Today, leaders from the American Society of Nephrology (ASN) will meet with their congressional delegations and call for their support of an $8 million increase for the Health Resources and Services Administration (HRSA) Organ Transplantation Program in FY 25 This funding, totaling $67 million, will be used to continue Congress’ commitment to people seeking a transplant and will implement reforms to modernize the transplant system and make transplant care more accessible.
Tag: Organ Transplant
Apply Today! Advance Media Registration for American College of Surgeons Clinical Congress
Members of the media can apply today to cover the American College of Surgeons Clinical Congress 2023.
The Medical Minute: Six organ donation facts knock down six myths
More than 100,000 people in the U.S. are awaiting new organs. Many won’t live long enough to get them. The new chief of transplant at Penn State Health Milton S. Hershey Medical Center debunks the myths that get between donors and recipients.
Livers have the potential to function for more than 100 years
There is a small, but growing, subset of livers that have been transplanted and have a cumulative age of more than 100 years.
Father’s Life is Saved after Receiving Heart, Kidney and Liver Transplant
After a rare disease caused organ failure, UC San Diego Heath transplant teams performed a heart, liver and kidney transplant on a patient. The surgery is a first for UC San Diego Health and a first in the nation to use three organs from a donor after circulatory death.
Children’s Hospital Los Angeles: The Best Care for Kids in California and the West Coast
U.S. News has again ranked CHLA as the top children’s hospital in California and in the survey’s Pacific U.S. region—which encompasses Alaska, California, Hawaii, Oregon and Washington. CHLA also made the publication’s annual Honor Roll of Best Children’s Hospitals for the 14th consecutive year—every year since its inception—finishing No. 8 in the United States in this showcase of the nation’s leading destinations for pediatric medical care.
Stanley C. Jordan, MD, Elected to Association of American Physicians
Stanley C. Jordan, MD, director of the Cedars-Sinai Nephrology and Transplant Immunology programs in the Cedars-Sinai Comprehensive Transplant Center, has been elected to the Association of American Physicians (AAP).
“Lungs in a Box” Now Offered at Northwestern Medicine
Due to COVID-19 and a rapidly expanding list of conditions for which lung transplantation can be lifesaving, the need for new organs is growing. However, there’s a global shortage of donated lungs, which results in numerous deaths among patients on the waitlist. To help expand the donor pool, Northwestern Medicine is now using a device from XVIVO called XPS™ which is used for ex vivo lung perfusion (EVLP) – nicknamed “lungs in a box” – to rescue potentially viable lungs and those initially deemed “unacceptable” for transplant. Out of all solid organs, lungs have the lowest utilization, with only one in five donated lungs getting transplanted.
Reducing lung transplant rejection aim of clinical trial funded with $22 million grant
Physicians at Washington University School of Medicine in St. Louis and Massachusetts General Hospital/Harvard Medical School in Boston have received a seven-year, $22 million grant from the National Institute of Allergy and Infectious Diseases (NIAID) of the National Institutes of Health (NIH) to help lead a multicenter clinical trial evaluating whether a novel immunosuppressant can reduce the risk of organ rejection after a lung transplant.
Lung Ventilation after Death May Keep Organs Healthy for Transplantation for Hours
Article title: Rapid postmortem ventilation improves donor lung viability by extending the tolerable warm ischemic time after cardiac death in mice Authors: Junyi Yu, Che Xu, Janet S. Lee, Jonathan K. Alder, Zongmei Wen, Guifang Wang, Agustin Alejandro Gil Silva,…
AMERICAN SOCIETY OF NEPHROLOGY CALLS ON BIDEN- HARRIS ADMINISTRATION TO INCREASE TRANSPLANT AVAILABILITY AND EQUITY
— The American Society of Nephrology (ASN) re- affirms its supporti for the Organ Procurement Organizations (OPOs) Conditions for Coverage final rule issued on November 20, 2020. The society calls for the Biden-Harris administration to implement this final policy as expediently as possible. By bringing objective and verifiable standards to assess the performance of OPOs, this final rule will increase the number of organs available for transplant and reduce racial inequity in the U.S. transplant system.
