3DBioFibR Inc., a leader in the development of nature-inspired biomaterials, has announced its partnership with the RegeneratOR Test Bed to further its mission of revolutionizing tissue engineering.
Tag: Regenerative Medicine

Polymeric coating improved piezoelectric properties of composites for drug delivery
Scientists from Immanuel Kant Baltic Federal University found out that polymeric coating enables to improve the structure and properties of magnetoelectric composites, that are used in medicine for drug delivery and also in creation of implants and tissues. Thus, modification with polymer helps equal distribution of composite’s components, and also enhances its piezoelectric properties by 40%.
Advancing regenerative medicine therapies
University and community guests recently gathered to celebrate the 7,700 square-foot Good Manufacturing Practice facility’s grand opening in Hewitt Hall’s basement on the UC Irvine campus. Although the highly sterile environment remains off-limits for tours, the gala highlighted its importance to the campus, the UC system and the local community.
Bladder buzz: technologies to improve bladder surgery and monitoring
NIBIB-funded researchers are working to make bladder surgeries better, tackling the issue from two vantage points: improving bladder function using a biodegradable construct that facilitates tissue regeneration, and enhancing patient monitoring by developing an implantable bladder sensor.
A nanomaterial one-two punch quickly heals wounds in diabetic animal model
Wounds that are superficial for some can be life-threatening for others. With diabetic wounds, healing can be slow, particularly in the feet, increasing the tissue’s susceptibility to infection. Foot ulcers and other diabetic foot complications have similar mortality rates to some cancers, yet progress toward improved treatments has plateaued.
Deer antler stem cell niche: An interesting perspective
In recent years, there has been considerable exploration into methods aimed at enhancing the regenerative capacity of transplanted and/or tissue-resident cells. Biomaterials, in particular, have garnered significant interest for their poten
Therapeutic potential of urine-derived stem cells in renal regeneration following acute kidney injury: A comparative analysis with mesenchymal stem cells
BACKGROUNDAcute kidney injury (AKI) is a common clinical syndrome with high morbidity and mortality rates. The use of pluripotent stem cells holds great promise for the treatment of AKI. Urine-derived stem cells (USCs) are a novel and versa
Nano Drug Accelerates Diabetic Wound Healing in Mice
Researchers at the Icahn School of Medicine at Mount Sinai have designed a regenerative medicine therapy to speed up diabetic wound repair. Using tiny fat particles loaded with genetic instructions to calm down inflammation, the treatment was shown to target problem-causing cells and reduce swelling and harmful molecules in mouse models of damaged skin. Details on their findings were published in the May 20 online issue of the Proceedings of the National Academy of Sciences (PNAS).
Combining novel biomaterial and microsurgery might enable faster tissue recovery
For soft tissue to recover and regrow, it needs blood vessels to grow to deliver oxygen and nutrients. Sluggish vascularization, however, can slow or even prevent recovery and regrowth of lost or damaged soft tissue after a severe injury or serious illness such as cancer.
Human dental pulp stem/stromal cells in clinical practice
Dental pulp stem/stromal cells (DPSCs) are fibroblast-like, neural crest-derived, and multipotent cells that can differentiate into several lineages. They are relatively easy to isolate from healthy and inflamed pulps, with little ethical c
Regener-Eyes®: Industry Spotlight with CEO & Founder of Regener-Eyes® & Mechanisms Behind Tear Hyperosmolarity in Dry Eye
Dr. Maria Sampalis, host of the Reframing Eye Care podcast, welcomes Dr. C. Randall Harrell, the esteemed CEO & Founder of Regener-Eyes®, for an exclusive industry spotlight.
