The Norwegian Academy of Science and Letters announced the 2024 Kavli Prize Laureates, recognizing groundbreaking science for the discovery and characterization of extra-solar planets and their atmospheres; foundational research integrating synthetic nanoscale materials for biomedical use; and the localization of areas in the brain specialized for face recognition and processing.
Tag: Nanomedicine

Sylvester Researchers Develop a Nanoparticle That Can Penetrate the Blood-Brain Barrier
Researchers at Sylvester Comprehensive Cancer Center have developed a nanoparticle that can penetrate the blood-brain barrier. Their goal is to kill primary breast cancer tumors and brain metastases in one treatment.
Nanomedicine paves the way for new treatments for spinal cord injury
A Study by Politecnico di Milano and Istituto Mario Negri has been published in Advanced Materials.
Rigoberto Castillo Advincula on the 2023 Nobel Prize in Chemistry laureates for their groundbreaking work on Quantum Dots!
The field of quantum dots and nanoparticles bridges chemistry and physics like never before with colloidal phenomena and ease of materials synthesis. Bawendi, Brus, and Ekimov enabled this seminal contribution to be widespread to many researchers and applications in nanomedicine…
Nanoparticle vaccine could curb cancer metastasis to lungs by targeting a protein
UC San Diego engineers have developed an experimental vaccine that could prevent the spread of metastatic cancers to the lungs. Its success lies in targeting a protein known to play a central role in cancer growth and spread, rather than targeting the primary tumor itself.
Research identifies new potential hurdle for nano-based therapies
Researchers at The University of Texas MD Anderson Cancer Center have discovered that certain nano-based cancer therapies may be less effective in younger patients, highlighting the need for further investigation into the impact of aging on the body’s ability to respond to treatment.
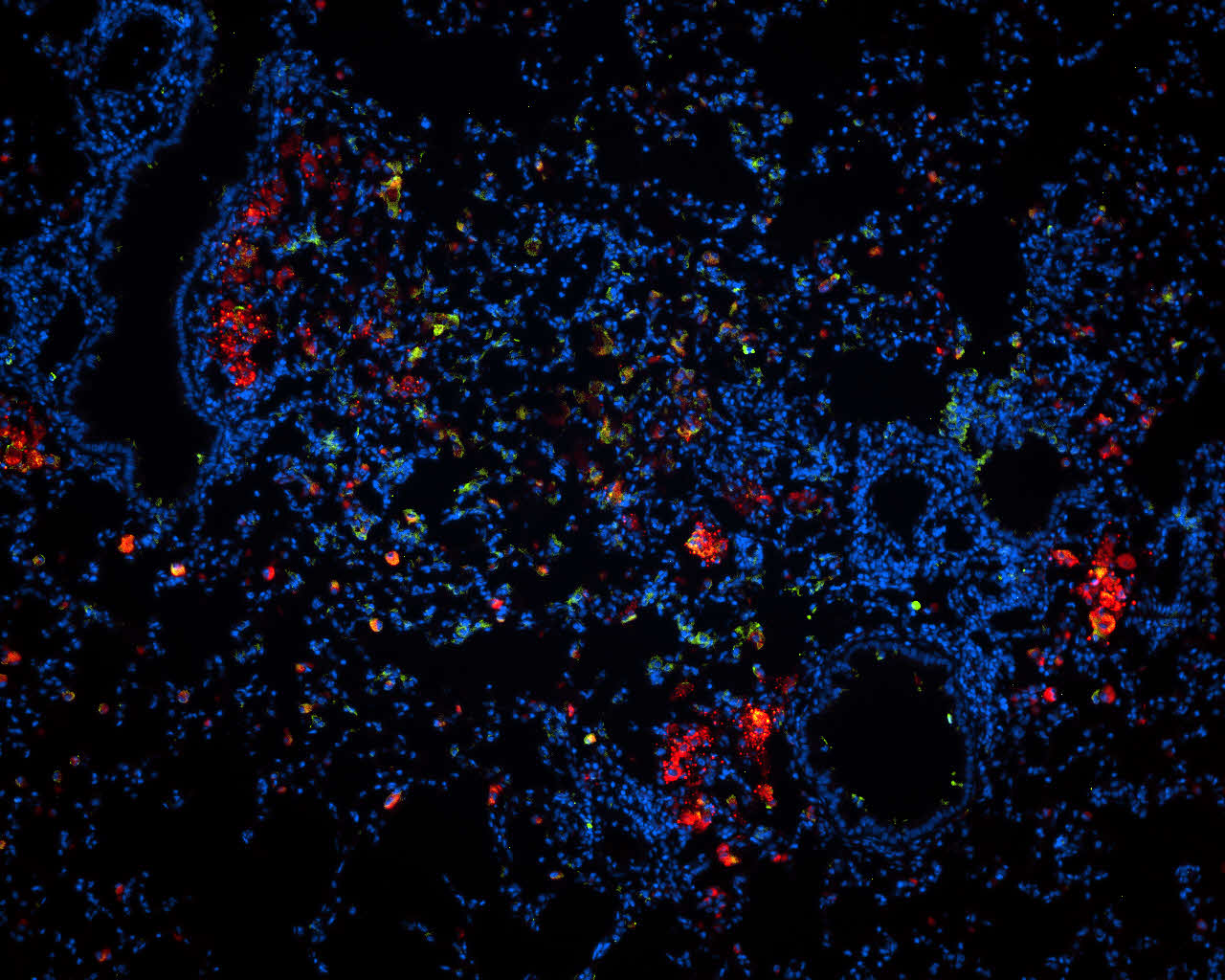
Tuberculosis Therapy: Smallest Particles Will Deliver the Drug to the Lungs in Future
Therapy of the dangerous infectious disease of tuberculosis faces the challenge of pathogens frequently being resistant to several common antibiotics. Researchers of Karlsruhe Institute of Technology (KIT) have now developed nanoparticles to deliver new antibiotics directly to the lungs in future. Surfactants ensure that the highly fat-soluble antibiotics disperse very finely in water and can be inhaled. First tests at the Research Center Borstel, Leibniz Lung Center, reveal a high effectiveness and good compatibility of the nanocarriers of antibiotics. The researchers report in ACS Nano. (DOI: 10.1021/acsnano.3c01664)