COVID-19 Outcomes for Patients on Immunosuppressive Drugs on Par with Non- Immunosuppressed Patients
People taking immunosuppressive drugs to prevent organ transplant rejection or to treat inflammatory or autoimmune diseases do not fare worse than others on average when they are hospitalized with COVID-19.

Lung, Heart, Kidney and Liver Transplant Programs Rank among Nation’s Best
UC San Diego Health’s lung, heart, kidney and liver transplant programs rank at the top nationally in the latest biannual Scientific Registry of Transplant Recipients (SRTR) report. Innovative treatment and multi-disciplinary care contribute to the high rankings for one-year survival outcomes.

Despite Pandemic, Cedars-Sinai on Track for Transplant Record
In a year rocked by the COVID-19 (coronavirus) pandemic, the Cedars-Sinai Comprehensive Transplant Center is on track to match or break records.
COVID-19 Found in The Cornea: Are Transplants a Transmission Risk?
A multi-institutional study finds that COVID-19 can be found in post-mortem corneal tissue, highlighting the importance of the donor screening process.
Does the New Heart Transplant Allocation Policy Encourage Gaming by Providers?
A new national policy was created to make determining who receives a heart transplant more fair. But new data shows it changed some practice patterns, too.
Are Organ Transplant Recipients at Greater Risk of Death from COVID-19?
A new study analyzes death risk from COVID-19 in organ transplant recipients and finds one treatment method greatly increased the risk.
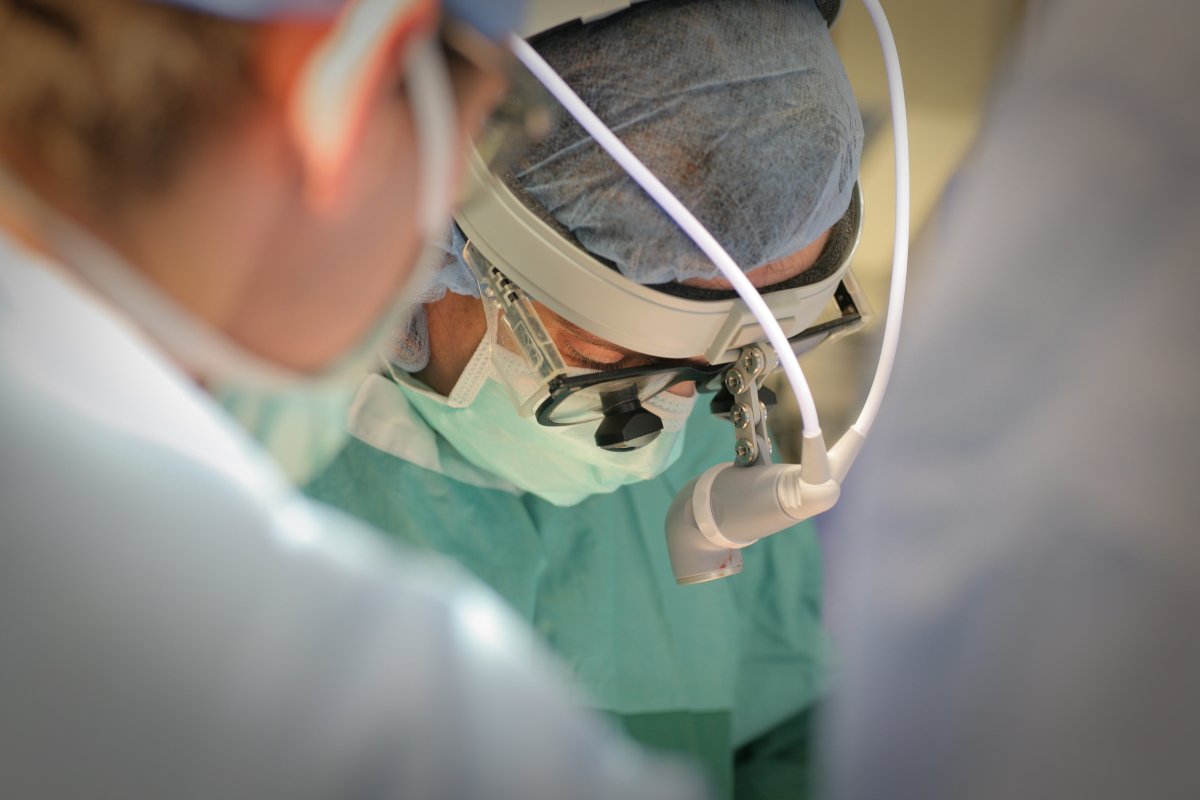
The Medical Minute: How COVID-19 has affected organ donation
With more than 109,000 people on the transplant waiting list nationwide, the need for organ donors remains great. A Penn State Health transplant surgeon explains how donors and recipients are kept safe during the COVID-19 pandemic.

