Researchers at Washington University School of Medicine in St. Louis have shown that the cancer therapy known as CAR-T can be applied to multiple sclerosis (MS), an autoimmune disease of the nervous system. The findings extend the powerful tool of immunotherapy to autoimmune diseases, a class of diseases that are often debilitating and difficult to treat.
Tag: CAR-T cell therapy
Researchers seek to improve success of chimeric antigen receptor-T cell therapy in non-Hodgkin lymphoma
A study published by researchers from Mayo Clinic Cancer Center at Mayo Clinic in Florida and Case Western, Cleveland Medical Center, investigates the reasons for decreasing remission rates for patients with non-Hodgkin lymphoma treated with chimeric antigen receptor-T cell therapy (CAR-T cell therapy).
Therapy Using Dual Immune System Cells Effectively Controls Neuroblastoma
A newly developed immunotherapy that simultaneously uses modified immune-fighting cells to home in on and attack two antigens, or foreign substances, on cancer cells was highly effective in mice implanted with human neuroblastoma tissue.
Mayo Clinic researchers study potential new CAR-T cell therapy for multiple myeloma
Researchers at Mayo Clinic Cancer Center are studying a potential new chimeric antigen receptor-T cell therapy (CAR-T cell therapy) treatment for multiple myeloma. Their findings were published on Friday, June 24, in The Lancet.
Mayo Clinic researchers study new class of drugs to treat multiple myeloma
Mayo Clinic researchers are studying a new class of immunotherapy drugs called “bispecific antibodies” that have demonstrated potent tumor-killing activity in multiple myeloma. A paper highlighting this work was published in Blood Cancer Discovery.
The University of Kansas Cancer Center Among the First to Offer CAR T-cell Therapy to Treat Multiple Myeloma
The University of Kansas Cancer Center is the first and only site in the region to offer CAR T-cell therapy to treat multiple myeloma, a type of blood cancer that affects about 30,000 people each year.
Seattle Cancer Care Alliance Selected as an Authorized Treatment Center for BreyanziTM/Liso-Cel CAR T-Cell Treatment
Seattle Cancer Care Alliance (SCCA), the only NCCN-designated cancer center in Washington State, has been selected as an authorized treatment center for the new chimeric antigen receptor (CAR) T-cell therapy lisocabtagene maraleucel, also known as liso-cel and by the brand name BreyanziTM. Liso-cel was approved by the U.S. Food and Drug Administration (FDA) on February 5, 2021.
Fred Hutch statement regarding the FDA approval of CD19 immunotherapy, lisocabtagene maraleucel
SEATTLE — Feb. 5, 2021 — Today the U.S. Food and Drug Administration approved the chimeric antigen receptor immunotherapy, Breyanzi (lisocabtagene maraleucel or liso-cel), for the treatment of adults with relapsed or refractory (R/R) large B-cell lymphoma after at least two prior therapies.The approval was granted to Bristol Myers Squibb, and development of the therapy was supported by physician-scientists at Fred Hutchinson Cancer Research Center.
New approach to fighting cancer could reduce costs and side effects
CAR-T biotherapeutics company Carina Biotech and researchers at the University of South Australia have developed a novel approach based on microfluidic technology to “purify” the immune cells of patients in the fight against cancer.
Seattle Cancer Care Alliance Selected as an Authorized Treatment Center for TecartusTM, a Novel Immunotherapy Treatment
Seattle Cancer Care Alliance (SCCA), the only National Comprehensive Cancer Network (NCCN)-designated cancer center in Washington state, has been selected as an authorized treatment center to offer brexucabtagene autoleucel, also known by the brand name TecartusTM. It is the first and only chimeric antigen receptor (CAR) T-cell therapy approved by the U.S. Food and Drug Administration (FDA) for the treatment of adult patients with relapsed or refractory mantle cell lymphoma (MCL).