Implantable device shrinks pancreatic tumors
Houston Methodist nanomedicine researchers have found a way to tame pancreatic cancer – one of the most aggressive and difficult to treat cancers – by delivering immunotherapy directly into the tumor with a device that is smaller than a grain of rice.
Ask the expert: What are nanomedicines?
Morteza Mahmoudi, an assistant professor in MSU’s Department of Radiology, explains why addressing disagreements with stronger standards will help ensure future nanomedicines are safe, effective and successful.
A greener route to blue – a new method drastically reduces the amount of solvent needed to produce widely used organic dyes
Phthalocyanines dyes can be produced with solid-state synthesis instead of high- boiling organic solvents.
Fixing Spinal Cord Injuries With ‘Dancing Molecules’
Researchers have created an injectable therapy for spinal cord injuries that uses specially engineered molecules that trigger a healing response in spinal cells. These molecules come together to form tiny fibers in a liquid solution. Scientists can control the motion of these fibers, allowing the fibers to connect more effectively with cells in the spine. The research may lead to a cure for spinal injuries in humans.
Study finds nanomedicine targeting lymph nodes key to triple negative breast cancer treatment
Research from the University of Michigan Rogel Cancer Center could provide a new approach to treating an aggressive form of breast cancer. A study led by Duxin Sun, Ph.D., found that targeting the immune microenvironment in lymph nodes and tumors simultaneously led to long-term tumor remission in mice models of metastatic triple negative breast cancer.
Putting Functional Proteins in Their Place
Using DNA, scientists organized bioactive proteins in desired 2-D and 3-D ordered arrays—promising for structural biology, biomedicine, and more.
Nanomedicine’s ‘crown’ is ready for its close up
An international team of researchers led by Michigan State University’s Morteza Mahmoudi has developed a new method to better understand how nanomedicines — emerging diagnostics and therapies that are very small yet very intricate — interact with patients’ biomolecules.

Research News Tip Sheet: Story Ideas from Johns Hopkins Medicine
During the COVID-19 pandemic, Johns Hopkins Medicine Media Relations is focused on disseminating current, accurate and useful information to the public via the media. As part of that effort, we are distributing our “COVID-19 Tip Sheet: Story Ideas from Johns Hopkins” every other Tuesday.
