Therapeutic tool used for children with kidney issues stemming from sepsis
Tag: Sepsis
“Anti-Choke Mug” – Chula Innovation for Neuro Patients to Drink Water Confidently
Chula Medicine has designed an anti-choke mug with calculated angle, amount, and time of water flow from the mug to the patient’s lips hoping to reduce choking that may lead to lung infection, bring peace of mind to caregivers, and make it safer for patients who will have a better quality of life.

Detecting Pathogens–and Sepsis–Faster and More Accurately by Melting DNA
A new analysis method can detect pathogens in blood samples faster and more accurately than blood cultures, which are the current state of the art for infection diagnosis. The new method, called digital DNA melting analysis, can produce results in under six hours, whereas culture typically requires 15 hours to several days, depending on the pathogen.
Study finds SARS-CoV-2-associated sepsis was more common, deadly than previously thought
Using data from Mass General Brigham’s electronic health records, Brigham researchers quantified the burden of SARS-CoV-2-associated sepsis early in the pandemic
More people develop sepsis than we thought — but more survive
Sepsis, also colloquially referred to as blood poisoning, is a serious condition. Just over 3,000 people die with a diagnosis of sepsis in Norwegian hospitals each year.
Sepsis – as common as cancer, as deadly as a heart attack
In 2016, the research team conducted an initial study in southern Sweden (Skåne) where they revealed that sepsis is much more common than previously believed.
Analysis Reveals Factors Associated With Patients With Sepsis Who Require Mechanical Ventilation
An analysis of 10 years of health data showed that risk factors for needing mechanical ventilation changed for patients with newly diagnosed sepsis as more time passed after onset.
MD Anderson Research Highlights for June 7, 2023
The University of Texas MD Anderson Cancer Center’s Research Highlights showcases the latest breakthroughs in cancer care, research and prevention.
Antibiotics crisis: nanoparticles as therapy guide
In the case of blood poisoning, the bacteria in the blood must be identified as fast as possible so that a life-saving therapy can be started. Empa researchers have now developed “sepsis sensors” with magnetic nanoparticles that detect bacterial pathogens within a short period of time and identify suitable candidates for antibiotic therapies.
AACC Releases Guidance on Procalcitonin Testing to Improve Care for Patients with Bacterial Infections
AACC has issued expert guidance on clinical testing for procalcitonin, a blood marker that helps detect serious bacterial infections and sepsis. By giving clinicians and laboratory professionals much-needed clarity on how to best use procalcitonin tests, the new guidelines could improve the treatment of critically ill patients and those with certain lower respiratory infections.
Optimizing sepsis treatment timing with a machine learning model
A new machine learning model that estimates optimal treatment timing for sepsis could pave the way for support tools that help physicians personalize treatment decisions at the patient bedside, researchers say.
Patients with septic shock benefit from a combination of hydrocortisone-fludrocortisone therapy
A new study in JAMA Internal Medicine by researchers from Boston University Chobanian & Avedisian School of Medicine shows that patients receiving a combination of hydrocortisone and fludrocortisone had lower death rates and discharge to hospice compared to those who only received hydrocortisone.
Critical care specialists debate best management strategy for sepsis and septic shock
In a new Annals ‘Beyond the Guideline’s feature, two critical care specialists discuss and debate conditional guideline recommendations on using lactate to guide resuscitation, the use of balanced crystalloids versus normal saline, and the use of corticosteroids for management of sepsis and septic shock. All ‘Beyond the Guidelines’ features are based on the Department of Medicine Grand Rounds at Beth Israel Deaconess Medical Center (BIDMC) in Boston and include print, video, and educational components published in Annals of Internal Medicine.
Study Comparing Early Interventions for Sepsis Shows Patients Have Identical Outcomes
Sepsis can cause dangerously low blood pressure, which is typically treated with intravenous (IV) fluids and/or a vasopressor, a drug that causes constriction of the blood vessels. Whether treatment of sepsis-induced low pressure should primarily be treated with IV fluids or vasopressors has been debated for decades with no clear answer.
Gut bugs control the body’s thermostat
A new University of Michigan study reveals the gut microbiome’s role in regulating body temperature.
Sepsis and COVID-19 patients most at risk predicted with genetic model
A new model for understanding which patients with sepsis, Covid-19 and influenza have immune dysfunction and are more likely to suffer poor outcomes has been developed by researchers at the Wellcome Sanger Institute, the University of Oxford, Queen Mary University, Imperial College and their collaborators.
CYTOVALE REVEALS 10-MINUTE, 510(K) PENDING CYTOVALE SYSTEM AND INTELLISEP TEST FOR SEPSIS AT AACC 2022
Cytovale®, a medical diagnostics company focused on providing rapid and insightful tools to improve early detection of fast-moving and immune-mediated diseases, will reveal its 510(k) pending Cytovale system and 10-minute IntelliSep® sepsis risk stratification test at the American Association for Clinical Chemistry (AACC) annual meeting, where new data featuring the test will also be shared. The instrument can be seen in the Cytovale booth, no. 5045, in the exhibit hall during Clinical Lab Expo hours. The IntelliSep test was recently named an AACC Disruptive Technology Award Semifinalist and is also being featured in the Disruptive Tech area of the exhibit hall during the meeting.
New nanoparticles aid sepsis treatment in mice
Sepsis, the body’s overreaction to an infection, affects more than 1.5 million people and kills at least 270,000 every year in the U.S. alone. The standard treatment of antibiotics and fluids is not effective for many patients, and those who survive face a higher risk of death.
In new research, the lab of Shaoqin “Sarah” Gong at the University of Wisconsin–Madison reported a new nanoparticle-based treatment that delivers anti-inflammatory molecules and antibiotics.
Sanford Burnham Prebys awarded $13.5 million by NIH to investigate the pathogenesis and treatment of sepsis
Sanford Burnham Prebys professor Jamey Marth, Ph.D., has been awarded $13.5 million from the National Heart, Lung, and Blood Institute to continue his team’s work on sepsis, a condition that occurs when infectious and pathogenic organisms enter the bloodstream. This five-year award is a continuation of a multi-institution initiative, now totaling $27 million, that Marth began in 2016 with the goal of identifying the molecular basis of sepsis to achieve more effective treatments.
Hospital AI Learns to Say ‘I Don’t Know’
Sepsis occurs when the body works so hard to fight an infection that the immune system injures the patient’s own tissues. Detecting sepsis early and delivering antibiotics promptly is key to saving lives. UC San Diego Health researchers developed an…
MitoQ Antioxidant Prevents Sepsis-induced Diaphragm Weakness in Mice
Article title: Mitoquinone mesylate (MitoQ) prevents sepsis-induced diaphragm dysfunction Authors: Gerald S. Supinski, Elizabeth A. Schroder, Lin Wang, Andrew J. Morris, Leigh Ann P. Callahan From the authors: “This is the first study to show that mitoquinone mesylate (MitoQ), a…
What Makes Blood Vessels Leaky: New Insights for Sepsis Therapeutics
Lab studies reveal protein HSP27’s role in blood vessel leakage, opening the possibility that therapeutically dialing its activity up or down might stabilize patients with sepsis.
Early-warning system for sepsis shown to improve survival rates and cut hospital stays, new study finds
Emergency room patients who were flagged by an artificial intelligence algorithm for possibly having sepsis received antibiotics sooner and had better outcomes, according to a peer-reviewed study conducted by physician-researchers at Case Western Reserve University and MetroHealth.
Heparin-based Blood Purification Protects Baboon Kidneys in Severe Pneumonia, Sepsis
Article title: Heparin-based blood purification attenuates organ injury in baboons with S. pneumoniae pneumonia Authors: Lingye Chen, Bryan D. Kraft, Victor L. Roggli, Zachary R. Healy, Christopher W. Woods, Ephraim L. Tsalik, Geoffrey S. Ginsburg, David M. Murdoch, Hagir B.…

