A new study by Penn researchers examined, for the first time, the differences in lung transplant graft outcomes from organs recovered from the two types of deceased organ donor care facilities operating in the United States.
Tag: Lung Transplant

Cedars-Sinai Pulmonary and Critical Care Experts Present Latest Research at International Conference
Cedars-Sinai experts in pulmonology, critical care medicine and lung transplant attending the May 17-22 American Thoracic Society’s (ATS) 2024 International Conference in San Diego are available to comment on scientific advances being presented throughout the conference.
Baylor Scott & White Presents at ISHLT 44th Annual Meeting
The International Society of Heart and Lung Transplantation (ISHLT) 44th Annual Meeting is April 10-13 in Prague. Baylor Scott & White researchers will present the latest insights to better serve patients with end-stage heart and lung disease.Investigators at Baylor Scott &…
Lung Transplant Recipient’s Generous Donation Creates Rehabilitation Area for Patients Recovering from Transplant
Loyola Medicine recently celebrated the dedication of the Chris and Neil Blitstein Rehabilitation Track with a ribbon cutting ceremony at Loyola University Medical Center (LUMC).
Cleveland Clinic Researchers Develop New Model for Prioritizing Lung Transplant Candidates
CLEVELAND: A team from Cleveland Clinic has developed a new model for prioritizing patients waiting for a lung transplant, aimed at improving outcomes and reducing deaths among those in need of donor lungs. The new method offers an improved strategy for organ allocation by taking into account how the time a patient has spent on the waiting list could impact the severity of their disease and the urgency of their need for a transplant.
The results of a study looking at this new method were published today in The American Journal of Respiratory and Critical Care Medicine.
Clinical Outcomes of more than 500 Lung Transplants using Ex vivo Lung Perfusion: A Large-Volume, Single-Center Retrospective Analysis
To compare the outcomes of patients receiving lungs transplanted after undergoing ex vivo lung perfusion (EVLP) versus those transplanted conventionally at the Toronto General Hospital, Aadil Ali, PhD, and coauthors looked at 14 years of data from the Toronto Lung Transplant Database.
‘This Is Your Only Option’ — After COVID, Double Lung Transplant, University of Kentucky Patient Breathes Sigh of Relief
“The only way out of this is with new lungs.”
That’s what Andy Wilkins and his wife Michelle were told after Andy was hospitalized with COVID-19.
“Lungs in a Box” Now Offered at Northwestern Medicine
Due to COVID-19 and a rapidly expanding list of conditions for which lung transplantation can be lifesaving, the need for new organs is growing. However, there’s a global shortage of donated lungs, which results in numerous deaths among patients on the waitlist. To help expand the donor pool, Northwestern Medicine is now using a device from XVIVO called XPS™ which is used for ex vivo lung perfusion (EVLP) – nicknamed “lungs in a box” – to rescue potentially viable lungs and those initially deemed “unacceptable” for transplant. Out of all solid organs, lungs have the lowest utilization, with only one in five donated lungs getting transplanted.
16-Year-Old with Cystic Fibrosis Receives Double Lung Transplant, a First for Hassenfeld Children’s Hospital at NYU Langone
Hassenfeld Children’s Hospital at NYU Langone and the NYU Langone Transplant Institute reached a historic, first-ever milestone when surgeons replaced the lungs of a 16-year-old girl with cystic fibrosis.
Second Breath: Region’s First Double Lung Transplant for COVID-19 Patient
After more than 50 days on advanced life support, a multi-disciplinary team at UC San Diego Health helps a patient who contracted COVID-19 become a candidate for a successful double lung transplant. The transplant surgery was the first in the region performed on a COVID-19 patient.
Vanderbilt Transplant Center Reaches New Record Number of Transplants Performed
The Vanderbilt Transplant Center performed a record number of solid organ transplants in fiscal year 2021 (FY 21) — 637 life-saving procedures among its adult and pediatric programs — despite occurring entirely during the COVID-19 pandemic.
National Donor Day – Lung Transplant Recipient and Pulmonary Fibrosis Patient Available for Interview
This National Donor Day (Feb. 14), the Pulmonary Fibrosis Foundation (PFF) honors lung donors for their life-saving contributions while celebrating the priceless impact that lung transplantation makes on the lives of those with diseases like pulmonary fibrosis (PF). More than…

Lung, Heart, Kidney and Liver Transplant Programs Rank among Nation’s Best
UC San Diego Health’s lung, heart, kidney and liver transplant programs rank at the top nationally in the latest biannual Scientific Registry of Transplant Recipients (SRTR) report. Innovative treatment and multi-disciplinary care contribute to the high rankings for one-year survival outcomes.