Technion Harvey Prize Honors Pioneers in Chemical Engineering and Medical Sciences
The prestigious prize for 2019-2020 goes to Professor Joseph DeSimone of Stanford University for significant contributions to materials science, chemistry, polymer science nano medicine, and 3D printing; and to Professor Raphael Mechoulam of the Hebrew University of Jerusalem for the discovery of the active molecules in cannabis
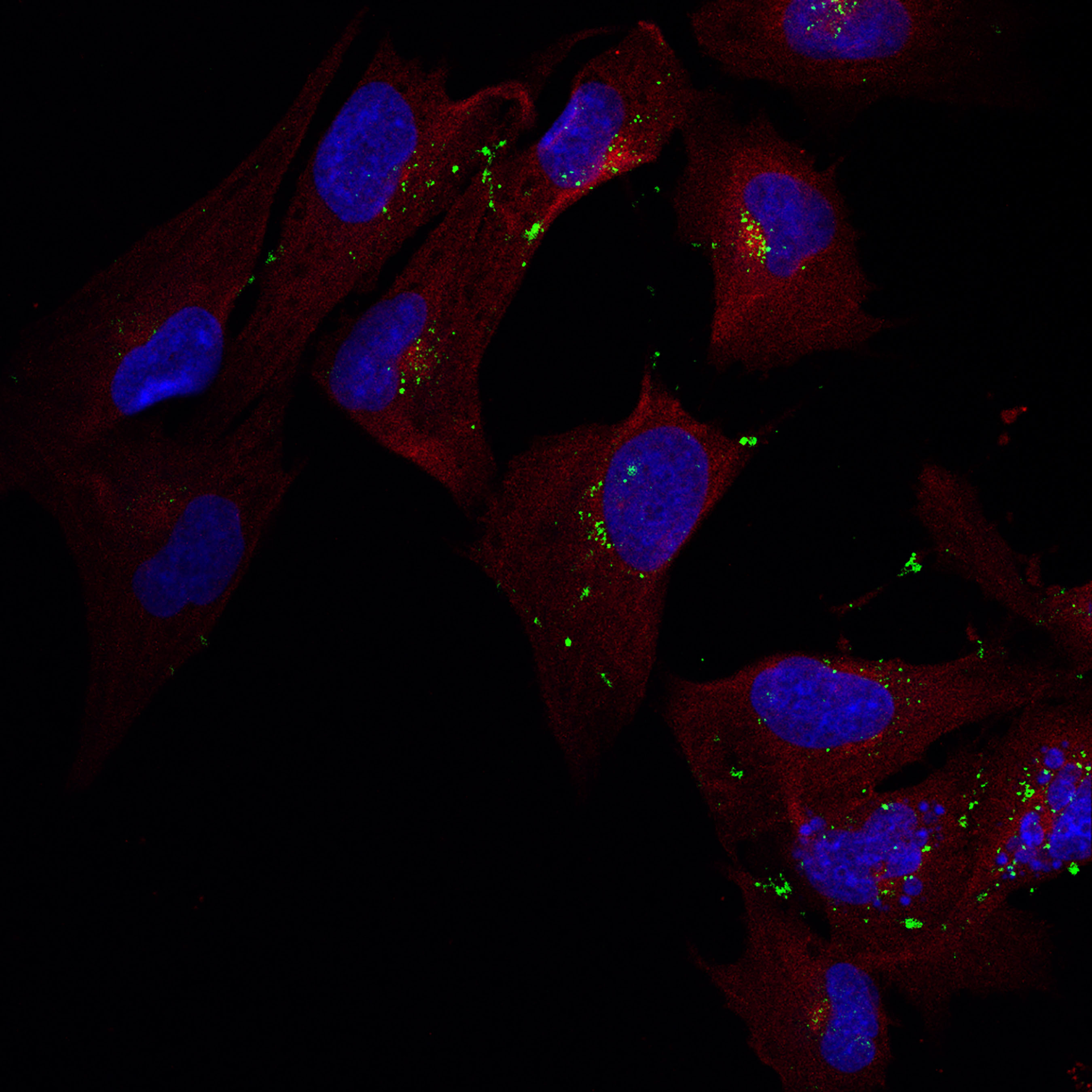
Brain’s Immune Cells Promising Cellular Target for Therapeutics
Inspired by the need for new and better therapies for neurodegenerative diseases, Rutgers University researchers are exploring the link between uncontrolled inflammation within the brain and the brain’s immune cells, known as microglia, which are emerging as a promising cellular target because of the prominent role they play in brain inflammation. In APL Bioengineering, the group highlights the design considerations and benefits of creating therapeutic nanoparticles for carrying pharmacological factors directly to the sites of the microglia.
