A University of Chicago Medicine patient became the first in the world to receive the drug guselkumab (Tremfya) since its Sept. 11 approval by the FDA for treating moderate to severe ulcerative colitis.
Tag: IBD
Gut bioelectricity provides a path for bad bacteria to cause diseases
UC Davis Health researchers has discovered a novel bioelectrical mechanism pathogens like Salmonella use to find entry points in the gut lining that would allow them to pass and cause infection.
Oral Probiotic Delivers Colitis Treatment Directly to Gut in Multiple Animal Models
Article title: Oral administration of CXCL12-expressing Limosilactobacillus reuteri improves colitis by local immunomodulatory actions in preclinical models Authors: Emelie Öhnstedt, Cristian Doñas, Kristel Parv, Yanhong Pang, Hava Lofton Tomenius, Macarena Carrasco López, Venkata Ram Gannavarapu, Jacqueline Choi, Maria Ovezik, Peter Frank, Margareth…
New research points to ‘stem-like’ T cells as culprits in ulcerative colitis
The researchers hope to one day target this T cell population via drug therapy. “These cells may be a very important target for treating ulcerative colitis and perhaps other autoimmune diseases…”

The Rising Costs of Alcohol-Associated Liver Disease and More in the February Issue of AJG
A modeling study projecting the economic and social burden of alcohol-associated liver disease by 2040 is featured in the February 2024 issue of AJG, just one month after the new ACG Clinical Guideline on Alcohol-Associated Liver Disease
Inflammatory Bowel Disease Linked to Atopic Dermatitis, Penn Medicine Research Finds
Adults with atopic dermatitis (AD) have a 34 percent increased risk of developing new-onset inflammatory bowel disease (IBD) compared with individuals who do not have the skin condition, and children have a 44 percent increased risk, according to a new study from the Perelman School of Medicine at the University of Pennsylvania.

Digital Therapeutics and Innovations in GI Highlighted in the August Issue of AJG
The August issue of The American Journal of Gastroenterology includes several articles on digital therapeutics and innovations in GI, encouraging adoption of emerging GI technologies to advance GI care.
The Medical Minute: Crohn’s disease has no cure, but new treatments bring hope
Anyone newly diagnosed with Crohn’s disease probably has some anxiety about having a chronic ailment for which there’s no cure. A Penn State Health doctor talks about how treatments and medication offer reason for hope.

New gut calming discovery to bring relief to IBS sufferers
The discovery of a strain of bacteria shown to reduce inflammation in the intestine caused by irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD) could bring relief to millions of sufferers after being turned into an innovative natural food supplement by University of Bristol biotech spin-out Ferryx.
$2.9M NIH Grant to Study Genetics of IBD in Hispanic Population
Researchers at the University of Miami Miller School of Medicine were awarded a $2.9 million grant by the National Institutes of Health (NIH) to spend the next five years collecting and analyzing the genetic data of more than 3,000 Hispanic individuals, to better understand IBD in that community.
Financial assistance programs improve outcomes for indigent patients with inflammatory bowel disease
Patients with inflammatory bowel diseases (IBD) who required treatment and were enrolled in a financial assistance program were less likely to need surgery after starting medication than those not enrolled in a program, a study by UT Southwestern researchers found.
Mount Sinai Study Uncovers Mechanisms of Reactive Oxygen Species in Stem Cell Function and Inflammation Prevention
Mount Sinai researchers have published one of the first studies to demonstrate the importance of reactive oxygen species in maintaining stem cell function and preventing inflammation during wound repair, which could provide greater insights into the prevention and treatment of inflammatory bowel diseases (IBD), according to findings published in the journal Gut on October 3.
Smartphone App to Assess Stool Form, Rural-Urban Disparities in Cirrhosis Mortality, Lung Infection Risk in Severe Alcoholic Hepatitis in July Issue of AJG
The July issue of The American Journal of Gastroenterology highlights new clinical science including using a smartphone app to assess stool form, rural-urban disparities in cirrhosis mortality, and lung infection risk in severe alcohol-related hepatitis. This issue also includes articles on pediatric IBD, therapy options for Crohn’s disease, a novel endoscopic suturing device, proton pump inhibitors, and more.
