Eric Martinez, MD, at Baylor Scott & White Health, discusses how living kidney donors can help those in need of a transplant. What You Need to Know: Risk factors that could lead to kidney transplant include high blood pressure and…
Tag: Transplant
Study: Black men may be less likely to receive heart transplant than white men, women
Black patients in need of a heart transplant may be less likely to receive one than white patients, according to a new study led by Indiana University School of Medicine researchers.
FDA Approves Semaglutide for Heart Disease Prevention
Last week, the U.S. Food and Drug Administration approved the drug semaglutide, commonly known as Wegovy or Ozempic, to be used to reduce the risk of cardiovascular death, heart attack and stroke in adults with heart disease and obesity. Eric…
Novel risk score for cardiovascular complications after bone marrow transplant
While lifesaving, bone marrow transplants can affect various organs, including the cardiovascular system. Researchers led by Michigan Medicine have not only determined the contemporary prevalence of cardiovascular complications after bone marrow transplant — they developed a novel tool to predict a person’s risk for such problems following the procedure and help guide the pre-transplant process.The work formed the basis of a scientific statement published by the American Health Association geared towards the cardiovascular management of patients undergoing bone marrow transplant.
Two Texas transplant programs team up to save lives
Two hard-to-match transplant patients 250 miles apart are starting 2024 on a new path to healthy lives.
Mount Sinai Researchers Receive $5 Million Gift From the Blavatnik Family Foundation to Expand Revolutionary Organ Perfusion Platform
The Mount Sinai Recanati/Miller Transplantation Institute has received a $5 million gift from the Blavatnik Family Foundation, pledged across five years.
Promising Kidney Transplant Solution Taps Expertise of Dr. Jim Lowe
In August, two U.S. surgical teams announced successful experimental kidney transplant from transgenic pigs into brain-dead human recipients. In both instances, the pig kidneys produced urine, carried out other functions of a kidney, and were not rejected by the body.
Partial Liver Transplants for Kids Key to Preventing Waitlist Deaths and Improving Outcomes
Dozens of children die each year in the U.S. while waiting for a new liver. A new analysis suggests that greater use of partial liver transplants — either from a living donor or by splitting a deceased donor’s liver for two recipients — could save many of these young lives.
U-M Health performs its first heart transplant after cardiac death
Transplant surgeons at the University of Michigan Health completed the health system’s first heart transplant using a donation after circulatory death, or DCD, heart. DCD transplants increased 68% in 2022.
Research May Speed Identification of Patients Who Need Liver Transplants
Simple blood measurement of a short-lived protein helped predict which patients would and wouldn’t likely survive without a liver transplant, according to a Rutgers study
UChicago Medicine celebrates 2022 transplant milestones
The University of Chicago Medicine liver transplant teams performed their 2,000th liver transplant in 2022, a milestone figure for the South Side academic medical center.
National Donor Day is February 14. Ochsner Health transplant surgeon available to discuss this significant day
Each year on February 14th, we recognize the importance of spreading awareness about organ, eye and tissue donation. With over 100,000 Americans currently waiting for organ donation, it is crucial that we provide education on the need for individuals to…
CMU Research Supported by PSC Wins Artificial Intelligence Award
Tuomas Sandholm’s work since 2010 to improve the fairness and effectiveness of organ donations using PSC supercomputers has won the 2023 AAAI Award for Artificial Intelligence for the Benefit of Humanity.
Penn Medicine Launches New Center for Living Donation to Increase Transplant Opportunities for Those in Need of Livers or Kidneys
The Penn Transplant Institute at Penn Medicine has opened a new Center for Living Donation which will expand Penn’s exceptional care for living donors, helping to maximize the number of lives saved through liver and kidney transplantation. For the thousands waiting on a lifesaving organ, living donation—when a living person donates an organ, or part of an organ, for transplantation to another person—can help those in need receive life-saving care sooner.
Father’s Life is Saved after Receiving Heart, Kidney and Liver Transplant
After a rare disease caused organ failure, UC San Diego Heath transplant teams performed a heart, liver and kidney transplant on a patient. The surgery is a first for UC San Diego Health and a first in the nation to use three organs from a donor after circulatory death.
Great Actions Leave a Mark campaign celebrates the Gift of Life through Living Organ Donation
UHN’s Ajmera Transplant Centre and The Centre for Living Organ Donation announce today the launch of a new campaign, Great Actions Leave a Mark, www.greatactions.ca. The campaign showcases through artistic photos and video, the stories and scars (the mark) from 39 living organ donors and transplant recipients across Canada.
Pediatric kidney transplant patients fare better when kidney is from live donor
Do pediatric kidney transplant patients have better long-term outcomes when their kidney comes from living, biologically unrelated donors compared to deceased donors? A new UC Davis Health study published in the journal Pediatric Transplantation finds that they do.
AMERICAN SOCIETY OF NEPHROLOGY STRONGLY SUPPORTS CONGRESSIONAL OVERSIGHT OF TRANSPLANT SYSTEM
