Since the start of the pandemic, scientists have worked endlessly to understand SARS-CoV-2, the coronavirus that causes COVID-19. Even with the arrival of vaccines, the virus is still spreading and there is a need to develop alternative therapies. Scientists hope to achieve this by studying how SARS-CoV-2 infects cells and propagates itself while avoiding the body’s natural immune system.
Now researchers at UT Southwestern have added another piece to this puzzle with their study published in Science Advances.
“When a virus infects a cell, the way the host cell reacts is to alter cellular pathways (or networks) in certain ways to counteract the viral infection. Viruses can target many of these pathways to favor their own replication,” says Beatriz Fontoura, Ph.D., professor of cell biology at UTSW and corresponding author of the paper.
Viruses replicate by suppressing the host cell’s genes in favor of their own. One way they do this is by blocking the export of messenger RNA (mRNA) from the nucleus of the cell to another compartment called the cytoplasm. Some of these RNAs code for proteins that can only be made by the cell in the cytoplasm. So, by blocking their export from the nucleus, viruses prevent some proteins from being made (e.g., antiviral proteins) and simultaneously free up the cell’s machinery for their own replication.
“We’ve been studying the NS1 protein of the influenza virus and we have shown that one of its functions is to block mRNA nuclear export. Due to some similarities between NS1 from flu and Nsp1 from coronaviruses in their roles in suppressing antiviral response in the host cell, we decided to test whether these two proteins shared a similar function,” says Ke Zhang, Ph.D., a postdoctoral researcher in Fontoura’s lab and first author of the paper.
The researchers landed on the protein Nsp1. Coronavirus Nsp1 has been described as a multifunctional protein capable of altering viral replication and suppressing the production of other proteins, some of which are involved in immune response. Fontoura’s group sought to find out how Nsp1 does this and if it uses a mechanism similar to that of the influenza virus protein NS1.
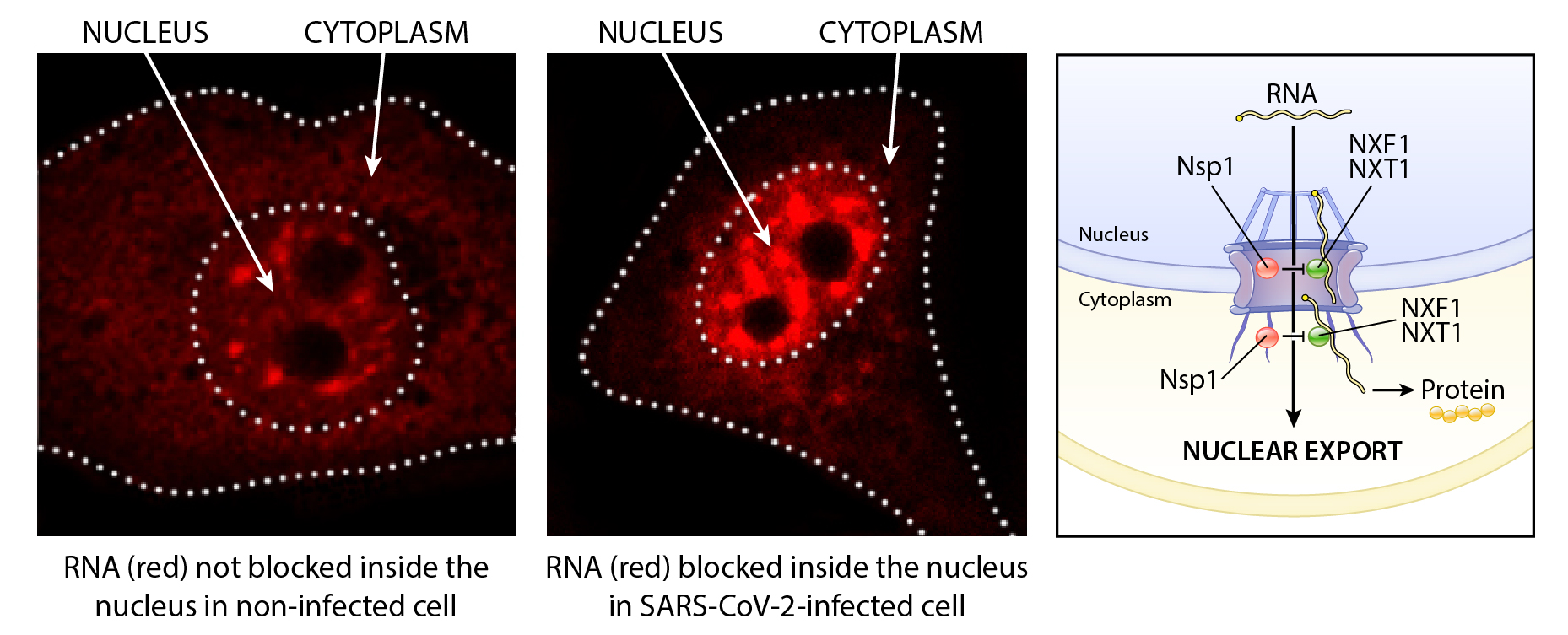
Indeed, the group found that like NS1 from influenza, SARS-CoV-2 Nsp1 inhibits host cell mRNA nuclear export by binding to the export factor NXF1. This new role of Nsp1 complements the protein’s other function, blocking host cell mRNA translation into protein. By obstructing two steps that lead to the production of proteins, Nsp1 suppresses a cell’s ability to respond to the viral infection, allowing SARS-CoV-2 to replicate. So what would happen, researchers wondered, if Nsp1 could be stopped from performing one of these functions?
In a proof-of-principle experiment, the researchers infected cells with SARS-CoV-2 and added an excess of NXF1 to see if this would block virus replication. Strikingly, that’s exactly what they found. When the cells had access to more NXF1 than the SARS-CoV-2 virus could suppress, the cells were able to stop the virus from multiplying.
The study offers insight into the mechanism behind how coronaviruses, and SARS-CoV-2 in particular, are able to promote their replication inside host cells. Understanding this mechanism provides a building block for potential therapeutics.
“If you find a way to block the interaction between Nsp1 and NXF1 or increase the amount of NXF1 in the cell, you’ll get mRNAs out of the nucleus and may get a protective effect, as suggested by our experiments,” says Fontoura.
COVID-19 treatments focus on management of symptoms while the body fights off the infection with its natural defenses. A key area of interest in viral therapies is to target the infected cells to stop the virus from replicating. Focusing on Nsp1 or its interaction with NXF1 represents a possible way to do this.
“We still need to know more, like the structure of Nsp1 bound to NXF1, which would shed light on how this blocks mRNA export and how we can revert it,” says Zhang. “The research is promising, but in order to develop therapies down the line, we first need to better understand the mechanism.”
This research was supported by funds from the National Institutes of Health (R01-AI154635 and U54 CA260560 Project 2), a Career Enhancement Program Award SPORE; a Mary Kay Foundation International Postdoctoral Scholar Fellowship; the Canadian Institutes of Health Research; the Center for Research on Influenza Pathogenesis; DARPA grant HR0011-19-2-0020; a Lung Cancer SPORE; the Cancer Prevention and Research Institute of Texas; and philanthropic donations from the JPB Foundation, the Open Philanthropy Project, and anonymous donors.
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty has received six Nobel Prizes, and includes 23 members of the National Academy of Sciences, 17 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 2,500 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide care in about 80 specialties to more than 105,000 hospitalized patients, nearly 370,000 emergency room cases, and oversee approximately 3 million outpatient visits a year.