Tipsheet: Cedars-Sinai Experts Share Research, Healthcare Innovations at Digestive Disease Week 2022
Cedars-Sinai physicians and scientists will share their latest advancements and research at Digestive Disease Week, known as DDW, an international scientific and clinical meeting featuring the work of physicians and researchers in gastroenterology, hepatology, endoscopy, and gastrointestinal surgery. DDW will take place May 21-24 in San Diego, California, and is available for virtual attendance.
McMaster scientists pinpoint key trigger of Crohn’s disease
Researchers gleaned their results by analyzing blood and biopsy samples from two groups totalling 18 people with Crohn’s disease, comparing them to a matching number of people from two healthy control groups. A mouse model of IBD was also used. Khan said his study was the first demonstration of the interaction between serotonin, autophagy and gut microbiota in intestinal inflammation. The paper was published by Science Advances today. Sabah Haq, a PhD student who works with Khan, is first author.
New Clinical Advances in Gastroenterology Presented at the American College of Gastroenterology’s 86th Annual Scientific Meeting
Featured science includes increased incidence of pancreatic cancer among young women, quality of life improvements in IBD, colorectal cancer risk from weight loss surgery and medications, and more
Novel mechanism links genetic defect in IBD patients to gut leakiness
A team of researchers led by a biomedical scientist at the University of California, Riverside, has identified a novel mechanism by which loss-of-function mutations in the gene PTPN2, found in many patients with inflammatory bowel disease, or IBD, affect how intestinal epithelial cells maintain a barrier.
Study Finds COVID-19 Vaccines Safe for IBD Patients
Patients with inflammatory bowel diseases (IBD) do not appear to have increased risk of side effects from the Pfizer or Moderna COVID-19 vaccines, according to a recent Cedars-Sinai study published online and upcoming in print in the American Journal of Gastroenterology. In fact, those being treated with advanced immune-modifying therapies may experience them less often than the general population.
‘Good’ Bacteria Show Promise for Clinical Treatment of Crohn’s Disease, Ulcerative Colitis
A new study published in Nature Communications demonstrates that a consortium of bacteria designed to complement missing or underrepresented functions in the imbalanced microbiome of inflammatory bowel disease (IBD) patients, prevented and treated chronic immune-mediated colitis in humanized mouse models.
Inflammatory Bowel Disease Impairs Artery Function in GI Tract
Article title: Role of perivascular nerve and sensory neurotransmitter dysfunction in inflammatory bowel disease Authors: Charles E. Norton, Elizabeth A. Grunz-Borgmann, Marcia L. Hart, Benjamin W. Jones, Craig L. Franklin, Erika M. Boerman From the authors: “Our study is the…
Irritable Bowel Syndrome: Mark Pimentel, MD
Irritable bowel syndrome (IBS) is the most common gastrointestinal disorder, affecting 10-15% of the world’s population. Approximately two-thirds of those who suffer from IBS are women. The disease can have mild forms or cause severe debilitation as diarrhea alternates with constipation. Severe cramping and bloating also are common. Because chronic IBS is so debilitating, it often disrupts the daily lives of people with this disorder.
Study Reveals Details of Immune Defense Guidance System
At the beginning of an immune response, a molecule known to mobilize immune cells into the bloodstream, where they home in on infection sites, rapidly shifts position, a new study shows. Researchers say this indirectly amplifies the attack on foreign microbes or the body’s own tissues.
Surgery to Heal Inflamed Gut May Create New Target for Disease
A surgical procedure meant to counter ulcerative colitis, an immune disease affecting the colon, may trigger a second immune system attack, a new study shows.
Multi-Population Risk Scores Could Improve Risk Prediction for Inflammatory Bowel Diseases, Study Finds
New study illustrates how studying diverse populations can help predict patient outcomes and reduce health disparities

University of Miami Health System Gastroenterologist Honored with ‘Lifetime Disruptor’ Award
Maria T. Abreu, M.D., a renowned gastroenterologist at the University of Miami Miller School of Medicine, was honored with the “Lifetime Disruptor” award at the American College of Gastroenterology’s 2020 virtual meeting.