Story Ideas from Johns Hopkins Medicine
During the COVID-19 pandemic, Johns Hopkins Medicine Media Relations is focused on disseminating current, accurate and useful information to the public via the media. As part of that effort, we are distributing our “COVID-19 Tip Sheet: Story Ideas from Johns Hopkins” every other Tuesday.
Finding a Personalized Approach To Treating Chronic Rejection After Lung Transplantation
By studying the roles of an inflammatory protein and antibodies in chronic rejection after lung transplantation, researchers discover possibilities for new treatments.
Study finds lung transplant patients not given antifungal preventive drugs have higher risk of death
Antifungal preventive medications reduce mortality risk by half in the first year following lung transplantation, according to Mayo Clinic research involving 667 patients who received lung transplants from 2005 to 2018.
Story Tips from Johns Hopkins Experts on COVID-19
As COVID-19 continues to impact the world, health care professionals are finding more patients who were diagnosed with the illness but still are dealing with symptoms long after the initial infection has gone. This condition is sometimes referred to as “long COVID.”

Remote, real-time monitoring of post-operative lung transplant patients significantly decreases hospital readmissions
To provide another layer of support for lung transplant recipients, the Keck Medicine of USC lung transplant team launched a two-year observational pilot study to monitor patients post-discharge using Bluetooth-enabled devices and computer tablets.
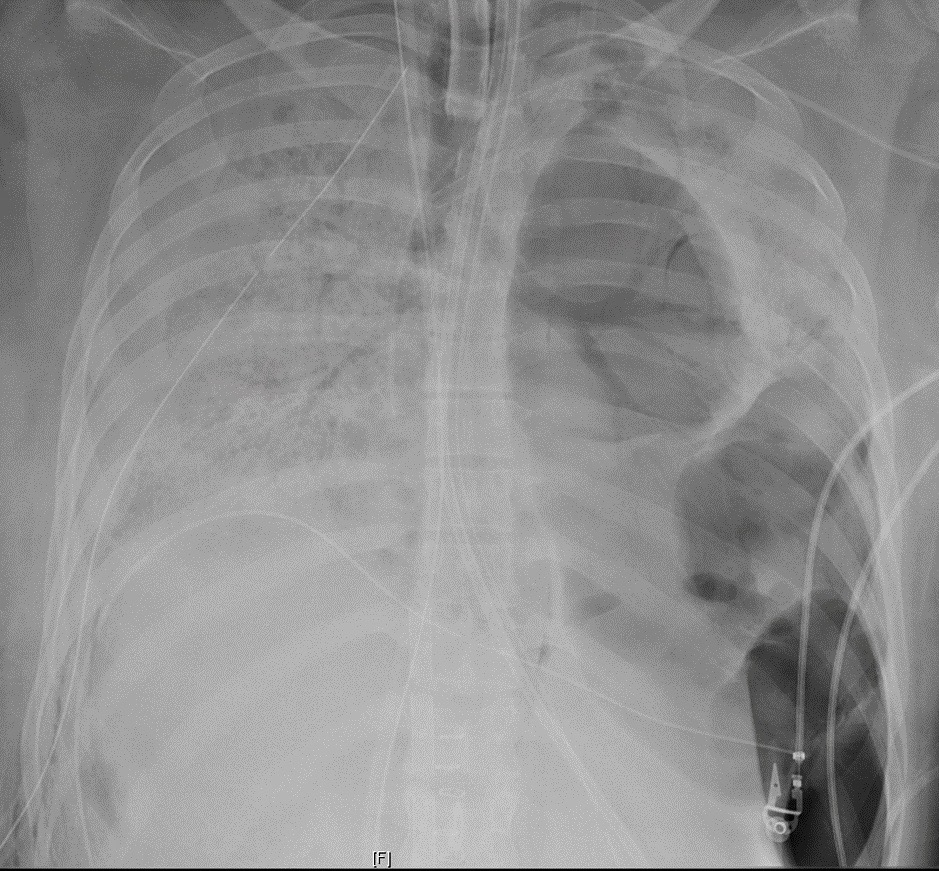
Lung Transplant Performed on a COVID-19 Patient at Northwestern Medicine
For the first time, surgeons at Northwestern Medicine performed a double-lung transplant on a patient whose lungs were damaged by COVID-19. The patient, a Hispanic woman in her 20s, spent six weeks in the COVID ICU on a ventilator and extracorporeal membrane oxygenation (ECMO), a life support machine that does the work of the heart and lungs.