MedStar Washington Hospital Center has been perfecting ways to perform complex cervical spine surgery, and recently performed the first MySpine® Cervical surgery in the country.
Tag: Spine Surgery
April 2024 Issue of Neurosurgical Focus: Video: “Minimally Invasive and Endoscopic Spine Surgery Techniques”
Announcement of contents of the April 2024 issue of Neurosurgical Focus: Video
HSS Research Evaluates Whether AI Chatbots Provide Reliable Medical Information
Artificial intelligence (AI) chatbots are more accurate than expected when asked to answer medical questions about spine surgery, but patients still need to use extreme caution when turning to these tools for help with medical decision-making.
FDA Issues Clearance for Woven Orthopedic’s Simple Solution to Massive, Unspoken Challenge in Orthopedic Spine Surgery
Woven Orthopedic Technologies, developer of an implantable sleeve to aid screw fixation in challenging scenarios, announced today that its Ogmend® Implant Enhancement System has received 510(k) clearance from the Food and Drug Administration (FDA) for use in spine surgery.
January 2023 Issue of Neurosurgical Focus: “Minimally Invasive Surgery of Lumbar Spine”
Announcement of contents of the January 2023 issue of Neurosurgical Focus
Computer Vision Is Superior to Surgeons in Identifying Spinal Implants
Computer vision model outperforms surgeons when identifying types of spinal implants.
More than the Eye Can See: Hospital for Special Surgery First in NYS to Use Augmented Reality Guidance in Spine Surgery
An orthopedic surgeon at Hospital for Special Surgery (HSS) performed the first augmented reality-guided spine surgery in New York State: a successful spinal decompression and fusion on a 28-year-old male patient.
July 2022 Issue of Neurosurgical Focus: Video: “Lateral Access Spine Surgery”
Announcement of contents of the July 2022 issue of Neurosurgical Focus: Video
Pain in the Neck? New Surgical Method Could be Game-changing
Anterior cervical discectomy and fusion is widely used to treat spinal disorders. The fusion involves placing a bone graft or “cage” and/or implants where the surgically removed damaged disc was originally located to stabilize and strengthen the area. The risk factors for cage migration are multifactorial and include patient, radiological characteristics, surgical techniques and postoperative factors. A study is the first to evaluate the effect of the range of motion, cage migration and penetration using variable angle screws and cervical spine models. The plate developed and tested by the researchers provided directional stability and excellent fusion, showing promising clinical outcomes for patients with degenerative cervical spine disease.
HSS Study Evaluates Robotic- and Navigation-Assisted Pedicle Screw Placement in Adult Degenerative Spinal Surgery
Researchers at Hospital for Special Surgery launched a study to evaluate the accuracy of robotic- and navigation-assisted technology in the placement of pedicle screws in spine surgery. They also set out to determine the extra time needed in the operating room when implementing the new system.
HSS Team Shares Enhanced Recovery Pathway for Complex Spine Surgery at AAOS Annual Meeting
Surgery to treat spine deformities in the lower back in adults is often complex. Experts at Hospital for Special Surgery (HSS) have been exploring ways to increase the efficacy and efficiency of these procedures. At the AAOS annual meeting, details of an enhanced recovery pathway were presented.
First Two-Level Lumbar Disc Replacement Performed In Metro DC, Maryland, And Virginia By Spine Surgeon Dr. Christopher Good
The first two-level lumbar disc replacement was performed in Metro DC, Maryland, and Virginia on Friday, June 25, 2021, by Spine Surgeon Dr. Christopher Good (Virginia Spine Institute) – ending an around-the-world journey for one patient looking for relief to more than ten years of debilitating back pain and offering hope to many others looking for an option beyond a conventional spinal fusion that limits mobility.
UC San Diego Health is Region’s First to Use Augmented Reality in Spine Surgery
Augmented reality headsets give UC San Diego Health spine surgeons “x-ray vision” during procedures for accurate and personalized implant placement, while keeping their eyes on their patients.