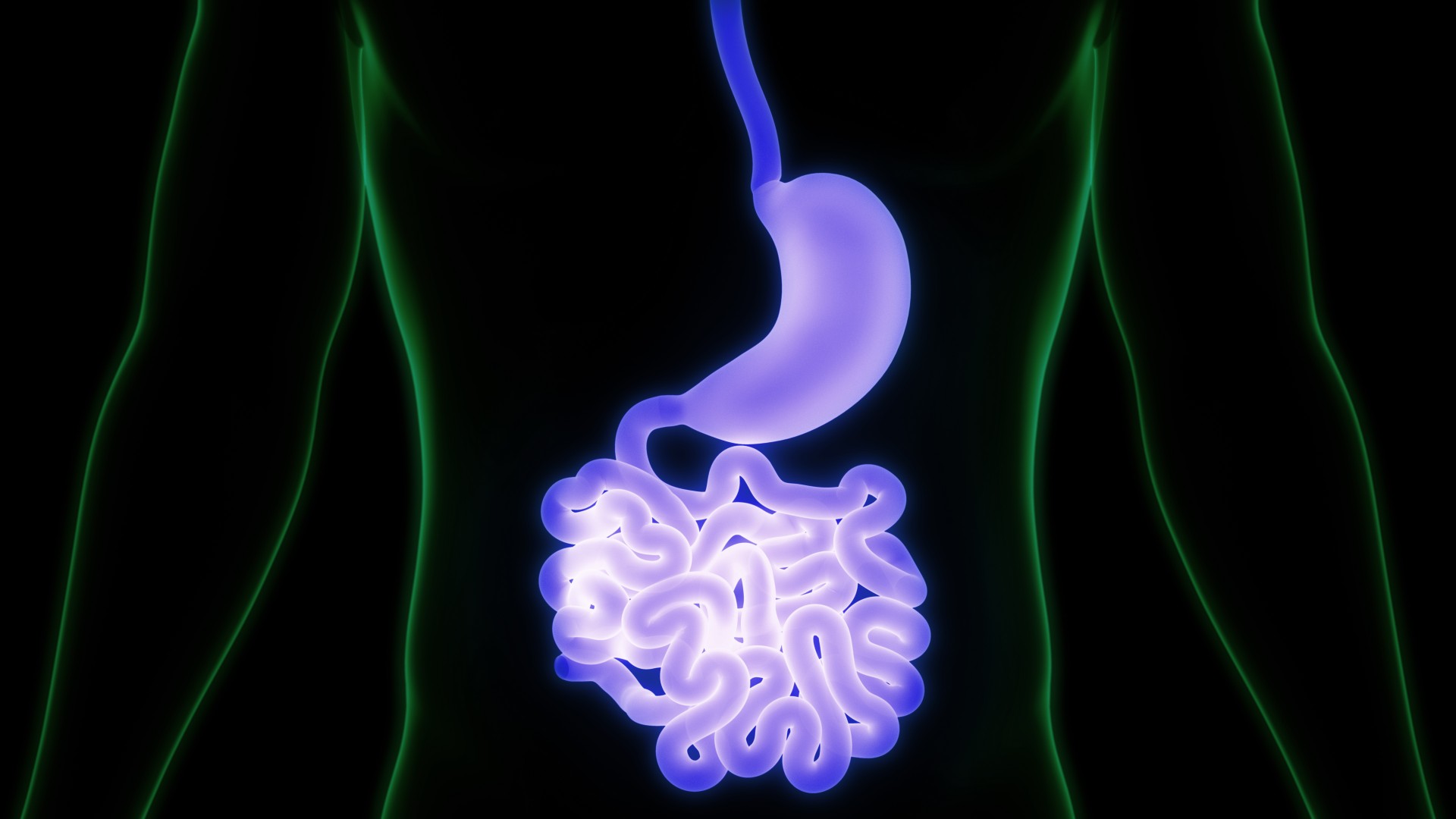
Genetic Risk for Fatal Blood Clots Identified in IBD Patients
Blood clots are the biggest cause of death in patients with inflammatory bowel disease (IBD) ─ ulcerative colitis or Crohn’s disease. In a retrospective study recently published in the journal Gastroenterology, Cedars-Sinai investigators found that a combination of rare and common genetic variants in some IBD patients significantly increased their risk of developing clot-causing thromboembolic diseases.