New grant-funded research could help improve therapies for sepsis
A University of Kentucky College of Medicine professor has been awarded a $1.9 million NIH grant for his research on the body’s immune response to sepsis, which could potentially help to improve therapies for the common disease.
Apes show dramatically different early immune responses compared to monkeys
A new study out of the University of Chicago and the University of Illinois Urbana-Champaign in humans, chimpanzees, rhesus macaques and baboons has found key differences in early gene expression in response to pathogen exposure, highlighting the importance of choosing the right animal model for the right questions.
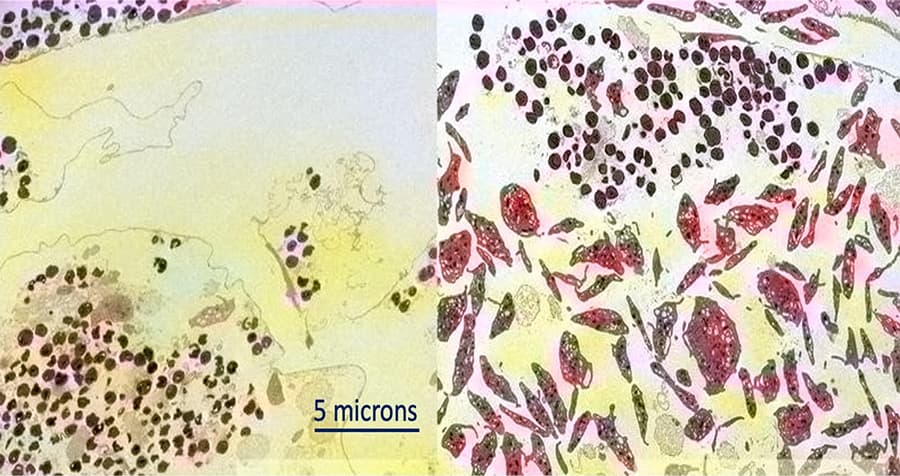
Repurposed Heart and Flu Drugs May Help Body Fight Sepsis
UC San Diego researchers discovered that patient survival from sepsis is associated with higher platelet counts, and identified two currently available drugs that protect these blood cells and improve survival in mice with sepsis.
Antibiotic-Resistant Strains of Staph Bacteria May Be Spreading Between Pigs Raised in Factory Farms and People in North Carolina
DNA sequencing of bacteria found in pigs and humans in rural eastern North Carolina, an area with concentrated industrial-scale pig-farming, suggests that multidrug-resistant Staphylococcus aureus strains are spreading between pigs, farmworkers, their families and community residents, and represents an emerging public health threat, according to a study led by researchers at the Johns Hopkins Bloomberg School of Public Health.
Researchers discover new particle in the blood of septic patients
Researchers at La Jolla Institute for Immunology (LJI) have found that people with sepsis have never-before-seen particles in their blood. The scientists are the first to show that these particles, called elongated neutrophil-derived structures (ENDS), break off of immune cells and change their shape as they course through the body.
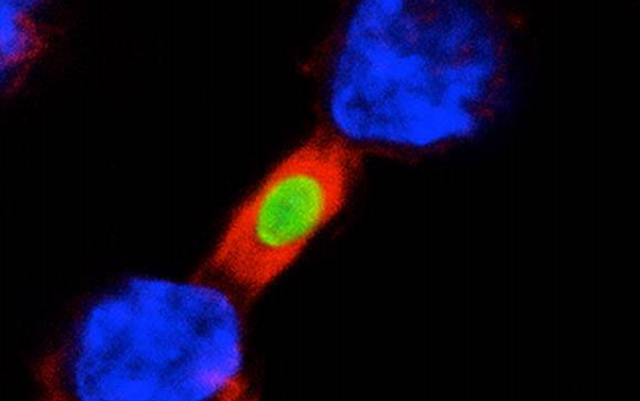
Protein that Keeps Immune System from Freaking Out Could Form Basis for New Therapeutics
Treatment with a peptide that mimics the naturally occurring protein GIV prevents immune overreaction and supports a mechanism critical for survival in mouse models of sepsis and colitis, according to a UC San Diego study.