What You Need to Know About Revision Spine Surgery
Spine surgery may sound scary, but for many people living with failed back surgery syndrome (FBSS), revision spine surgery is a welcomed procedure that may improve their quality of life in ways they have not experienced in years.
Hospital rankings for complications after spinal fusion are ‘unreliable’
Routinely collected data on patients undergoing spinal fusion surgery do not provide a valid basis for assessing and comparing hospital performance on patient safety outcomes, reports a study in Spine. The journal is published in the Lippincott portfolio by Wolters Kluwer.
Cannabis use disorder linked to increased complications after spinal surgery
For patients undergoing spinal surgery, the diagnosis of cannabis use disorder is associated with higher complication rates, including substantially increased risks of stroke and respiratory complications, reports a study in Spine. The journal is published in the Lippincott portfolio by Wolters Kluwer.

Lending a Hand: Use of Robotic-Arm Enables Pinpoint Accuracy During Spine Surgery
Advances such as computer navigation, 3D imaging and robotic-assisted surgery are enabling spine surgeons to perform less invasive, yet more precise procedures at Hospital for Special Surgery in New York City.

Rush University Is Bringing Innovative Education To The Table
Rush University’s Center for Innovative and Lifelong Learning (CILL) is leading the way in innovative education in the field of orthopedics. Launching the Rush International Spine Education (RISE) initiative, the world’s first academically supported, international program in blended learning for spine specialists.

Baylor Scott & White Medical Center – Frisco Becomes First Hospital in Texas to Deploy New Technology to Enhance Patient Safety During Spine Surgery
Baylor Scott & White Medical Center – Frisco has added an innovative operating room technology aimed at improving patient safety during spine surgery.
