Hackensack University Medical Center Foundation to Host 6th Annual NICUSTRONG Walk to Advance Care for Smallest Patients
Tag: NICU

Neonatologist Travels to China to Share ECMO Experience
This spring, Rachel Chapman, MD, traveled to two cities in China to share expertise on one of the most complex lifesaving interventions for critically ill newborns: extracorporeal membrane oxygenation (ECMO).Dr. Chapman, Associate Division Chief of Neonatology and Medical Director of the Newborn and Infant Critical Care Unit (NICCU) at Children’s Hospital Los Angeles, was invited to speak at two meetings: the National Conference of the Chinese Neonatologist Association, held March 24-26 in Beijing, and the Guangzhou Newborn and Infant ECMO International Forum, held March 31-April 2 in Guangzhou.
Going Beyond Lung Care for Babies With Bronchopulmonary Dysplasia
The Infant Chronic Lung Disease Program takes a coordinated, multidisciplinary approach to support each baby’s overall development. For Manvi Bansal, MD, one of the biggest challenges of caring for babies with severe bronchopulmonary dysplasia (BPD) is dealing with “the elephant in the room.”

Time to Extubate Varies Widely After Mandibular Distraction Osteogenesis
Nearly two decades ago, Children’s Hospital Los Angeles was among a handful of centers that pioneered mandibular distraction osteogenesis (MDO) for infants with airway obstructions due to micrognathia (undersized jaw).
New UNLV Program Training Next Generation of Occupational Therapists
UNLV’s new intensive and innovative three-year doctoral program in occupational therapy, housed in the School of Integrated Health Sciences, is training students to meet the needs of Nevada patients — from babies in the NICU to those recovering from accidents and strokes — reclaim their lives.
Depression in Dads of Preemies Deserves More Attention
While postpartum depression in new mothers is well recognized and known to increase if the newborn requires intensive care, depression in new fathers has not received much attention. A large study, published in the journal Pediatrics, found that both parents with a baby in the NICU are at risk, with depression symptoms identified in 33 percent of mothers and 17 percent of fathers. Strikingly, the probability of reporting depression symptoms declined significantly for mothers but not for fathers after the baby came home.
Thirdhand smoke impacts gut bacteria for infants, study finds
Infants exposed to thirdhand smoke while hospitalized in the neonatal intensive care unit (NICU) show a difference in the composition of their gut microbiome, according to a new study by researchers with The University of Texas Health Science Center at Houston (UTHealth).
Specialized Care Team Launched in Central Texas to Help High-Risk Expectant Mothers
To offer transport to a high level of specialty care for expectant mothers and their babies, Baylor Scott & White Health has launched the system’s first Central Texas maternal transport team.
Baylor Scott & White maternal nurses staff the team, which also includes pilots, paramedics and EMTs who will facilitate transfers of high-risk obstetrics patients via air and ground transfers from hospitals throughout the region. The maternal transport team began service May 17, transporting patients to and from facilities inside and outside of the Baylor Scott & White Health system.
American Association of Critical-Care Nurses Announces Recipients of 2021 Circle of Excellence Awards
The 18 nurses who receive the Circle of Excellence award from AACN this year demonstrate an exceptional commitment to achieving excellent outcomes in the care of acutely and critically ill patients and their families, with solution-oriented approaches to challenges, including the COVID-19 pandemic.

Cincinnati Children’s Develops Model to Help Identify Risk Factors for Reading Difficulties in Children before Kindergarten
Researchers at Cincinnati Children’s Hospital Medical Center have developed a new framework for different factors influencing how a child’s brain is “wired” to learn to read before kindergarten.
Dunkin’, March of Dimes Team Up to Bring Joy to Rush Children’s Hospital
Spider-Man made a surprise visit at Rush University Children’s Hospital on Tuesday as it celebrated “Superhero Day” to recognize the strength of young patients and their families.

Boy Scout Donates 100 Quilts to Rush Neonatal Intensive Care Unit
A Boy Scout who received care in the Rush Neonatal Intensive Care Unit after being born prematurely, donated 100 blankets to the Rush NICU as part of his project to become an Eagle Scout.
Hospitals Leaned Toward Strict COVID-19 NICU Policies Despite Low Prevalence of Infection, New Study Finds
Two studies examining the impact of COVID-19 on neonatal intensive care units (NICUs) found the prevalence of COVID-19 in NICU infants is low, yet many hospitals at the start of the pandemic put in place strict parental visitation policies and scaled back NICU services such as lactation support and therapy.

Hackensack Meridian Hackensack University Medical Center Foundation Raises Over $50,000 in Third Annual NICUSTRONG Walk, Reimagined Virtually
Hackensack University Medical Center Foundation Raises Over $50,000 in Third Annual NICUSTRONG Walk, Reimagined Virtually

NewYork-Presbyterian Alexandra Cohen Hospital for Women and Newborns Opens
NewYork-Presbyterian today celebrated the opening of the NewYork-Presbyterian Alexandra Cohen Hospital for Women and Newborns, a state-of-the-art facility dedicated to providing exceptional, individualized care to pregnant women and their newborn babies before, during, and after childbirth—including advanced care for high-risk pregnancies and newborns who require extra support.
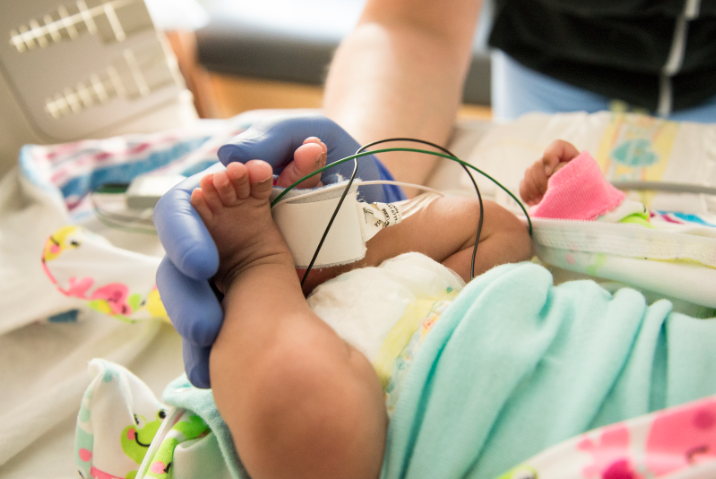
Use of hormone provides no neuroprotection in preemies
NIH-funded, nationwide study, led by a UW Medicine newborn care physician, suggests erythropoietin, while safe, may not protect against severe brain damage.

Study Answers When Moderate to Late Preterm Babies Go Home
“When is my baby going home?” is one of the first questions asked by families of infants admitted to the neonatal intensive care unit (NICU). Now clinicians have a data-based answer. Moderate to late preterm babies (born at gestational age of 32 to 36 weeks) who have no significant medical problems on admission are likely to be discharged at 36 weeks of postmenstrual age (gestational age plus age since birth), according to a study published in the American Journal of Perinatology. Small for gestational age infants and those with specific diagnoses may stay longer.