Study reveals element in blood is part of human — and hibernating squirrel — stress response
A new study published in the journal Critical Care Explorations shows for the first time that part of the stress response in people and animals involves increasing the levels of a naturally circulating element in blood. The discovery demonstrates a biological mechanism that rapidly responds to severe physiologic stress and potentially serves to protect us from further damage due to life-threatening conditions.
Massachusetts Study Examines Relationships Between Staffing, Sepsis Rates
Sepsis rates at a sample of Massachusetts hospitals were significantly lower with increased nurse staffing and intensivist hours, according to new research published in the October issue of Critical Care Nurse.

New Version of AACN’s Critical Care Orientation Course Includes Stand-alone and Specialty-focused Options
The American Association of Critical-Care Nurses has released the latest version of its Essentials of Critical Care Orientation online course. Since its initial launch in 2002, ECCO has been used at more than 1,100 hospitals and healthcare facilities as an integral part of their critical care orientation or to supplement classroom-based education.
Early Steroids Improve Outcomes in Patients with Septic Shock
Some critically ill patients with septic shock need medications called vasopressors to correct dangerously low blood pressure. When high doses of vasopressors are needed or blood pressure isn’t responding well, the steroid hydrocortisone is often used. In this situation, earlier treatment with hydrocortisone reduces the risk of death and other adverse outcomes, reports a study in SHOCK®: Injury, Inflammation, and Sepsis: Laboratory and Clinical Approaches, Official Journal of the Shock Society. The journal is published in the Lippincott portfolio by Wolters Kluwer.
Patient Monitoring Systems for Sepsis – Mixed Results on Patient Outcomes
Automated patient monitoring systems (PMSs) have been designed to reduce delays in diagnosis of sepsis in hospitalized patients. But so far, studies evaluating these systems have shown inconsistent effects on mortality rates and other patient outcomes, according to an evidence review in a special September supplement to the Journal of Patient Safety, which was funded by the Agency for Healthcare Research and Quality (AHRQ). The journal is published in the Lippincott portfolio by Wolters Kluwer.
Implementation of an Evidence-Based, Nurse-Driven Sepsis Protocol to Reduce Acute Care Transfer Readmissions in the Inpatient Rehabilitation Facility Setting
The aim of this study was to determine if implementing an evidence-based, nurse-driven sepsis protocol would reduce acute care transfer (ACT) readmissions from an inpatient rehabilitation facility compared to nonprotocolized or usual standard of care for adult sepsis patients undergoing physical rehabilitation.