John Theurer Cancer Center Investigators Participated in ZUMA-2 Study Leading to FDA Approval of First CAR T-Cell Therapy for Recurrent/Persistent Mantle Cell Lymphoma
The U.S. Food and Drug Administration granted accelerated approval for brexucabtagene autoleucel (TECARTUS™, formerly KTE-X19) as the first and only CAR T-cell therapy for patients with mantle cell lymphoma (MCL) relapsed or refractory to prior treatments. Investigators from Hackensack Meridian John Theurer Cancer Center (JTCC) at Hackensack University Medical Center in New Jersey participated in the pivotal trial which the approval was based: the ZUMA-2 clinical trial, which assessed the safety and effectiveness of brexucabtagene autoleucel in patients with relapsed or refractory MCL who had received up to five prior regimens of treatment and had exhausted all other therapies. That transformative study showed that 93% of patients responded to treatment, with 67% achieving a complete response (no evidence of disease). The data were published in the April 2, 2020 issue of the New England Journal of Medicine.
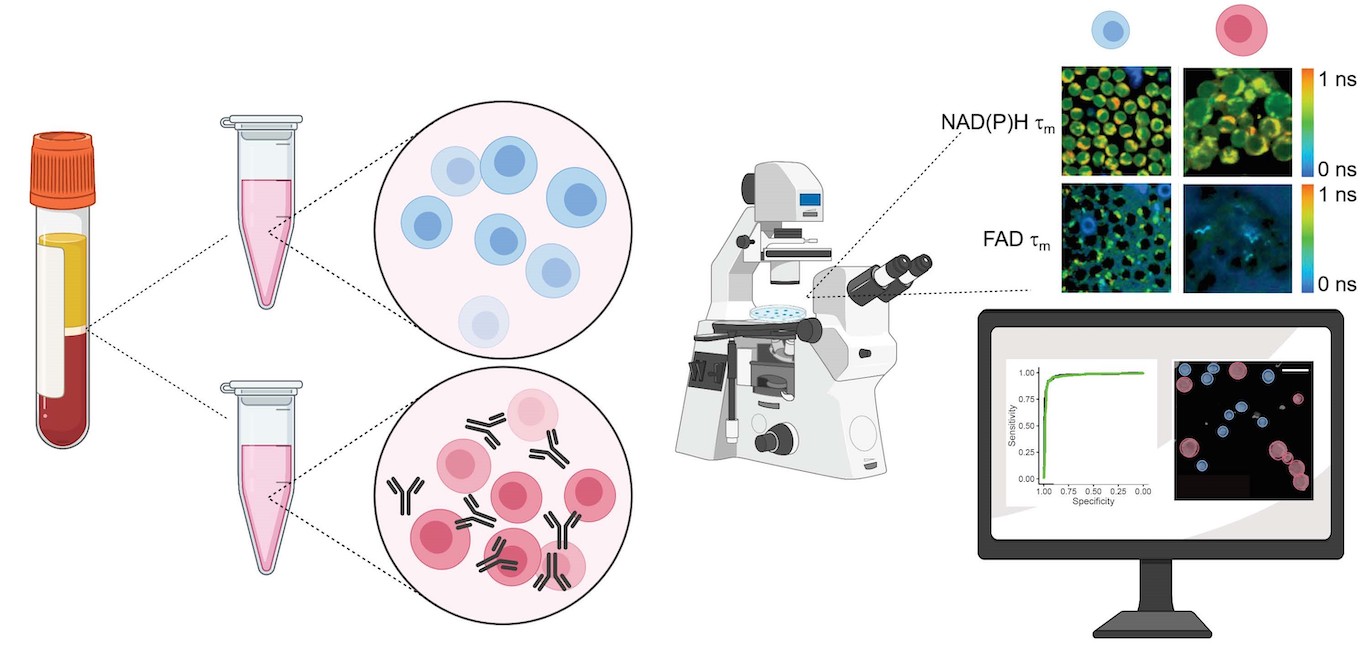
Novel label-free imaging technique brings out the inner light within T cells
A new imaging method developed by the Skala lab uses the natural autofluorescence within cells to assess T cell activity. The technique could help assess T cell involvement in immunotherapies.
Excellent Research Results for CAR-T Cell Therapy Against Hodgkin Lymphoma
CAR-T cell therapy, which attacks cancer cells using a person’s reprogrammed immune cells, has been used to treat Hodgkin lymphoma with remarkable success for the first time, according to the results of an early phase clinical trial.

CAR-T immunotherapy for lymphoma studied at UNC Lineberger receives fast-track designation from FDA
Based on proof-of-concept results from clinical trials at University of North Carolina Lineberger Comprehensive Cancer Center and Baylor College of Medicine, an investigational cellular immunotherapy for Hodgkin lymphoma has received a Regenerative Medicine Advanced Therapy designation from the U.S. Food and Drug Administration.
Discovery would allow researchers to fine-tune CAR-T activity
In a study published in Cancer Cell, researchers reported new findings about the regulation of co-stimulatory molecules that could be used to activate cancer-killing immune cells – chimeric antigen receptor T-cells, or CAR-T – or decrease their activity.

CAR T Cell Clinical Trial for Non-Hodgkin’s Lymphoma Begins at Atlantic Health System
Atlantic Health System is treating patients in a new Phase 2 clinical trial of CAR T-cell therapy at Morristown Medical Center. A select number of sites across the U.S. are involved in this study, which is done on an outpatient basis. The study is sponsored by Juno Therapeutics, Inc. The study’s principal investigator, Mohamad Cherry, MD, medical director of hematology for Atlantic Health System Cancer Care, is a nationally known expert at treating and researching blood-related cancers such as lymphoma, leukemia and myeloma. Dr. Cherry is triple board-certified in internal medicine, hematology and medical oncology

NUS scientist designs ‘express courier service’ for immune cells
Dr Andy Tay, a researcher with the National University of Singapore (NUS) who is currently doing his post-doctoral training at Stanford University, has successfully invented a novel transfection method to deliver DNA into immune cells with minimal stress on these cells. This new technique is expected to boost DNA-based cancer immunotherapy by significantly improving the process of generating high-quality genetically modified immune cells.