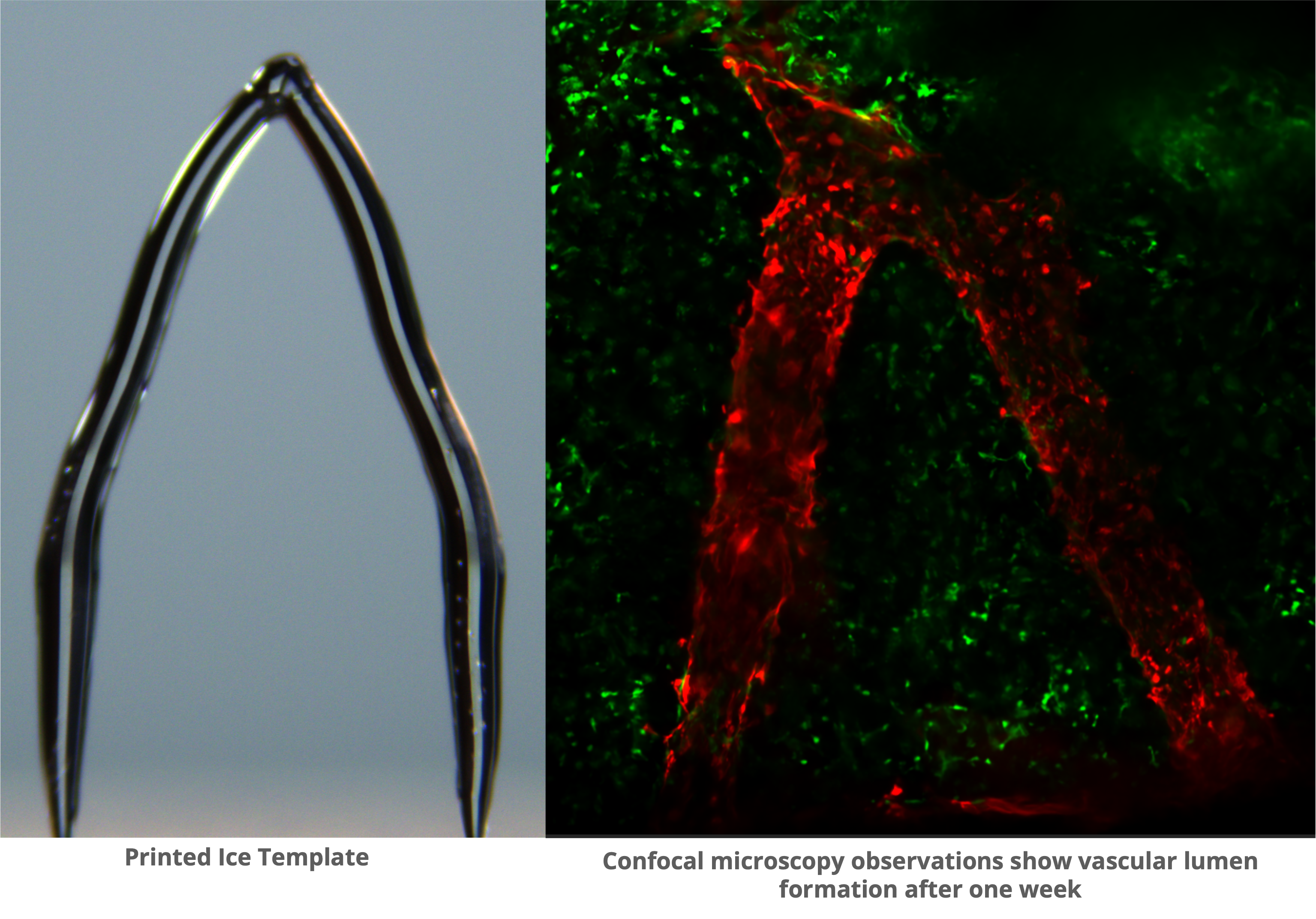
3D Ice Printing can Create Artificial Blood Vessels in Engineered Tissue
Over 100,000 individuals in the United States are currently in need of organ transplants. The demand for organs, such as hearts, kidneys, and livers, far exceeds the available supply and people sometimes wait years to receive a donated organ.

RESEARCH ALERT: The New Geography of the Gut
Investigators from Cedars-Sinai; the University of California, San Francisco (UCSF); Harvard University; and the Weizmann Institute of Science in Israel conducted a study to determine where individual nutrients are absorbed in the small intestine. For the first time, they identified the molecular markers that define five distinct intestinal regions.
