An increase in nightmares and hallucinations could signal the onset of autoimmune diseases such as lupus, according to a new study.
Tag: Lupus
Atlantic Health System Enrolls First U.S. Patient in Lupus Treatment Trial
NJ-based Atlantic Health System is the first in the U.S. to enroll a patient in a study to examine the effectiveness of using Chimeric Antigen Receptor (CAR- T) cells in the treatment of the autoimmune disease lupus.
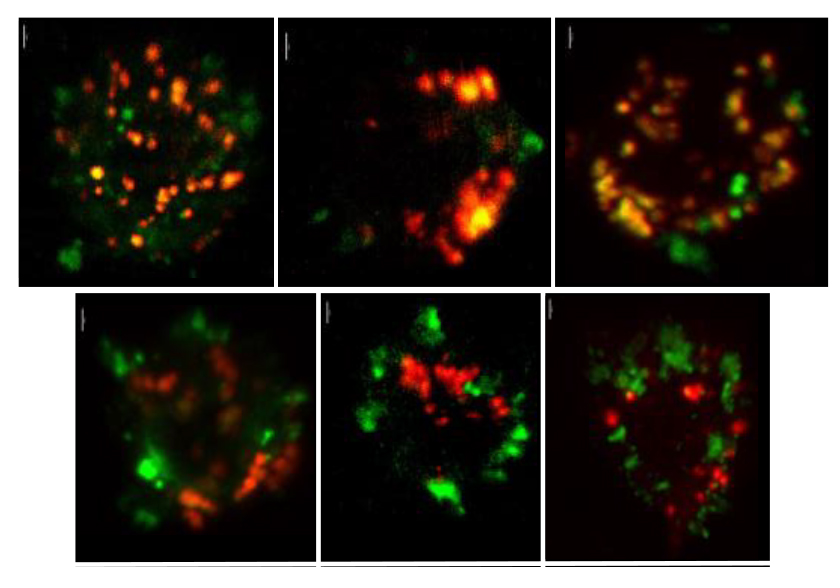
Study identifies new pathway to suppressing autoimmunity
Researchers at Stanford University School of Medicine, Yale University School of Medicine, and the Hospital for Special Surgery Research Institute have uncovered new details about how the immune system prevents the production of antibodies that can recognize and damage the body’s own, healthy tissues. The study, to be published September 29 in the Journal of Experimental Medicine (JEM), also reveals how this process is impaired in autoimmune disorders such as systemic sclerosis and systemic lupus erythematosus and suggests potential new strategies to treat these diseases.
Researchers ID Kidney Pathway Involved with Autoimmune-related Hypertension in Female Mice
Article title: Renal TLR-7/ TNF-α pathway as a potential female-specific mechanism in the pathogenesis of autoimmune-induced hypertension Authors: Sarika Chaudhari, Bradley M. D’Souza, Jessica Y. Morales, Cassandra M. Young-Stubbs, Caroline G. Shimoura, Rong Ma, Keisa W. Mathis From the authors:…
American College of Rheumatology Educating Dermatologists and Nephrologists on Lupus Clinical Trials Racial Disparities
The American College of Rheumatology (ACR) has released Continuing Medical Education (CME) for dermatologists and nephrologists to help them learn more about clinical trials for lupus patients in their treatment areas and the importance of getting more of African American/Black patients enrolled.
Media Briefing Schedule for ACS Fall 2022
Media Briefing Schedule for ACS Fall 2022
Lupus pill shows promise in mice; clinical trial underway
There’s no cure for lupus, an autoimmune disease that attacks organs. But today, scientists report they have begun phase 2 clinical trials with a pill containing a compound that, in mice, reverses organ damage and prevents death. They will present their results at ACS Fall 2022.
Pathway uncovered for greatest lupus genetic risk factor, study shows
Researchers at Michigan Medicine have uncovered the enigmatic mechanism that genetically predisposes people to the worst effects of the most typical form of lupus, a study suggests. Researchers say the findings could potentially facilitate the discovery of safe, simple and effective treatments.
Patients with Lupus Benefit from COVID-19 Vaccine Booster
People with systemic lupus erythematosus, or SLE, who received a “booster” dose of SARS-CoV-2 vaccine after full vaccination are roughly half as likely to have a subsequent “breakthrough” COVID-19 infection, a new study shows.