Too Much Haste Leads to Little Speed
Researchers at the La Jolla Institute for Immunology (LJI) have written a new first draft chapter in the book of immunology. They have discovered a protective biological switch that, briefly, turns on the immune response at the first whiff of an invader—an important feature—but can also turn off potentially destructive immune rampage that may also occur. This “off” switch can protect against serious, life threatening inflammation.
New Algorithm Tracks Pediatric Sepsis Epidemiology Using Clinical Data
Researchers at Children’s Hospital of Philadelphia (CHOP) have developed a novel computational algorithm to track the epidemiology of pediatric sepsis, allowing for the collection of more accurate data about outcomes and incidence of the condition over time, which is essential to the improvement of care.
Sepsis: Using Big Data to Cut a Killer Down to Size
Sepsis causes nearly 270,000 deaths in the United States each year. Find out how big data approaches are helping clinicians catch it sooner, treat it better, and help survivors cope with long-term effects.

UM School of Medicine’s Shock Trauma and Anesthesiology Research (STAR) Center Announces Leadership Transition
University of Maryland School of Medicine (UMSOM) Dean E. Albert Reece, MD, PhD, MBA, announced today that the UMSOM”s Shock, Trauma and Anesthesiology Research (STAR) Center will begin the next phase of its history with new leadership.

Vitamin C-B1-Steroid Combo Linked to Lower Septic Shock Mortality in Kids
Treating septic shock in children with a combination of intravenous vitamin C, vitamin B1 and hydrocortisone (a commonly used steroid) is associated with lower mortality, according to a study from Ann & Robert H. Lurie Children’s Hospital of Chicago. This is the first pediatric study of the safe and relatively inexpensive treatment for septic shock, and the preliminary data supports the promising outcomes seen in adults. Findings were published in the American Journal of Respiratory and Critical Care Medicine.
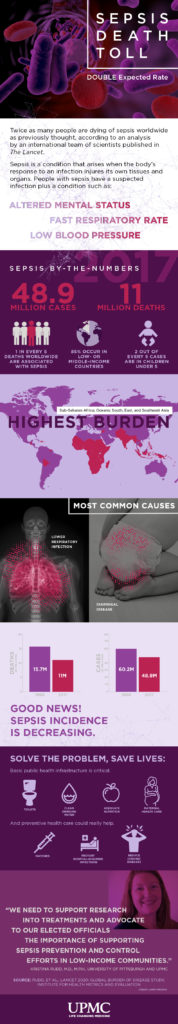
Sepsis Associated with 1 in 5 Deaths Globally, Double Previous Estimate
Twice as many people as previously believed are dying of sepsis worldwide, according to an analysis published today in The Lancet and announced at the Critical Care Reviews annual meeting in Belfast. Among them are a disproportionately high number of children in poor areas.
Finding a new way to fight late-stage sepsis
Researchers have developed a way to prop up a struggling immune system to enable its fight against sepsis, a deadly condition resulting from the body’s extreme reaction to infection.
For Patients with Sepsis, an Infectious Disease Expert May Reduce the Risk of Death
When people with severe sepsis, an extreme overreaction by the body to a serious infection, come to the emergency room (ER), they require timely, expert care to prevent organ failure and even death. When that care includes the early involvement of an infectious disease (ID) specialist, patient mortality can be reduced by as much as 40 percent, according to a new retrospective, single-center study published in Open Forum Infectious Diseases.
Antibody Improves Survival from Sepsis-Related Fungal Infections in Mice
An antibody that blocks the “programmed cell death” pathway may help the immune system fight off sepsis-related fungal infections, according to animal studies reported in SHOCK®: Injury, Inflammation, and Sepsis: Laboratory and Clinical Approaches, Official Journal of the Shock Society. The journal is published in the Lippincott portfolio by Wolters Kluwer.