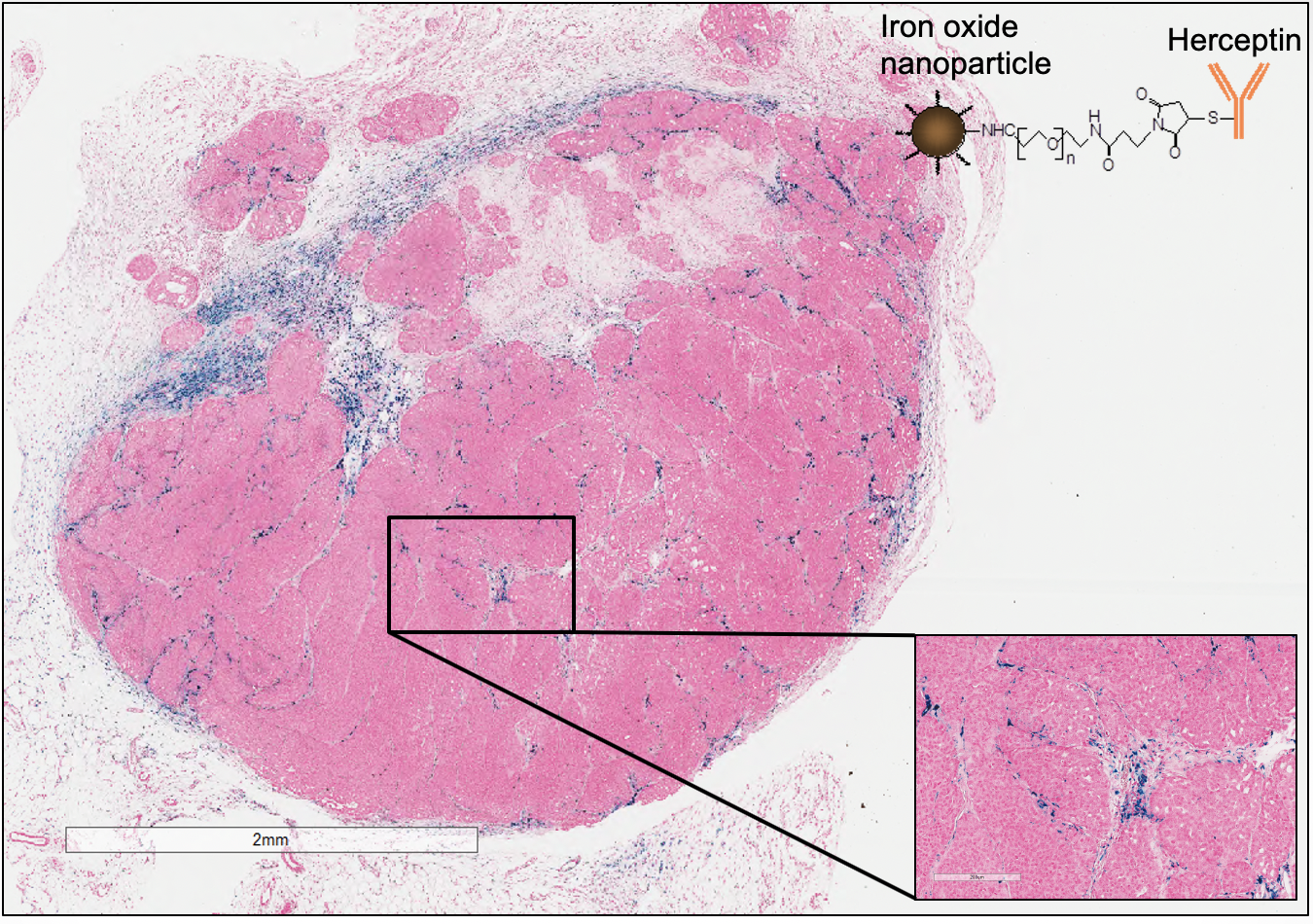
Experiments in Mice And Human Cells Shed Light On Best Way to Deliver Nanoparticle Therapy For Cancer
Researchers in the cancer nanomedicine community debate whether use of tiny structures, called nanoparticles, can best deliver drug therapy to tumors passively — allowing the nanoparticles to diffuse into tumors and become held in place, or actively — adding a targeted anti-cancer molecule to bind to specific cancer cell receptors and, in theory, keep the nanoparticle in the tumor longer. Now, new research on human and mouse tumors in mice by investigators at the Johns Hopkins Kimmel Cancer Center suggests the question is even more complicated.
Nanoparticles Deliver ‘Suicide Gene’ Therapy to Pediatric Brain Tumors Growing in Mice
Johns Hopkins researchers report that a type of biodegradable, lab-engineered nanoparticle they fashioned can successfully deliver a “suicide gene” to pediatric brain tumor cells implanted in the brains of mice. The poly(beta-amino ester) nanoparticles, known as PBAEs, were part of a treatment that also used a drug to kill the cells and prolong the test animals’ survival.

Houston Methodist researchers test-drive Lamborghini’s carbon fiber materials in space
Houston Methodist researchers are studying Italian sports car maker Automobili Lamborghini’s carbon fiber materials in space.