The American Society of Nephrology (ASN) supports efforts by Congress to improve the US transplant system. Today, the Senate Finance Committee will conduct an oversight hearing, A System in Need of Repair: Addressing Organizational Failures of the U.S.’s Organ Procurement and Transplantation Network (OPTN).
Researchers Discover Mechanisms of Drug-Resistant Fungal Infection in Transplant Patient
Experts Encourage Rapid Genomic Screenings and Development of New Therapeutics for Drug-Resistant Pathogens to Address Emerging Global Health Concern
Mayo Clinic study confirms living kidney donor surgery is low risk for most patients
The risk of major complications for people who donate a kidney via laparoscopic surgery is minimal. That is the conclusion of a 20-year Mayo Clinic study of more than 3,000 living kidney donors. Only 2.5% of patients in the study experienced major complications, and all recovered completely.
“Lungs in a Box” Now Offered at Northwestern Medicine
Due to COVID-19 and a rapidly expanding list of conditions for which lung transplantation can be lifesaving, the need for new organs is growing. However, there’s a global shortage of donated lungs, which results in numerous deaths among patients on the waitlist. To help expand the donor pool, Northwestern Medicine is now using a device from XVIVO called XPS™ which is used for ex vivo lung perfusion (EVLP) – nicknamed “lungs in a box” – to rescue potentially viable lungs and those initially deemed “unacceptable” for transplant. Out of all solid organs, lungs have the lowest utilization, with only one in five donated lungs getting transplanted.
Expert Alert: 5 ways patients who are immunocompromised can protect themselves from COVID-19
As families prepare to gather later this month for Thanksgiving, it is important for patients who are immunocompromised to take extra steps to protect themselves from becoming infected with COVID-19. People who are immunocompromised have weakened immune systems, which means they have a higher risk of becoming severely ill from COVID-19.
World-first COVID vaccine booster randomized clinical trial in transplant patients proves third shot is very effective
The study enrolled 120 transplant patients between May 25th and June 3rd. None of them had COVID previously and all of them had received two doses of the Moderna vaccine. Half of the participants received a third shot of the vaccine (at the 2-month mark after their second dose) and the other half received placebo.
The primary outcome was based on antibody level greater than 100 U/ml against the spike protein of the virus. In the placebo group – after three doses (where the third dose was placebo), the response rate was only 18% whereas in the Moderna three-dose group, the response rate was 55%.
World-first COVID vaccine booster randomized clinical trial in transplant patients proves third shot is very effective
The study enrolled 120 transplant patients between May 25th and June 3rd. None of them had COVID previously and all of them had received two doses of the Moderna vaccine. Half of the participants received a third shot of the vaccine (at the 2-month mark after their second dose) and the other half received placebo. The primary outcome was based on antibody level greater than 100 U/ml against the spike protein of the virus. In the placebo group – after three doses (where the third dose was placebo), the response rate was only 18% whereas in the Moderna three-dose group, the response rate was 55%.
Vanderbilt Transplant Center Reaches New Record Number of Transplants Performed
The Vanderbilt Transplant Center performed a record number of solid organ transplants in fiscal year 2021 (FY 21) — 637 life-saving procedures among its adult and pediatric programs — despite occurring entirely during the COVID-19 pandemic.
Monoclonal antibody therapy for COVID-19 safe, effective for transplant patients
Treating transplant patients with mild to moderate cases of COVID-19 with monoclonal antibodies is safe and helps prevent serious illness, according to a Mayo Clinic study recently published in Open Forum Infectious Diseases. These results are especially important because transplant patients who are infected with COVID-19 have a higher risk of severe illness and death.
Announcing Virtual Press Conference for Experimental Biology 2021 Meeting
Reporters are invited to join a live Q&A discussion of exciting research announcements at the forefront of the life sciences during a virtual press conference for the Experimental Biology (EB) 2021 meeting. The press conference will be held online from 1–1:45 p.m. EDT on Monday, April 26, 2021 (RSVP by Friday, April 23).
Mount Sinai Surgeons Perform First Human Tracheal Transplant Surgery
Historic case launches Mount Sinai’s Tracheal Transplant Program for treating patients worldwide, including those with severe intubation damage after COVID-19
Reverse-order heart-liver transplant helps prevent rejection for highly sensitized patients
Patients with high levels of antibodies face major challenges getting a transplant. These highly sensitized patients have a higher risk of death while waiting for suitable organs. But there is new hope for highly sensitized patients in need of a combined heart and liver transplant, thanks to an innovative surgical approach at Mayo Clinic.
Researchers Identify Immune Cells that Contribute to Transplant Rejection
‘Tissue-resident memory T cells’, whose main function is to provide local protection against re-infection, contribute to chronic transplant rejection.
Vanderbilt University Medical Center Now Leads World in Heart Transplantation
Vanderbilt University Medical Center performed more heart transplants in 2020 than any other center in the world — 124 adult hearts, 23 pediatric hearts and VUMC’s first heart-lung transplant since 2006.