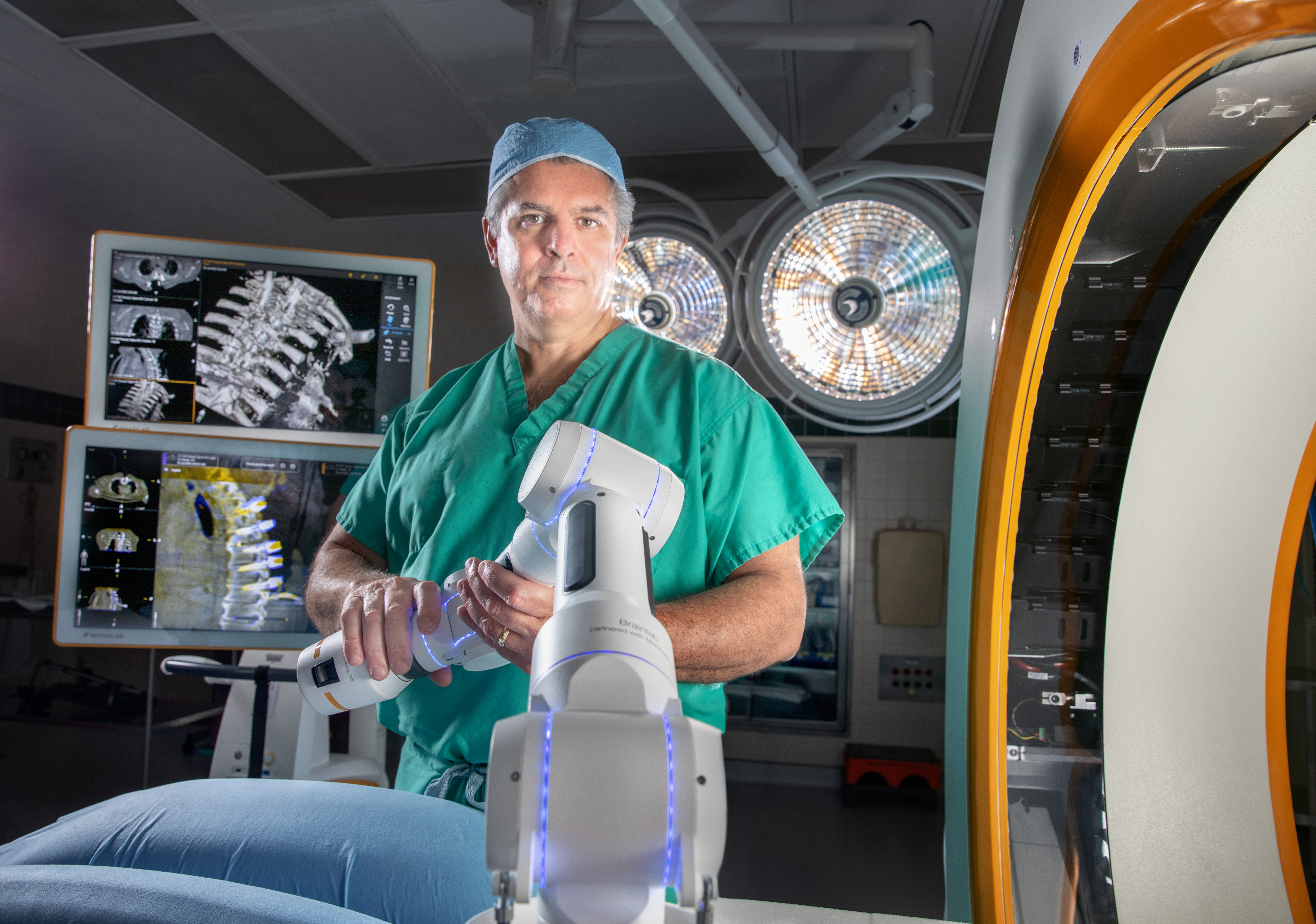
Cirq Robotic Arm Enhances Spine Surgeries and Increases Precision
Two MedStar Health hospitals now offer an innovative technology that improves accuracy and speeds recovery time for patients who undergo spine surgery. MedStar Washington Hospital Center became first in the U.S. to use the Cirq® robotic arm. MedStar Georgetown University Hospital started using the Cirq in September.
Predicting Poor Pain Control Following Elective Spine Surgery
Researchers at the University of Calgary have developed and validated a clinical prediction scale that can be used to determine which patients are more likely to experience inadequate pain control following elective spine surgery.

Hackensack Meridian Mountainside Medical Center Appoints Robert F. Heary Medical Director of Spine Program
MONTCLAIR, New Jersey (September 8, 2020) – Mountainside Medical Center has announced that Robert. F. Heary will take on the new role as Medical Director of the Spine Program. In this new role, Dr. Heary will oversee the Montclair Spine Center at Mountainside Medical Center to ensure the organization and delivery of excellent, timely, evidence-based care.
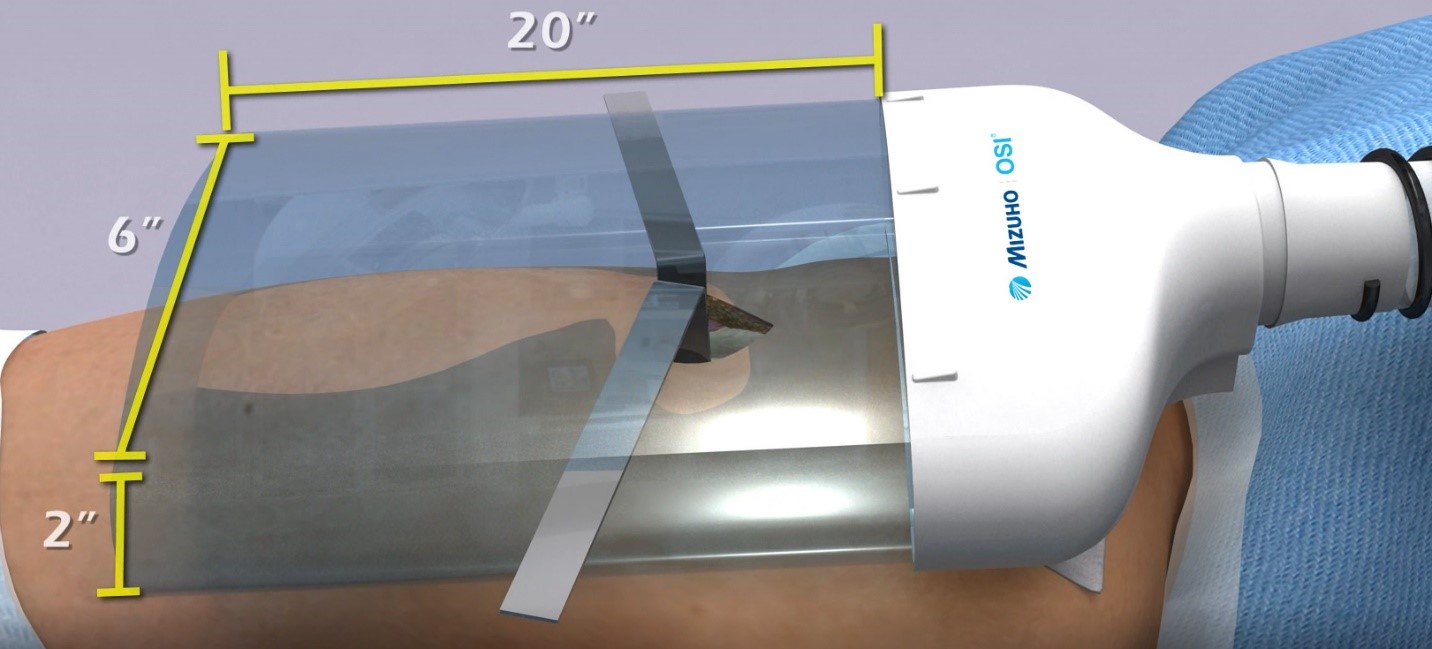
Mizuho OSI® Acquires the Nimbic Air Barrier System to Expand into Helping Protect Surgical Sites from Airborne Particulates
Mizuho OSI®, a leading manufacturer of specialty surgical tables and pressure injury abatement solutions is pleased to announce the acquisition of the Air Barrier System (ABS) from Nimbic Systems, Inc.

HSS Doctors Offer Practical Advice on Reaching Peak Performance During Surgical Training in AAOS Journal
Studies show that athletes and musicians achieve peak performance by constant practice, by setting specific goals, having strong mentors and cultivating perseverance, stoicism and grit. Could incorporating these principles into the training of surgeons improve their residency experience?
The September 2020 Issue of Neurosurgical Focus Examines Thoracolumbar Anterior Spine Surgery