Study Underscores Importance of Multidisciplinary Medical Team for Pregnant Women with Lupus
A study that includes researchers at Hospital for Special Surgery (HSS) underscores the importance of a multidisciplinary medical team to counsel and provide care for women with systemic lupus erythematosus, the most common form of lupus, who become pregnant. Using a nationwide database, the investigators reviewed the records of more than 50,000 patients with lupus who gave birth over a 10-year period. Findings revealed a higher rate of fetal morbidity and severe maternal morbidity compared to women who did not have lupus.
Mount Sinai Microbiome Lab Joins NIH’s Accelerating Medicines Partnership
The National Institutes of the Health (NIH) has awarded researchers at the Icahn School of Medicine at Mount Sinai a four-year grant to study the role of the human microbiome in rheumatoid arthritis, systemic lupus, and other autoimmune diseases. The grant is part of the NIH’s Accelerating Medicines Partnership® Autoimmune and Immune-Mediated Diseases (AMP® AIM) program, which is designed to speed the discovery of new treatments and diagnostics. It will support the Microbiome Technology and Analytic Center Hub (Micro-TEACH), a multidisciplinary team of researchers at Icahn Mount Sinai and NYU Langone Health.
Research Reveals Racial and Ethnic Disparities Persist in Pregnancy Outcomes of Patients with Lupus
While investigators have known that maternal and fetal outcomes of pregnancy among women with systemic lupus erythematosus (SLE) have improved over time, it is unknown whether the improved outcomes are shared equally among different racial and ethnic groups. Lupus has been shown to disproportionately affect minorities of childbearing age. A new study that includes researchers from Hospital for Special Surgery (HSS) presented today at the American College of Rheumatology (ACR) annual meeting shows that pregnancy outcomes in women with lupus have improved in all racial and ethnic groups over the past decade, but disparities still exist.
Study Finds Racial Gaps in Renal Complications Persist for Children with Lupus
New research presented this week at ACR Convergence, the American College of Rheumatology’s annual meeting, found that while hospitalized children with juvenile lupus have fewer adverse kidney outcomes overall, significant racial gaps for developing these complications persist and do not seem to be narrowing (Abstract #0956).
Nearly One Third of Lupus Patients in One Study Had Low Responses to COVID-19 Vaccines
New research presented this week at ACR Convergence, the American College of Rheumatology’s annual meeting, shows that nearly 30% of patients with lupus in a multi-ethnic and multi-racial study had a low response to the new COVID-19 vaccines.
Hydroxychloroquine, Mainstay Lupus Treatment, Not Associated With Serious Cardiac Complication
New research presented this week at ACR Convergence, the American College of Rheumatology’s annual meeting, shows that hydroxychloroquine does not appear to be associated with QTc interval prolongation.
NYU Langone Presentations at American College of Rheumatology Convergence 2021 to Address Vaccine Efficacy and High-risk Pregnancy
NYU Langone rheumatologists are presenting their discoveries at the annual American College of Rheumatology conference, November 1 to November 9. The conference will be held virtually.
Evaluation of lupus arthritis using frequency domain optical imaging
Systemic lupus erythematosus (SLE), commonly referred to as simply “lupus”, is an autoimmune disorder where the body’s immune system attacks healthy tissue.
Newly Approved Lupus Drug Based on Discoveries Made in HSS Lab
The US Food and Drug Administration approved the drug anifrolumab (Saphnelo) on August 2, 2021 for the treatment of adult patients with moderate to severe systemic lupus erythematosus (SLE) who are receiving standard therapy. Much of the groundwork for the development of this drug was done in laboratories at Hospital for Special Surgery (HSS) in the early 2000s.
AARDA Approved for a $97,498 Engagement Award for Stakeholder Convenings
The American Autoimmune Related Diseases Association (AARDA) has been approved for a $97,498 funding award through the Eugene Washington PCORI Engagement Awards program, an initiative of the Patient-Centered Outcomes Research Institute (PCORI).