Roswell Park Study: Delaying Antiviral Treatment May Boost Immunity in Stem Cell Transplant Recipients
Patients who develop cytomegalovirus infections after allogeneic stem cell transplantation may be able to develop an immunity against the virus, strengthen their immune system and reduce reliance on strong antiviral medications, a team from Roswell Park reports in the journal Biology of Blood and Marrow Transplantation.
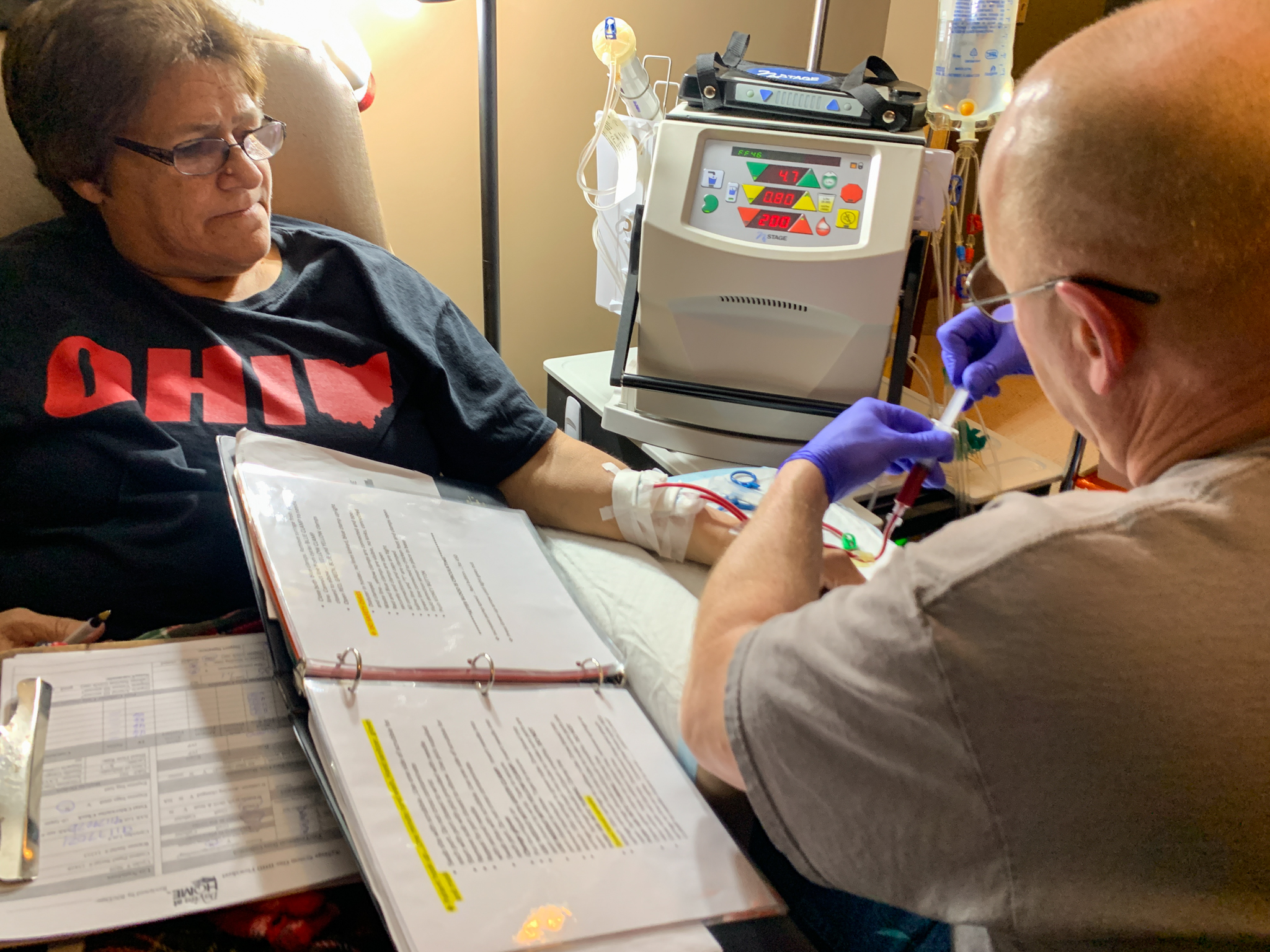
Study Finds Immune Cell That Predicts Risk of Organ Rejection In Transplant Patients
Researchers at The Ohio State University College of Medicine are the first to identify an immune cell that may predict a transplant patient’s risk of developing antibodies that can cause organ rejection. This discovery could lead to the development of therapies to prevent complications after transplant surgery.