CHOP Genomic Study Reveals Role for Hypothalamus in Inflammatory Bowel Disease
Using sophisticated 3D genomic mapping and integrating with public data resulting from genome-wide association studies (GWAS), researchers at Children’s Hospital of Philadelphia (CHOP) have found significant genetic correlations between inflammatory bowel disease (IBD) and stress and depression. The researchers went on to implicate new genes involved in IBD risk that are enriched in both derived hypothalamic neurons, from a part of the brain that has a vital role in controlling stress and depression, and organoids derived from colon cells, a region more commonly studied in the context of IBD.
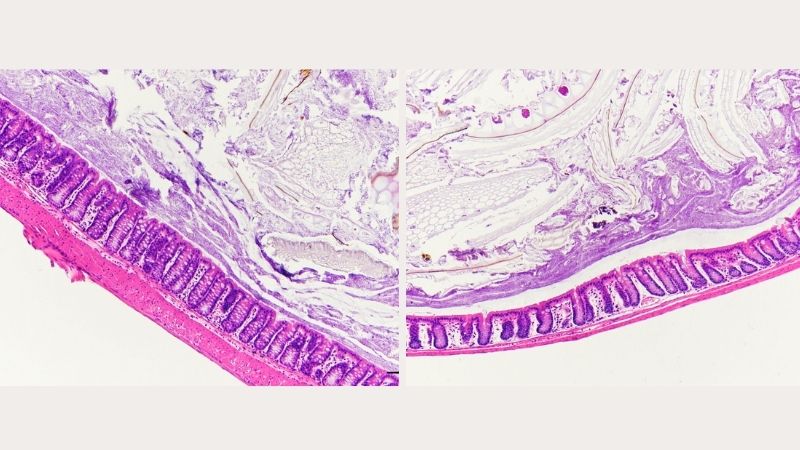
High-Sugar Diet Can Damage The Gut, Intensifying Risk For Colitis
DALLAS – Oct. 28, 2020 – Mice fed diets high in sugar developed worse colitis, a type of inflammatory bowel disease (IBD), and researchers examining their large intestines found more of the bacteria that can damage the gut’s protective mucus layer.
Resilience-Driven Care for Inflammatory Bowel Disease Leads to Sharp Drops in Emergency Room Visits and Hospitalizations
A personalized program to increase resilience in patients with inflammatory bowel disease (IBD) can substantially reduce hospitalizations and emergency room visits, Mount Sinai researchers report. The research is being unveiled on October 27th in a plenary presentation at the annual scientific meeting of the American College of Gastroenterology (ACG 2020).

Medical Mystery: ‘Creeping Fat’ in Crohn’s Patients Linked to Bacteria
Cedars-Sinai researchers might have solved a mystery surrounding Crohn’s disease: Why does fat appear to migrate into patients’ small intestines?
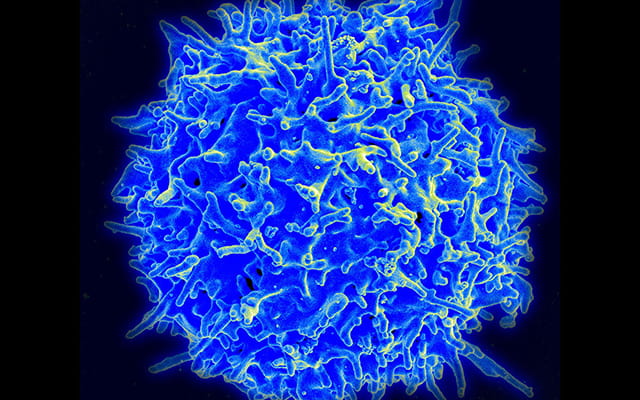
Inflammatory Bowel Disease Linked to an Immune Cell Run Amok
Researchers at UC San Diego School of Medicine report that the lasting nature of inflammatory bowel disease may be due to a type of long-lived immune cell that can provoke persistent, damaging inflammation in the intestinal tract.