Research News Tip Sheet: Story Ideas from Johns Hopkins Medicine
During the COVID-19 pandemic, Johns Hopkins Medicine Media Relations is focused on disseminating current, accurate and useful information to the public via the media. As part of that effort, we are distributing our “COVID-19 Tip Sheet: Story Ideas from Johns Hopkins” every other Wednesday.

Helping Childhood-Onset Lupus Patients Stay Healthy As Adults
DALLAS – March 30, 2021 – UT Southwestern researchers have identified factors that put patients with childhood-onset lupus at elevated risk for poor outcomes, such as end-stage renal disease or death, as they transition from pediatric to adult health care. The findings, published online in Seminars in Arthritis and Rheumatism, emphasize the precarious nature of this period and shine a spotlight on areas prime for intervention to help protect these vulnerable patients.
Research Group Identifies Potential Therapeutic Target for Lupus
Inhibiting IRE1α, a molecule activated by the endoplasmic reticulum in neutrophils, counters disease progression in lupus mice.
Cross-Country Research Collaboration Brings First Ever Lupus Estimates
A meta-analysis of lupus finds the disease is less common than previously thought, but disproportionally affects women and racial and ethnic minorities of both sexes.
STUDY PINS DOWN NUMBER OF AMERICANS WITH MOST COMMON FORM OF LUPUS
Just over 200,000 Americans suffer from systemic lupus erythematosus, or SLE, a condition in which the body’s immune system mistakenly attacks its own healthy tissues, especially joints and skin, a new study shows.
Black Patients with Lupus Have Three Times Higher Risk of Stroke, 24 Times Higher Risk of Ischemic Heart Disease
New research reveals that, in the U.S., Black patients with lupus have a threefold higher risk of stroke and a 24-fold higher risk of ischemic heart disease. The study also found several lupus-specific symptoms that predict stroke and IHD in these patients. Details of the study was presented at ACR Convergence, the American College Rheumatology’s annual meeting.
Many with Lupus at High Risk for Adverse Reactions to Pneumocystis Pneumonia Preventive Drug
New research shows that adults with systemic lupus erythematosus, who receive trimethoprim-sulfamethoxazole (TMP-SMX) are at high risk for adverse reactions to the drug, particularly if they are also positive for anti-Smith (anti-Sm) antibodies. Details of the study was presented at ACR Convergence, the American College of Rheumatology’s annual meeting.
Hydroxychloroquine Not Linked to Longer Heart Rhythm Intervals in Rheumatoid Arthritis or Lupus Patients
New research presented at ACR Convergence, the American College of Rheumatology’s annual meeting, discovers that use of hydroxychloroquine does not cause any significant differences in QTc length or prolonged QTc in people with rheumatoid arthritis (RA) or systemic lupus erythematosus (SLE).
‘Incredibly generous’ $25 million donation to create the Schroeder Arthritis Institute at UHN, consolidating research, education and patient care under one global brand
One in five Canadian adults is currently living with arthritis, a disease causing inflammation of the joints, which can result in chronic, debilitating pain, reduced mobility and premature disability. Arthritis is the leading cause of disability globally. To address this growing crisis, the Schroeder Arthritis Institute, launched with a $25 million donation by philanthropists Walter and Maria Schroeder, will help UHN’s innovative arthritis program become a world-class hub for innovation in research, education and patient care.
American College of Rheumatology Secures $7M Grant to Address Gaps in Lupus Care and Treatment
The American College of Rheumatology (ACR) was recently awarded a $7M grant to reduce inequities in symptom recognition, care and disease management of systemic lupus erythematosus (lupus). The grant, which will be led by the ACR’s Collaborative Initiatives (COIN) department, begins on Sept. 30.
“My Disease May Be Invisible, But I’m Not”: Patients Tell Their Stories During Rheumatic Disease Awareness Month
The American College of Rheumatology (ACR) and Simple Tasks™ will recognize the fifth annual Rheumatic Disease Awareness Month (RDAM) this September with an awareness campaign that focuses on amplifying patient voices and experiences.
New Study Identifies Better Treatment Option for Common Complication of Dialysis
Use of drug-coated balloon angioplasty to treat blocked blood vessels used for hemodialysis offers hope for millions of patients globally
New study: Hydroxychloroquine ineffective as a preventive antiviral against COVID-19
esearchers at Case Western Reserve University have added to the growing body of understanding about how hydroxychloroquine (HCQ) is not a possible defense against COVID-19.
