The rate at which Americans died from firearm injuries increased sharply starting in 2015, a new study shows. The change occurred to varying degrees across different states, types of firearm death such as homicide and suicide, and demographics.
In all, the United States saw a 14% rise in the rate of firearm deaths from 2015 through 2017, compared with the rate seen in the years 1999 through 2014.
During the entire 19-year period, 612,310 Americans died from firearm injuries that were self-inflicted, caused by others, accidental or of undetermined cause. Nearly one-fifth of the deaths happened in just the last three years of that time.
The study, published in the October issue of Health Affairs by a team led by University of Michigan researchers, used data from the federal Centers for Disease Control and Prevention.
Jason Goldstick, Ph.D., a research assistant professor of emergency medicine at the U-M Medical School, led the analysis. “What we can see is a worsening epidemic of firearm mortality that is geographically and demographically broad,” he says. “But our analysis of subpopulations also reveals clues to how to focus efforts to reverse the overall trend.”
Geographic differences
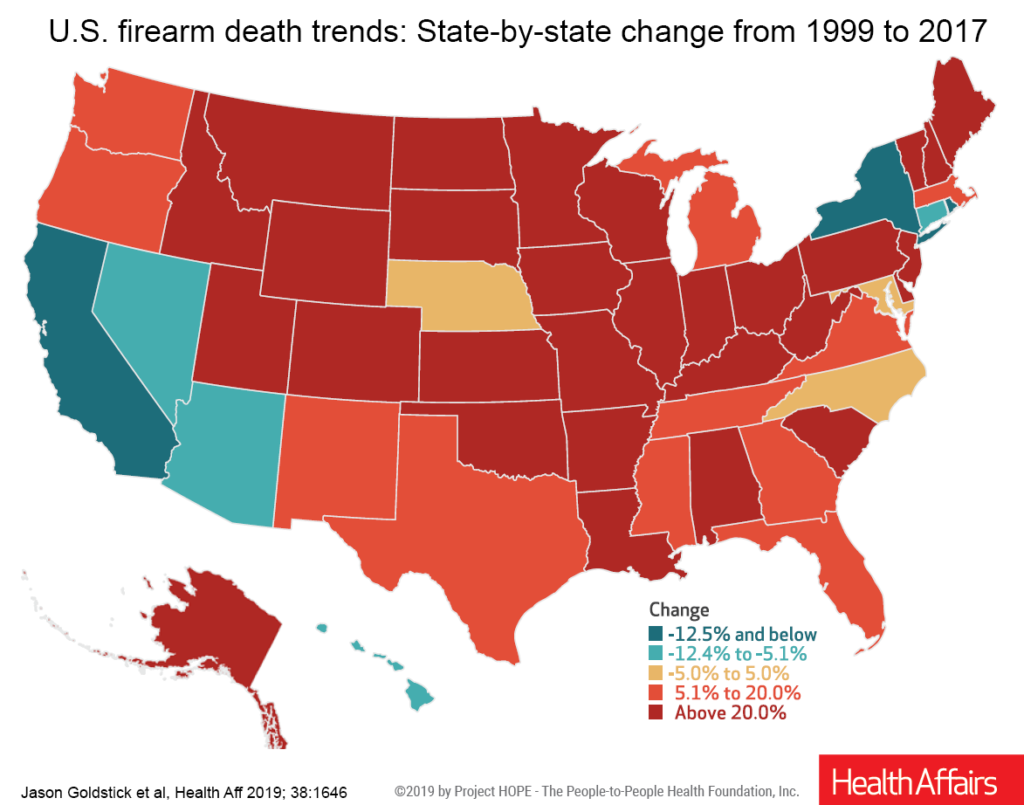
The research reveals differences across states in the change in firearm mortality rates over time. From 1999 to 2017, a majority of states had firearm trends that increased by more than 20%, but a few states had declines.
For instance, New York, California and the District of Columbia bucked the national trend and saw decreases in their firearm death rates across most categories of people in 2015 through 2017. Those three areas, plus Arizona and Nevada, also saw an overall decrease in firearm deaths from 1999 to 2017.
Demographic differences
Across the country, nearly all demographic groups saw increases in firearm death rates, but the level of increase varied across groups. For example, males had larger absolute increases than females.
Hispanic whites were the only racial or ethnic group that saw reductions in mortality in recent years, while firearm mortality rates among both non-Hispanic whites and African-Americans increased significantly. There were broad increases across age groups.
Type of firearm death differences
Throughout the study period, suicides and homicides remained consistent in their share of all firearm-related deaths. Specifically, suicide accounted for about 60% of deaths, and homicides about 38%, in both 1999 to 2014, and 2015 to 2017. Rates of firearm deaths categorized as unintentional dropped in recent years, but these made up less than 1% of all firearm deaths.
Trends and implications for states
The researchers also point out state-specific trends in the demographics and causes of firearm deaths. Now that the data in the paper and its detailed state-by-state appendices are available, the authors point out that policymakers could identify which sub-populations are most affected by firearm deaths in their states. They could then seek to determine which approaches may be most appropriate based on evidence about the effects of different policy-based interventions on different subgroups.
For example, while many states saw their suicide and homicide rates change at about the same pace, some did not. Delaware’s overall firearm mortality rate rise was mainly due to a rise in homicides in recent years, for instance, but this was not the case for most other states.
“In our home state of Michigan, homicide has remained at an unacceptably high, but steady, rate over the period from 1999 through 2017, and we’ve seen an increase in suicide rates in that same time,” says senior author Rebecca Cunningham, M.D., a professor of emergency medicine and interim vice president for research at U-M. “Also in Michigan, firearm mortality has remained concerningly high among all groups, but we now see increased rates among non-Hispanic whites, and older adults.”
Because different prevention strategies address different mechanisms and sub-populations, these trends have implications for prevention. “For instance, suicide remains the most common mechanism of firearm mortality in most states and prevention efforts could be concentrated into the highest-risk groups for suicide, such as older males and rural adults,” says Goldstick.
To address domestic violence-related homicides among women, states might want to heed research showing that restricting firearm access among domestic violence offenders and people convicted of violent crime can reduce domestic violence homicide. To address suicides and unintentional deaths by firearms among young people, states might look to research showing that reducing access to firearms by children can affect rates of both types of death.
About the study
Goldstick and Cunningham worked on the study with April Zeoli, Ph.D., M.P.H., of the Michigan State University College of Criminal Justice, and Christina Mair, Ph.D. of the University of Pittsburgh School of Public Health. Cunningham is a co-director, and Goldstick and Zeoli are members, of the Firearm Safety Among Children and Teens Consortium, funded by the National Institutes of Child Health and Human Development.
The authors note that they can’t tell from the data they used what factors led to the increase in firearm death rates in recent years, nor the decreases seen in certain groups and geographic areas. They do say that the consistent findings across so many states and demographic groups indicate that the rise from 2015 to 2017 was not due to random variation.
The authors also acknowledge that deaths are only one way to measure the impact of firearms on individuals and society. But data on non-fatal firearm injuries and other impacts of firearm injury has not been compiled, a fact that the FACTS Consortium’s members laid out in a group of recent papers published in the Journal of Behavioral Medicine. They also laid out the most urgent firearm-related pediatric research questions that need answers in a recent piece in the journal Pediatrics.
To protect identities, CDC data were not available (or “suppressed”) when fewer than 10 people of a given characteristic group died from a firearm injury in a particular state in a year.
Reference: Health Affairs, 10.1377/hlthaff.2019.00258
Original post https://alertarticles.info