Announcement of contents of the Neurosurgical Focus September issue
CHOP Spine Surgeons Outline Framework for Prioritizing Procedures as Elective Surgeries Resume
As hospitals resume elective procedures, including pediatric spine surgeries, surgeons from Children’s Hospital of Philadelphia (CHOP) have outlined a framework for prioritizing pediatric spine surgeries amid the pandemic. The recommendations were published recently in The Journal of Bone and Joint Surgery.
Study Finds Patients Who Undergo Spine Surgery Prescribed Most Narcotics Three Months Following Surgery
As Americans have the highest opioid use rates, leading to abuse, the orthopaedic community has committed itself to studying prescription methods and patient populations to help mitigate potential addiction. A new scientific review article titled, “Ninety-day Postoperative Narcotic Use After Hospitalization for Orthopaedic Trauma,” published in the July issue of the Journal of the American Academy of Orthopaedic Surgeons (JAAOS), found a correlation between patient-reported pain at discharge from inpatient surgery and the number of opioids prescribed during the 90-day postoperative period.
Spine Surgeons Face COVID-19 Challenges Worldwide
Spine surgeons across the world are experiencing effects of COVID-19, including canceled procedures, changes in clinical roles, anxiety and risk of exposure to the disease themselves due to insufficient protective equipment. An international team of researchers reported these findings recently in the Global Spine Journal.

Mercy Medical Center Named America’s 100 Best for Orthopedic Surgery, Joint Replacement, and Spine Surgery
A recognized leader in the field of orthopedic medicine, Mercy Medical Center is one of America’s 100 Best Hospitals for Orthopedic Surgery, Joint Replacement and Spine Surgery, according to a national study by Healthgrades, the leading online resource for information about physicians and hospitals.