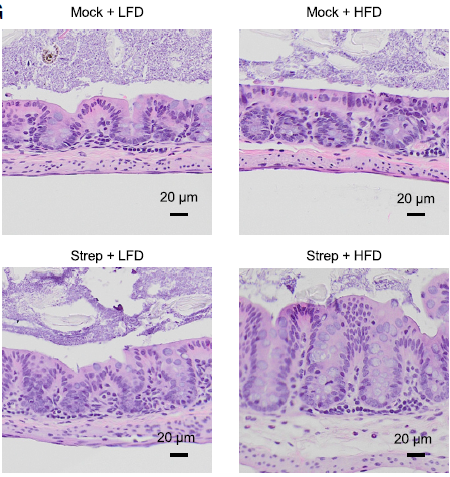
High-fat diet with antibiotic use linked to gut inflammation
UC Davis researchers have found that combining a Western-style high-fat diet with antibiotic use significantly increases the risk of developing pre- inflammatory bowel disease. This combination shuts down the mitochondria in cells of the colon lining, leading to gut inflammation. Mesalazine can help restart the mitochondria and treat pre-IBD condition.
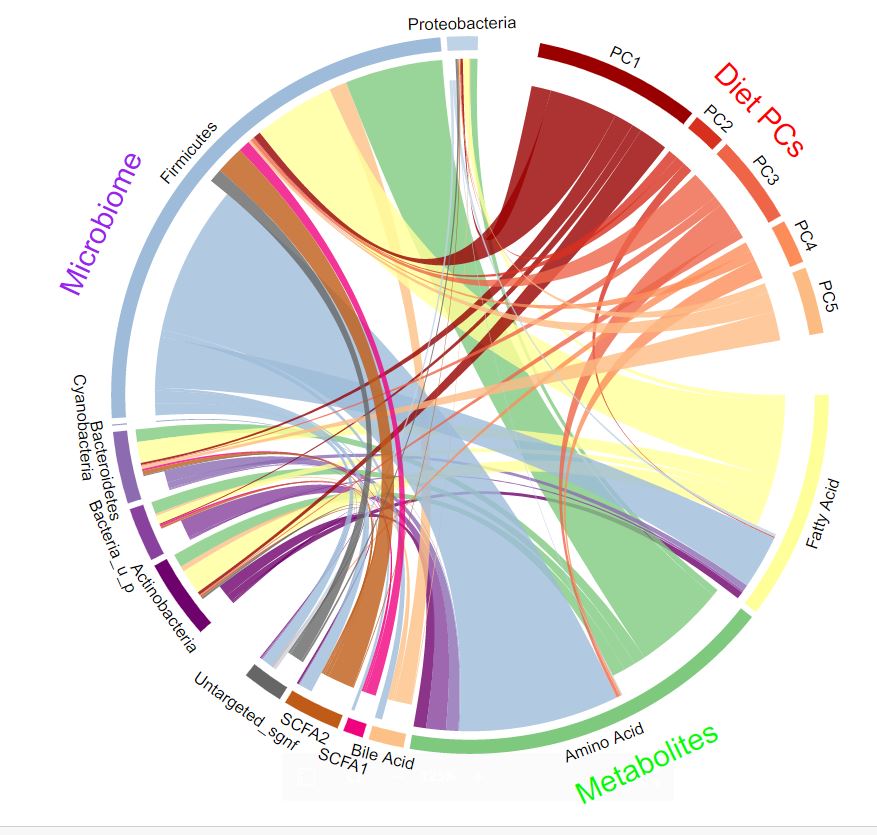
University of Miami Study Finds Dietary Changes May Help People with Ulcerative Colitis
A new study published in Clinical Gastroenterology and Hepatology led by Maria T. Abreu, M.D., professor of medicine and professor of microbiology and immunology at the University of Miami Miller School of Medicine, found that eating diets low in fat and high in fiber may improve the quality of life of patients with ulcerative colitis (UC) — even those in remission.
Could the Cure for IBD Be Inside Your Mouth?
A new study describes how poor oral health may worsen gut inflammation.

Yes, inflammatory bowel disease and celiac disease are linked
A systematic review and meta-analysis has determined there is a nine-fold increased risk of having IBD for patients with a previous diagnosis of celiac disease. Similarly, the risk for celiac disease is increased in IBD patients, though to a smaller extent.
Mount Sinai Researchers Unveil Mechanisms to Prevent Crohn’s Disease and First Study Linking Metals Exposure w/ IBD
In a series of four studies published today in Gastroenterology, a journal of the American Gastroenterological Association, Mount Sinai inflammatory bowel disease (IBD) researchers, describe the identification of predictive tools and a new understanding of environmental factors that trigger IBD.