Wake Forest Institute for Regenerative Medicine Awarded $160 Million 10-Year U.S. National Science Foundation Regional Innovation Engines Grant
The Wake Forest Institute for Regenerative Medicine (WFIRM) is the recipient of an inaugural U.S. National Science Foundation (NSF) Engines Program award. The NSF Engines: Piedmont Triad Regenerative Medicine Engine is a regional project that provides an innovation ecosystem to stimulate workforce development, job creation, and economic growth through the development of technologies that benefit the emerging industry.
Wake Forest Institute for Regenerative Medicine (WFIRM) Secures National Science Foundation (NSF) Grant Renewal for Summer Undergraduate Research Program
Building upon the success of its previous REU program (Award #1659663, 2018-2022), WFIRM’s renewed grant has a specific focus on growing the increasing the engagement of underrepresented minority groups, women, and non-traditional students, including students attending 2- and 4-year universities.
UC Irvine study exposes risks of direct-to-consumer stem cell, exosome COVID-19 therapy ads
Irvine, Calif., Oct. 26, 2023 — A study from the University of California, Irvine has revealed that in 2022, 38 North American businesses used direct-to-consumer advertising to promote unproven stem cell interventions and exosome products as purported treatments and preventatives for COVID-19. Collectively, these organizations operated or facilitated access to 60 clinics – with 24 in the U.
DNA aptamer finds novel application in regulating cell differentiation
Generating specific cell lineages from induced pluripotent stem cells and embryonic stem cells is the holy grail of regenerative medicine.
ReMDO Grants Support Commercialization of Regenerative Medicine Therapies
The grant opportunity will create a continued impact on the rate of clinical translation for regenerative medicine therapies and the commercialization of regenerative medicine products within the global market.
Brinter Joins the RegenMed Hub
Brinter Bio-Implant company joined the RegeneratOR’s Innovation Accelerator in 2023, located in the Regenerative Medicine Hub (RegenMed Hub), a rapidly growing regenerative medicine ecosystem based in the Innovation Quarter, in Winston-Salem.
Skin deep: breakthrough drug gives hope to ‘butterfly’ children
It’s a beautiful moniker, but for the world’s butterfly children’ it belies a devastating reality filled with enormous pain and suffering caused by a rare skin condition – Epidermolysis Bullosa (EB).
Discovery of Skin Cell Function Could Open Doors to Improved Burn Healing
Tissue engineering research has shown that a skin cell type could be a new therapeutic target to accelerate the healing of burns and possibly other wounds.
WFIRM bioprinting research makes history when it soars to the ISS
The Wake Forest Institute for Regenerative Medicine (WFIRM) will make history this month when the first bioprinted solid tissue constructs soar to the International Space Station (ISS) on board the next all private astronaut mission by commercial space leader Axiom Space.
Mount Sinai Launches Institute for Regenerative Medicine
Institute, including three new centers, will lead research to foster novel discoveries and explore new treatments for a range of diseases from leukemia to Alzheimer’s disease.
Former Senior Level Department of Defense Official Joins RegenMed Hub
The Regenerative Medicine Hub continues to grow and attract top talent with the addition of Ron Hann, PhD, a former senior level official with the Department of Defense.
Immunaeon Joins the RegenMed Hub
Immunaeon is the latest addition to the RegeneratOR’s Innovation AcceleratOR, located in the Regenerative Medicine Hub (RegenMed Hub), a rapidly growing regenerative medicine ecosystem based in the Innovation Quarter of Winston-Salem.
Silicon nanochip could treat traumatic muscle loss
Technology that can change skin tissue into blood vessels and nerve cells also shows promise as a treatment for traumatic muscle loss.
15 Years of Heart
Pioneering heart care is a tradition at Cedars-Sinai. It’s a tradition that took root in 1924, when Cedars-Sinai became home to the first electrocardiogram machine in Los Angeles.