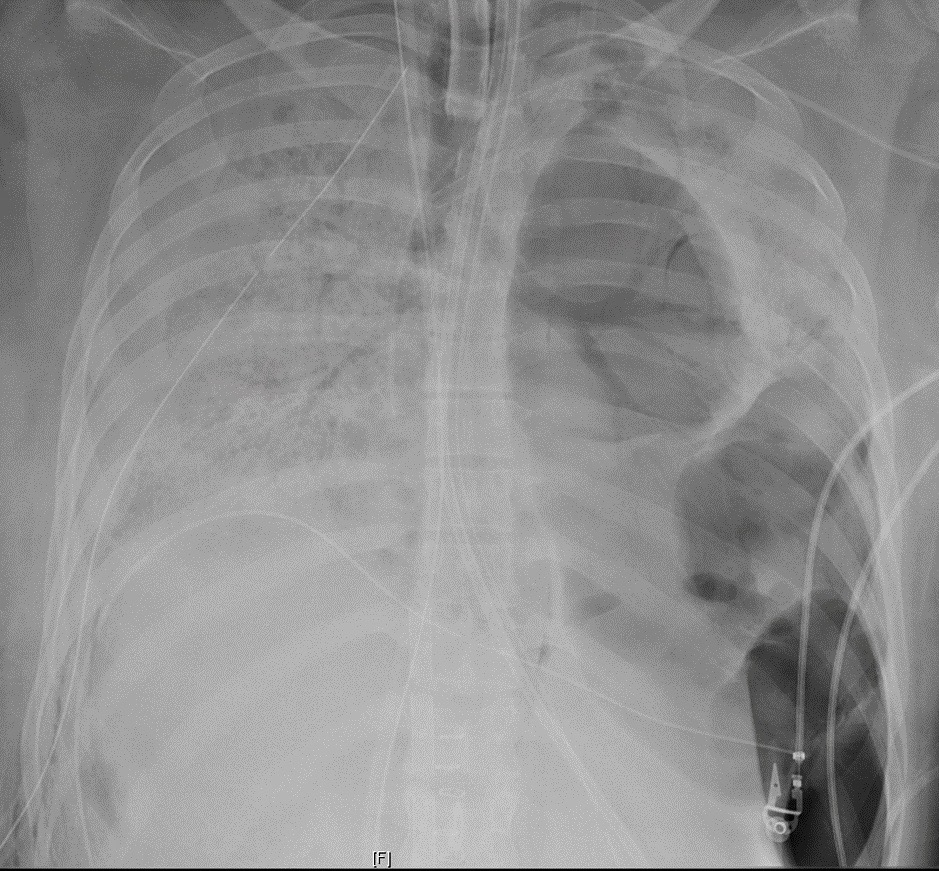
Lung Transplant Performed on a COVID-19 Patient at Northwestern Medicine
For the first time, surgeons at Northwestern Medicine performed a double-lung transplant on a patient whose lungs were damaged by COVID-19. The patient, a Hispanic woman in her 20s, spent six weeks in the COVID ICU on a ventilator and extracorporeal membrane oxygenation (ECMO), a life support machine that does the work of the heart and lungs.