Case Western Reserve University researchers discover critical link to controlling inflammation in Crohn’s disease
Investigators at the Case Western Reserve University School of Medicine discovered that blocking interleukin-1α (IL1α), a protein that controls inflammation in the gut, markedly decreases the severity of intestinal inflammation in a mouse model of Crohn’s disease (CD).
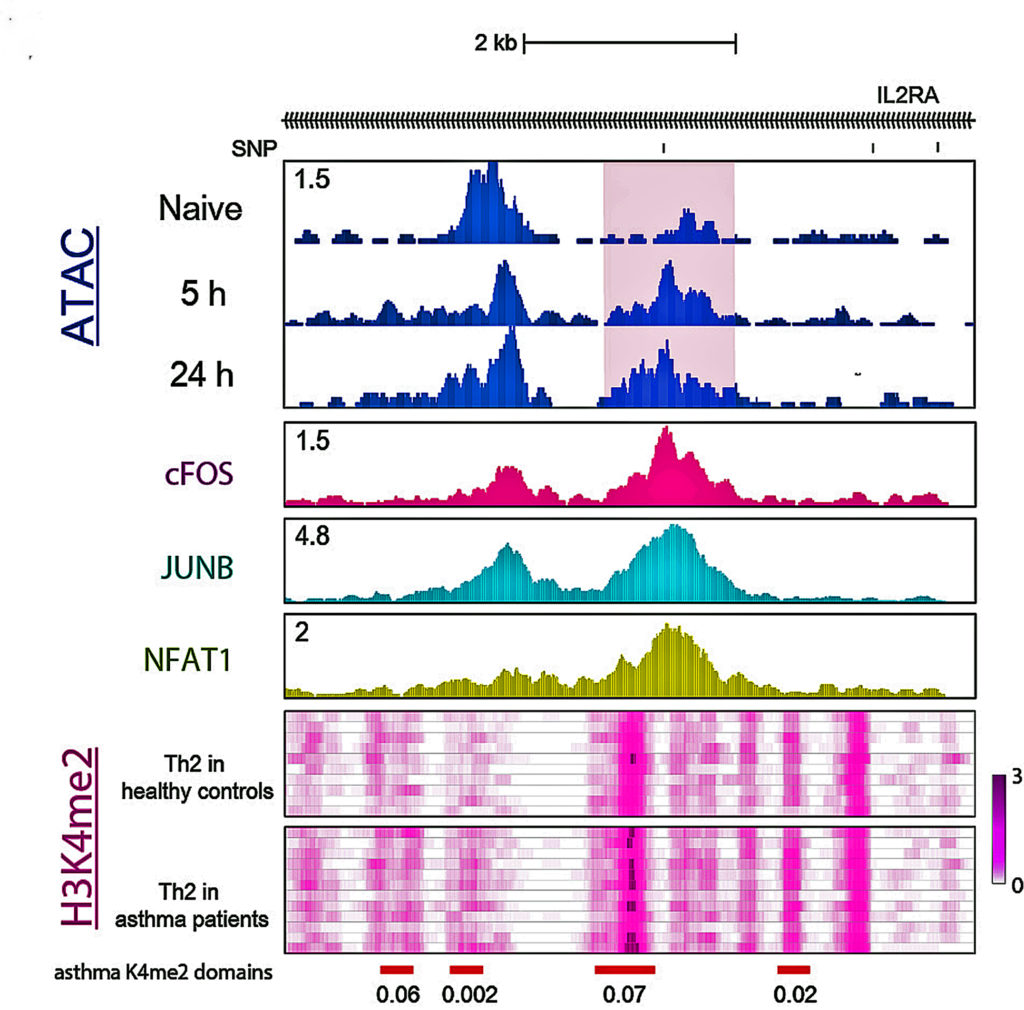
Scientists Find Molecular Key to Body Making Healthy T Cells
In a finding that could help lead to new therapies for immune diseases like multiple sclerosis and IBD, scientists report in the Journal of Experimental Medicine identifying a gene and family of proteins critical to the formation of mature and fully functioning T cells in the immune system.