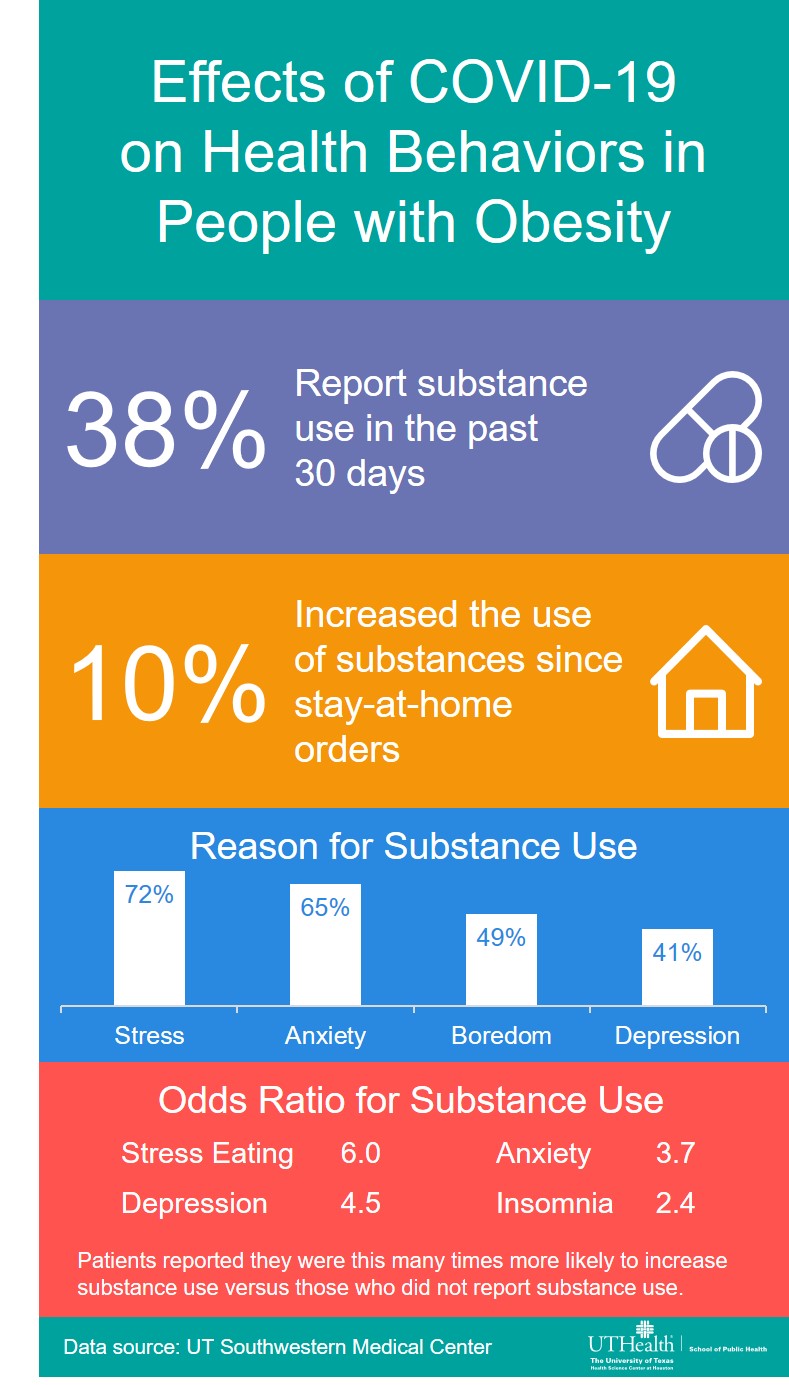
The study, published in the journal Clinical Obesity, surveyed 589 patients with obesity who are enrolled in the UT Southwestern Weight Wellness Program, a multidisciplinary weight management and post-bariatric care clinic. Nearly half of the group reported using recreational drugs and alcohol, and 10 percent reported increased use since the start of the pandemic. Seventeen of the patients have tested positive for COVID-19.
Almost a quarter (24.3 percent) of the patients reported using opioids in the 30 days preceding the survey, 9.5 percent sedatives or tranquilizers, 3.6 percent marijuana, and 1 percent stimulants. Patients were surveyed from June 1, 2020, to Sept. 30, 2020, after COVID-19 stay-at-home orders had been lifted in North Texas.
“Many patients with obesity are also challenged by mental health conditions. Those who reported anxiety, depression, and trouble sleeping were two to four times more likely to increase their use of substances. For those who reported stress eating, there was a sixfold increase in substance use,” says study author Jaime Almandoz, M.D., MBA, medical director of the Weight Wellness Program and assistant professor of internal medicine at UT Southwestern.
According to the Centers for Disease Control and Prevention, more than 42 percent of American adults are obese. Obesity-related health conditions include heart disease, stroke, Type 2 diabetes, and certain types of cancer that are some of the leading causes of preventable, premature death.
Nearly 70 percent of the patients reported that it was more difficult to achieve their weight loss goals during the pandemic, with about half spending less time on exercise. These findings were similar to another paper authored by Almandoz last spring, which was one of the first studies to show the impact of shelter-in-place orders on health behaviors in people with obesity.
“This study demonstrates that adults with obesity continued to engage in the same behaviors and struggled with mental health challenges, even after lockdown orders were lifted. We need to develop interventions targeting these vulnerable groups, such as telehealth options and outreach efforts,” says senior author Sarah Messiah, Ph.D., M.P.H., an adjunct professor in the UTSW department of population and data sciences and a professor in the department of epidemiology, human genetics, and environmental sciences at the UTHealth School of Public Health.
The researchers noted that the patients surveyed were predominantly white, college-educated individuals with middle- to high-income levels. Thus, the survey results may not be generalizable to other populations, and may not accurately assess the burden of the pandemic on obesity-related health behaviors in lower socioeconomic status and/or ethnic minority populations disproportionately affected more by obesity and COVID-19. The survey participants were established weight management patients with health insurance – not representative of the average American challenged with obesity, in which less than 2 percent receive anti-obesity medications and fewer than 1 percent undergo bariatric surgery.
Other researchers involved in the study include Luyu Xie, Jeffrey N. Schellinger, M. Sunil Mathew, Nora Bismar, Ashley Ofori, Sachin Kukreja, Benjamin Schneider, and Denise Vidot.
This work was funded by the National Institutes of Health’s National Institute on Minority Health and Health Disparities.