Lung, Heart, Kidney and Liver Transplant Programs Rank among Nation’s Best
UC San Diego Health’s lung, heart, kidney and liver transplant programs rank at the top nationally in the latest biannual Scientific Registry of Transplant Recipients (SRTR) report. Innovative treatment and multi-disciplinary care contribute to the high rankings for one-year survival outcomes.

Despite Pandemic, Cedars-Sinai on Track for Transplant Record
In a year rocked by the COVID-19 (coronavirus) pandemic, the Cedars-Sinai Comprehensive Transplant Center is on track to match or break records.
COVID-19 Found in The Cornea: Are Transplants a Transmission Risk?
A multi-institutional study finds that COVID-19 can be found in post-mortem corneal tissue, highlighting the importance of the donor screening process.

Synthetic Biology and Machine Learning Speed the Creation of Lab-Grown Livers
Researchers at the University of Pittsburgh School of Medicine have combined synthetic biology with a machine learning algorithm to create human liver organoids with blood and bile handling systems. When implanted into mice with failing livers, the lab-grown replacement livers extended life.
Does the New Heart Transplant Allocation Policy Encourage Gaming by Providers?
A new national policy was created to make determining who receives a heart transplant more fair. But new data shows it changed some practice patterns, too.
Mayo Clinic heart transplant program recognized for top patient outcomes
The Mayo Clinic heart transplant program in Arizona has been recognized as one of the top transplant programs in the U.S. based on quality and patient outcomes. The Scientific Registry of Transplant Recipients, a national medical database that evaluates solid organ transplantation in the U.S., has reported that the Mayo program has achieved the top long-term outcomes in the country.
Are Organ Transplant Recipients at Greater Risk of Death from COVID-19?
A new study analyzes death risk from COVID-19 in organ transplant recipients and finds one treatment method greatly increased the risk.

UI Health performs first-ever robotic kidney transplant for patient with polycystic kidney disease
Surgeons at UI Health — the University of Illinois Chicago’s clinical and academic health enterprise — have performed the world’s first robotic-assisted double-kidney removal followed immediately by a living-donor kidney transplant in a patient with severe polycystic kidney disease.
Study finds pioneering dual surgery a safe option for patients with polycystic kidney disease
Patients with large polycystic kidneys in need of a kidney transplant can have their diseased kidneys safely removed laparoscopically at the same time as their transplant surgery. That is the finding of a Mayo Clinic study recently published in the American Journal of Transplantation.