MIMEDX Joins the RegenMed Hub
MIMEDX is the latest addition to the RegeneratOR Innovation Accelerator, located in the Regenerative Medicine Hub (RegenMed Hub), a rapidly growing regenerative medicine ecosystem based in the Innovation Quarter of Winston-Salem.
RTT Medical Joins RegenMed Hub Innovation Accelerator
RTT Medical is the newest tenant of the Innovation Accelerator, a support ecosystem created by the RegenMed Development Organization (ReMDO) to help companies with new or emerging regenerative medicine technologies speed up the translation of products to patients.
Eliksa Therapeutics launched with University of Utah’s commercial and clinical-stage regenerative medicine technology
Eliksa Therapeutics, a regenerative medicine company developing novel therapeutics for a range of debilitating diseases, announced today it has launched with investments from the University of Utah (U) and Militia Hill Ventures (MHV) to develop and commercialize multiple clinical programs using the regenerative medicine technology developed at the U.
Scientists develop blueprint for turning stem cells into sensory interneurons
Key takeaways:
• Just like the real thing. The stem cell–derived interneurons, which play a role in sensations like touch and pain, are indistinguishable from their real-life counterparts in the body.
• Tomorrow’s therapies. In addition to potential treatments for injury-related sensation loss, the discovery could lead to new methods for screening drugs for chronic pain.
• Moving forward. While stem cells from mice were used in the research, scientists are now working to replicate the findings with human cells.
Recharging cartilage after knee damage
Osteoarthritis – a painful condition that results from the deterioration of the cartilage in our joints – affects millions of people worldwide. To combat this issue, NIBIB-funded researchers are developing an implantable, biodegradable film that helps to regenerate the native cartilage at the site of damage. Their study, performed in rabbits, could be an initial, important step in the establishment of a new treatment for this common condition.
Scientists Gain Ground on Rare Congenital Neurological Disorder
Two recent discoveries co-led by scientists at Cedars-Sinai may help lead to new ways to treat patients with Allan-Herndon-Dudley syndrome (AHDS), a brain development disorder that causes severe intellectual disability and problems with movement.
Smidt Heart Institute: Annual Report Highlights
The 2022 Annual Report from the Smidt Heart Institute at Cedars-Sinai is available now, detailing the latest research and medical achievements by the expert team ranked No. 1 for cardiology and cardiac surgery in California by U.S. News & World Report.
Businesses selling non-FDA-approved stem cell products grew four-fold in five years, UCI study says
More than four times as many businesses and clinics than were identified in 2016 are selling stem cell products not approved by the U.S. Food and Drug Administration and lack convincing evidence of safety and efficacy, according to a five-year study conducted by University of California, Irvine Program in Public Health professor of health, society and behavior Leigh Turner. The analysis appears online in the journal Cell Stem Cell.
AMSSM Releases Position Statement on Regenerative Medicine in Sports Medicine
The American Medical Society for Sports Medicine (AMSSM) has released a position statement on Principles for the Responsible Use of Regenerative Medicine in Sports Medicine.
UCI receives 5-year, $5 million CIRM award for training of diverse researchers
The University of California, Irvine has received a five-year, $5 million award from the California Institute for Regenerative Medicine to support a comprehensive doctoral, postdoctoral and clinical researcher training program to prepare the current and next generation of leaders in stem cell biology, gene therapy and regenerative medicine.
The Promise of Regenerative Medicine to Treat Chronic Pain
Regenerative medicine has enormous implications for treatment and prevention of chronic pain including conditions like osteoarthritis, diabetic and peripheral neuropathy, and even spinal cord injuries and degenerative disk disease. According to one expert, there is potential to “[turn] back the time clock.”
RegeneratOR Workforce Development Receives NSF Award
With the recent announcement of the RegeneratOR Test Bed to support regenerative medicine start up companies, the Wake Forest Institute for Regenerative Medicine (WFIRM) and the RegenMed Development Organization (RemDO) are embarking on the next step – to help create the future workforce.
Phase Holographic Imaging Supports New RegeneratOR Test Bed with Label Free Non-destructive Live Cell Imaging
Phase Holographic Imaging is collaborating with the RegeneratOR Test Bed, a new regenerative medicine endeavor in North Carolina, by providing its technology to help support start-up companies in the regenerative medicine space.