Specifically, they found that HCQ is not effective in preventing COVID-19 in patients with lupus and rheumatoid arthritis (RA), suggesting a broader interpretation of HCQ as ineffective preventive medicine for the general population. Their findings were recently published in the Annals of the Rheumatic Diseases.
ANTILUPUS DRUG PREVENTS LOW HEARTBEAT CONDITION IN NEWBORNS
A drug used to treat systemic lupus erythematosus (SLE) significantly reduces the incidence of a rare and sometimes fatal heart condition in newborn babies, a new study from NYU Grossman School of Medicine researchers shows.
CHOP-Pioneered Spatial Mapping Method Pinpoints Potential New Therapeutic Targets in Lupus
A team of researchers from Children’s Hospital of Philadelphia (CHOP) used a new method of pinpointing potential disease-causing changes in the genome to identify two new potential therapeutic targets for lupus, while also paving the way for more accurately identifying disease-causing variations in other autoimmune disorders.

Prominent Rheumatologist to Create Scleroderma Program at Kao Institute
Nationally recognized rheumatology expert Francesco Boin, MD, has been appointed director of the division of Rheumatology and director of the new Scleroderma Program at Cedars-Sinai. Boin is an accomplished and widely published investigator of autoimmune diseases, with a reputation for clinical excellence and a multidisciplinary approach to patient care.

First Do No Harm – Researchers Urge Halt in Prescribing Hydroxycholoroquine for COVID-19
Researchers urge a moratorium on prescribing chloroquine or hydroxychloroquine, with or without azithromycin, to treat or prevent COVID-19, and caution that the reassuring safety profile of hydroxychloroquine may be more apparent than real. Safety data derive from decades of prescriptions by clinicians, primarily for their patients with lupus and rheumatoid arthritis, both of which are of greater prevalence in younger and middle age women, who are at very low risk of fatal heart outcomes due to hydroxychloroquine.

Complement genes add to sex-based vulnerability in lupus and schizophrenia
Variants in a gene of the human immune system cause men and women to have different vulnerabilities to the autoimmune diseases lupus and Sjögren’s syndrome, according to findings published in the journal Nature. The gene variants are a member of the complement system.
Sex, Genes and Vulnerability
New work led by researchers in the Blavatnik Institute at Harvard Medical School and at the Broad Institute of MIT and Harvard provides a clear genetic explanation behind the long-standing yet mysterious observation that some diseases occur more often, hit harder or elicit different symptoms in men or women.
HOW TO REDUCE FLARES IF YOU HAVE LUPUS
Medications for lupus — a long-term autoimmune disease that occurs when a person’s immune system attacks different parts of their body, including their skin — are currently being explored as a treatment for COVID-19 patients. This may significantly limit access to the drugs by those who depend on it to manage their health conditions.
Half of Lupus Rashes Harbor High Levels of Bacteria Responsible for Infections
A new study finds that one side effect of lupus could also make patients with the autoimmune condition more vulnerable to a skin infection, or spreading the infection to others.

Cedars-Sinai Receives $20M to Create Kao Autoimmunity Institute
Cedars-Sinai today announced a $20 million gift from Dr. and Mrs. Min H. Kao and the Kao Family Foundation to create the Kao Autoimmunity Institute to advance research and treatment of rheumatologic diseases. The gift also will establish the Scleroderma Program within the institute to provide interdisciplinary and integrated care for scleroderma patients and to support research, outreach, training and education to help those with the disease.
Survey: More than Half of Male Patients with Lupus Report Feeling Depressed, Receiving Little Support
Researchers at Hospital for Special Surgery (HSS) in New York City launched a nationwide survey to assess the needs of male patients and found that 58% reported feeling depressed for several days or more than half the days in the previous two weeks.

Nearly 1 in 3 Patients with Lupus Use Prescription Opioids for Pain
A new study finds nearly one in three adults with lupus use prescription opioids to manage pain, despite a lack of evidence that opioids are effective for reducing pain from rheumatic diseases.