UC San Diego Health Revives Non-Beating Donor Heart for Successful Transplantation
UC San Diego Health is the first hospital on the West Coast to perform heart transplant surgery from a donor after circulatory death using a new portable organ care system. The investigational procedure could significantly decrease transplant waiting list times and improve patient outcomes.
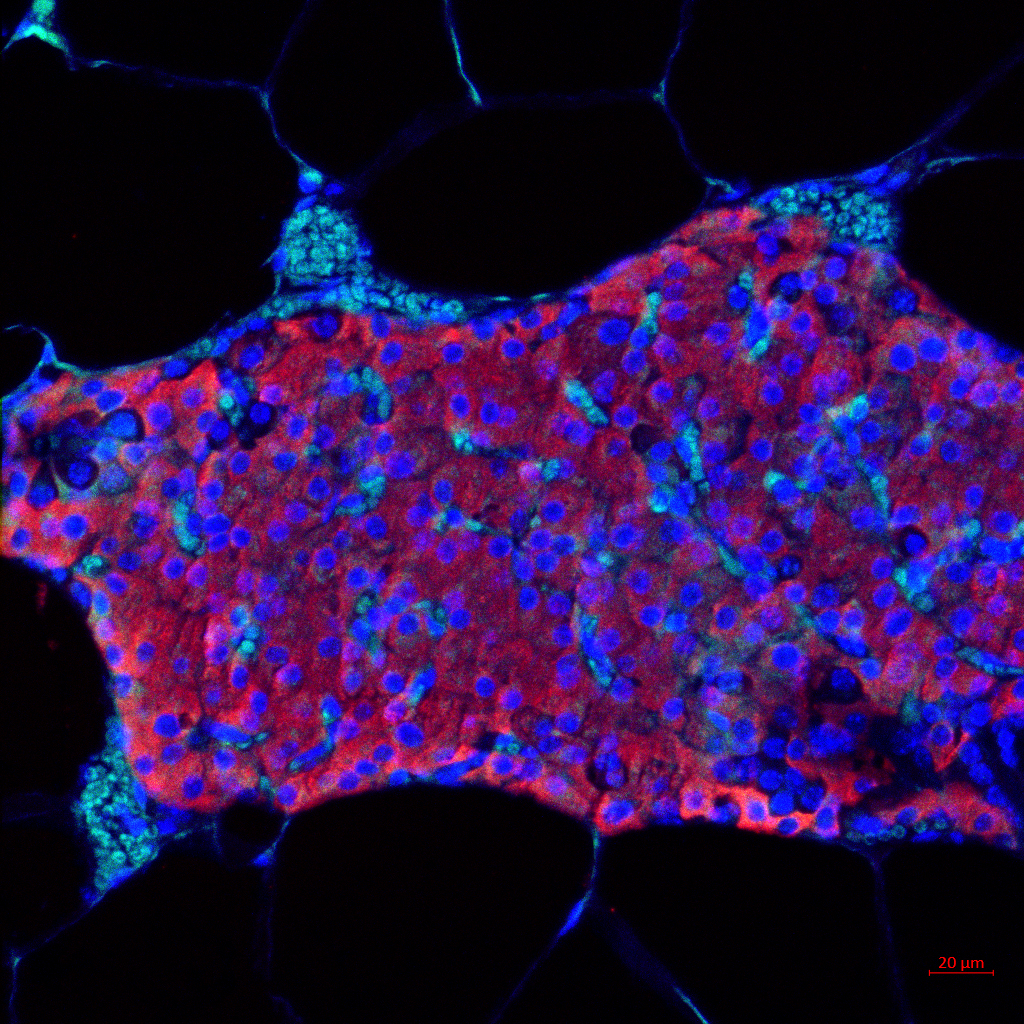
Microgel Immuno-acceptance Method Could Improve Pancreatic Islet Transplant Success
Researchers at the Georgia Institute of Technology and University of Missouri developed a new microgel drug delivery method that could extend the effectiveness of pancreatic islet transplantations — from several years to possibly the entire lifespan of a recipient.
How a Baby in Heart Failure Received a New Heart in the Midst of the Pandemic
A pandemic story with a happy ending. How a baby received a new heart after months of waiting amid the pandemic.

Division of Organ Transplantation at Hackensack University Medical Center Welcomes Two New Transplant Physicians
Two physicians — David Serur, M.D., and Vikram Wadhera, M.B. B.S. — have joined the surgical team at Hackensack Meridian Hackensack University Medical Center’s Division of Organ Transplantation.
Severely Damaged Human Lungs Can Now Be Successfully Recovered
A multidisciplinary team from Columbia Engineering and Vanderbilt University has now demonstrated that severely injured donor lungs that have been declined for transplant can be recovered outside the body by a system that uses cross-circulation of whole blood between the donor lung and an animal host. For the first time, a severely injured human lung that failed to recover using the standard clinical EVLP was successfully recovered during 24 hours on the team’s cross-circulation platform.
Study Finds Immune Cell That Predicts Risk of Organ Rejection In Transplant Patients
Researchers at The Ohio State University College of Medicine are the first to identify an immune cell that may predict a transplant patient’s risk of developing antibodies that can cause organ rejection. This discovery could lead to the development of therapies to prevent complications after transplant surgery.

Lab-Grown Miniature Human Livers Successfully Transplanted in Rats
Using skin cells from human volunteers, researchers at the University of Pittsburgh School of Medicine have created fully functional mini livers, which they then transplanted into rats. In this proof-of-concept experiment, the lab-made organs survived for four days inside their animal hosts.

Mimicking Cancer’s Evasive Tactics, Microparticles Show Promise Against Transplant Rejection
Inspired by a tactic cancer cells use to evade the immune system, University of Pittsburgh researchers have engineered tiny particles that can trick the body into accepting transplanted tissue as its own, while leaving the immune system intact.
Certain liver cells may help prevent organ rejection after transplant and other conditions, study finds
Mesenchymal stromal cells from fat tissue and bone marrow are widely used in therapeutic trials for their anti-inflammatory qualities, but new Mayo Clinic research finds that liver cells may be of greater value.
The study, published in Liver Transplantation, finds that liver mesenchymal stromal cells have immunoregulatory qualities that make them more effective than similar cells derived from adipose, or fat, tissue and bone marrow.

Living Liver Transplant Program to Increase Availability of Organs
Vanderbilt University Medical Center is launching a living liver donor transplant program, significantly increasing the number of available organs for life-saving transplants