insights about how young people understand chronic pain, potentially helping thousands of sufferers to better manage their symptoms and long-term wellbeing.
Cleveland Clinic was awarded $5.5 million from the National Institutes of Health to develop a stem cell treatment for complex regional pain syndrome, a disease that causes debilitating chronic pain.
The research shows long-term potential for providing patients suffering from chronic pain an alternative to addictive treatments like opioids.
The American Association of Nurse Anesthesiology (AANA) applauds the Centers for Disease Control and Prevention (CDC) for providing more flexibility and clarity in their updated Clinical Practice Guidelines for Prescribing Opioids. The final guidelines include acknowledgment of the role of Certified Registered Nurse Anesthetists (CRNAs) as pain care providers, how pain care is administered, and the consideration for nonopioid therapies for subacute and chronic pain.
Popping a pill may bring short-term relief for arthritis-related joint pain, but many older adults may not realize that what they swallow could raise their risk of other health problems, or that other non-drug options could help them, a new poll suggests.
Adults who use cannabis consume more opioids after surgery. Reducing noise in the operating room (OR) improves postoperative behavior in children, including decreased temper tantrums and fussiness about eating. Minorities are less likely to have patient-centered end-of-life care. These are among the important research findings being presented at ANESTHESIOLOGY® 2022, the annual meeting of the American Society of Anesthesiologists (ASA), Oct. 21-25 in New Orleans.
Houston Methodist researchers present clinical evidence supporting the safety and efficacy of injecting pain medication directly into the tibia during knee replacement surgery for better postoperative pain management. The study revealed patients receiving a mixture of morphine and vancomycin injected into the shin bone have less pain post-surgery than those who received the infusion without morphine during surgery.
Like it or not, bumps and bruises are an unavoidable part of childhood. But while no parent wants their child to feel pain, teaching children about pain when they’re young can help them better understand and respond to pain when they’re older.
Cannabidiol is effective in improving immediate post-operative pain following arthroscopic rotator cuff repair, according to research presented today at the American Orthopaedic Society of Sports Medicine 2022 Annual Meeting.
Mindfulness meditation is effective in reducing pain relief; UC San Diego study reveals the underlying neural circuitry.
A new UC Davis Health study suggests that the increased rates of overdose and mental health crisis observed during the first year after opioid dose tapering persist through the second year. The study was published in JAMA Network Open.
A study by researchers at Hospital for Special Surgery (HSS) found that the antidepressant duloxetine reduced the use of opioid medication when added to a multimodal pain management regimen after knee replacement surgery. The study appeared in The Journal of Arthroplasty.
Researchers at UC San Diego School of Medicine report that high-frequency spinal cord stimulation proved more effective at improving perceived pain reduction than low-frequency SCS in patients studied, and that there was some variation in PPR between male and female patients.
Neuroimaging study reveals potential brain mechanism underlying chronic neuropathic pain in individuals with HIV. Findings may guide new clinical treatments targeting patients’ expectations for pain relief.
A new multi-society organizational consensus statement published in Regional Anesthesia & Pain Medicine establishes seven guiding principles for acute perioperative pain management to help institutions better care for patients having surgery.
Regenerative medicine has enormous implications for treatment and prevention of chronic pain including conditions like osteoarthritis, diabetic and peripheral neuropathy, and even spinal cord injuries and degenerative disk disease. According to one expert, there is potential to “[turn] back the time clock.”
Physicians prescribed opioids more often to their white patients who complained of new-onset low back pain than to their Black, Asian and Hispanic patients during the early days of the national opioid crisis, when prescriptions for these powerful painkillers were surging but their dangers were not fully apparent.
Treatment provides non-opiate alternative that is minimally invasive with emphasis on functional restoration.
Surgeons can ease their patients’ pain from common operations without prescribing opioids, and avoid the possibility of starting someone on a path to long-term use, a pair of new studies suggests.

A pain-management protocol designed by Emese Zsiros, MD, PhD, FACOG, to be reported at the American Society of Clinical Oncology 2021 annual meeting, resulted in a 45% decrease in opioids prescribed to patients undergoing surgery, without significant effect on recovery or satisfaction.
UC San Diego Health is conducting the first known randomized, double-blind, placebo-controlled clinical trial looking at cannabis as a potentially effective treatment for acute migraines.
Researchers find that opioids are not necessary for managing post-knee surgery pain.
For the first time, an app has been shown to reduce key symptoms of chronic pain. A UNH-led study evaluated the impact of Manage My Pain(MMP), a digital health solution on chronic pain patients.

In the wake of the opioid addiction crisis that has cost more than 500,000 U.S. lives, medical investigators have focused on finding new methods to help patients control pain.

UC San Diego School of Medicine researchers report that older adults are increasingly using cannabis to treat a variety of common health conditions, including pain, sleep disturbances and psychiatric conditions like anxiety and depression.

A team of researchers in the United States and Japan reports that spinal cord stimulation (SCS) measurably decreased pain and reduced motor symptoms of Parkinson’s disease, both as a singular therapy and as a “salvage therapy” after deep brain stimulation (DBS) therapies were ineffective.