RegeneratOR Test Bed to Launch Start Ups, Advance Regenerative Medicine Ecosystem
The RegenMed Development Organization (ReMDO), a non-profit foundation headquartered in Winston-Salem, NC, and dedicated to advancing the regenerative medicine field nationwide, and the Wake Forest Institute for Regenerative Medicine (WFIRM), the largest regenerative medicine institute in the world, announce the launch of the RegeneratOR Test Bed.
ACSM Annual Meeting Research Highlights for June 3
ACSM’s comprehensive sports medicine and exercise science conference takes place virtually from June 1 to 5 with programming covering the science, practice, public health and policy aspects of sports medicine, exercise science and physical activity.
Research Highlights from 2021 ACSM Virtual Annual Meeting: Exercise in Regenerative Medicine
The 2021 Virtual ACSM Basic Science World Congress focuses on regenerative medicine. Chaired by Marcas M. Bamman, Ph.D., FACSM, from the University of Alabama at Birmingham, this world congress brings together researchers to discuss cutting-edge science in this rapidly developing field.
Journalists: Be our guest at the 2021 Virtual ACSM Research Conference
Gain story ideas and learn about cutting-edge science at ACSM’s comprehensive sports medicine and exercise science conference that covers the science, practice, public health and policy aspects of sports medicine, exercise science and physical activity.

Helping humans heal
In a lab on the upper floors of Engineering Hall, something is growing. It’s not a plant. And it’s not an animal. What Ronke Olabisi is growing in her lab is us. From new skin and retinal tissue to hearts and livers, she’s developing the tools to rebuild and repair the human body. A UCI assistant professor of biomedical engineering, Olabisi has been working with regenerative tissue for the better part of seven years, using a hydrogel based on polyethylene glycol diacrylate.
UCI biomedical engineers spotlight disparities in knee and jaw joint treatments
Irvine, Calif., May 5, 2021 – If you haven’t had knee surgery, you may have a friend or relative who has. But do you know anyone who has had an operation on their jaw? Although the temporomandibular joint is crucial to speaking, chewing and even breathing, treatments for TMJ disorders are far less common than those for the knee.
Mayo Clinic preclinical discovery triggers wound healing, skin regeneration
Difficult-to-treat, chronic wounds in preclinical models healed with normal scar-free skin after treatment with an acellular product discovered at Mayo Clinic. Derived from platelets, the purified exosomal product, known as PEP, was used to deliver healing messages into cells of preclinical animal models of ischemic wounds. The Mayo Clinic research team documented restoration of skin integrity, hair follicles, sweat glands, skin oils and normal hydration.
Ischemic wounds occur when arteries are clogged or blocked, preventing important nutrients and oxygen from reaching the skin to drive repair. This groundbreaking study titled, “TGF-β Donor Exosome Accelerates Ischemic Wound Healing,” is published in Theranostics.
Audacious projects develop imaging technology to aid eye tissue regeneration
As regenerative therapies for blinding diseases move closer to clinical trials, the National Eye Institute’s functional imaging consortium, a part of the NEI Audacious Goals Initiative (AGI), is pioneering noninvasive technologies to monitor the function of the retina’s light-sensing neurons and their connections to the brain.
Pericardial Injection Effective, Less Invasive Way to Get Regenerative Therapies to Heart
Injecting hydrogels containing stem cell or exosome therapeutics directly into the pericardial cavity could be a less invasive, less costly, and more effective means of treating cardiac injury.

Evan Snyder named Fellow of the American Institute for Medical and Biological Engineering
The American Institute for Medical and Biological Engineering (AIMBE) has elected to its College of Fellows Evan Y. Snyder, M.D., Ph.D., professor and founding director of the Center for Stem Cells and Regenerative Medicine at Sanford Burnham Prebys Medical Discovery Institute. Snyder was nominated, reviewed, and elected by his peers and members of the College of Fellows for his seminal contributions to regenerative medicine.