The NIH has awarded NYU College of Dentistry researchers Nigel Bunnett, PhD, and Brian Schmidt, DDS, MD, PhD, a $3.9 million grant to study targeting endosomal receptors for the treatment of chronic pain. The five-year grant will support Bunnett and Schmidt’s collaborative research, which aims to ultimately yield improved pain management without the need for opioids.
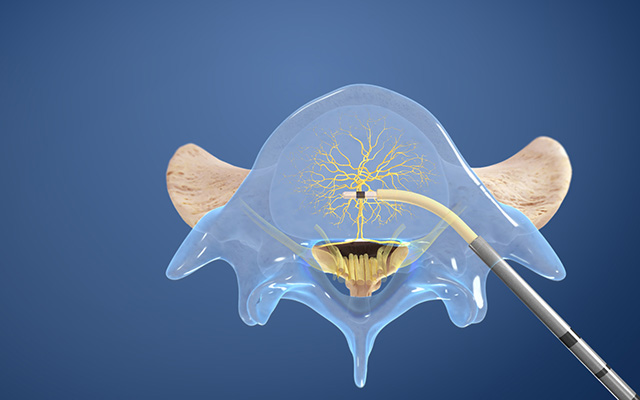
UC San Diego Health is now offering a new minimally invasive approach to provide relief for patients suffering from chronic low back pain (CLBP).The new treatment is called “Intracept,” an outpatient procedure that targets nerves located in the vertebrae or bones of the spine.

Choice and control are important factors for ensuring a positive childbirth experience, yet until recently, little was known about the impact of alternative administrations of fentanyl – one of the pain relief drugs used during labour– on both mother and baby.

A Henry Ford Hospital study published in the Journal of Arthroscopic and Related Surgery has found that patients who underwent knee surgery and other types of sports medicine procedures could manage their pain without opioids or a minimal dosage. “This is a large prospective study and our hope is that non-opioid use will gain momentum and that others may tweak our protocol and use it throughout orthopedics, from joint surgery to spine surgery and other surgeries” says Vasilios (Bill) Moutzouros, M.D., chief of Sports Medicine, a division of the Department of Orthopedic Surgery and the study’s lead author.
The use of medical cannabis has garnered a lot of recent attention, especially as parts of the United States and Canada have legalized its use. While it has been studied in cancer and nerve pain, not much is known about the usage rate and its efficacy in managing chronic musculoskeletal (MSK) pain. According to a new study released as part of the American Academy of Orthopaedic Surgeons’ (AAOS) Virtual Education Experience, up to 20% of patients presenting to an orthopaedic surgeon with chronic MSK pain are using cannabis to manage their pain, with many reporting success. Additionally, two-thirds of non-users are interested in using it for the management of MSK pain, prompting a need to further study its effects.
The COVID-19 pandemic is an unprecedented situation that has raised healthcare questions for patients of all ages. If you need an orthopaedic surgeon to discuss the impact of COVID-19 on patients’ musculoskeletal health, the American Academy of Orthopaedic Surgeons (AAOS)…

Diane Hoffmann is the Jacob A. France Professor of Health Law at University of Maryland School of Law where she directs the Law & Health Care Program and the Maryland Health Care Ethics Committee Network. She is able to speak…

A Texas hospital developed an integrated approach that reduced ventilation time for ICU patients. The 2018 study, in AACN Advanced Critical Care, is the first to examine the effects of implementing protocol-directed sedation with the coordinated use of two evidence-based assessments across multiple disciplines.
Medical marijuana users who say they have high levels of pain are more likely than those with low pain to say they use cannabis three or more times a day, a new study finds.
Every day nearly 200 people die from an overdose of drugs or from alcohol poisoning, with opioids responsible for the majority. Recognizing the signs and knowing how to respond to medical emergencies, including carrying and administering naloxone in cases of opioid overdose, can save lives says the ASA.
In honor of National CRNA Week (Jan. 19-25, 2020), Reps. Jan Schakowsky (D-IL), Lucille Roybal-Allard (D-CA), and Sam Graves (R-MO) today introduced a bipartisan resolution on the House floor, “Recognizing the roles and the contributions of America’s Certified Registered Nurse Anesthetists (CRNAs) and their role in providing quality health care for the public.”

A series of seven articles in AACN Advanced Critical Care focuses on the challenges of safe, effective pain management in the ICU, including more Americans reporting daily chronic pain and the rapidly increasing prevalence of opioid misuse and opioid use disorder.
Mount Sinai Kravis Children’s Hospital announced today that PetSmart Charities has offered a gift of $75,000 to extend the tenure of Professor Bunsen Honeydew the hospital’s first of three facility dogs, through October 2020.
Patients who have chosen to treat chronic pain with implanted peripheral nerve stimulation no longer need to be tethered permanently to the device. According to findings from a study in amputees, placing the device for just 60 days resulted in sustained pain relief and functional improvements.
Researchers at Thomas Jefferson University and the University of Virginia retrospectively analyzed patient records see if side effects increased after repeated infusions. They actually found a couple of benefits.
Colleagues at the University of California at Irvine have developed an electronic prescription drug accountability program to keep track of prescribing among hospitalists, primary care physicians, and emergency department physicians within an institution.